Abstract
Background/Objective
Limited studies have examined the effects of meals containing processed foods or ultra-processed foods (UPF) on appetite regulation and results were inconsistent and difficult to generalize. Therefore, the study aimed to evaluate the potential efficacy of two different breakfasts containing processed foods or UPF on postprandial appetite regulation in adults with different body mass index (BMI).
Methods
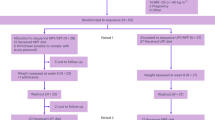
Twenty-eight participants (eighteen with normal BMI (BMI: 18.50–24.99 kg/m2), ten with high BMI (BMI > 25.0 kg/m2) were included in the study. General demographic information form, food consumption records, and Screening Questionnaire of Highly Processed Food Consumption (sQ-HPF) were applied and anthropometric measurements (body weight, height, waist circumference, waist/hip ratio and waist/height ratio) were taken. Participants made two visits, 2 weeks apart, and were offered two different breakfasts: Processed Breakfast and UPF Breakfast. Blood samples were collected before starting the meal (0 min) and 30, 60, 90, and 120 min after taking the first bite, and serum glucose, insulin, amylin, GLP-1, and GIP levels were analyzed using ELISA/colorimetric methods. Also, participants were administrated a visual analogue scale (VAS) to subjectively assess appetite regulation at the same times.
Results
Daily energy, macro and micronutrients consumption were similar across BMI groups for both breakfast in prior the experiment and throughout the rest of the experimental day (p > 0.05). The total area under the curve (tAUC) for hunger sensation and insulin were higher after the UPF Breakfast compared to the Processed Breakfast (p = 0.009, p = 0.016, respectively). Other data were no different both between breakfast types and different BMI groups.
Conclusion
Overall, while short-term appetite hormone responses to UPF Breakfast and Processed Breakfasts were similar, higher insulin levels and subjective feelings of hunger, following UPF Breakfast independent of BMI status. These findings suggest that the degree of food processing, rather than BMI, may influence specific aspects of postprandial appetite regulation.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
Data availability
Data will be made available by the authors upon reasonable request.
References
World Health Organization. Obesity and overweight. 2024; Available from: https://www.who.int/news-room/fact-sheets/detail/obesity-and-overweight.
The Obesity Society. International Obesity Collaborative (IOC) Consensus Statement Obesity Care vs. Weight-Loss. 2025. Available from: https://www.obesity.org/international-obesity-collaborative/.
Stroebe W. Is the energy balance explanation of the obesity epidemic wrong?. Appetite. 2023;188:106614.
Longo S, Rizza S, Federic M. Microbiota-gut-brain axis: relationships among the vagus nerve, gut microbiota, obesity, and diabetes. Acta Diabetol. 2023;60:1007–17.
Campos A, Port JD, Acosta A. Integrative Hedonic and Homeostatic Food Intake Regulation by the Central Nervous System: Insights from Neuroimaging. Brain Sci. 2022;12:431.
Page AJ. Gastrointestinal Vagal Afferents and Food Intake: Relevance of Circadian Rhythms. Nutrients. 2021;13:844.
van Meer F, van der Laan LN, Eiben G, Lissner L, Wolters M, Rach S, et al. Age and body mass index are associated with dorsolateral prefrontal cortex activation in response to unhealthy food cues. Appetite. 2025;213:108138.
Dicken S, Makaronidis J, van Tulleken C, Jassil FC, Hall K, Brown AC, et al. UPDATE trial: investigating the effects of ultra-processed versus minimally processed diets following UK dietary guidance on health outcomes: a protocol for an 8-week community-based cross-over randomised controlled trial in people with overweight or obesity, followed by a 6-month behavioural intervention. BMJ Open. 2024;14:e079027.
Horner KM, Mullen B, Quinn A, Scheufele P, Gola S, Gonnelli F, et al. Plant protein, fibre and physical activity solutions to address poor appetite and prevent undernutrition in older adults: study protocol for the appetite randomised controlled trial. Br J Nutr. 2024;132:823–34.
Kalam F, Gabel K, Cienfuegos S, Wiseman E, Ezpeleta M, Pavlou V, et al. Changes in subjective measures of appetite during 6 months of alternate day fasting with a low carbohydrate diet. Clin Nutr ESPEN. 2021;41:417–22.
Elizabeth L, Machado P, Zinöcker M, Baker P, Lawrence M. Ultra-processed foods and health outcomes: a narrative review. Nutrients. 2020;12:1955.
Mirmiran P, Moslehi N, Golzarand M, Azizi F. Ultra-processed foods consumption and the risk of metabolically unhealthy phenotype in normal-weight and overweight/obese adults: a prospective investigation. Int J Food Sci Nutr. 2023;74:522–31.
Ulug E, Acikgoz Pinar A, Yildiz BO. Impact of ultra-processed foods on hedonic and homeostatic appetite regulation: A systematic review. Appetite. 2025;213:108139.
Monteiro CA, Cannon G, Levy RB, Moubarac JC, Louzada ML, Rauber F, et al. Ultra-processed foods: what they are and how to identify them. Public Health Nutr. 2019;22:936–41.
Monteiro CA, Cannon G, Moubarac JC, Levy RB, Louzada MLC, Jaime PC, et al. The UN Decade of Nutrition, the NOVA food classification and the trouble with ultra-processing. Public Health Nutr. 2018;21:5–17.
Monteiro CA, Cannon G, Levy R, Moubarac JC, Jaime P, Martins AP, et al. NOVA. The star shines bright. World Nutr. 2016;7:28–38.
Meine GC, et al. Ultra-Processed Food Consumption and Gastrointestinal Cancer Risk: A Systematic Review and Meta-Analysis. Am J Gastroenterol. 2024;119:1056–65.
Meine GC, Picon RV, Santo PAE, Sander GB. Ultra-processed food consumption and adult obesity risk: a systematic review and dose-response meta-analysis. Crit Rev Food Sci Nutr. 2023;63:249–60.
Coricelli C, Toepel U, Notter ML, Murray MM, Rumiati RI. Distinct brain representations of processed and unprocessed foods. Eur J Neurosci. 2019;50:3389–401.
Cummings JR, Schiestl ET, Tomiyama AJ, Mamtora T, Gearhardt AN. Highly processed food intake and immediate and future emotions in everyday life. Appetite. 2022;169:105868.
Reynolds AN, Pham HTD, Åberg S, Neumann S, Mann J. The effects of wholegrain processing on appetite: randomised crossover trial in adults with type 2 diabetes. Food Funct. 2023;14:7240–6.
Hafiz MS, Campbell MD, Orsi NM, Mappa G, Orfila C, Boesch C. Impact of food processing on postprandial glycaemic and appetite responses in healthy adults: a randomized, controlled trial. Food Funct. 2022;13:1280–90.
Hall KD, Ayuketah A, Brychta R, Cai H, Cassimatis T, Chen KY, et al. Ultra-processed diets cause excess calorie intake and weight gain: an inpatient randomized controlled trial of ad libitum food intake. Cell Metab. 2019;30:67–77.e3.
Böhm A, Heitmann BL. The use of bioelectrical impedance analysis for body composition in epidemiological studies. Eur J Clin Nutr. 2013;67:S79–85.
WHO Expert Consultation. Waist circumference and waist-hip ratio. Report of a WHO Expert Consultation. Geneva: World Health Organization; 2008. p. 8–11.
Gunes FE, Imeryuz N, Akalin A, Bekiroglu N, Alphan E, Oguz A, et al. Development and validation of a semi-quantitative food frequency questionnaire to assess dietary intake in Turkish adults. JPMA. 2015;65:756–63.
Neslişah R, Emine AY. Energy and nutrient intake and food patterns among Turkish university students. Nutr Res Pr. 2011;5:117–23.
Martinez-Perez C, Daimiel L, Climent-Mainar C, Martínez-González MÁ, Salas-Salvadó J, Corella D, et al. Integrative development of a short screening questionnaire of highly processed food consumption (sQ-HPF). Int J Behav Nutr Phys Act. 2022;19:6.
Erdoğan Gövez N, Köksal E, Martinez-Perez C, Daimiel L. Validity and Reliability of the Turkish Version of the Screening Questionnaire of Highly Processed Food Consumption (sQ-HPF). Nutrients. 2024;16:2552.
Ahmed A, Imran A, R. Wei C, Nadeem R, Shankar A, Balaji J, et al. Contribution of ultra-processed foods to increased obesity and non-communicable diseases. Cogent Food Agric. 2024;10:2438405.
Hamano S, Sawada M, Aihara M, Sakurai Y, Sekine R, Usami S, et al. Ultra-processed foods cause weight gain and increased energy intake associated with reduced chewing frequency: A randomized, open-label, crossover study. Diab Obes Metab. 2024;26:5431–43.
Gibney MJ. Ultra-processed foods: definitions and policy issues. Curr Dev Nutr. 2019;3:nzy077.
Blundell J, De Graaf C, Hulshof T, Jebb S, Livingstone B, Lluch A, et al. Appetite control: methodological aspects of the evaluation of foods. Obes Rev. 2010;11:251–70.
Blundell JE, Rogers PJ, Hill AJ. Evaluating the satiating power of foods: implications for acceptance and consumption. In: Colms J, Booth DA, Pangborn RM, Raunhardt O (eds). Food acceptance and nutrition, 1987. pp 205–19.
Galdino-Silva MB, Almeida KMM, Oliveira ADSD, Santos JVLD, Macena MDL, Silva DR, et al. A Meal with Ultra-Processed Foods Leads to a Faster Rate of Intake and to a Lesser Decrease in the Capacity to Eat When Compared to a Similar, Matched Meal Without Ultra-Processed Foods. Nutrients. 2024;16:4398.
Garutti M, Sirico M, Noto C, Foffano L, Hopkins M, Puglisi F. Hallmarks of Appetite: A Comprehensive Review of Hunger, Appetite, Satiation, and Satiety. Curr Obes Rep. 2025;14:1–20.
Lin CY, Lin YC, Kuo HK, Hwang JJ, Lin JL, Chen PC, et al. Association among acrylamide, blood insulin, and insulin resistance in adults. Diab Care. 2009;32:2206–11.
Feroe AG, Attanasio R, Scinicariello F. Acrolein metabolites, diabetes and insulin resistance. Environ Res. 2016;148:1–6.
Jhuo JY, Tong ZJ, Ku PH, Cheng HW, Wang HT. Acrolein induces mitochondrial dysfunction and insulin resistance in muscle and adipose tissues in vitro and in vivo. Environ Pollut. 2023;336:122380.
Mehrabani S, Shoaei N, Shateri Z, Askarpour M, Nouri M, Keshani P, et al. Consumption of ultra-processed foods could influence the metabolic syndrome odds: A cross-sectional study. Food Sci Nutr. 2024;12:2567–77.
Rinaldi AEM, Gabriel GFCP, Moreto F, Corrente JE, McLellan KCP, Burini RC. Dietary factors associated with metabolic syndrome and its components in overweight and obese Brazilian schoolchildren: a cross-sectional study. Diabetol Metab Syndr. 2016;8:1–10.
Dioneda B, Healy M, Paul M, Sheridan C, Mohr AE, Arciero PJ. A gluten-free meal produces a lower postprandial thermogenic response compared to an iso-energetic/macronutrient whole food or processed food meal in young women: A single-blind randomized cross-over trial. Nutrients. 2020;12:2035.
Andreasen CR, Andersen A, Knop FK, Vilsbøll T. How glucagon-like peptide 1 receptor agonists work. Endocr Connect. 2021;10:R200–12.
Imai S, Kajiyama S, Kitta K, Miyawaki T, Matsumoto S, Ozasa N, et al. Eating vegetables first regardless of eating speed has a significant reducing effect on postprandial blood glucose and insulin in young healthy women: randomized controlled cross-over study. Nutrients. 2023;15:1174.
Holst JJ, Rosenkilde MM. GIP as a therapeutic target in diabetes and obesity: insight from incretin co-agonists. J Clin Endocrinol Metab. 2020;105:e2710–6.
Müller TD, Blüher M, Tschöp MH, DiMarchi RD. Anti-obesity drug discovery: advances and challenges. Nat Rev Drug Discov. 2022;21:201–23.
Kern KA, Mietlicki-Baase EG. Distributed amylin receptor signaling and its influence on motivated behavior. Physiol Behav. 2020;222:112958.
Parmar RM, Can AS Physiology, appetite and weight regulation. In: StatPearls. StatPearls Publishing; 2023.
Acknowledgements
We thank all volunteers who agreed to participate in the study.
Funding
This work supported by Ondokuz Mayis University Scientific Research Projects Coordination Unit with project number BAP01-2024-5085.
Author information
Authors and Affiliations
Contributions
Menşure Nur Çelik; Conceptualization, Formal Analysis, Funding Acquisition, Investigation, Methodology, Project Administration, Writing – Original Draft, Writing – Review and Editing. Elif Ulug; Conceptualization, Formal Analysis, Data Curation, Methodology, Visualization, Writing – Original Draft, Writing – Review and Editing. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethics approval
Ethics committee approval suitable for the Declaration of Helsinki was received from Ondokuz Mayıs University Clinical Research Ethics Committee (Reference Number: B.30.2.ODM.0.20.08/663, Decision no: 2023/444, Date: 13 December 2023).
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Çelik, M.N., Ulug, E. Impact of ultra-processed foods on short-term appetite regulation: Does body mass index make a difference?. Int J Obes 50, 450–458 (2026). https://doi.org/10.1038/s41366-025-01961-9
Received:
Revised:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41366-025-01961-9