Abstract
Background
Given the multiple risk factors associated with bronchopulmonary dysplasia, the impact of advances in early respiratory management, particularly non-invasive ventilation, remains uncertain.
Methods
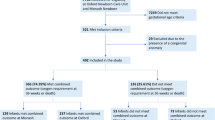
The early respiratory management and outcomes in 593 infants born at less than 32 weeks’ gestational age were retrospectively analyzed. The combined rate of bronchopulmonary dysplasia-mortality was compared across four propensity score-matched periods (2007-2010, 2011-2014, 2015-2018, 2019-2022).
Results
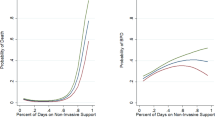
Delivery room intubation rate decreased from 54% to 36.7% (P < 0.001). Surfactant administration was delayed in the first three periods from 0.33 to 1.5 h (P < 0.001). The composite outcome of death or bronchopulmonary dysplasia rose from 14.9% to 39.8% over time, while mortality alone remained stable. In parallel, non-invasive ventilation duration increased with an adjusted mean difference of 21.98 days in 2019–2022.
Conclusion
The incidence of bronchopulmonary dysplasia continues to rise for very preterm infants, despite changes in early respiratory management and the increased use of non-invasive ventilation.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
Data availability
These data are generated from patient records as part of a retrospective study conducted in a Belgian academic hospital. The legal framework permits their consultation and use by investigators authorized by the ethics committee and hospital management. However, their reproduction or transmission is prohibited without institutional approval, as they are protected under GDPR.
References
Thebaud B, Goss KN, Laughon M, Whitsett JA, Abman SH, Steinhorn RH, et al. Bronchopulmonary dysplasia. Nat Rev Dis Prim. 2019;5:78.
Jobe AH, Steinhorn R. Can We Define Bronchopulmonary Dysplasia?. J Pediatr. 2017;188:19–23.
Lui K, Lee SK, Kusuda S, Adams M, Vento M, Reichman B, et al. Trends in Outcomes for Neonates Born Very Preterm and Very Low Birth Weight in 11 High-Income Countries. J Pediatr. 2019;215:32–40.e14.
Stoll BJ, Hansen NI, Bell EF, Walsh MC, Carlo WA, Shankaran S, et al. Trends in Care Practices, Morbidity, and Mortality of Extremely Preterm Neonates, 1993–2012. JAMA. 2015;314:1039–51.
Owen LS, Manley BJ, Davis PG, Doyle LW. The evolution of modern respiratory care for preterm infants. Lancet. 2017;389:1649–59.
Sweet DG, Carnielli VP, Greisen G, Hallman M, Klebermass-Schrehof K, Ozek E, et al. European Consensus Guidelines on the Management of Respiratory Distress Syndrome: 2022 Update. Neonatology. 2023;120:3–23.
Subramaniam P, Ho JJ, Davis PG. Prophylactic nasal continuous positive airway pressure for preventing morbidity and mortality in very preterm infants. Cochrane Database Syst Rev. 2016;6:CD001243.
Morley CJ, Davis PG, Doyle LW, Brion LP, Hascoet JM, Carlin JB, et al. Nasal CPAP or intubation at birth for very preterm infants. N Engl J Med. 2008;358:700–8.
Lodha A, Seshia M, McMillan DD, Barrington K, Yang J, Lee SK, et al. Association of early caffeine administration and neonatal outcomes in very preterm neonates. JAMA Pediatr. 2015;169:33–8.
BOOST II United Kingdom Collaborative Group, BOOST II Australia Collaborative Group, BOOST II New Zealand Collaborative Group, Stenson BJ, Tarnow-Mordi WO, Darlow BA, et al. Oxygen saturation and outcomes in preterm infants. N Engl J Med. 2013;368:2094–104.
Sweet D, Bevilacqua G, Carnielli V, Greisen G, Plavka R, Saugstad OD, et al. European consensus guidelines on the management of neonatal respiratory distress syndrome. J Perinat Med. 2007;35:175–86.
Sweet DG, Carnielli V, Greisen G, Hallman M, Ozek E, Plavka R, et al. European consensus guidelines on the management of neonatal respiratory distress syndrome in preterm infants - 2010 update. Neonatology. 2010;97:402–17.
Sweet DG, Carnielli V, Greisen G, Hallman M, Ozek E, Plavka R, et al. European consensus guidelines on the management of neonatal respiratory distress syndrome in preterm infants-2013 update. Neonatology. 2013;103:353–68.
Sweet DG, Carnielli V, Greisen G, Hallman M, Ozek E, Plavka R, et al. European Consensus Guidelines on the Management of Respiratory Distress Syndrome - 2016 Update. Neonatology. 2017;111:107–25.
Sweet DG, Carnielli V, Greisen G, Hallman M, Ozek E, Te Pas A, et al. European Consensus Guidelines on the Management of Respiratory Distress Syndrome - 2019 Update. Neonatology. 2019;115:432–50.
Cavolo A, Dierckx de Casterle B, Naulaers G, Gastmans C. Neonatologists’ Resuscitation Decisions at Birth for Extremely Premature Infants. A Belgian Qualitative Study. Front Pediatr. 2022;10:852073.
Richmond S, Wyllie J. European Resuscitation Council Guidelines for Resuscitation 2010 Section 7. Resuscitation of babies at birth. Resuscitation. 2010;81:1389–99.
Jensen EA, Dysart K, Gantz MG, McDonald S, Bamat NA, Keszler M, et al. The Diagnosis of Bronchopulmonary Dysplasia in Very Preterm Infants. An Evidence-based Approach. Am J Respir Crit Care Med. 2019;200:751–9.
Isayama T, Lee SK, Yang J, Lee D, Daspal S, Dunn M, et al. Revisiting the Definition of Bronchopulmonary Dysplasia: Effect of Changing Panoply of Respiratory Support for Preterm Neonates. JAMA Pediatr. 2017;171:271–9.
Corbet A, Bucciarelli R, Goldman S, Mammel M, Wold D, Long W. Decreased mortality rate among small premature infants treated at birth with a single dose of synthetic surfactant: a multicenter controlled trial. American Exosurf Pediatr Study Group 1 J Pediatr. 1991;118:277–84.
Lapcharoensap W, Gage SC, Kan P, Profit J, Shaw GM, Gould JB, et al. Hospital variation and risk factors for bronchopulmonary dysplasia in a population-based cohort. JAMA Pediatr. 2015;169:e143676.
McCaffrey DF, Griffin BA, Almirall D, Slaughter ME, Ramchand R, Burgette LF. A tutorial on propensity score estimation for multiple treatments using generalized boosted models. Stat Med. 2013;32:3388–414.
Badr DA, Mattern J, Carlin A, Cordier AG, Maillart E, El Hachem L, et al. Are clinical outcomes worse for pregnant women at >/=20 weeks’ gestation infected with coronavirus disease 2019? A multicenter case-control study with propensity score matching. Am J Obstet Gynecol. 2020;223:764–8.
Austin PC. The use of propensity score methods with survival or time-to-event outcomes: reporting measures of effect similar to those used in randomized experiments. Stat Med. 2014;33:1242–58.
Zorzato P, Torcia E, Carlin A, Familiari A, Cosmi E, Visentin S, et al. Comparison of two aspirin doses for the prophylaxis of pre-eclampsia in twin pregnancy: a multicentre retrospective study with propensity score matching. Am J Obstet Gynecol. 2025;233:55.e1–55.e10.
Regin Y, Gie A, Eerdekens A, Toelen J, Debeer A. Ventilation and respiratory outcome in extremely preterm infants: trends in the new millennium. Eur J Pediatr. 2022;181:1899–907.
García-Muñoz Rodrigo F, Losada Martínez A, Elorza Fernández MD, Moreno Hernando J, Figueras Aloy J, Vento Torres M. The Burden of Respiratory Disease in Very-Low-Birth-Weight Infants: Changes in Perinatal Care and Outcomes in a Decade in Spain. Neonatology. 2017;112:30–9.
Cheong JLY, Doyle LW. An update on pulmonary and neurodevelopmental outcomes of bronchopulmonary dysplasia. Semin Perinatol. 2018;42:478–84.
Chung J, Iyengar A, Santry L, Swanson E, Davis JM, Volpe MV. Changes in respiratory management and the impact on bronchopulmonary dysplasia. Pediatr Pulmonol. 2022;57:2327–34.
White H, Merritt K, Martin K, Lauer E, Rhein L. Respiratory support strategies in the prevention of bronchopulmonary dysplasia: A single center quality improvement initiative. Front Pediatr. 2022;10:1012655.
Brix N, Sellmer A, Jensen MS, Pedersen LV, Henriksen TB. Predictors for an unsuccessful INtubation-SURfactant-Extubation procedure: a cohort study. BMC Pediatr. 2014;14:155.
Ancora G, Maranella E, Grandi S, Pierantoni L, Guglielmi M, Faldella G. Role of bilevel positive airway pressure in the management of preterm newborns who have received surfactant. Acta Paediatr. 2010;99:1807–11.
Gopel W, Rausch TK, Mitschdorfer B, Mader S, Herting E, Konig IR, et al. A randomised controlled trial in preterm infants comparing prophylactic with selective “less invasive surfactant administration” (pro.LISA). Trials. 2023;24:612.
Härtel C, Kribs A, Gopel W, Dargaville P, Herting E. Less Invasive Surfactant Administration for Preterm Infants - State of the Art. Neonatology. 2024;121:584–95.
Askie LM, Darlow BA, Finer N, Schmidt B, Stenson B, Tarnow-Mordi W, et al. Association Between Oxygen Saturation Targeting and Death or Disability in Extremely Preterm Infants in the Neonatal Oxygenation Prospective Meta-analysis Collaboration. JAMA. 2018;319:2190–201.
Lui K, Jones LJ, Foster JP, Davis PG, Ching SK, Oei JL, et al. Lower versus higher oxygen concentrations titrated to target oxygen saturations during resuscitation of preterm infants at birth. Cochrane Database Syst Rev. 2018;5:CD010239.
Lyu Y, Shah PS, Ye XY, Warre R, Piedboeuf B, Deshpandey A, et al. Association between admission temperature and mortality and major morbidity in preterm infants born at fewer than 33 weeks’ gestation. JAMA Pediatr. 2015;169:e150277.
Bell EF, Hintz SR, Hansen NI, Bann CM, Wyckoff MH, DeMauro SB, et al. Mortality, In-Hospital Morbidity, Care Practices, and 2-Year Outcomes for Extremely Preterm Infants in the US, 2013-2018. JAMA. 2022;327:248–63.
Glaser K, Wright CJ. Indications for and Risks of Noninvasive Respiratory Support. Neonatology. 2021;118:235–43.
Adler-Haltovsky T, Gileles-Hillel A, Erlichman I, Eventov-Friedman S. Changes in ventilation modes in the last decade and their impact on the prevalence of bronchopulmonary dysplasia in preterm infants. Pediatr Pulmonol. 2023;58:1959–66.
Doyle LW, Carse E, Adams A-M, Ranganathan S, Opie G, Cheong JLY. Ventilation in Extremely Preterm Infants and Respiratory Function at 8 Years. N Engl J Med. 2017;377:329–37.
Deprest JA, Nicolaides KH, Benachi A, Gratacos E, Ryan G, Persico N, et al. Randomized Trial of Fetal Surgery for Severe Left Diaphragmatic Hernia. N Engl J Med. 2021;385:107–18.
Vuckovic A, Herber-Jonat S, Flemmer AW, Roubliova XI, Jani JC. Alveolarization genes modulated by fetal tracheal occlusion in the rabbit model for congenital diaphragmatic hernia: a randomized study. PLoS ONE. 2013;8:e69210.
Zhang EY, Bartman CM, Prakash YS, Pabelick CM, Vogel ER. Oxygen and mechanical stretch in the developing lung: risk factors for neonatal and pediatric lung disease. Front Med. 2023;10:1214108.
MacFarlane PM, Mayer CA, Jafri A, Pabelick CM, Prakash YS, Martin RJ. CPAP protects against hyperoxia-induced increase in airway reactivity in neonatal mice. Pediatr Res. 2021;90:52–7.
Gie AG, Salaets T, Vignero J, Regin Y, Vanoirbeek J, Deprest J, et al. Intermittent CPAP limits hyperoxia-induced lung damage in a rabbit model of bronchopulmonary dysplasia. Am J Physiol Lung Cell Mol Physiol. 2020;318:L976–L87.
McEvoy CT, MacDonald KD, Go MA, Milner K, Harris J, Schilling D, et al. Extended Continuous Positive Airway Pressure in Preterm Infants Increases Lung Growth at 6 Months: A Randomized Controlled Trial. Am J Respir Crit Care Med. 2025;211:610–8.
Farley RC, Hough JL, Jardine LA. Strategies for the discontinuation of humidified high flow nasal cannula (HHFNC) in preterm infants. Cochrane Database Syst Rev. 2015;2015:CD011079.
DeMauro SB, Roberts RS, Davis P, Alvaro R, Bairam A, Schmidt B. Impact of delivery room resuscitation on outcomes up to 18 months in very low birth weight infants. J Pediatr. 2011;159:546–50.e1.
Kwok TC, Szatkowski L, Sharkey D. Impact of postnatal dexamethasone timing on preterm mortality and bronchopulmonary dysplasia: a propensity score analysis. Eur Respir J. 2023;62:2300825.
Funding
First author is the recipient of a Grant of The Belgian Kids’ Fund (BKF) for Pediatric Research. The other authors received no additional funding. Role of Funder/Sponsor (if any): The BKF had no role in the design or conduct of the study.
Author information
Authors and Affiliations
Contributions
Emilie Goffinon, MD, PhD student, made a substantial contribution to conception and design, to acquisition and interpretation of data, as well as to drafting of the article. Dr Goffinon provided final approval of the version to be published. Aline Vuckovic, MD, PhD, made a substantial contribution to conception and design, interpretation of data, as well as to drafting and revising the article critically for important intellectual content. Dr Vuckovic provided final approval of the version to be published. Dr Badr made a substantial contribution to the design of the study, data analysis, and data interpretation. He largely contributed to drafting the methodology/results section of the review manuscript and provided final approval of the submitted version. Nicolas Lefèvre, MD, PhD made a substantial contribution to revising the article critically for important intellectual content. All authors approved the final manuscript as submitted and agree to be accountable for all aspects of the work.
Corresponding author
Ethics declarations
Competing interests
Emilie Goffinon has no conflicts of interest to disclose. The other authors have no conflicts of interest to disclose.
Ethics approval and consent to participate
All methods were performed in accordance with the relevant guidelines and regulations. The local Ethics Committee approved the protocol (Nos. 21/19). No parental consent was needed due to the retrospective nature of this study. No identifiable images were used in this study.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Goffinon, E., Badr, D.A., Lefèvre, N. et al. Rising rates of non-invasive ventilation and bronchopulmonary dysplasia: A propensity score-matched analysis. J Perinatol 46, 224–232 (2026). https://doi.org/10.1038/s41372-025-02494-9
Received:
Revised:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41372-025-02494-9