Abstract
Study design:
Prospective cohort study with medical record review.
Objective:
To evaluate the clinical utility of an infection control program in a patient cohort at high risk for methicillin-resistant Staphylococcus aureus (MRSA) infection and to identify risk factors interfering with successful decolonization of MRSA.
Setting:
All spinal cord injured (SCI) patients hospitalized at the Swiss Paraplegic Center (SPC) Nottwil from April 1991 to April 2001.
Methods:
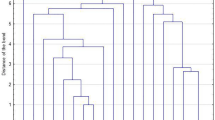
Patients whose medical records indicated laboratory-confirmed MRSA colonization or infection were included. Incidence of MRSA colonization or infection was classified as community acquired, nosocomial or transferred based on standardized criteria. Risk factors for community-acquired MRSA colonization in SCI patients were determined. MRSA subtyping and identification of nosocomial spread was performed through pulse-field gel electrophoresis (PFGE).
Results:
Of 5992 admissions, 100 episodes of MRSA (colonization 22 cases, infection 78 cases) were identified among 76 patients. Overall incidence (1991–2001) per 1000 patient days was 0.26 cases on admission compared to 0.08 at discharge (P<0.001). Community-acquired MRSA was most frequent (56%) followed by nosocomial acquisition (34%). PFGE subtyping identified two nosocomial clusters with six and three cases, respectively. Most of community-acquired MRSA isolates were genetically unrelated and also distinct from epidemic strains identified in Switzerland during the study period. Decolonization was successful in 60 of 76 (78.9%) MRSA-positive patients.
Conclusion:
In the largest European SCI center, MRSA controlling is feasible if infection control policies are vigorously applied.
Similar content being viewed by others
Log in or create a free account to read this content
Gain free access to this article, as well as selected content from this journal and more on nature.com
or
References
Diekema DJ, Pfaller MA, Schmitz FJ, Smayevsky J, Bell J, Jones RN et al. Survey of infections due to Staphylococcus species: frequency of occurrence and antimicrobial susceptibility of isolates collected in the United States, Canada, Latin America, Europe, and the Western Pacific region of the SENTRY antimicrobial surveillance program, 1997–1999. Clin Infect Dis 2001; 32: S114–S132.
Thom JD, Wolfe V, Perkash I, Lin VW . Methicillin-resistant Staphylococcus aureus in patients with spinal cord injury. J Spinal Cord Med 1999; 22: 125–131.
Mylotte JM, Kahler L, Graham R, Young L, Goodnough S . Prospective surveillance for antibiotic-resistant organisms in patients with spinal cord injury admitted to an acute rehabilitation unit. Am J Infect Control 2000; 28: 291–297.
Crisostomo MI, Westh H, Tomasz A, Mk C, Oliveria DC, de Lencastre H . The evolution of methicillin resistance in Staphylococcus aureus: similarity of genetic backgrounds in historically early methicillin-susceptible and resistant and contemporary epidemic clones. Proc Natl Acad Sci USA 2001; 98: 9865–9870.
Vancomycin-resistant Staphylococcus aureus—Pennsylvania, 2002. MMWR Morb Mortal Wkly Rep 2002; 51: 902.
Charlson ME, Pompei P, Ales KL, MacKenzie CR . A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis 1987; 40: 373–383.
Marino RJ, Barros T, Biering-Sorensen F, Burns SP, Donovan WH, Graves DE et al. International standards for neurological classification of spinal cord injury. J Spinal Cord Med 2003; 26 (Suppl 1): S50–S56.
Garner JS, Jarvis WR, Emori TG, Horan TC, Hughes JM . CDC definitions for nosocomial infections. Am J Infect Control 1988; 16: 128–140.
Fluckiger U, Widmer AF . Epidemiology of methicillin-resistant Staphylococcus aureus. J Chemother 1999; 45: 121–134.
Tenover FC, Arbeit RD, Goering RV, Mickelsen PA, Murray BE, Persing DH et al. Interpreting chromosomal DNA restriction pattern produced by pulsed-field gel electrophoresis: criteria for bacterial strain typing. J Clin Microbiol 1995; 33: 2233–2239.
Blanc DS, Pittet D, Ruef C, Widmer AF, Muhlemann K, Petignat C et al. Molecular epidemiology of predominant clones and sporadic strains of methicillin resistant Staphylococcus aureus in Switzerland and comparison with European epidemic clones. Clin Microbiol Infect 2002; 8: 419–426.
Jackson MM, Lynch P . Guideline for isolation precautions in hospitals. Am J Infect Control 1996; 24: 203–206.
National Committee for Clinical Laboratory Standards. Performance Standards for Antimicrobial Disk Susceptibility Tests, 4th edn. Approved Standard. NCCLS document M2-A4. NCCLS: Villanova, PA, 1990.
Strandιn A, Frei R, Widmer AF . Molecular typing of methicillin-resistant Staphylococcus aureus: can PCR replace pulsed-field gel electrophoresis? J Clin Microbiol 2003; 41: 3181–3186.
Blanc DS, Petignat C, Moreillon P, Entenza JM, Eisenring M, Kleiber H et al. Unusual spread of a penicillin-susceptible methicillin resistant Staphylococcus aureus clone in a geographic area of low incidence. Clin Infect Dis 1999; 29: 1512–1518.
Muto CA, Jernigan CA, Ostrowsky BE, Richet HM, Jarvis WR, Boyce JM et al. SHEA guideline for preventing nosocomial transmission of multidrug-resistant strains of Staphylococcus aureus and Enterococcus. Infect Control Hosp Epidemiol 2003; 24: 362–386.
Mylotte JM, Graham R, Kahler L, Young R, Goodnough S . Epidemiology of nosocomial infection and resistant organisms in patients admitted for the first time to an acute rehabilitation unit. Clin Infect Dis 2000; 30: 425–432.
Kotilainen P, Routamaa M, Peltonen R, Evesti P, Eerola E, Salmenlinna S et al. Eradication of methicillin-resistant Staphylococcus aureus from a health center ward and associated nursing home. Arch Intern Med 2001; 161: 859–863.
Tenover FC, Arbeit R, Archer G, Biddle J, Byrne S, Goering R et al. Comparison of traditional and molecular methods of typing isolates of Staphylococcus aureus. J Clin Microbiol 1994; 32: 407–415.
Deplano A, Schuermans A, Van Eldere J, Witte W, Meugnier H, Etienne J et al. Multicenter evaluation of epidemiological typing of methicillin-resistant Staphylococcus aureus strains by repetitive-element PCR analysis. J Clin Microbiol 2000; 38: 3527–3533.
Acknowledgements
This study was supported by the Swiss Paraplegic Foundation.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kappel, C., Widmer, A., Geng, V. et al. Successful control of methicillin-resistant Staphylococcus aureus in a spinal cord injury center: a 10-year prospective study including molecular typing. Spinal Cord 46, 438–444 (2008). https://doi.org/10.1038/sj.sc.3102135
Received:
Revised:
Accepted:
Published:
Issue date:
DOI: https://doi.org/10.1038/sj.sc.3102135