Abstract
Objective
To determine the association of overnight extubation (OE) with extubation success.
Study design
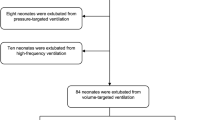
Retrospective cohort study in three NICUs from 2016 to 2020. Infants without congenital anomalies, less than 1500 grams at birth, who were ventilated and received an extubation attempt were included. Primary exposure was OE (7:00 pm–6:59 am) and outcome was extubation success defined as no mechanical ventilation for at least 7 days after extubation.
Results
A total of 76/379 (20%) infants received OE. Infants extubated during the daytime were older and had higher illness severity markers. Extubation success rates did not differ for overnight (57/76, 75%) versus daytime extubations (231/303, 76%) after adjusting for confounders (adjusted relative risk 0.95, 95% CI 0.82–1.11).
Conclusion
Though infants in our cohort undergoing daytime and OE were dissimilar, extubation success rates did not differ. Larger multicenter studies are needed to test our findings and identify markers of extubation readiness in preterm infants.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Stoll BJ, Hansen NI, Bell EF, Walsh MC, Carlo WA, Shankaran S, et al. Trends in care practices, morbidity, and mortality of extremely preterm neonates, 1993–2012. JAMA. 2015;314:1039–51.
Vendettuoli V, Bellu R, Zanini R, Mosca F, Gagliardi L. Italian Neonatal Network. Changes in ventilator strategies and outcomes in preterm infants. Arch Dis Child Fetal Neonatal Ed. 2014;99:F321–4.
Laptook AR, O’Shea TM, Shankaran S, Bhaskar B. Neonatal Research Network. Adverse neurodevelopmental outcomes among extremely low birth weight infants with a normal head ultrasound: prevalence and antecedents. Pediatrics. 2005;115:673–80.
Guillot M, Guo T, Ufkes S, Schneider J, Synnes A, Chau V, et al. Mechanical ventilation duration, brainstem development, and neurodevelopment in children born preterm: a prospective cohort study. J Pediatr. Published online May 23, 2020. https://doi.org/10.1016/j.jpeds.2020.05.039.
Tsai WH, Hwang YS, Hung TY, Weng SF, Lin SJ, Chang WT. Association between mechanical ventilation and neurodevelopmental disorders in a nationwide cohort of extremely low birth weight infants. Res Dev Disabil. 2014;35:1544–50.
Jensen EA, DeMauro SB, Kornhauser M, Aghai ZH, Greenspan JS, Dysart KC. Effects of multiple ventilation courses and duration of mechanical ventilation on respiratory outcomes in extremely low-birth-weight infants. JAMA Pediatr. 2015;169:1011–7.
Walsh MC, Morris BH, Wrage LA, Vohr BR, Poole WK, Tyson JE, et al. Extremely low birthweight neonates with protracted ventilation: mortality and 18-month neurodevelopmental outcomes. J Pediatr. 2005;146:798–804.
Chawla S, Natarajan G, Shankaran S, Carper B, Brion LP, Keszler M, et al. Markers of successful extubation in extremely preterm infants, and morbidity after failed extubation. J Pediatr. 2017;189:113–9.e2.
Manley BJ, Doyle LW, Owen LS, Davis PG. Extubating extremely preterm infants: predictors of success and outcomes following failure. J Pediatr. 2016;173:45–9.
Everhart KK, Khorsand S, Khandelwal N, Michaelsen KE, Spiekerman CF, Joffe AM. Nighttime extubation does not increase risk of reintubation, length of stay, or mortality: experience of a large, Urban, Teaching Hospital. Anesth Analg. 2019;128:918–23.
Tischenkel BR, Gong MN, Shiloh AL, Pittignano VC, Keschner YG, Glueck JA, et al. Daytime versus nighttime extubations: a comparison of reintubation, length of stay, and mortality. J Intensive Care Med. 2016;31:118–26.
Krebs ED, Hawkins RB, Mehaffey JH, Fonner CE, Speir AM, Quader MA, et al. Is routine extubation overnight safe in cardiac surgery patients? J Thorac Cardiovasc Surg. 2019;157:1533–42.e2
Stark AR. American Academy of Pediatrics Committee on Fetus and Newborn. Levels of neonatal care. Pediatrics. 2004;114:1341–7.
Gershengorn HB, Scales DC, Kramer A, Wunsch H. Association between overnight extubations and outcomes in the intensive care unit. JAMA Intern Med. 2016;176:1651–60.
Giaccone A, Jensen E, Davis P, Schmidt B. Definitions of extubation success in very premature infants: a systematic review. Arch Dis Child Fetal Neonatal Ed. 2014;99:F124–7.
Zou G. A modified poisson regression approach to prospective studies with binary data. Am J Epidemiol. 2004;159:702–6.
Funk MJ, Westreich D, Wiesen C, Sturmer T, Brookhart MA, Davidian M. Doubly robust estimation of causal effects. Am J Epidemiol. 2011;173:761–7.
Austin PC, Stuart EA. Moving towards best practice when using inverse probability of treatment weighting (IPTW) using the propensity score to estimate causal treatment effects in observational studies. Stat Med. 2015;34:3661–79.
Hainmueller J. Entropy balancing for causal effects: a multivariate reweighting method to produce balanced samples in observational studies. Political Anal. 2012;20:25–46.
Austin PC. Balance diagnostics for comparing the distribution of baseline covariates between treatment groups in propensity-score matched samples. Stat Med. 2009;28:3083–107.
Rubin DB. Using propensity scores to help design observational studies: application to the tobacco litigation. Health Serv Outcomes Res Methodol. 2001;2:169–88.
Gershengorn HB, Wunsch H, Hua M, Bavaria JE, Gutsche J. Association of overnight extubation with outcomes after cardiac surgery in the intensive care unit. Ann Thorac Surg. 2019;108:432–42.
da Silva PS, Reis ME, Fonseca TS, Fonseca MC. Do in-hours or off-hours matter for extubating children in the pediatric intensive care unit? J Crit Care. 2016;36:97–101.
Al-Mandari H, Shalish W, Dempsey E, Keszler M, Davis PG, Sant’Anna G. International survey on periextubation practices in extremely preterm infants. Arch Dis Child Fetal Neonatal Ed. 2015;100:F428–31.
Cnossen MC, van Essen TA, Ceyisakar IE, Polinder S, Andriessen TM, van der Naalt J, et al. Adjusting for confounding by indication in observational studies: a case study in traumatic brain injury. Clin Epidemiol. 2018;10:841–52.
Tubbs-Cooley HL, Mara CA, Carle AC, Mark BA, Pickler RH. Association of nurse workload with missed nursing care in the neonatal intensive care unit. JAMA Pediatr. 2019;173:44–51.
Rogowski JA, Staiger D, Patrick T, Horbar J, Kenny M, Lake ET. Nurse staffing and NICU infection rates. JAMA Pediatr. 2013;167:444–50.
Funding
Use of the Research Electronic Data Capture program (REDCap) was supported by UL1 TR000445 from NCATS/NIH. Mrs. Guy was supported by the Vanderbilt-Meharry James P. Carter Scholars program. Dr. Hatch was supported by the Vanderbilt Department of Pediatrics Turner-Hazinski Research Award and the Gerber Foundation Research Award.
Author information
Authors and Affiliations
Contributions
BG and LDH conceptualized and designed the study and wrote the first draft of the manuscript. BG, MED, LR, and SOG performed and oversaw data collection. LDH designed and performed the statistical analyses. BG, MED, LR, SOG, and LDH reviewed and made significant edits to the manuscript and all authors agree with the final version as submitted.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Guy, B., Dye, M.E., Richards, L. et al. Association of time of day and extubation success in very low birthweight infants: a multicenter cohort study. J Perinatol 41, 2532–2536 (2021). https://doi.org/10.1038/s41372-021-01168-6
Received:
Revised:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41372-021-01168-6
This article is cited by
-
Peri-extubation settings in preterm neonates: a systematic review and meta-analysis
Journal of Perinatology (2024)
-
The best time for extubation—daylight at the end of the tunnel?
Journal of Perinatology (2021)