Abstract
Background/Objectives
Human studies suggest that fathers with obesity influence infant growth and development. This study aimed to evaluate the relationship between paternal body mass index (BMI) and waist circumference (WC) with neonatal anthropometry and adiposity.
Methods
This study is a cohort nested in a randomized controlled clinical trial of nutritional counseling for pregnant women with overweight. In total, 89 partner-pregnant woman-neonate triads were included. Paternal anthropometric measurements were taken at the time of the interview. Secondary data related to birth were obtained through access to the health information systems. Neonatal skinfold thickness was assessed and the adiposity was estimated using a predictive anthropometric model. Pearson’s correlation and adjusted multivariate linear regression models were employed to evaluate the relationship between paternal BMI and WC with neonatal anthropometric measurements and adiposity.
Results
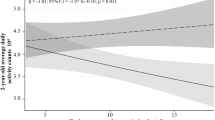
In total, 57.0% of the fathers presented a BMI ≥ 25 kg/m² and 14.6% a waist circumference ≥102 cm. The mean ± SD birth weight of the newborns (g) was 3357 ± 538. Paternal BMI and WC were inversely correlated with head circumference at birth [r = −0.31 (p = 0.004), r = −0.23 (p = 0.03), respectively]. Paternal BMI was also inversely correlated with the birth weight standardized by gestational age (z-score) [r = −0.23 (p = 0.03)]. In adjusted multivariate linear regression models, the paternal BMI (kg/m²) was inversely associated with the head circumference at birth (cm) [β = −0.07 (95% CI −0.15; −0.001) p = 0.04].
Conclusion
The data suggest that paternal excessive weight have a negative effect on fetal development, as assessed by anthropometric measurements. The inverse association between paternal BMI and the head circumference at birth was independent of confounders. Future studies with larger sample sizes are necessary to confirm or refute such hypotheses.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
Data availability
To request access conditional on approval from the appropriate institutional ethics and data owners, please email daniss@fmrp.usp.br.
References
Fullston T, Teague EMCO, Palmer NO, Deblasio MJ, Mitchell M, Corbett M, et al. Paternal obesity initiates metabolic disturbances in two generations of mice with incomplete penetrance to the F2 generation and alters the transcriptional profile of testis and sperm microRNA content. FASEB J. 2013;27:4226–43.
Ng SF, Lin RCY, Laybutt DR, Barres R, Owens JA, Morris MJ. Chronic high-fat diet in fathers programs β 2-cell dysfunction in female rat offspring. Nature. 2010;467:963–6.
Soubry A. Epigenetic inheritance and evolution: a paternal perspective on dietary influences. Prog Biophys Mol Biol. 2015;118:79–85.
Soubry A. POHaD: why we should study future fathers. Environ Epigenet. 2018;4:1–7.
Silveira PP, Portella AK, Goldani MZ, Barbieri MA. Origens desenvolvimentistas da saúde e da doença (DOHaD). J Pediatr. 2007;83:494–504.
Ornellas F, Carapeto PV, Mandarim-de-Lacerda CA, Aguila MB. Obese fathers lead to an altered metabolism and obesity in their children in adulthood: review of experimental and human studies. J Pediatr. 2017;93:551–9.
Dodd JM, Du Plessis LE, Deussen AR, Grivell RM, Yelland LN, Louise J, et al. Paternal obesity modifies the effect of an antenatal lifestyle intervention in women who are overweight or obese on newborn anthropometry. Sci Rep. 2017;7:3–11.
Chia AR, Tint MT, Han CY, Chen LW, Colega M, Aris IM, et al. Adherence to a healthy eating index for pregnant women is associated with lower neonatal adiposity in a multiethnic Asian cohort: the Growing Up in Singapore Towards healthy Outcomes (GUSTO) Study. Am J Clin Nutr. 2018;107:71–9.
Matthews EK, Wei J, Cunningham SA. Relationship between prenatal growth, postnatal growth and childhood obesity: a review. Eur J Clin Nutr. 2017;71:919–30.
Rallis D, Balomenou F, Tzoufi M, Giapros V. A systematic review indicates an association between birth weight and body fat in childhood. Acta Paediatr. 2021;110:2023–39.
Hillman S, Peebles DM, Williams DJ. Paternal metabolic and cardiovascular risk factors for fetal growth restriction: a case-control study. Diabetes Care. 2013;36:1675.
Liu B, Khalil A. Fetal growth restriction. In: Twin higher-order pregnancies. 2023. pp. 189–204 (Cham: Springer International Publishing).
Pomeroy E, Wells JCK, Cole TJ, O’Callaghan M, Stock JT. Relationships of maternal and paternal anthropometry with neonatal body size, proportions and adiposity in an Australian cohort. Am J Phys Anthropol. 2015;156:625–36.
Sun M, Zhang S, Chen L, Li Y, Diao J, Li J. et al. Association between paternal pre-pregnancy body mass index with preterm birth and low birth weight. Front Pediatr. 2022;10:955544.
Craig JR, Jenkins TG, Carrell DT, Hotaling JM. Obesity, male infertility, and the sperm epigenome. Fertil Steril. 2017;107:848–59. https://doi.org/10.1016/j.fertnstert.2017.02.115.
Monteiro CA, Cannon G, Moubarac JC, Levy RB, Louzada MLC, Jaime PC. The UN Decade of Nutrition, the NOVA food classification and the trouble with ultra-processing. Public Health Nutr. 2018;21:5–17.
Harris PA, Taylor R, Thielke R, Payne J, Gonzalez N, Conde JG. Research electronic data capture (REDCap)—a metadata-driven methodology and workflow process for providing translational research informatics support. J Biomed Inf. 2009;42:377–81. https://doi.org/10.1016/j.jbi.2008.08.010.
Sartorelli DS, Crivellenti LC, Baroni NF, de Andrade Miranda DEG, da Silva Santos I, Carvalho MR, et al. Effectiveness of a minimally processed food-based nutritional counselling intervention on weight gain in overweight pregnant women: a randomized controlled trial. Eur J Nutr. 2023;62:443.
Baroni NF, Carvalho MR, da Silva Santos I, Chaves AVL, de Andrade Miranda DEG, Crivellenti LC, et al. Effect of a lifestyle intervention among pregnant women with overweight on neonatal adiposity: a randomized controlled clinical trial. Early Hum Dev. 2024;194:106038. https://doi.org/10.1016/j.earlhumdev.2024.106038.
Fo L, Paulo S. Seqüência básica na elaboração de protocolos de pesquisa. Arq Bras Cardiol. 1998;71:735–40. https://www.scielo.br/j/abc/a/nGZdPqsrpXJjDqCmmwbLDmJ/?lang=pt.
Kang H. Sample size determination and power analysis using the G*Power software. J Educ Eval Health. 2021;18:17. https://doi.org/10.3352/jeehp.2021.18.17.
Ministério da Saúde. VIGITEL Brasil 2019: Vigilância de Fatores de Risco para Doenças Cronicas por Inquérito Telefônico. Vigitel Brasil 2019: vigilância de fatores de risco e proteção para doenças crônicas por inquérito telefônico: estimativas sobre frequência e distribuição sociodemográfica de fatores de risco e proteção para doenças crônicas nas capitais dos 26 estados. 2020. p. 139.
Monteiro CA, Moura EC, Jaime PC, Claro RM. Validade de indicadores do consumo de alimentos e bebidas obtidos por inquérito telefônico. Rev Saude Publica. 2008;42:582–9.
Brasil. Guia de Atividade Física para a População Brasileira. Vol. 26, Ministério da Saúde, Secretaria de Atenção Primária à Saúde, Departamento de Promoção da Saúde. Brasília: Ministério da Saúde; 2021. pp. 1–54. https://bvsms.saude.gov.br/bvs/publicacoes/guia_atividade_fisica_populacao_brasileira.pdf.
ABEP. Alterações na aplicação do Critério Brasil. Abep. 2018;1:1–5. https://www.abep.org/criterio-brasil.
Sociedade Brasileira de Cardiologia. Diagnóstico e tratamento. Arq Bras Cardiol. 2005;84:1–27.
Villar J, Altman DG, Purwar M, Noble JA, Knight HE, Ruyan P, et al. The objectives, design and implementation of the INTERGROWTH-21 st Project. BJOG Int J Obstet Gynaecol. 2013;120:9–26.
Sociedade Brasileira de Pediatria. Avaliação nutricional da criança e do adolescente: manual de orientações. Dep Nutrologia. 2009:21–105.
Slaughter MH, Lohman TG, Boileau RA. Relationship of anthropometric dimensions to lean body mass in children. Ann Hum Biol. 2009;5:469–82. https://doi.org/10.1080/03014467800003121.
Slaughter MH, Lohman TG, Boileau RA, Stillman RJ, Van Loan M, Horswill CA, et al. Influence of maturation on relationship of skinfolds to body density: a cross-sectional study. Hum Biol. 1984;56:681–9.
Deierlein AL, Thornton J, Hull H, Paley C, Gallagher D. An anthropometric model to estimate neonatal fat mass using air displacement plethysmography. Nutr Metab. 2012;9:1–5.
Textor J, Hardt J. DAGitty: a graphical tool for analyzing causal diagrams. Epidemiology. 2011;22:745.
Tennant PWG, Murray EJ, Arnold KF, Berrie L, Fox MP, Gadd SC, et al. Use of directed acyclic graphs (DAGs) to identify confounders in applied health research: review and recommendations. Int J Epidemiol. 2021;50:620–32.
McCowan LME, North RA, Kho EM, Black MA, Chan EH, Dekker GA, et al. Paternal contribution to small for gestational age babies: a multicenter prospective study. Obesity. 2011;19:1035–9.
S‚l‚nou C, Brioude F, Giabicani E, Sobrier ML, Netchine I. IGF2: development, genetic and epigenetic abnormalities. Cells. 2022;11:1886.
Ishida M, Ohashi S, Kizaki Y, Naito JI, Horiguchi K, Harigaya T. Expression profiling of mouse placental lactogen II and its correlative genes using a cDNA microarray analysis in the developmental mouse placenta. J Reprod Dev. 2007;53:69–76.
Coan PM, Fowden AL, Constancia M, Ferguson-Smith AC, Burton GJ, Sibley CP. Disproportional effects of Igf2 knockout on placental morphology and diffusional exchange characteristics in the mouse. J Physiol. 2008;586:5023–32.
Dupont C, Faure C, Sermondade N, Boubaya M, Eustache F, Clément P, et al. Obesity leads to higher risk of sperm DNA damage in infertile patients. Asian J Androl. 2013;15:622–5.
H†konsen L, Thulstrup A, Aggerholm A, Olsen J, Bonde J, Andersen C. et al. Does weight loss improve semen quality and reproductive hormones? Results from a cohort of severely obese men. Reprod Health. 2011;8:24.
D’Agostin M, Di Sipio Morgia C, Vento G, Nobile S. Long-term implications of fetal growth restriction. World J Clin Cases. 2023;11:2855–63.
Lindsay RS, Dabelea D, Roumain J, Hanson RL, Bennett PH, Knowler WC. Type 2 diabetes and low birth weight: the role of paternal inheritance in the association of low birth weight and diabetes. Diabetes. 2000;49:445–9.
Hyppönen E, Davey Smith G, Power C. Parental diabetes and birth weight of offspring: intergenerational cohort study. Br Med J. 2003;326:19.
Wannamethee SG, Lawlor DA, Whincup PH, Walker M, Ebrahim S, Davey-Smith G. Birthweight of offspring and paternal insulin resistance and paternal diabetes in late adulthood: cross sectional survey. Diabetologia. 2004;47:12–8.
Nahum GG, Stanislaw H. Relationship of paternal factors with birth weight. J Reprod Med. 2003;48:963–8. https://doi.org/10.1038/s41588-019-0403-1.
Kaikkonen JE, Mikkilä V, Juonala M, Keltikangas-Järvinen L, Hintsanen M, Pulkki-Råback L, et al. Factors associated with six-year weight change in young and middle-aged adults in the Young Finns Study. Scand J Clin Lab Invest. 2015;75:133–44. https://doi.org/10.3109/00365513.2014.992945.
Wiechers C, Kirchhof S, Maas C, Poets CF, Franz AR. Neonatal body composition by air displacement plethysmography in healthy term singletons: a systematic review. BMC Pediatr. 2019;19:489.
Demerath EW, Fields DA. Body composition assessment in the infant. Am J Hum Biol. 2014;26:291.
Tokhi M, Comrie-Thomson L, Davis J, Portela A, Chersich M, Luchters S. Involving men to improve maternal and newborn health: a systematic review of the effectiveness of interventions. PLoS ONE. 2018;13:1–16.
Brasil. Ministério da Saúde. Secretaria de Atenção à Saúde. Departamento de Ações Programáticas Estratégicas. Guia do pré-natal do parceiro para profissionais de Saúde. 2018;56. https://bvsms.saude.gov.br/bvs/publicacoes/guia_pre_natal_profissionais_saude_1ed.pdf.
Funding
This work was supported by the São Paulo Research Foundation (FAPESP 2017/15386–2, 2017/18980–2, 2021/06586-3, and 2021/06486-9), the National Council for Scientific and Technological Development (CNPq 406000/2018–2 and 302487/2018–2), the Coordination for the Improvement of Higher Education Personnel (CAPES) and the Foundation for Support to Teaching, Research and Assistance of the Clinical Hospital, Ribeirão Preto Medical School, University of São Paulo (FAEPA 1039/2018, 1114/2018, 61/2019, 62/2019 and 754/2021). The funders had no role in the study design, data collection, analysis, decision to publish, or preparation of the manuscript.
Author information
Authors and Affiliations
Contributions
MRC: conceptualization, methodology, data curation, statistical analysis, and roles/writing—original draft. DEGAM: conceptualization, methodology, and data curation. NFB: conceptualization, methodology, and data curation. ISS: investigation. NPC: data analysis, and writing—review & editing. LCC: conceptualization, methodology, and investigation. DSS: conceptualization, methodology, data curation, supervision, project administration, funding acquisition and writing—review & editing.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethical approval
This study was conducted in accordance with the guidelines of the Declaration of Helsinki and its execution was authorized by the Municipal Health Department of Ribeirão Preto and approved by the Research Ethics Committee of the School Health Center of the Ribeirão Preto School of Medicine University of São Paulo (96680318.5.0000.5414). It was also registered in the Brazilian Clinical Trials Registry (REBEC) under protocol RBR-5jy777. Written consent was obtained from all participants.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Carvalho, M.R., Miranda, D.E.G.d.A., Baroni, N.F. et al. Relationship between paternal excessive weight and neonatal anthropometry in a clinical trial of nutritional counseling for pregnant women with overweight. Int J Obes 48, 1831–1838 (2024). https://doi.org/10.1038/s41366-024-01639-8
Received:
Revised:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41366-024-01639-8