Abstract
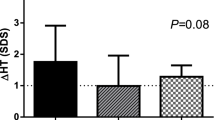
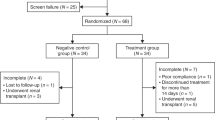
Transition of growth from infancy to childhood is associated with activation of the GH-IGF-I axis. Children with a delayed infancy-childhood transition (DICT) are short as adults. Thus, age at ICT may impact on growth response to GH. The objective was to investigate associations between growth response to GH treatment and ICT timing in children with idiopathic short stature (ISS) in a randomized, controlled, multicenter trial, TRN 88-080. A total of 147 prepubertal children (mean age, 11.5 ± 1.4 y) were randomized to receive GH 33 μg/kg/d (GH33, n = 43), GH 67 μg/kg/d (GH67, n = 61), or no treatment (n = 43). Data on growth to final height (FH) were analyzed after categorization into those with normal (n = 76) or delayed ICT (n = 71). Within the GH33 group, significant height gain at FH was only observed in children with a DICT (p < 0.001), with each month of delay corresponding to gain of 0.13 SD score (SDS). For the GH67 group, the timing of the onset of the ICT had no impact on growth response. In conclusion, ISS children with a DICT responded to standard GH dose (better responsiveness), whereas those with a normal ICT required higher doses to attain a significant height gain to FH.
Similar content being viewed by others
Log in or create a free account to read this content
Gain free access to this article, as well as selected content from this journal and more on nature.com
or
Abbreviations
- AGA:
-
appropriate for GA
- AITT:
-
arginine-insulin tolerance test
- DICT:
-
delayed infancy-childhood transition
- diffMPHSDS:
-
difference in child heightSDS versus midparental height (MPH)SDS
- FH:
-
final height
- GH33:
-
GH dose 33 μg/kg/d
- GH67:
-
GH dose 67 μg/kg/d
- GHD:
-
growth hormone deficiency
- GHmax:
-
maximum peak of GH
- ICP:
-
infancy-childhood-puberty
- ICT:
-
infancy-childhood-transition
- ISS:
-
idiopathic short stature
- IGFBP3:
-
insulin-like growth-factor-I-binding protein 3
- ITT:
-
intention-to-treat
- MPH:
-
midparental height
- non-DICT:
-
normal infancy-childhood-transition
- PP:
-
per-protocol
- SDS:
-
standard deviation score
- SGA:
-
small for GA
REFERENCES
Wit JM, Clayton PE, Rogol AD, Savage MO, Saenger PH, Cohen P 2008 Idiopathic short stature: definition, epidemiology, and diagnostic evaluation. Growth Horm IGF Res 18: 89–110
Hochberg Z, Albertsson-Wikland K 2008 Evo-devo of infantile and childhood growth. Pediatr Res 64: 2–7
Hochberg Z 2009 Evo-devo of child growth II: human life history and transition between its phases. Eur J Endocrinol 160: 135–141
Albertsson-Wikland K 1987 Clinical trial with authentic recombinant somatropin in Sweden and Finland. Acta Paediatr Scand Suppl 331: 28–34
Hintz RL, Attie KM, Baptista J, Roche A 1999 Effect of growth hormone treatment on adult height of children with idiopathic short stature. Genentech Collaborative Group. N Engl J Med 340: 502–507
Leschek EW, Rose SR, Yanovski JA, Troendle JF, Quigley CA, Chipman JJ, Crowe BJ, Ross JL, Cassorla FG, Blum WF, Cutler GB Jr, Baron J 2004 Effect of growth hormone treatment on adult height in peripubertal children with idiopathic short stature: a randomized, double-blind, placebo-controlled trial. J Clin Endocrinol Metab 89: 3140–3148
Wit JM, Rekers-Mombarg LT, Cutler GB, Crowe B, Beck TJ, Roberts K, Gill A, Chaussain JL, Frisch H, Yturriaga R, Attanasio AF 2005 Growth hormone (GH) treatment to final height in children with idiopathic short stature: evidence for a dose effect. J Pediatr 146: 45–53
Albertsson-Wikland K, Aronson AS, Gustafsson J, Hagenäs L, Ivarsson SA, Jonsson B, Kriström B, Marcus C, Nilsson KO, Ritzen EM, Tuvemo T, Westphal O, Åman J 2008 Dose-dependent effect of growth hormone on final height in children with short stature without growth hormone deficiency. J Clin Endocrinol Metab 93: 4342–4350
Albertsson-Wikland K, Kristrom B, Rosberg S, Svensson B, Nierop AF 2000 Validated multivariate models predicting the growth response to GH treatment in individual short children with a broad range in GH secretion capacities. Pediatr Res 48: 475–484
Dahlgren J, Kriström B, Niklasson A, Nierop AF, Rosberg S, Albertsson-Wikland K 2007 Models predicting the growth response to growth hormone treatment in short children independent of GH status, birth size and gestational age. BMC Med Inform Decis Mak 7: 40
Kriström B, Dahlgren J, Niklasson A, Nierop AF, Albertsson-Wikland K 2009 The first-year growth response to growth hormone treatment predicts the long-term prepubertal growth response in children. BMC Med Inform Decis Mak 9: 1
Kriström B, Löfqvist C, Rosberg S, Albertsson-Wikland K 2001 Effect of spontaneous GH secretion and the GH sampling period on the accuracy of models for predicting growth responses to GH treatment. J Clin Endocrinol Metab 86: 4963–4964
Kriström B, Aronson AS, Dahlgren J, Gustafsson J, Halldin M, Ivarsson SA, Nilsson NO, Svensson J, Tuvemo T, Albertsson-Wikland K 2009 Growth Hormone (GH) dosing during catch-up growth guided by individual responsiveness decreases growth response variability in prepubertal children with gh deficiency or idiopathic short stature. J Clin Endocrinol Metab 94: 483–490
Karlberg J, Albertsson-Wikland K 1988 Infancy growth pattern related to growth hormone deficiency. Acta Paediatr Scand 77: 385–391
Leger J, Noel M, Limal JM, Czernichow P 1996 Growth factors and intrauterine growth retardation. II. Serum growth hormone, insulin-like growth factor (IGF) I, and IGF-binding protein 3 levels in children with intrauterine growth retardation compared with normal control subjects: prospective study from birth to two years of age. Study Group of IUGR. Pediatr Res 40: 101–107
Albertsson-Wikland K, Luo ZC, Niklasson A, Karlberg J 2002 Swedish population-based longitudinal reference values from birth to 18 years of age for height, weight and head circumference. Acta Paediatr 91: 739–754
Karlberg J, Albertsson-Wikland K 1995 Growth in full-term small-for-gestational-age infants: from birth to final height. Pediatr Res 38: 733–739
Niklasson A, Ericson A, Fryer JG, Karlberg J, Lawrence C, Karlberg P 1991 An update of the Swedish reference standards for weight, length and head circumference at birth for given gestational age (1977–1981). Acta Paediatr Scand 80: 756–762
Clayton PE, Cianfarani S, Czernichow P, Johannsson G, Rapaport R, Rogol A 2007 Management of the child born small for gestational age through to adulthood: a consensus statement of the International Societies of Pediatric Endocrinology and the Growth Hormone Research Society. J Clin Endocrinol Metab 92: 804–810
Karlberg J 1989 On the construction of the infancy-childhood-puberty growth standard. Acta Paediatr Scand Suppl 356: 26–37
Liu YX, Albertsson-Wikland K, Karlberg J 2000 New reference for the age at childhood onset of growth and secular trend in the timing of puberty in Swedish. Acta Paediatr 89: 637–643
Xu X, Wang W, Guo Z, Karlberg J 2002 Longitudinal growth during infancy and childhood in children from Shanghai: predictors and consequences of the age at onset of the childhood phase of growth. Pediatr Res 51: 377–385
Luo ZC, Albertsson-Wikland K, Karlberg J 1998 Target height as predicted by parental heights in a population-based study. Pediatr Res 44: 563–571
Karlberg J, Luo ZC, Albertsson-Wikland K 2001 Body mass index reference values (mean and SD) for Swedish children. Acta Paediatr 90: 1427–1434
Albertsson-Wikland K, Rosberg S 1988 Analyses of 24-hour growth hormone profiles in children: relation to growth. J Clin Endocrinol Metab 67: 493–500
Jansson C, Boguszewski C, Rosberg S, Carlsson L, Albertsson-Wikland K 1997 Growth hormone (GH) assays: influence of standard preparations, GH isoforms, assay characteristics, and GH-binding protein. Clin Chem 43: 950–956
Löfqvist C, Andersson E, Gelander L, Rosberg S, Blum WF, Albertsson-Wikland K 2001 Reference values for IGF-I throughout childhood and adolescence: a model that accounts simultaneously for the effect of gender, age, and puberty. J Clin Endocrinol Metab 86: 5870–5876
Löfqvist C, Andersson E, Gelander L, Rosberg S, Hulthen L, Blum WF, Albertsson-Wikland K 2005 Reference values for IGF-I Binding Protein-3 (IGFBP-3) and the ratio of IGF-I to IGFBP-3 throughout childhood and adolescence. J Clin Endocrinol Metab 90: 1420–1427
Carlsson B, Ankarberg C, Rosberg S, Norjavaara E, Albertsson-Wikland K, Carlsson LM 1997 Serum leptin concentrations in relation to pubertal development. Arch Dis Child 77: 396–400
Acknowledgements
We thank the study group for allowing us to use the data for this analysis. The study group included Kerstin Albertsson-Wikland, A. Stefan Aronson, Jan Gustafsson, Lars Hagenäs, Sten A. Ivarsson, Berit Kriström, Claude Marcus, Karl Olof Nilsson, E. Martin Ritzén, Torsten Tuvemo, Otto Westphal, and Jan Åman.
Author information
Authors and Affiliations
Corresponding author
Additional information
This study TR 88-080 was initiated in 1988 as a Kabi-sponsored study and changed to an Investigator-sponsored study in the 1990s. The study was supported by grants from Swedish Research Council (7509) and Foundation Växthuset for Children.
An unrestricted research grant and free drug was kindly provided by Pharmacia/Pfizer. B.J. and B.K. have received a consultancy fee from Pfizer. Pfizer had no influence on collection, analyses, and interpretation of data or in writing of this manuscript.
Rights and permissions
About this article
Cite this article
Albertsson-Wikland, K., Kriström, B., Jonsson, B. et al. Long-Term Response to GH Therapy in Short Children With a Delayed Infancy-Childhood Transition (DICT). Pediatr Res 69, 504–510 (2011). https://doi.org/10.1203/PDR.0b013e3182139243
Received:
Accepted:
Issue date:
DOI: https://doi.org/10.1203/PDR.0b013e3182139243