Abstract
Objective:
To assess the need for respiratory support in late preterm infants treated with sustained lung inflation (SLI) at birth.
Study design:
In this controlled trial, we randomly assigned infants born at 34+0 to 36+6 weeks of gestation to receive SLI (25 cmH2O for 15 s) at birth, followed by continuous positive airway pressure (CPAP) or assistance according to the recommendations of the American Academy of Pediatrics. The primary outcome was the need for any type of respiratory support. The secondary outcomes included neonatal intensive care unit (NICU) admission for respiratory distress and length of stay. The risk ratios (RRs) and 95% confidence intervals (CIs) of the outcomes were calculated for the SLI group in reference to the control group.
Results:
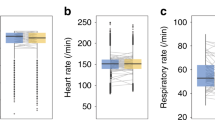
A total of 185 infants were enrolled: 93 in the SLI group and 92 in the control group. No difference was found in the need for any type of respiratory support between the infants treated with SLI and the control group (10.6 vs 8.7%, RR 1.24, 95% CI 0.51 to 2.99). The NICU admission for respiratory distress and the length of stay did not differ between the groups.
Conclusion:
Providing SLI at birth in late preterm infants does not affect their need for respiratory support.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Shapiro-Mendoza CK, Lackritz EM . Epidemiology of late and moderate preterm birth. Semin Fetal Neonatal Med 2012; 17 (3): 120–125.
Kugelman A, Colin AA . Late preterm infants: near term but still in a critical developmental time period. Pediatrics 2013; 132 (4): 741–751.
Gouyon JB, Iacobelli S, Ferdynus C, Bonsante F . Neonatal problems of late and moderate preterm infants. Semin Fetal Neonatal Med 2012; 17 (3): 146–152.
De Luca R, Boulvain M, Irion O, Berner M, Pfister RE . Incidence of early neonatal mortality and morbidity after late-preterm and term cesarean delivery. Pediatrics 2009; 123 (6): e1064–e1071.
Consortium on safe labour Consortium on safe labour, Hibbard JU, Wilkins I, Sun L, Gregory K, Haberman S et al. Respiratory morbidity in late preterm births. JAMA 2010; 304 (4): 419–425.
Lindner W, Vossbeck S, Hummler H, Pohlandt F . Delivery room management of extremely low birth weight infants: spontaneous breathing or intubation? Pediatrics 1999; 103 (5 Pt 1): 961–967.
te Pas AB, Siew M, Wallace MJ, Kitchen MJ, Fouras A, Lewis RA et al. Establishing functional residual capacity at birth: the effect of sustained inflation and positive end-expiratory pressure in a preterm rabbit model. Pediatr Res 2009; 65 (5): 537–541.
te Pas AB, Siew M, Wallace MJ, Kitchen MJ, Fouras A, Lewis RA et al. Effect of sustained inflation length on establishing functional residual capacity at birth in ventilated premature rabbits. Pediatr Res 2009; 66 (3): 295–300.
Polglase GR, Tingay DG, Bhatia R, Berry CA, Kopotic RJ, Kopotic CP et al. Pressure-versus volume-limited sustained inflations at resuscitation of premature newborn lambs. BMC Pediatr 2014; 14: 43.
te Pas AB, Walther FJ . A randomized, controlled trial of delivery room respiratory management in very preterm infants. Pediatrics 2007; 120 (2): 322–329.
Lindner W, Hoegel J, Pohlandt F . Sustained pressure-controlled inflation or intermittent mandatory ventilation in preterm infants in the delivery room? A randomized, controlled trial on initial respiratory support via nasopharyngeal tube. Acta Paediatr 2005; 94 (3): 303–309.
Lista G, Fontana P, Castoldi F, Cavigioli F, Dani C . Does sustained lung inflation at birth improve outcome of preterm infants at risk for respiratory distress syndrome? Neonatology 2011; 99 (1): 45–50.
Bland M . The tyranny of power: is there a better way to calculate sample size? BMJ 2009; 339: b3985.
Goodman SN, Berlin JA . The use of predicted confidence intervals when planning experiments and the misuse of power when interpreting results. Ann Intern Med 1994; 121: 200–206.
Te Pas AB, Davis PG, Hooper SB et al. From liquid to air: breathing after birth. J Pediatr 2008; 152: 607–611.
Vento M, Lista G . Managing preterm infants in the first minutes of life. Paediatr Respir Rev 2015; 16 (3): 151–156.
Hooper SB, Siew ML, Kitchen MJ, te Pas AB . Establishing functional residual capacity in the non-breathing infant. Semin Fetal Neonatal Med 2013; 18 (6): 336–343.
Hillman NH, Kemp MW, Noble PB, Kallapur SG, Jobe AH . Sustained inflation at birth did not protect preterm fetal sheep from lung injury. Am J Physiol Lung Cell Mol Physiol 2013; 305 (6): L446–L453.
Klingenberg C, Sobotka KS, Ong T, Allison BJ, Schmolzer GM, Moss TJ et al. Effect of sustained inflation duration; resuscitation of near-term asphyxiated lambs. Arch Dis Child Fetal Neonatal Ed 2013; 98: F222–F227.
Sobotka KS, Hooper SB, Allison BJ, Te Pas AB, Davis PG, Morley CJ et al. An initial sustained inflation improves the respiratory and cardiovascular transition at birth in preterm lambs. Pediatr Res 2011; 70 (1): 56–60.
Lista G, Boni L, Scopesi F, Mosca F, Trevisanuto D, Messner H et al. Sustained lung inflation at birth for preterm infants: a randomized clinical trial. Pediatrics 2015; 135 (2): e457–e464.
Vyas H, Milner A, Hopkin I, Boon A . Physiologic responses to prolonged and slow-rise inflation in the resuscitation of the asphyxiated newborn infant. J Pediatr 1981; 99 (4): 635–639.
Teune MJ, Bakhuizen S, Gyamfi Bannerman C, Opmeer BC, van Kaam AH, van Wassenaer AG et al. A systematic review of severe morbidity in infants born late preterm. Am J Obstet Gynecol 2011; 205 (4): 374.e1-9.
Pike KC, Lucas JS . Respiratory consequences of late preterm birth. Paediatr Respir Rev 2014; 16 (3): 182–188.
Colin AA, McEvoy C, Castile RG . Respiratory morbidity and lung function in preterm infants of 32 to 36 weeks’ gestational age. Pediatrics 2010; 126 (1): 115–128.
Jain L, Eaton DC . Physiology of fetal lung fluid clearance and the effect of labor. Semin Perinatol 2006; 30 (1): 34–43.
van Vonderen JJ, Hooper SB, Hummler HD, Lopriore E, te Pas AB . Effects of a sustained inflation in preterm infants at birth. J Pediatr 2014; 165 (5): 903–8.e1.
Keszler M . Sustained inflation during neonatal resuscitation. Curr Opin Pediatr 2015; 27 (2): 145–151.
Schmölzer GM, Kumar M, Aziz K, Pichler G, O’Reilly M, Lista G et al. Sustained inflation versus positive pressure ventilation at birth: a systematic review and meta-analysis. Arch Dis Child Fetal Neonatal Ed 2015; 100 (4): F361–F368.
Acknowledgements
The authors have no financial relationships relevant to this article to disclose. No honorarium, grant or other form of payment was given to any of the authors to produce the manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Mercadante, D., Colnaghi, M., Polimeni, V. et al. Sustained lung inflation in late preterm infants: a randomized controlled trial. J Perinatol 36, 443–447 (2016). https://doi.org/10.1038/jp.2015.222
Received:
Revised:
Accepted:
Published:
Issue date:
DOI: https://doi.org/10.1038/jp.2015.222
This article is cited by
-
Feasibility of combining two individualized lung recruitment maneuvers at birth for very low gestational age infants: a retrospective cohort study
BMC Pediatrics (2020)
-
Sustained inflations versus UK standard inflations during initial resuscitation of prematurely born infants in the delivery room: a study protocol for a randomised controlled trial
Trials (2017)