Abstract
Background
We aimed to assess whether a gene expression assay provided insights for understanding the heterogeneity among newborns affected by neonatal encephalopathy (NE).
Methods
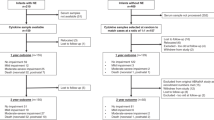
Analysis by RT-qPCR of the mRNA expression of candidate genes in whole blood from controls (n = 34) and NE (n = 24) patients at <6, 12, 24, 48, 72 and 96 h of life, followed by determination of differences in gene expression between conditions and correlation with clinical variables.
Results
During the first 4 days of life, MMP9, PPARG, IL8, HSPA1A and TLR8 were more expressed and CCR5 less expressed in NE patients compared to controls. MMP9 and PPARG increased and CCR5 decreased in moderate/severe NE patients compared to mild. At 6–12 h of life, increased IL8 correlated with severe NE and death, decreased CCR5 correlated with chorioamnionitis and increased HSPA1A correlated with expanded multiorgan dysfunction, severe NE and female sex.
Conclusions
MMP9, PPARG and CCR5 mRNA expression within first days of life correlates with the severity of NE. At 6–12 h, IL8 and HSPA1A are good reporters of clinical variables in NE patients. HSPA1A may have a role in the sexual dimorphism observed in NE. CCR5 is potentially involved in the link between severe NE and chorioamnionitis.
Similar content being viewed by others
Log in or create a free account to read this content
Gain free access to this article, as well as selected content from this journal and more on nature.com
or
References
Ferriero, D. M. & Bonifacio, S. L. The search continues for the elusive biomarkers of neonatal brain injury. J. Pediatr. 164, 438–440 (2014).
Arnaez, J. et al. Population-based study of the national implementation of therapeutic hypothermia in infants with hypoxic-ischemic encephalopathy. Ther. Hypothermia Temp. Manag. 8, 24–29 (2018).
Merchant, N. & Azzopardi, D. Early predictors of outcome in infants treated with hypothermia for hypoxic-ischaemic encephalopathy. Dev. Med. Child Neurol. 57(Suppl 3), 8–16 (2015).
Chalak, L. F. et al. Prospective research in infants with mild encephalopathy identified in the first six hours of life: neurodevelopmental outcomes at 18-22 months. Pediatr. Res. 84, 861–868 (2018).
Jacobs, S. E. et al. Cooling for newborns with hypoxic ischaemic encephalopathy. Cochrane Database Syst. Rev. 1, CD003311 (2013).
Davidson, J. O. et al. Therapeutic hypothermia for neonatal hypoxic-ischemic encephalopathy—where to from here? Front. Neurol. 6, 198 (2015).
Charriaut-Marlangue, C., Besson, V. C. & Baud, O. Sexually dimorphic outcomes after neonatal stroke and hypoxia-ischemia. Int. J. Mol. Sci. 19, E61 (2017).
Negro, S. et al. Early prediction of hypoxic-ischemic brain injury by a new panel of biomarkers in a population of term newborns. Oxid. Med. Cell Longev. 2018, 7608108 (2018).
Chalak, L. F. et al. Biomarkers for severity of neonatal hypoxic-ischemic encephalopathy and outcomes in newborns receiving hypothermia therapy. J. Pediatr. 164, 468–474 e461 (2014).
Tang, Y. et al. Gene expression in blood changes rapidly in neutrophils and monocytes after ischemic stroke in humans: a microarray study. J. Cereb. Blood Flow Metab. 26, 1089–1102 (2006).
Moore, D. F. et al. Using peripheral blood mononuclear cells to determine a gene expression profile of acute ischemic stroke: a pilot investigation. Circulation 111, 212–221 (2005).
Ohta, H., Terao, Y., Shintani, Y. & Kiyota, Y. Therapeutic time window of post-ischemic mild hypothermia and the gene expression associated with the neuroprotection in rat focal cerebral ischemia. Neurosci. Res. 57, 424–433 (2007).
Rutherford, M. et al. Assessment of brain tissue injury after moderate hypothermia in neonates with hypoxic-ischaemic encephalopathy: a nested substudy of a randomised controlled trial. Lancet Neurol. 9, 39–45 (2010).
Agut, T. et al. Early identification of brain injury in infants with hypoxic ischemic encephalopathy at high risk for severe impairments: accuracy of MRI performed in the first days of life. BMC Pediatr. 14, 177 (2014).
Alsina, M. et al. The severity of hypoxic-ischemic encephalopathy correlates with multiple organ dysfunction in the hypothermia era. Pediatr. Crit. Care Med. 18, 234–240 (2017).
Nair, J. & Kumar, V. H. S. Current and emerging therapies in the management of hypoxic ischemic encephalopathy in neonates. Children 5, E99 (2018).
Varsami, M. X. T. et al. Inflammation and oxidative stress biomarkers in neonatal brain hypoxia and prediction of adverse neurological outcome: a review. J. Pediatr. Neonat. Individual. Med. 2, 1–14 (2013).
Echeverria-Palacio, C. M. et al. Neuron-specific enolase in cerebrospinal fluid predicts brain injury after sudden unexpected postnatal collapse. Pediatr. Neurol. 101, 71–77 (2019).
Alderliesten, T. et al. MR imaging and outcome of term neonates with perinatal asphyxia: value of diffusion-weighted MR imaging and (1)H MR spectroscopy. Radiology 261, 235–242 (2011).
Zhu, L. et al. Circular RNA expression in the brain of a neonatal rat model of periventricular white matter damage. Cell Physiol. Biochem. 49, 2264–2276 (2018).
Massaro, A. N. et al. Plasma biomarkers of brain injury in neonatal hypoxic-ischemic encephalopathy. J. Pediatr. 194, 67–75 e61 (2018).
Mallard, C. & Vexler, Z. S. Modeling ischemia in the immature brain: how translational are animal models? Stroke 46, 3006–3011 (2015).
Lenglet, S., Montecucco, F. & Mach, F. Role of matrix metalloproteinases in animal models of ischemic stroke. Curr. Vasc. Pharm. 13, 161–166 (2015).
Souvenir, R. et al. Tissue inhibitor of matrix metalloproteinase-1 mediates erythropoietin-induced neuroprotection in hypoxia ischemia. Neurobiol. Dis. 44, 28–37 (2011).
Ranasinghe, H. S. et al. Inhibition of MMP-9 activity following hypoxic ischemia in the developing brain using a highly specific inhibitor. Dev. Neurosci. 34, 417–427 (2012).
Al-Shargabi, T. et al. Inflammatory cytokine response and reduced heart rate variability in newborns with hypoxic-ischemic encephalopathy. J. Perinatol. 37, 668–672 (2017).
Jenkins, D. D. et al. Serum cytokines in a clinical trial of hypothermia for neonatal hypoxic-ischemic encephalopathy. J. Cereb. Blood Flow Metab. 32, 1888–1896 (2012).
Calderwood, S. K., Mambula, S. S., Gray, P. J. Jr. & Theriault, J. R. Extracellular heat shock proteins in cell signaling. FEBS Lett. 581, 3689–3694 (2007).
Guisasola, M. C. et al. An overview of cytokines and heat shock response in polytraumatized patients. Cell Stress Chaperones 23, 483–489 (2018).
Borges, T. J., Lang, B. J., Lopes, R. L. & Bonorino, C. Modulation of alloimmunity by heat shock proteins. Front. Immunol. 7, 303 (2016).
Wu, Y. W. et al. Nighttime delivery and risk of neonatal encephalopathy. Am. J. Obstet. Gynecol. 204, 37 e31–36 (2011).
Reddy, A. T., Lakshmi, S. P. & Reddy, R. C. PPARgamma in bacterial infections: a friend or foe? PPAR Res. 2016, 7963540 (2016).
Schmidt, M. V., Brune, B. & von Knethen, A. The nuclear hormone receptor PPARgamma as a therapeutic target in major diseases. Sci. World J. 10, 2181–2197 (2010).
Wu, J. S. et al. Ligand-activated peroxisome proliferator-activated receptor-gamma protects against ischemic cerebral infarction and neuronal apoptosis by 14-3-3 epsilon upregulation. Circulation 119, 1124–1134 (2009).
Martin-Blondel, G. et al. CCR5 blockade for neuroinflammatory diseases–beyond control of HIV. Nat. Rev. Neurol. 12, 95–105 (2016).
Bierstone, D. et al. Association of histologic chorioamnionitis with perinatal brain injury and early childhood neurodevelopmental outcomes among preterm neonates. JAMA Pediatr. 172, 534–541 (2018).
Xiao, D. et al. Maternal chorioamnionitis and neurodevelopmental outcomes in preterm and very preterm neonates: a meta-analysis. PLoS ONE 13, e0208302 (2018).
Hassell, K. J. et al. New horizons for newborn brain protection: enhancing endogenous neuroprotection. Arch. Dis. Child Fetal Neonatal Ed. 100, F541–F552 (2015).
Bosl, K. et al. Coactivation of TLR2 and TLR8 in primary human monocytes triggers a distinct inflammatory signaling response. Front. Physiol. 9, 618 (2018).
Chaparro-Huerta, V. et al. Proinflammatory cytokines, enolase and S-100 as early biochemical indicators of hypoxic-ischemic encephalopathy following perinatal asphyxia in newborns. Pediatr. Neonatol. 58, 70–76 (2017).
Acknowledgements
This work was supported by a grant (PI08/1366) from the Instituto de Salud Carlos III cofounded by the European Regional Development Fund.
Author information
Authors and Affiliations
Contributions
A.G.-A. and S.A. conceived and supervised the study. M.L., G.A. and A.G.-A. provided samples and clinical data of the patients. R.B. performed the experiments and collected the data. C.T. performed the statistical analysis. A.-A.C performed leukocyte purification and western blot analysis. R.B. wrote and S.A. and A.G.-A. critically revised the manuscript. All authors reviewed the article for intellectual content and approved the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Balada, R., Tebé, C., León, M. et al. Enquiring beneath the surface: can a gene expression assay shed light into the heterogeneity among newborns with neonatal encephalopathy?. Pediatr Res 88, 451–458 (2020). https://doi.org/10.1038/s41390-020-0764-2
Received:
Revised:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41390-020-0764-2
This article is cited by
-
Emerging modalities for neuroprognostication in neonatal encephalopathy: harnessing the potential of artificial intelligence
Pediatric Research (2025)
-
CSF neopterin and beta-2-microglobulin as inflammation biomarkers in newborns with hypoxic–ischemic encephalopathy
Pediatric Research (2023)
-
Biomarkers of hypoxic–ischemic encephalopathy: a systematic review
World Journal of Pediatrics (2023)
-
Reply to “The use of gene expression as disease stratification tool of neonatal encephalopathy”
Pediatric Research (2021)
-
The use of gene expression as a disease stratification tool of neonatal encephalopathy
Pediatric Research (2021)