Abstract
Background:
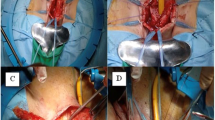
Congenital abnormalities vary in presentation, yet studies using model organisms tend to focus on occurrence rather than severity of the defect. Scoring severity of abnormalities in model systems allows explicit hypothesis testing during basic, translational, and reverse translational studies. We developed and validated a protocol to quantify severity of male urogenital feminization (hypospadias) in the mouse model. Hypospadias is one of the most common birth defects in the world.
Methods:
To induce genital feminization, pregnant mice were exposed to different concentrations of the antiandrogen vinclozolin. Genitalia were photographed at gestational age 18.5. A dichotomous scoring system to evaluate genital feminization was developed, and validated against histological measurements of urethral length. A training protocol was developed for novice scorers, and criteria were defined to evaluate precision and accuracy of scores.
Results:
Vinclozolin induced variation in hypospadias severity. Severity scores were tightly correlated with histologically determined urethral length and both techniques showed similar dose–response relationships. Novice observers were trained to precisely and accurately score hypospadias severity.
Conclusion:
This standardized scoring system advances the mouse as a model to study urogenital development, and will facilitate research on the mechanisms driving genital feminization in males, and aid translational hypospadias research.
Similar content being viewed by others
Log in or create a free account to read this content
Gain free access to this article, as well as selected content from this journal and more on nature.com
or
References
Cooper WJ, Albertson RC. Quantification and variation in experimental studies of morphogenesis. Dev Biol 2008;321:295–302.
Bergman Å, Heindel JJ, Jobling S, Kidd KA, Zoeller RT. State of the science of endocrine disrupting chemicals - 2012. WHO 2012:63–8.
Kalfa N, Liu B, Klein O, et al. Mutations of CXorf6 are associated with a range of severities of hypospadias. Eur J Endocrinol 2008;159:453–8.
Manzoni G, Bracka A, Palminteri E, Marrocco G. Hypospadias surgery: when, what and by whom? BJU Int 2004;94:1188–95.
van der Toorn F, de Jong TP, de Gier RP, et al. Introducing the HOPE (Hypospadias Objective Penile Evaluation)-score: a validation study of an objective scoring system for evaluating cosmetic appearance in hypospadias patients. J Pediatr Urol 2013;9(6 Pt B):1006–16.
Cunha GR, Sinclair A, Risbridger G, Hutson J, Baskin LS. Current understanding of hypospadias: relevance of animal models. Nat Rev Urol 2015;12:271–80.
Yang JH, Menshenina J, Cunha GR, Place N, Baskin LS. Morphology of mouse external genitalia: implications for a role of estrogen in sexual dimorphism of the mouse genital tubercle. J Urol 2010;184(4 Suppl):1604–9.
Buckley J, Willingham E, Agras K, Baskin LS. Embryonic exposure to the fungicide vinclozolin causes virilization of females and alteration of progesterone receptor expression in vivo: an experimental study in mice. Environ Health 2006;5:4.
Rider CV, Furr J, Wilson VS, Gray LE Jr . A mixture of seven antiandrogens induces reproductive malformations in rats. Int J Androl 2008;31:249–62.
Rocheleau CM, Romitti PA, Dennis LK. Pesticides and hypospadias: a meta-analysis. J Pediatr Urol 2009;5:17–24.
Kim KS, Torres CR Jr, Yucel S, Raimondo K, Cunha GR, Baskin LS. Induction of hypospadias in a murine model by maternal exposure to synthetic estrogens. Environ Res 2004;94:267–75.
Silversides DW, Price CA, Cooke GM. Effects of short-term exposure to hydroxyflutamide in utero on the development of the reproductive tract in male mice. Can J Physiol Pharmacol 1995;73:1582–8.
Khoury MJ, Gwinn M, Yoon PW, Dowling N, Moore CA, Bradley L. The continuum of translation research in genomic medicine: how can we accelerate the appropriate integration of human genome discoveries into health care and disease prevention? Genet Med 2007;9:665–74.
van der Zanden LF, van Rooij IA, Feitz WF, Franke B, Knoers NV, Roeleveld N. Aetiology of hypospadias: a systematic review of genes and environment. Hum Reprod Update 2012;18:260–83.
Carmichael SL, Mohammed N, Ma C, et al. Diacylglycerol kinase K variants impact hypospadias in a California study population. J Urol 2013;189:305–11.
Ogata T, Laporte J, Fukami M. MAMLD1 (CXorf6): a new gene involved in hypospadias. Horm Res 2009;71:245–52.
Czeizel AE. The primary prevention of birth defects: multivitamins or folic acid? Int J Med Sci 2004;1:50–61.
Mavrogenis S, Urban R, Czeizel AE, Ács N. Possible preventive effect of high doses of folic acid for isolated hypospadias: a national population-based case-control study. Am J Med Genet A 2014;164A:3108–14.
Ormond G, Nieuwenhuijsen MJ, Nelson P, et al. Endocrine disruptors in the workplace, hair spray, folate supplementation, and risk of hypospadias: case-control study. Environ Health Perspect 2009;117:303–7.
Kelce WR, Monosson E, Gamcsik MP, Laws SC, Gray LE Jr. Environmental hormone disruptors: evidence that vinclozolin developmental toxicity is mediated by antiandrogenic metabolites. Toxicol Appl Pharmacol 1994;126:276–85.
Vilela ML, Willingham E, Buckley J, et al. Endocrine disruptors and hypospadias: role of genistein and the fungicide vinclozolin. Urology 2007;70:618–21.
Theiler K. The house mouse- Atlas of embryonic development: Springer; 1989.
Lleonart J, Salat J, Torres GJ. Removing allometric effects of body size in morphological analysis. J Theor Biol 2000;205:85–93.
Bates D, Machler M, Bolker BMM, and Walker SC. Fitting linear mixed-effects models using lme4. R News 2005:27–30.
Fox J. Effect displays in R for generalised linear models. J Stat Softw 2003;8:1–19.
Acknowledgements
We thank J. Kelly and B. Blake for recording detailed notes and participating in the training protocol and A. Helms for providing helpful comments and edits. We would also like to thank M. McCoy for help with project development and data analysis.
Author information
Authors and Affiliations
Corresponding author
Supplementary information
Supplementary Figure S1
(TIFF 10956 kb)
Supplementary Methods
(DOCX 24 kb)
Rights and permissions
About this article
Cite this article
Amato, C., McCoy, K. A validated protocol to quantify severity of male urogenital feminization using the MOUSE (Mouse objective urethral severity evaluation). Pediatr Res 80, 880–885 (2016). https://doi.org/10.1038/pr.2016.157
Received:
Accepted:
Published:
Issue date:
DOI: https://doi.org/10.1038/pr.2016.157