Abstract
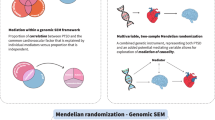
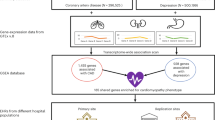
The association between coronary artery disease (CAD) and posttraumatic stress disorder (PTSD) contributes to the high morbidity and mortality observed for these conditions. To understand the dynamics underlying PTSD-CAD comorbidity, we investigated large-scale genome-wide association (GWA) statistics from the Million Veteran Program (MVP), the UK Biobank (UKB), the Psychiatric Genomics Consortium, and the CARDIoGRAMplusC4D Consortium. We observed a genetic correlation of CAD with PTSD case-control and quantitative outcomes, ranging from 0.18 to 0.32. To investigate possible cause-effect relationships underlying these genetic correlations, we performed a two-sample Mendelian randomization (MR) analysis, observing a significant bidirectional relationship between CAD and PTSD symptom severity. Genetically-determined PCL-17 (PTSD 17-item Checklist) total score was associated with increased CAD risk (odds ratio = 1.04; 95% confidence interval, 95% CI = 1.01–1.06). Conversely, CAD genetic liability was associated with reduced PCL-17 total score (beta = −0.42; 95% CI = −0.04 to −0.81). Because of these opposite-direction associations, we conducted a pleiotropic meta-analysis to investigate loci with concordant vs. discordant effects on PCL-17 and CAD, observing that concordant-effect loci were enriched for molecular pathways related to platelet amyloid precursor protein (beta = 1.53, p = 2.97 × 10−7) and astrocyte activation regulation (beta = 1.51, p = 2.48 × 10−6) while discordant-effect loci were enriched for biological processes related to lipid metabolism (e.g., triglyceride-rich lipoprotein particle clearance, beta = 2.32, p = 1.61 × 10−10). To follow up these results, we leveraged MVP and UKB electronic health records (EHR) to assess longitudinal changes in the association between CAD and posttraumatic stress severity. This EHR-based analysis highlighted that earlier CAD diagnosis is associated with increased PCL-total score later in life, while lower PCL total score was associated with increased risk of a later CAD diagnosis (Mann–Kendall trend test: MVP tau = 0.932, p < 2 × 10−16; UKB tau = 0.376, p = 0.005). In conclusion, both our genetically-informed analyses and our EHR-based follow-up investigation highlighted a bidirectional relationship between PTSD and CAD where multiple pleiotropic mechanisms are likely to be involved.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
Data availability
All data used discussed in this study are provided as Supplementary Material.
References
O’Donnell CJ, Schwartz Longacre L, Cohen BE, Fayad ZA, Gillespie CF, Liberzon I, et al. Posttraumatic stress disorder and cardiovascular disease: state of the science, knowledge gaps, and research opportunities. JAMA Cardiol. 2021;6:1207–16.
De Hert M, Detraux J, Vancampfort D. The intriguing relationship between coronary heart disease and mental disorders. Dialogues Clin Neurosci. 2018;20:31–40.
Coughlin SS. Post-traumatic stress disorder and cardiovascular disease. Open Cardiovasc Med J. 2011;5:164–70.
Seligowski AV, Steuber ER, Hinrichs R, Reda MH, Wiltshire CN, Wanna CP, et al. A prospective examination of sex differences in posttraumatic autonomic functioning. Neurobiol Stress. 2021;15:100384.
Vaccarino V, Shah AJ, Moncayo V, Nye J, Piccinelli M, Ko YA, et al. Posttraumatic stress disorder, myocardial perfusion, and myocardial blood flow: A Longitudinal Twin Study. Biol Psychiatry. 2022;91:615–25.
Davies NM, Holmes MV, Davey Smith G. Reading Mendelian randomisation studies: a guide, glossary, and checklist for clinicians. BMJ. 2018;362:k601.
Bountress KE, Wendt F, Bustamante D, Agrawal A, Webb B, Gillespie N, et al. Potential causal effect of posttraumatic stress disorder on alcohol use disorder and alcohol consumption in individuals of European descent: A Mendelian Randomization Study. Alcohol Clin Exp Res. 2021;45:1616–23.
Zhang F, Rao S, Cao H, Zhang X, Wang Q, Xu Y, et al. Genetic evidence suggests posttraumatic stress disorder as a subtype of major depressive disorder. J Clin Invest. 2022;132:e145942.
Hubel C, Gaspar HA, Coleman JRI, Hanscombe KB, Purves K, Prokopenko I, et al. Genetic correlations of psychiatric traits with body composition and glycemic traits are sex- and age-dependent. Nat Commun. 2019;10:5765.
Polimanti R, Amstadter AB, Stein MB, Almli LM, Baker DG, Bierut LJ, et al. A putative causal relationship between genetically determined female body shape and posttraumatic stress disorder. Genome Med. 2017;9:99.
Zhu Z, Zhu X, Liu CL, Shi H, Shen S, Yang Y, et al. Shared genetics of asthma and mental health disorders: a large-scale genome-wide cross-trait analysis. Eur Respir J. 2019;54:1901507.
Yuan S, Yao H, Larsson SC. Associations of cigarette smoking with psychiatric disorders: evidence from a two-sample Mendelian randomization study. Sci Rep. 2020;10:13807.
Muniz Carvalho C, Wendt FR, Maihofer AX, Stein DJ, Stein MB, Sumner JA, et al. Dissecting the genetic association of C-reactive protein with PTSD, traumatic events, and social support. Neuropsychopharmacology 2021;46:1071–7.
Lind MJ, Brick LA, Gehrman PR, Duncan LE, Gelaye B, Maihofer AX, et al. Molecular genetic overlap between posttraumatic stress disorder and sleep phenotypes. Sleep. 2020;43:zsz257.
Orri M, Pingault JB, Turecki G, Nuyt AM, Tremblay RE, Cote SM, et al. Contribution of birth weight to mental health, cognitive and socioeconomic outcomes: two-sample Mendelian randomisation. Br J Psychiatry. 2021:219:507–14.
Tamman AJF, Wendt FR, Pathak GA, Krystal JH, Montalvo-Ortiz JL, Southwick SM, et al. Attachment Style Moderates Polygenic Risk for Posttraumatic Stress in United States Military Veterans: Results From the National Health and Resilience in Veterans Study. Biol Psychiatry. 2021;89:878–87.
Polimanti R, Ratanatharathorn A, Maihofer AX, Choi KW, Stein MB, Morey RA, et al. Association of Economic Status and Educational Attainment With Posttraumatic Stress Disorder: A Mendelian Randomization Study. JAMA Netw Open. 2019;2:e193447.
Sumner JA, Maihofer AX, Michopoulos V, Rothbaum AO, Almli LM, Andreassen OA, et al. Examining Individual and Synergistic Contributions of PTSD and Genetics to Blood Pressure: A Trans-Ethnic Meta-Analysis. Front Neurosci. 2021;15:678503.
Pathak GA, Singh K, Wendt FR, Fleming TW, Overstreet C, Koller D, et al. Genetically regulated multi-omics study for symptom clusters of posttraumatic stress disorder highlights pleiotropy with hematologic and cardio-metabolic traits. Mol Psychiatry. 2022;27:1394–404.
Fu Q. Autonomic dysfunction and cardiovascular risk in post-traumatic stress disorder. Auton Neurosci. 2022;237:102923.
Edmondson D, von Kanel R. Post-traumatic stress disorder and cardiovascular disease. Lancet Psychiatry. 2017;4:320–9.
Koenen KC, Sumner JA, Gilsanz P, Glymour MM, Ratanatharathorn A, Rimm EB, et al. Post-traumatic stress disorder and cardiometabolic disease: improving causal inference to inform practice. Psychol Med. 2017;47:209–25.
Hunter-Zinck H, Shi Y, Li M, Gorman BR, Ji SG, Sun N, et al. Genotyping Array Design and Data Quality Control in the Million Veteran Program. Am J Hum Genet. 2020;106:535–48.
Sullivan PF, Agrawal A, Bulik CM, Andreassen OA, Borglum AD, Breen G, et al. Psychiatric Genomics: An Update and an Agenda. Am J Psychiatry. 2018;175:15–27.
Nelson CP, Goel A, Butterworth AS, Kanoni S, Webb TR, Marouli E, et al. Association analyses based on false discovery rate implicate new loci for coronary artery disease. Nat Genet. 2017;49:1385–91.
Bycroft C, Freeman C, Petkova D, Band G, Elliott LT, Sharp K, et al. The UK Biobank resource with deep phenotyping and genomic data. Nature 2018;562:203–9.
Wilkins KC, Lang AJ, Norman SB. Synthesis of the psychometric properties of the PTSD checklist (PCL) military, civilian, and specific versions. Depress Anxiety. 2011;28:596–606.
Stein MB, Levey DF, Cheng Z, Wendt FR, Harrington K, Pathak GA, et al. Genome-wide association analyses of post-traumatic stress disorder and its symptom subdomains in the Million Veteran Program. Nat Genet. 2021;53:174–84.
Harrington KM, Quaden R, Stein MB, Honerlaw JP, Cissell S, Pietrzak RH, et al. Validation of an Electronic Medical Record-Based Algorithm for Identifying Posttraumatic Stress Disorder in U.S. Veterans. J Trauma Stress. 2019;32:226–37.
Davis KAS, Coleman JRI, Adams M, Allen N, Breen G, Cullen B, et al. Mental health in UK Biobank - development, implementation and results from an online questionnaire completed by 157 366 participants: a reanalysis. BJPsych Open. 2020;6:e18.
Nievergelt CM, Maihofer AX, Klengel T, Atkinson EG, Chen CY, Choi KW, et al. International meta-analysis of PTSD genome-wide association studies identifies sex- and ancestry-specific genetic risk loci. Nat Commun. 2019;10:4558.
Nikpay M, Goel A, Won HH, Hall LM, Willenborg C, Kanoni S, et al. A comprehensive 1,000 Genomes-based genome-wide association meta-analysis of coronary artery disease. Nat Genet. 2015;47:1121–30.
Evangelou E, Warren HR, Mosen-Ansorena D, Mifsud B, Pazoki R, Gao H, et al. Genetic analysis of over 1 million people identifies 535 new loci associated with blood pressure traits. Nat Genet. 2018;50:1412–25.
Zhu Z, Wang X, Li X, Lin Y, Shen S, Liu CL, et al. Genetic overlap of chronic obstructive pulmonary disease and cardiovascular disease-related traits: a large-scale genome-wide cross-trait analysis. Respir Res. 2019;20:64.
Shah S, Henry A, Roselli C, Lin H, Sveinbjornsson G, Fatemifar G, et al. Genome-wide association and Mendelian randomisation analysis provide insights into the pathogenesis of heart failure. Nat Commun. 2020;11:163.
Zhang Y, Qi G, Park JH, Chatterjee N. Estimation of complex effect-size distributions using summary-level statistics from genome-wide association studies across 32 complex traits. Nat Genet. 2018;50:1318–26.
Bulik-Sullivan B, Finucane HK, Anttila V, Gusev A, Day FR, Loh PR, et al. An atlas of genetic correlations across human diseases and traits. Nat Genet. 2015;47:1236–41.
Euesden J, Lewis CM, O’Reilly PF. PRSice: Polygenic Risk Score software. Bioinformatics 2015;31:1466–8.
Dastani Z, Hivert MF, Timpson N, Perry JR, Yuan X, Scott RA, et al. Novel loci for adiponectin levels and their influence on type 2 diabetes and metabolic traits: a multi-ethnic meta-analysis of 45,891 individuals. PLoS Genet. 2012;8:e1002607.
Choi SW, Mak TS, O’Reilly PF. Tutorial: a guide to performing polygenic risk score analyses. Nat Protoc. 2020;15:2759–72.
Genomes Project C, Auton A, Brooks LD, Durbin RM, Garrison EP, Kang HM, et al. A global reference for human genetic variation. Nature. 2015;526:68–74.
Sanderson E, Glymour MM, Holmes MV, Kang H, Morrison J, Munafò MR, et al. Mendelian randomization. Nat Rev Methods Prim. 2022;2:6.
Skrivankova VW, Richmond RC, Woolf BAR, Yarmolinsky J, Davies NM, Swanson SA, et al. Strengthening the Reporting of Observational Studies in Epidemiology Using Mendelian Randomization: The STROBE-MR Statement. JAMA. 2021;326:1614–21.
Hemani G, Zheng J, Elsworth B, Wade KH, Haberland V, Baird D, et al. The MR-Base platform supports systematic causal inference across the human phenome. Elife 2018;7:e34408.
Bowden J, Davey Smith G, Burgess S. Mendelian randomization with invalid instruments: effect estimation and bias detection through Egger regression. Int J Epidemiol. 2015;44:512–25.
Hartwig FP, Davey Smith G, Bowden J. Robust inference in summary data Mendelian randomization via the zero modal pleiotropy assumption. Int J Epidemiol. 2017;46:1985–98.
Bowden J, Davey, Smith G, Haycock PC, Burgess S. Consistent Estimation in Mendelian Randomization with Some Invalid Instruments Using a Weighted Median Estimator. Genet Epidemiol. 2016;40:304–14.
Burgess S, Davey Smith G, Davies NM, Dudbridge F, Gill D, Glymour MM, et al. Guidelines for performing Mendelian randomization investigations. Wellcome Open Res. 2019;4:186.
Hemani G, Bowden J, Davey Smith G. Evaluating the potential role of pleiotropy in Mendelian randomization studies. Hum Mol Genet. 2018;27:R195–208.
Burgess S, Bowden J, Fall T, Ingelsson E, Thompson SG. Sensitivity Analyses for Robust Causal Inference from Mendelian Randomization Analyses with Multiple Genetic Variants. Epidemiology 2017;28:30–42.
Qingyuan Z, Jingshu W, Gibran H, Jack B, Dylan SS. Statistical inference in two-sample summary-data Mendelian randomization using robust adjusted profile score. Ann Stat. 2020;48:1742–69.
Verbanck M, Chen CY, Neale B, Do R. Detection of widespread horizontal pleiotropy in causal relationships inferred from Mendelian randomization between complex traits and diseases. Nat Genet. 2018;50:693–8.
O’Connor LJ, Price AL. Distinguishing genetic correlation from causation across 52 diseases and complex traits. Nat Genet. 2018;50:1728–34.
Bhattacharjee S, Rajaraman P, Jacobs KB, Wheeler WA, Melin BS, Hartge P, et al. A subset-based approach improves power and interpretation for the combined analysis of genetic association studies of heterogeneous traits. Am J Hum Genet. 2012;90:821–35.
de Leeuw CA, Mooij JM, Heskes T, Posthuma D. MAGMA: generalized gene-set analysis of GWAS data. PLoS Comput Biol. 2015;11:e1004219.
Watanabe K, Taskesen E, van Bochoven A, Posthuma D. Functional mapping and annotation of genetic associations with FUMA. Nat Commun. 2017;8:1826.
Liberzon A, Birger C, Thorvaldsdottir H, Ghandi M, Mesirov JP, Tamayo P. The Molecular Signatures Database (MSigDB) hallmark gene set collection. Cell Syst. 2015;1:417–25.
Townsend P, Phillimore P, Beattie A. Health and Deprivation: Inequality and the North. Croom Helm. 1988.
Wendt FR, Pathak GA, Overstreet C, Tylee DS, Gelernter J, Atkinson EG, et al. Characterizing the effect of background selection on the polygenicity of brain-related traits. Genomics 2021;113:111–9.
Burgess S, Davies NM, Thompson SG. Bias due to participant overlap in two-sample Mendelian randomization. Genet Epidemiol. 2016;40:597–608.
Maihofer AX, Choi KW, Coleman JRI, Daskalakis NP, Denckla CA, Ketema E, et al. Enhancing Discovery of Genetic Variants for Posttraumatic Stress Disorder Through Integration of Quantitative Phenotypes and Trauma Exposure Information. Biol Psychiatry. 2022;91:626–36.
Ralapanawa U, Sivakanesan R. Epidemiology and the Magnitude of Coronary Artery Disease and Acute Coronary Syndrome: A Narrative Review. J Epidemiol Glob Health. 2021;11:169–77.
Edmondson D. An Enduring Somatic Threat Model of Posttraumatic Stress Disorder Due to Acute Life-Threatening Medical Events. Soc Personal Psychol Compass 2014;8:118–34.
Hu YJ, Schmidt AF, Dudbridge F, Holmes MV, Brophy JM, Tragante V, et al. Impact of Selection Bias on Estimation of Subsequent Event Risk. Circ Cardiovasc Genet. 2017;10:e001616.
Evin G, Li QX. Platelets and Alzheimer’s disease: Potential of APP as a biomarker. World J Psychiatry. 2012;2:102–13.
Kitazume S, Yoshihisa A, Yamaki T, Oikawa M, Tachida Y, Ogawa K, et al. Soluble amyloid precursor protein 770 is released from inflamed endothelial cells and activated platelets: a novel biomarker for acute coronary syndrome. J Biol Chem. 2012;287:40817–25.
Plummer S, Van den Heuvel C, Thornton E, Corrigan F, Cappai R. The Neuroprotective Properties of the Amyloid Precursor Protein Following Traumatic Brain Injury. Aging Dis. 2016;7:163–79.
Meziab O, Kirby KA, Williams B, Yaffe K, Byers AL, Barnes DE. Prisoner of war status, posttraumatic stress disorder, and dementia in older veterans. Alzheimers Dement. 2014;10:S236–241.
Weiner MW, Veitch DP, Hayes J, Neylan T, Grafman J, Aisen PS, et al. Effects of traumatic brain injury and posttraumatic stress disorder on Alzheimer’s disease in veterans, using the Alzheimer’s Disease Neuroimaging Initiative. Alzheimers Dement. 2014;10:S226–235.
Anroedh S, Hilvo M, Akkerhuis KM, Kauhanen D, Koistinen K, Oemrawsingh R, et al. Plasma concentrations of molecular lipid species predict long-term clinical outcome in coronary artery disease patients. J Lipid Res. 2018;59:1729–37.
Mellon SH, Gautam A, Hammamieh R, Jett M, Wolkowitz OM. Metabolism, Metabolomics, and Inflammation in Posttraumatic Stress Disorder. Biol Psychiatry. 2018;83:866–75.
Vilchinsky N, Ginzburg K, Fait K, Foa EB. Cardiac-disease-induced PTSD (CDI-PTSD): A systematic review. Clin Psychol Rev. 2017;55:92–106.
Feng Y-CA, Ge T, Cordioli M, FinnGen, Ganna A, Smoller JW, et al. Findings and insights from the genetic investigation of age of first reported occurrence for complex disorders in the UK Biobank and FinnGen. medRxiv. 2020: 2020.2011.2020.20234302.
Pietrzak RH, Goldstein RB, Southwick SM, Grant BF. Prevalence and Axis I comorbidity of full and partial posttraumatic stress disorder in the United States: results from Wave 2 of the National Epidemiologic Survey on Alcohol and Related Conditions. J Anxiety Disord. 2011;25:456–65.
Pietrzak RH, Goldstein RB, Southwick SM, Grant BF. Medical comorbidity of full and partial posttraumatic stress disorder in US adults: results from Wave 2 of the National Epidemiologic Survey on Alcohol and Related Conditions. Psychosom Med. 2011;73:697–707.
Acknowledgements
We thank the veterans who participated in this study, and the members of the VA CSP and MVP study teams, without whom this work would not have been possible. This research has been also conducted using the UK Biobank Resource (application reference no. 58146).
Funding
This research is based on data from the MVP, Office of Research and Development, Veterans Health Administration and was supported by funding from the VA Cooperative Studies Program (CSP, no. CSP575B) and the Veterans Affairs Office of Research and Development MVP (grant nos. MVP000 and VA Merit MVP025). The views expressed in this article are those of the authors and do not necessarily reflect the position or policy of the Department of Veterans Affairs or the United States government.
Author information
Authors and Affiliations
Contributions
RP, CJO, TLA, MBS, JG designed the study. RP, FRW, GAP, DST, CT, ATH, DFL, KA, JMG, CJO, TLA, MBS, JG collected and interpreted the data. RP, FRW, GAP, DST analyzed the data. RP wrote the manuscript. RP, FRW, GAP, DST, CT, ATH, DFL, KA, JMG, CJO, TLA, MBS, JG edited the manuscript. RP, CJO, TLA, MBS, JG supervised the study.
Corresponding author
Ethics declarations
Competing interests
RP received a research grant from Alkermes. RP and JG received personal fees from Karger Publishers for their editorial work for Complex Psychiatry. JG is named as co-inventor on Patent Cooperation Treaty application no. 15/878,640 titled ‘Genotype-guided dosing of opioid agonists’, filed on January 24, 2018. CJO. received payment for editorial work for UpToDate and JAMA Cardiology and is currently employed by Novartis Institute of Biomedical Research. MBS received consulting fees from Acadia Pharmaceuticals, Aptinyx, Bionomics, Boehringer Ingelheim, Clexio Biosciences, EmpowerPharm, Engrail Therapeutics, Epivario, GW Pharmaceuticals, Janssen, and Jazz Pharmaceuticals; and payment for editorial work for UpToDate and the journals Biological Psychiatry and Depression and Anxiety. The other authors declare no competing financial interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Polimanti, R., Wendt, F.R., Pathak, G.A. et al. Understanding the comorbidity between posttraumatic stress severity and coronary artery disease using genome-wide information and electronic health records. Mol Psychiatry 27, 3961–3969 (2022). https://doi.org/10.1038/s41380-022-01735-z
Received:
Revised:
Accepted:
Published:
Issue date:
DOI: https://doi.org/10.1038/s41380-022-01735-z
This article is cited by
-
Shared genetic architecture of posttraumatic stress disorder with cardiovascular imaging, risk, and diagnoses
Nature Communications (2025)
-
Genes associated with depression and coronary artery disease are enriched for cardiomyopathy and inflammatory phenotypes
Nature Mental Health (2024)
-
Central stress pathways in the development of cardiovascular disease
Clinical Autonomic Research (2024)
-
Genome-wide association analyses identify 95 risk loci and provide insights into the neurobiology of post-traumatic stress disorder
Nature Genetics (2024)
-
Psychological and biological mechanisms linking trauma with cardiovascular disease risk
Translational Psychiatry (2023)