Abstract
Aim:
Dexibuprofen, the S(+)-isomer of ibuprofen, is an effective therapeutic agent for the treatment of neurodegenerative disorders. However, its clinical use is hampered by a limited brain distribution. The aim of this study was to design and synthesize brain-targeting dexibuprofen prodrugs and to evaluate their brain-targeting efficiency using biodistribution and pharmacokinetic analysis.
Methods:
In vitro stability, biodistribution and pharmacokinetic studies were performed on male Sprague-Dawley rats. The concentrations of dexibuprofen in biosamples, including the plasma, brain, heart, liver, spleen, lung, and kidney, were measured using high pressure lipid chromatography (HPLC). The pharmacokinetic parameters of the drug in the plasma and tissues were calculated using obtained data and statistics.
Results:
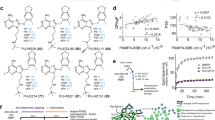
Five dexibuprofen prodrugs that were modified to contain ethanolamine-related structures were designed and synthesized. Their chemical structures were confirmed using 1H NMR, 13C NMR, IR, and HRMS. In the biodistribution study, 10 min after intravenous administration of dexibuprofen (11.70 mg/kg) and its prodrugs (the dose of each compound was equivalent to 11.70 mg/kg of dexibuprofen) in male Sprague-Dawley rats, the dexibuprofen concentrations in the brain and plasma were measured. The Cbrain/Cplasma ratios of prodrugs 1, 2, 3, 4, and 5 were 17.0-, 15.7-, 7.88-, 9.31-, and 3.42-fold higher than that of dexibuprofen, respectively (P<0.01). Thus, each of the prodrugs exhibited a significantly enhanced brain distribution when compared with dexibuprofen. In the pharmacokinetic study, prodrug 1 exhibited a brain-targeting index of 11.19 {DTI=(AUCbrain/AUCplasma)1/(AUCbrain/AUCplasma)dexibuprofen}.
Conclusion:
The ethanolamine-related structures may play an important role in transport across the brain blood barrier.
Similar content being viewed by others
Log in or create a free account to read this content
Gain free access to this article, as well as selected content from this journal and more on nature.com
or
References
Patel PM, Drummond JC, Sano T, Cole DJ, Kalkman CJ, Yaksh TL . Effect of ibuprofen on regional eicosanoid production and neuronal injury after forebrain ischemia in rats. Brain Res 1993; 614: 315–24.
Szekely CA, Thorne JE, Zandi PP, Messias E, Breitner JC, Goodman SN . Nonsteroidal anti-inflammatory drugs for the prevention of Alzheimer's disease: a systematic review. Neuroepidemiology 2004; 23: 159–69.
Silakova JM, Hewett JA, Hewett SJ . Naproxen reduces excitotoxic neurodegeneration in vivo with an extended therapeutic window. J Pharmacol Exp Ther 2004; 309: 1060–6.
Bannwarth B, Lapicque F, Pehourcq F, Gillet P, Schaeverbeke T, Laborde C, et al. Stereoselective disposition of ibuprofen enantiomers in human cerebrospinal fluid. Br J Clin Pharmacol 1995; 40: 266–9.
Mannila A, Rautio J, Lehtonen M, Jarvinen T, Savolainen J . Inefficient central nervous system delivery limits the use of ibuprofen in neurodegenerative diseases. Eur J Pharm Sci 2005; 24: 101–5.
Matoga M, Pehourcq F, Lagrange F, Tramu G, Bannwarth B . Influence of molecular lipophilicity on the diffusion of arylpropionate non-steroidal anti-inflammatory drugs into the cerebrospinal fluid. Arzneimittel-forschung 1999; 49: 477–82.
Eriksen JL, Sagi SA, Smith TE, Weggen S, Das P, McLendon DC, et al. NSAIDs and enantiomers of flurbiprofen target gamma-secretase and lower Abeta 42 in vivo. J Clin Invest 2003; 112: 440–9.
Brune K, Neubert A . Pharmacokinetic and pharmacodynamic aspects of the ideal COX-2 inhibitor: a pharmacologist's perspective. Clin Exp Rheumatol 2001; 19: S51–7.
Rainsford KD, Schweitzer A, Brune K . Autoradiographic and biochemical observations on the distribution of non-steroid anti-inflammatory drugs. Arch Int Pharmacodyn Ther 1981; 250: 180–94.
Golden PL, Pollack GM . Blood-brain barrier efflux transport. J Pharm Sci 2003; 92: 1739–53.
Neuwelt EA . Mechanisms of disease: the blood-brain barrier. Neurosurgery 2004; 54: 131–40.
Habgood MD, Begley DJ, Abbott NJ . Determinants of passive drug entry into the central nervous system. Cell Mol Neurobiol 2000; 20: 231–53.
Clark DE . In silico prediction of blood-brain barrier permeation. Drug Discov Today 2003; 8: 927–33.
Lee G, Dallas S, Hong M, Bendayan R . Drug transporters in the central nervous system: brain barriers and brain parenchyma considerations. Pharmacol Rev 2001; 53: 569–96.
Kusuhara H, Sugiyama Y . Active efflux across the blood-brain barrier: role of the solute carrier family. NeuroRx 2005; 2: 73–85.
Smith QR . Carrier-mediated transport to enhance drug delivery to brain. International Congress Series 2005; 1277: 63–74.
Kurihara A, Deguchi Y, Pardridge WM . Epidermal growth factor radiopharmaceuticals: 111ln chelation, conjugation to a blood-brain barrier delivery vector via a biotin-polyethylene linker, pharmacokinetics, and in vivo imaging of experimental brain tumors. Bioconjugate Chem 1999; 10: 502–11.
Friden PM, Walus LR, Musso GF . Anti-transferrin receptor antibody and antibody drug conjugates cross the blood brain barrier. Proc Natl Acad Sci U S A 1991; 88: 4771–5.
Pardridge WM, Kumagai AK, Eisenberg JB . Chimeric peptides as a vehicle for peptide pharmaceutical delivery through the blood-brain barrier. Biochem Biophys Res Commun 1987; 146: 307–13.
Kang YS, Pardridge L . Brain delivery of biotin bound to a conjugate of neutral avidin and cationized human albumin. Pharm Res 1994; 11: 1257–64.
Khan MSY, Akhter M . Synthesis, pharmacological activity and hydrolytic behavior of glyceride prodrugs of ibuprofen. Eur J Med Chem 2005; 40: 371–6.
Zhao XG, Tao XY, Wei DZ, Song QX . Pharmacological activity and hydrolysis behavior of novel ibuprofen glucopyranoside conjugates. Eur J Med Chem 2006; 41: 1352–8.
Perioli L, Ambrogi V, Bernardini C, Grandolini G, Ricci M, Giovagnoli S, et al. Potential prodrugs of non-steroidal anti-inflammatory agents for targeted drug delivery to the CNS. Eur J Med Chem 2004; 39: 715–27.
Siskou IC, Rekka EA, Kourounakis AP, Chrysselis MC, Tsiakitzis K, Kourounakis PN . Design and study of some novel ibuprofen derivatives with potential nootropic and neuroprotective properties. Bioorgan Med Chem 2007; 15: 951–61.
Shanbhag V, Crider AM, Gokhale R, Harpalani A, Dick RM . Prodrug and amide prodrugs of ibuprofen and naproxen: synthesis, anti-inflammatory activity, and gastrointestinal toxicity. J Pharm Sci 1992; 81: 149–54.
Halen PK, Chagti KK, Giridhar R, Yadav MR . Combining anticholinergic and anti-inflammatory activities into a single moiety: a novel approach to reduce gastrointestinal toxicity of ibuprofen and ketoprofen. Chem Biol Drug Des 2007; 70: 450–5.
Song N, Li YX, Sun X, Qu F . Synthesis of (±)ibuprofen sugar derivative. Acta Pharm Sin 2004; 39: 105–9.
Mork N, Bundgaard H . Stereoselective enzymatic hydrolysis of various ester prodrugs of ibuprofen and flurbiprofen in human plasma. Pharm Res 1992; 9: 492–6.
Acknowledgements
This work was supported by the National Natural Science Foundation of China (Grant No 81130060).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Zhang, X., Liu, X., Gong, T. et al. In vitro and in vivo investigation of dexibuprofen derivatives for CNS delivery. Acta Pharmacol Sin 33, 279–288 (2012). https://doi.org/10.1038/aps.2011.144
Received:
Accepted:
Published:
Issue date:
DOI: https://doi.org/10.1038/aps.2011.144
Keywords
This article is cited by
-
Dexibuprofen ameliorates peripheral and central risk factors associated with Alzheimer’s disease in metabolically stressed APPswe/PS1dE9 mice
Cell & Bioscience (2021)
-
The antipyretic efficacy and safety of propacetamol compared with dexibuprofen in febrile children: a multicenter, randomized, double-blind, comparative, phase 3 clinical trial
BMC Pediatrics (2018)
-
Mechanism of Brain Targeting by Dexibuprofen Prodrugs Modified with Ethanolamine-Related Structures
Journal of Cerebral Blood Flow & Metabolism (2015)