Abstract
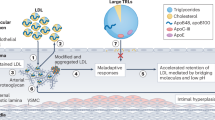
Plasma levels of high-density lipoprotein (HDL) cholesterol and its major apolipoprotein (apo), apo A-I, are inversely correlated with the incidence of ischemic cardiovascular diseases. Reverse cholesterol transport is likely the main mechanism underlying the atheroprotective effects of HDL. Here, we investigated whether increased HDL cholesterol following hepatocyte-directed adenoviral rabbit apo A-I (AdrA-I) or rabbit lecithin-cholesterol acyltransferase (LCAT) (AdrLCAT) transfer may induce cholesterol unloading in complex atherosclerotic lesions in heterozygous low-density lipoprotein receptor-deficient rabbits fed a 0.15% cholesterol diet for 420 days before and for 120 days after transfer. HDL cholesterol levels increased 2.0-fold (P<0.001) and 1.9-fold (P<0.001) in the 120 days after transfer with AdrA-I and AdrLCAT, respectively, compared to levels just before transfer whereas non-HDL cholesterol remained unchanged. Increased HDL cholesterol following AdrA-I and AdrLCAT transfer resulted in a 31% (P<0.05) reduction of the intima/media ratio in comparison with the control progression group. Compared to the baseline group killed after 420 days of cholesterol diet, AdrA-I and AdrLCAT transfer reduced the percentage of Oil Red O area 1.6-fold (P<0.001) and 1.4-fold (P<0.001), respectively. In conclusion, increased HDL cholesterol after AdrA-I and AdrLCAT transfer inhibits progression of atherosclerosis and induces cholesterol unloading in complex lesions in rabbits.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 6 print issues and online access
$259.00 per year
only $43.17 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
Abbreviations
- Apo:
-
apolipoprotein
- LCAT:
-
lecithin:cholesterol acyltransferase
- LDL:
-
low-density lipoproteins
- HDL:
-
high-density lipoproteins
- LDLr:
-
low-density lipoprotein receptor.
References
Gordon DJ, Rifkind BM . High-density lipoprotein—the clinical implications of recent studies. N Eng J Med 1989; 321: 1311–1316.
Rubin EM, Krauss RM, Spangler EA, Verstuyft JG, Clift SM . Inhibition of early atherogenesis in transgenic mice by human apolipoprotein AI. Nature 1991; 353: 265–267.
Duverger N, Kruth H, Emmanuel F, Caillaud JM, Viglietta C, Castro G et al. Inhibition of atherosclerosis development in cholesterol-fed human apolipoprotein A-I-transgenic rabbits. Circulation 1996; 94: 713–717.
Paszty C, Maeda N, Verstuyft J, Rubin EM . Apolipoprotein AI transgene corrects apolipoprotein E deficiency-induced atherosclerosis in mice. J Clin Invest 1994; 94: 899–903.
Plump AS, Scott CJ, Breslow JL . Human apolipoprotein A-I gene expression increases high density lipoprotein and suppresses atherosclerosis in the apolipoprotein E-deficient mouse. Proc Natl Acad Sci USA 1994; 91: 9607–9611.
Badimon JJ, Badimon L, Fuster V . Regression of atherosclerotic lesions by high density lipoprotein plasma fraction in the cholesterol-fed rabbit. J Clin Invest 1990; 85: 1234–1241.
Tangirala RK, Tsukamoto K, Chun SH, Usher D, Pure E, Rader DJ . Regression of atherosclerosis induced by liver-directed gene transfer of apolipoprotein A-I in mice. Circulation 1999; 100: 1816–1822.
Kosek AB, Durbin D, Jonas A . Binding affinity and reactivity of lecithin cholesterol acyltransferase with native lipoproteins. Biochem Biophys Res Commun 1999; 258: 548–551.
Greeve J, Altkemper I, Dieterich JH, Greten H, Windler E . Apolipoprotein B mRNA editing in 12 different mammalian species: hepatic expression is reflected in low concentrations of apoB-containing plasma lipoproteins. J Lipid Res 1993; 34: 1367–1383.
Nagashima M, McLean JW, Lawn RM . Cloning and mRNA tissue distribution of rabbit cholesteryl ester transfer protein. J Lipid Res 1988; 29: 1643–1649.
Tall AR . Plasma cholesteryl ester transfer protein. J Lipid Res 1993; 34: 1255–1274.
Barter P, Rye KA . Cholesteryl ester transfer protein: its role in plasma lipid transport. Clin Exp Pharmacol Physiol 1994; 21: 663–672.
Tall A . Plasma lipid transfer proteins. Annu Rev Biochem 1995; 64: 235–257.
Lievens J, Snoeys J, Vekemans K, Van Linthout S, de Zanger R, Collen D et al. The size of sinusoidal fenestrae is a critical determinant of hepatocyte transduction after adenoviral gene transfer. Gene Therapy 2004; 11: 1523–1531.
Snoeys J, Lievens J, Wisse E, Jacobs F, Duimel H, Collen D et al. Species differences in transgene DNA uptake in hepatocytes after adenoviral transfer correlate with the size of endothelial fenestrae. Gene Therapy 2007; 14: 604–612.
Wisse E, Jacobs F, Topal B, Frederik P, De Geest B . The size of endothelial fenestrae in human liver sinusoids: implications for hepatocyte-directed gene transfer. Gene Therapy 2008; 15: 1193–1199.
De Geest B, Van Linthout S, Collen D . Sustained expression of human apo A-I following adenoviral gene transfer in mice. Gene Therapy 2001; 8: 121–127.
De Geest BR, Van Linthout SA, Collen D . Humoral immune response in mice against a circulating antigen induced by adenoviral transfer is strictly dependent on expression in antigen-presenting cells. Blood 2003; 101: 2551–2556.
Mingozzi F, Liu YL, Dobrzynski E, Kaufhold A, Liu JH, Wang Y et al. Induction of immune tolerance to coagulation factor IX antigen by in vivo hepatic gene transfer. J Clin Invest 2003; 111: 1347–1356.
Van Linthout S, Collen D, De Geest B . Effect of promoters and enhancers on expression, transgene DNA persistence, and hepatotoxicity after adenoviral gene transfer of human apolipoprotein A-I. Hum Gene Ther 2002; 13: 829–840.
Van Linthout S, Lusky M, Collen D, De Geest B . Persistent hepatic expression of human apo A-I after transfer with a helper-virus independent adenoviral vector. Gene Therapy 2002; 9: 1520–1528.
Belalcazar LM, Merched A, Carr B, Oka K, Chen KH, Pastore L et al. Long-term stable expression of human apolipoprotein A-I mediated by helper-dependent adenovirus gene transfer inhibits atherosclerosis progression and remodels atherosclerotic plaques in a mouse model of familial hypercholesterolemia. Circulation 2003; 107: 2726–2732.
Brousseau ME, Kauffman RD, Herderick EE, Demosky Jr SJ, Evans W, Marcovina S et al. LCAT modulates atherogenic plasma lipoproteins and the extent of atherosclerosis only in the presence of normal LDL receptors in transgenic rabbits. Arterioscler Thromb Vasc Biol 2000; 20: 450–458.
Shore VG, Shore B, Hart RG . Changes in apolipoproteins and properties of rabbit very low density lipoproteins on induction of cholesteremia. Biochemistry 1974; 13: 1579–1585.
Roth RI, Gaubatz JW, Gotto Jr AM, Patsch JR . Effect of cholesterol feeding on the distribution of plasma lipoproteins and on the metabolism of apolipoprotein E in the rabbit. J Lipid Res 1983; 24: 1–11.
Chao YS, Yamin TT, Thompson GM, Kroon PA . Tissue-specific expression of genes encoding apolipoprotein E and apolipoprotein A-I in rabbits. J Biol Chem 1984; 259: 5306–5309.
Sun YP, Lu NC, Parmley WW, Hollenbeck CB . Effects of cholesterol diets on vascular function and atherogenesis in rabbits. Proc Soc Exp Biol Med 2000; 224: 166–171.
Kritchevsky D, Tepper SA, Vesselinovitch D, Wissler RW . Cholesterol vehicle in experimental atherosclerosis. 11. Peanut oil. Atherosclerosis 1971; 14: 53–64.
Adams CW, Miller NE, Morgan RS, Rao SN . Lipoprotein levels and tissue lipids in fatty-fibrous atherosclerosis induced in rabbits by two years’ cholesterol feeding at a low level. Atherosclerosis 1982; 44: 1–8.
Spagnoli LG, Orlandi A, Mauriello A, Santeusanio G, de Angelis C, Lucreziotti R et al. Aging and atherosclerosis in the rabbit. 1. Distribution, prevalence and morphology of atherosclerotic lesions. Atherosclerosis 1991; 89: 11–24.
Bocan TM, Mueller SB, Uhlendorf PD, Ferguson E, Newton RS . Dietary and mechanically induced rabbit iliac-femoral atherosclerotic lesions: a chemical and morphologic evaluation. Exp Mol Pathol 1991; 54: 201–277.
Lupu F, Danaricu I, Simionescu N . Development of intracellular lipid deposits in the lipid-laden cells of atherosclerotic lesions. A cytochemical and ultrastructural study. Atherosclerosis 1987; 67: 127–142.
Daley SJ, Klemp KF, Guyton JR, Rogers KA . Cholesterol-fed and casein-fed rabbit models of atherosclerosis. Part 2: differing morphological severity of atherogenesis despite matched plasma cholesterol levels. Arterioscler Thromb 1994; 14: 105–141.
Kolodgie FD, Katocs Jr AS, Largis EE, Wrenn SM, Cornhill JF, Herderick EE et al. Hypercholesterolemia in the rabbit induced by feeding graded amounts of low-level cholesterol. Methodological considerations regarding individual variability in response to dietary cholesterol and development of lesion type. Arterioscler Thromb Vasc Biol 1996; 16: 1454–1464.
Atkinson JB, Hoover RL, Berry KK, Swift LL . Cholesterol-fed heterozygous Watanabe heritable hyperlipidemic rabbits: a new model for atherosclerosis. Atherosclerosis 1989; 78: 123–136.
Hoeg JM, Santamarina-Fojo S, Berard AM, Cornhill JF, Herderick EE, Feldman SH et al. Overexpression of lecithin:cholesterol acyltransferase in transgenic rabbits prevents diet-induced atherosclerosis. Proc Natl Acad Sci USA 1996; 93: 11448–11453.
Berard AM, Foger B, Remaley A, Shamburek R, Vaisman BL, Talley G et al. High plasma HDL concentrations associated with enhanced atherosclerosis in transgenic mice overexpressing lecithin-cholesteryl acyltransferase. Nat Med 1997; 3: 744–749.
Mehlum A, Muri M, Hagve TA, Solberg LA, Prydz H . Mice overexpressing human lecithin:cholesterol acyltransferase are not protected against diet-induced atherosclerosis. APMIS 1997; 105: 861–868.
Mehlum A, Gjernes E, Solberg LA, Hagve TA, Prydz H . Overexpression of human lecithin:cholesterol acyltransferase in mice offers no protection against diet-induced atherosclerosis. APMIS 2000; 108: 336–342.
Furbee Jr JW, Parks JS . Transgenic overexpression of human lecithin:cholesterol acyltransferase (LCAT) in mice does not increase aortic cholesterol deposition. Atherosclerosis 2002; 165: 89–100.
Kondo T, Watanabe Y . [A heritable hyperlipemic rabbit (author's translation)]. Jikken Dobutsu 1975; 24: 89–94.
Watanabe Y . Serial inbreeding of rabbits with hereditary hyperlipidemia (WHHL- rabbit). Atherosclerosis 1980; 36: 261–268.
Sun H, Usui S, Shiomi M, Watanabe T, Fan J . A rapid PCR method of genotyping LDL receptor mutations in WHHL rabbits. J Atheroscler Thromb 2002; 9: 145–148.
Murata Y, Maeda E, Yoshino G, Kasuga M . Cloning of rabbit LCAT cDNA: increase in LCAT mRNA abundance in the liver of cholesterol-fed rabbits. J Lipid Res 1996; 37: 1616–1622.
Pan TC, Hao QL, Yamin TT, Dai PH, Chen BS, Chen SL et al. Rabbit apolipoprotein A-I mRNA and gene. Evidence that rabbit apolipoprotein A-I is synthesized in the intestine but not in the liver. Eur J Biochem 1987; 170: 99–104.
Feng Y, Jacobs F, Van Craeyveld E, Brunaud C, Snoeys J, Tjwa M et al. Human ApoA-I transfer attenuates transplant arteriosclerosis via enhanced incorporation of bone marrow-derived endothelial progenitor cells. Arterioscler Thromb Vasc Biol 2008; 28: 278–283.
Chapman MJ, Goldstein S, Lagrange D, Laplaud PM . A density gradient ultracentrifugal procedure for the isolation of the major lipoprotein classes from human serum. J Lipid Res 1981; 22: 339–358.
Jacobs F, Van Craeyveld E, Feng Y, Snoeys J, De Geest B . Adenoviral low density lipoprotein receptor attenuates progression of atherosclerosis and decreases tissue cholesterol levels in a murine model of familial hypercholesterolemia. Atherosclerosis 2008; 201: 289–297.
Junqueira LC, Bignolas G, Brentani RR . Picrosirius staining plus polarization microscopy, a specific method for collagen detection in tissue sections. Histochem J 1979; 11: 447–455.
Acknowledgements
This work was supported by grants G.0564.05 and G.0533.08 of the Fonds voor Wetenschappelijk Onderzoek-Vlaanderen. The Center for Molecular and Vascular Biology is supported by the Excellentiefinanciering KU Leuven (EF/05/013). Eline Van Craeyveld is a research assistant of the Fonds voor Wetenschappelijk Onderzoek-Vlaanderen. Frank Jacobs is a research assistant of the Instituut voor de Aanmoediging van Innovatie door Wetenschap en Technologie in Vlaanderen.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Van Craeyveld, E., Lievens, J., Jacobs, F. et al. Apolipoprotein A-I and lecithin:cholesterol acyltransferase transfer induce cholesterol unloading in complex atherosclerotic lesions. Gene Ther 16, 757–765 (2009). https://doi.org/10.1038/gt.2009.8
Received:
Revised:
Accepted:
Published:
Issue date:
DOI: https://doi.org/10.1038/gt.2009.8
Keywords
This article is cited by
-
Regression and stabilization of advanced murine atherosclerotic lesions: a comparison of LDL lowering and HDL raising gene transfer strategies
Journal of Molecular Medicine (2011)
-
Lecithin Cholesterol Acyltransferase: An Anti- or Pro-atherogenic Factor?
Current Atherosclerosis Reports (2011)
-
Protective molecules and their cognate antibodies: new players in autoimmunity
Autoimmunity Highlights (2010)