Abstract
Background
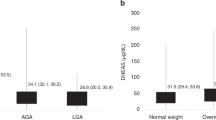
Children born small for gestational age (SGA) have higher serum dehydroepiandrosterone sulfate (DHEAS) concentrations than children born appropriate for gestational age (AGA). The overall metabolic risk associated with birth weight is U-shaped, but it is not known whether children born large for gestational age (LGA) have elevated serum DHEAS levels.
Methods
A cohort of 49 children born LGA, 56 children born AGA, and 23 children born SGA were studied at 5–8 years of age. Anthropometric data at birth, at the age of 2 years, and at examination were recorded. Fasting blood samples were collected for serum analyses of DHEAS, insulin-like growth factor 1 (IGF-1), and insulin concentrations.
Results
The children born LGA had lower serum DHEAS levels adjusted for body mass index (BMI) standard deviation score (SDS) and age than the rest of the children. Lower birth weight SDS and higher weight gain during the first 2 years of life predicted higher serum DHEAS levels. Higher serum IGF-1 levels were also associated with higher prevalence of adrenarchal DHEAS levels.
Conclusion
Being born LGA was associated with lower DHEAS levels, whereas small birth size and early catch-up growth predicted higher levels. This suggests that genetic or early epigenetic factors have an impact on adrenarche. IGF-1 may be a mediator in this process.
Similar content being viewed by others
Log in or create a free account to read this content
Gain free access to this article, as well as selected content from this journal and more on nature.com
or
References
Tenhola S, Martikainen A, Rahiala E, Parviainen M, Halonen P, Voutilainen R . Increased adrenocortical and adrenomedullary hormonal activity in 12-year-old children born small for gestational age. J Pediatr 2002;141:477–82.
Ibáñez L, Lopez-Bermejo A, Díaz M, Suárez L, de Zegher F . Low-birth weight children develop lower sex hormone binding globulin and higher dehydroepiandrosterone sulfate levels and aggravate their visceral adiposity and hypoadiponectinemia between six and eight years of age. J Clin Endocrinol Metab 2009;94:3696–9.
Idkowiak J, Lavery GG, Dhir V et al, Premature adrenarche: novel lessons from early onset androgen excess. Eur J Endocrinol 2011;165:189–207.
Voutilainen R, Jääskeläinen J . Premature adrenarche: etiology, clinical findings, and consequences. J Steroid Biochem Mol Biol 2015;145:226–36.
Utriainen P, Laakso S, Liimatta J, Jääskeläinen J, Voutilainen R . Premature adrenarche—a common condition with variable presentation. Horm Res Paediatr 2015;83:221–31.
Oppenheimer E, Linder B, DiMartino-Nardi J . Decreased insulin sensitivity in prepubertal girls with premature adrenarche and acanthosis nigricans. J Clin Endocrinol Metab 1995;80:614–8.
Utriainen P, Jääskeläinen J, Romppanen J, Voutilainen R . Childhood metabolic syndrome and its components in premature adrenarche. J Clin Endocrinol Metab 2007;92:4282–5.
Ibáñez L, Potau N, Chacon P, Pascual C, Carrascosa A . Hyperinsulinaemia, dyslipaemia and cardiovascular risk in girls with a history of premature pubarche. Diabetologia 1998;41:1057–63.
Utriainen P, Jääskeläinen J, Saarinen A, Vanninen E, Mäkitie O, Voutilainen R . Body composition and bone mineral density in children with premature adrenarche and the association of LRP5 gene polymorphisms with bone mineral density. J Clin Endocrinol Metab 2009;94:4144–51.
Harder T, Rodekamp E, Schellong K, Dudenhausen JW, Plagemann A . Birth weight and subsequent risk of type 2 diabetes: a meta-analysis. Am J Epidemiol 2007;165:849–57.
Whincup PH, Kaye SJ, Owen CG et al, Birth weight and risk of type 2 diabetes: a systematic review. JAMA 2008;300:2886–97.
Saenger P, Czernichow P, Hughes I, Reiter EO . Small for gestational age: short stature and beyond. Endocr Rev 2007;28:219–51.
Evagelidou EN, Giapros VI, Challa AS et al, Prothrombotic state, cardiovascular, and metabolic syndrome risk factors in prepubertal children born large for gestational age. Diabetes Care 2010;33:2468–70.
Bowers K, Liu G, Wang P et al, Birth weight, postnatal weight change, and risk for high blood pressure among Chinese children. Pediatrics 2011;127:e1272–9.
Taal HR, Vd Heijden AJ, Steegers EA, Hofman A, Jaddoe VW . Small and large size for gestational age at birth, infant growth, and childhood overweight. Obesity 2013;21:1261–8.
Johnsson IW, Haglund B, Ahlsson F, Gustafsson J . A high birth weight is associated with increased risk of type 2 diabetes and obesity. Pediatr Obes 2015;10:77–83.
Neville KA, Walker JL . Precocious pubarche is associated with SGA, prematurity, weight gain, and obesity. Arch Dis Child 2005;90:258–61.
Pere A, Perheentupa J, Peter M, Voutilainen R . Follow up of growth and steroids in premature adrenarche. Eur J Pediatr 1995;154:346–52.
Utriainen P, Voutilainen R, Jääskeläinen J . Girls with premature adrenarche have accelerated early childhood growth. J Pediatr 2009;154:882–7.
Ong KK, Potau N, Petry CJ et al, Opposing influences of prenatal and postnatal weight gain on adrenarche in normal boys and girls. J Clin Endocrinol Metab 2004;89:2647–51.
Nordman H, Voutilainen R, Laitinen T et al, Growth and cardiovascular risk factors in prepubertal children born large or small for gestational age. Horm Res Paediatr 2016;85:11–17.
Saari A, Sankilampi U, Hannila ML, Kiviniemi V, Kesseli K, Dunkel L . New Finnish growth references for children and adolescents aged 0 to 20 years: length/height-for-age, weight-for-length/height, and body mass index-for-age. Ann Med 2011;43:235–48.
Monteiro PO, Victora CG . Rapid growth in infancy and childhood and obesity in later life-a systematic review. Obes Rev 2005;6:143–54.
Mäntyselkä A, Jääskeläinen J, Lindi V et al, The presentation of adrenarche is sexually dimorphic and modified by body adiposity. J Clin Endocrinol Metab 2014;99:3889–3894.
Utriainen P, Voutilainen R, Jääskeläinen J . Continuum of phenotypes and sympathoadrenal function in premature adrenarche. Eur J Endocrinol 2009;160:657–665.
Schulte S, Wölfle J, Schreiner F et al, Birthweight differences in monozygotic twins influence pubertal maturation and near final height. J Pediatr 2016;170:288–94. e1–2.
Denburg MR, Silfen ME, Manibo AM et al, Insulin sensitivity and the insulin-like growth factor system in prepubertal boys with premature adrenarche. J Clin Endocrinol Metab 2002;87:5604–5609.
Corvalán C, Uauy R, Mericq V . Obesity is positively associated with dehydroepiandrosterone sulfate concentrations at 7 y in Chilean children of normal birth weight. Am J Clin Nutr 2013;97:318–325.
Silfen ME, Manibo AM, Ferin M, McMahon DJ, Levine LS, Oberfield SE . Elevated free IGF-I levels in prepubertal Hispanic girls with premature adrenarche: relationship with hyperandrogenism and insulin sensitivity. J Clin Endocrinol Metab 2002;87:398–403.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Nordman, H., Voutilainen, R., Antikainen, L. et al. Prepubertal children born large for gestational age have lower serum DHEAS concentrations than those with a lower birth weight. Pediatr Res 82, 285–289 (2017). https://doi.org/10.1038/pr.2017.44
Received:
Accepted:
Published:
Issue date:
DOI: https://doi.org/10.1038/pr.2017.44
This article is cited by
-
Association between being large for gestational age and cardiovascular metabolic health in children conceived from assisted reproductive technology: a prospective cohort study
BMC Medicine (2024)
-
Association of dehydroepiandrosterone sulfate, birth size, adiposity and cardiometabolic risk factors in 7-year-old children
Pediatric Research (2022)
-
Prenatal salivary sex hormone levels and birth-weight-for-gestational age
Journal of Perinatology (2019)
-
Birth size, body composition, and adrenal androgens as determinants of bone mineral density in mid-childhood
Pediatric Research (2018)