Abstract
Objective:
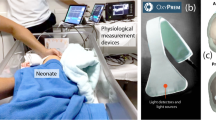
Monitoring the changes in buccal tissue oxygen saturation (StO2) may aid in early diagnosis of circulatory compromise. Our objective was to define the normal value of buccal StO2 and its correlation to the middle cerebral artery (MCA) flow indices and cardiac output in healthy term infants during the first 48 h after birth.
Study Design:
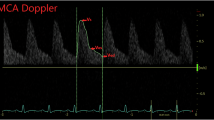
In this prospective study, we assessed buccal StO2 by visible light spectroscopy and assessed the left ventricular output (LVO) and MCA flow indices by ultrasound on postnatal days 1 and 2. We enrolled 20 term neonates. The Wilcoxon-matched pairs signed-rank test and Pearson correlation were used to analyze the data.
Result:
Median (range) buccal StO2 readings were 68% (62 to 72) on day 1 and 66% (61 to 69) on day 2 (P=0.03). A weak but significant positive correlation was found between buccal StO2 and LVO (r=0.37, P=0.023). There was no correlation between buccal StO2 and MCA mean velocity or pulsatility index.
Conclusion:
Under a physiological state, buccal StO2 in resting healthy neonates is 61 to 72%, regardless of variability in systemic and cerebral blood flow. Because of its ease of use and non-invasive nature, the use of visible light spectroscopy in conditions with circulatory compromise needs to be further investigated.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Noori S, Seri I . Etiology, pathophysiology, and phases of neonatal shock. In: Kleinman CS, Seri I, (eds). Hemodynamics and Cardiology. Neonatal Questions and Controversies. Saunders Elsevier: Philadelphia, 2008, pp 3–18.
Pigula FA, Gandhi SK, Siewers RD, Davis PJ, Webber SA, Nemoto EM . Regional low-flow perfusion provides somatic circulatory support during neonatal aortic arch surgery. Ann Thorac Surg 2001; 72: 401–406.
Amir G, Ramamoorthy C, Riemer RK, Davis CR, Hanley FL, Reddy VM . Visual light spectroscopy reflects flow-related changes in brain oxygenation during regional low-flow perfusion and deep hypothermic circulatory arrest. J Thorac Cardiovasc Surg 2006; 132: 1307–1313.
Heninger C, Ramamoorthy C, Amir G, Kamra K, Reddy VM, Hanley FL et al. Esophageal saturation during antegrade cerebral perfusion: a preliminary report using visible light spectroscopy. Paediatr Anaesth 2006; 16: 1133–1137.
Benaron DA, Parachikov IH, Friedland S, Soetikno R, Brock-Utne J, van der Starre PJ et al. Continuous, noninvasive, and localized microvascular tissue oximetry using visible light spectroscopy. Anesthesiology 2004; 100: 1469–1475.
Bronshtein V, LaGamma EF, Curry JM, Hoffman JG, Parvez B . Visual light spectrography (VLS) for detecting alteration in tissue oxygenation with administration of packed red blood cells (PRBC) in very low birth weight (VLBW) premature infants. Neonatology Today 2009; 4: 1–6.
Skinner J, Alverson D, Hunter S . Echocardiography for the Neonatologist. Churchill Livingstone: Edinburgh, 2000.
Kluckow M, Evans N . Early echocardiographic prediction of symptomatic patent ductus arteriosus in preterm infants undergoing mechanical ventilation. J Pediatr 1995; 127: 774–779.
Norman M . Low birth weight and the developing vascular tree: a systematic review. Acta Paediatr 2008; 97: 1165–1172.
Stark MJ, Clifton VL, Wright IM . Microvascular flow, clinical illness severity and cardiovascular function in the preterm infant. Arch Dis Child Fetal Neonatal Ed 2008; 93: F271–F274.
Kroth J, Weidlich K, Hiedl S, Nussbaum C, Christ F, Genzel-boroviczény O . Functional vessel density in the first month of life in preterm neonates. Pediatr Res 2008; 64: 567–571.
Rostami N, Keszler M . Validation of visible light tissue oximetry in newborn infants. E-PAS 2010; 4407.320.
Kluckow M, Evans N . Superior vena cava flow in newborn infants: a novel marker of systemic blood flow. Arch Dis Child Fetal Neonatal Ed 2000; 82: F182–F187.
Meek JH, Tyszczuk L, Elwell CE, Wyatt JS . Cerebral blood flow increases over the first three days of life in extremely preterm neonates. Arch Dis Child Fetal Neonatal Ed 1998; 78: F33–F37.
Kehrer M, Blumenstock G, Ehehalt S, Goelz R, Poets C, Schöning M . Development of cerebral blood flow volume in preterm neonates during the first two weeks of life. Pediatr Res 2005; 58: 927–930.
Raju TNK . Cerebral Doppler studies in the fetus and the newborn infant. J Pediatr 1991; 119: 165–174.
Greisen G, Johansen K, Ellison PH, Fredriksen PS, Mali J, Friis-Hansen B . Cerebral blood flow in the newborn: Comparison of Doppler ultrasound and 133xenon clearance. J Pediatr 1984; 104: 411–418.
Hansen NB, Stonestreet BS, Rosenkrantz TS, Oh W . Validity of Doppler measurements of anterior cerebral artery blood flow velocity: Correlation with brain blood flow in piglets. Pediatrics 1983; 72: 526–531.
Acknowledgements
We thank the families who gave us the permission to evaluate their babies, and Spectros for providing us with the T-Stat device and buccal sensors. We also thank Michael P Anderson, PhD (Department of Biostatistics and Epidemiology, OUHSC, Oklahoma City, OK, USA) for his statistical advice.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Noori, S., Drabu, B., McCoy, M. et al. Non-invasive measurement of local tissue perfusion and its correlation with hemodynamic indices during the early postnatal period in term neonates. J Perinatol 31, 785–788 (2011). https://doi.org/10.1038/jp.2011.34
Received:
Revised:
Accepted:
Published:
Issue date:
DOI: https://doi.org/10.1038/jp.2011.34