Abstract
The use of volume guarantee (VG) on high-frequency oscillatory ventilation (HFOV) allows to use fixed very low high-frequency tidal volume (VThf), maintaining adequate CO2 removal while potentially reducing the risk of ventilator-induced lung injury.
Objective
To demonstrate that the use of very low VThf can be protective compared with standard VThf on HFOV combined with VG in a neonatal animal model.
Study design
Experimental study in 2-day-old piglets with induced respiratory distress syndrome ventilated with two different HFOV strategies combined with VG (10 Hz with high VThf versus 20 Hz with very low VThf at similar PaCO2). After 12 h of mechanical ventilation, the pulmonary histologic pattern was analyzed.
Results
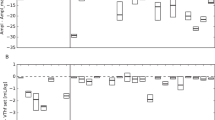
We found in the 10 Hz group with the higher VThf compared with the 20 Hz and very low VThf group more evident and more severe histological lesions with inflammatory infiltrate within the alveolar wall and alveolar space, as well as large areas of parenchyma consolidation and areas of alveolar hemorrhage in the more severe cases.
Conclusion
The use of very low VThf compared with higher VThf at similar CO2 removal reduces lung injury in a neonatal animal model of lung injury after prolonged mechanical ventilation with HFOV combined with VG.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Coalson JJ. Pathology of bronchopulmonary dysplasia. Semin Perinatol. 2006;30:179–84.
Gupta S, Sinha SK, Donn SM. Ventilatory management and bronchopulmonary dysplasia in preterm infants. Semin Fetal Neonatal Med. 2009;14:367–73.
Jobe AH, Ikegami M. Lung development and function in preterm infants in the surfactant treatment era. Annu Rev Physiol. 2000;62:825–46.
Slutsky AS. Lung injury caused by mechanical ventilation. Chest . 1999;116(1 Suppl):9S–15S.
Ambalavanan N, Carlo WA. Ventilatory strategies in the prevention and management of bronchopulmonary dysplasia. Semin Perinatol. 2006;30:192–9.
The Acute Respiratory Distress Syndrome Network. Ventilation with lower tidal volumes as compared with traditional tidal volumes for acute lung injury and the acute respiratory distress syndrome. N Eng J Med. 2000;342:1301–8.
Froese AB, Kinsella JP. High-frequency oscillatory ventilation: lessons from the neonatal/pediatric experience. Crit Care Med. 2005;33:S115–21.
Hamilton PP, Onayemi A, Smyth JA, Gillan JE, Cutz E, Froese AB, et al. Comparison of conventional and high-frequency ventilation: oxygenation and lung pathology. J Appl Physiol Respir Environ Exerc Physiol. 1983;55:131–8.
Meredith KS, deLemos RA, Coalson JJ, King RJ, Gerstmann DR, Kumar R, et al. Role of lung injury in the pathogenesis of hyaline membrane disease in premature baboons. J Appl Physiol (1985). 1989;66:2150–8.
Cools F, Offringa M, Askie LM. Elective high frequency oscillatory ventilation versus conventional ventilation for acute pulmonary dysfunction in preterm infants. Cochrane Database Syst Rev. 2015;3:CD000104. https://doi.org/10.1002/14651858.CD000104.pub4
Leipälä JA, Iwasaki S, Milner A, Greenough A. Accuracy of the volume and pressure displays of high frequency oscillators. Arch Dis Child Fetal Neonatal Ed. 2004;89:F174–6.
Sánchez Luna M, Santos González M, Tendillo Cortijo F. High-frequency oscillatory ventilation combined with volume guarantee in a neonatal animal model of respiratory distress syndrome. Crit Care Res Pract. 2013;2013:593915. https://doi.org/10.1155/2013/593915
Iscan B, Duman N, Tuzun F, Kumral A, Ozkan H. Impact of volume guarantee on high-frequency oscillatory ventilation in preterm infants: a randomized crossover clinical trial. Neonatology . 2015;108:277–82.
Kamitsuka MD, Boynton BR, Villanueva D, Vreeland PN, Frantz ID. Frequency, tidal volume, and mean airway pressure combinations that provide adequate gas exchange and low alveolar pressure during high frequency oscillatory ventilation in rabbits. Pediatr Res. 1990;27:64–9.
Slutsky AS, Kamm RD, Rossing TH, Loring SH, Lehr J, Shapiro AH, et al. Effects of frequency, tidal volume, and lung volume on CO2 elimination in dogs by high frequency (2-30 Hz), low tidal volume ventilation. J Clin Invest. 1981;68:1475–84.
Watson JW, Jackson AC, Gillespie JR. CO2 elimination and airway opening pressure during high frequency oscillation in dogs. Respir Physiol. 1984;58:235–44.
González-Pacheco N, Sánchez-Luna M, Ramos-Navarro C, Navarro-Patiño N, de la Blanca AR-S. Using very high frequencies with very low lung volumes during high-frequency oscillatory ventilation to protect the immature lung. A pilot study. J Perinatol. 2016;36:306–10.
Mukerji A, Belik J, Sanchez-Luna M. Bringing back the old: time to reevaluate the high-frequency ventilation strategy. J Perinatol. 2014;34:464–7.
Mann PC, Vahle J, Keenan CM, Baker JF, Bradley AE, Goodman DG, et al. International Harmonization of toxicologic pathology nomenclature: an overview and review of basic principles. Toxicol Pathol. 2012;40:7S–13S.
Slutsky AS. Ventilator-induced lung injury: from barotrauma to biotrauma. Respir Care. 2005;50:646–59.
Wakabayashi K, Wilson MR, Tatham KC, O’Dea KP, Takata M. Volutrauma, but not atelectrauma, induces systemic cytokine production by lung-marginated monocytes. Crit Care Med. 2014;42:e49–57.
Ronchi CF, dos Anjos Ferreira AL, Campos FJ, Kurokawa CS, Carpi MF, de Moraes MA, et al. High-frequency oscillatory ventilation attenuates oxidative lung injury in a rabbit model of acute lung injury. Exp Biol Med. 2011;236:1188–96.
Imai Y, Nakagawa S, Ito Y, Kawano T, Slutsky AS, Miyasaka K. Comparison of lung protection strategies using conventional and high-frequency oscillatory ventilation. J Appl Physiol. 2001;91:1836–44.
Meyer J, Cox PN, McKerlie C, Bienzle D. Protective strategies of high-frequency oscillatory ventilation in a rabbit model. Pediatr Res. 2006;60:401–6.
Liu S, Yi Y, Wang M, Chen Q, Huang Y, Liu L, Xie J, et al. Higher frequency ventilation attenuates lung injury during high-frequency oscillatory ventilation in sheep models of acute respiratory distress syndrome. Anesthesiology. 2013;119:398–411.
Leroy S, Caumette E, Waddington C, Hébert A, Brant R, Lavoie PM. A time-based analysis of inflammation in infants at risk of bronchopulmonary dysplasia. J Pediatr. 2018;192:60–5.
Acknowledgements
The authors thank Dräger Medical GmbH for providing the Babylog VN500 for the present study.
Funding
This study was supported in part by the National Grant of the Instituto de Salud Carlos III and the Fondo Europeo de Desarrollo Regional, FIS 14/00149.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
MS-L has received advisory board consulting fees from Dräger. The remaining authors declare that they have no conflict of interest.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
González-Pacheco, N., Sánchez-Luna, M., Chimenti-Camacho, P. et al. Use of very low tidal volumes during high-frequency ventilation reduces ventilator lung injury. J Perinatol 39, 730–736 (2019). https://doi.org/10.1038/s41372-019-0338-5
Received:
Revised:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41372-019-0338-5
This article is cited by
-
Evaluating tidal volume stability in extremely preterm infants on high-frequency oscillatory ventilation with volume guarantee
BMC Pediatrics (2025)
-
High-frequency oscillatory ventilation with volume guarantee in infants: a systematic review
Pediatric Research (2025)
-
Congenital diaphragmatic hernia: quality improvement using a maximal lung protection strategy and early surgery-improved survival
European Journal of Pediatrics (2023)
-
Gas Exchange Mechanism of High Frequency Ventilation: A Brief Narrative Review and Prospect
Journal of Shanghai Jiaotong University (Science) (2023)
-
Impact on cerebral hemodynamics of the use of volume guarantee combined with high frequency oscillatory ventilation in a neonatal animal respiratory distress model
European Journal of Pediatrics (2023)