Abstract
Background
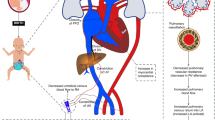
Many physiological aspects of the neonatal transition after birth are unobservable because relevant sensors do not yet exist, compromising clinicians’ understanding of a neonate’s physiological status. Given that a neonate’s true physiological state is currently unavailable, we explored the feasibility of using clinicians’ degree of concordance as an approximation of the true physiological state.
Methods
Two phases of structured interviews were conducted. In Phase 1 (N = 8) and Phase 2 (N = 12), we presented neonatal experts with eight graphical trajectories of real newborns’ heart rate and oxygen saturation values in the first 10–15 min after birth. We elicited the participants’ interpretations of potential underlying physiological conditions that could explain the vital sign patterns.
Results
The global differential diagnosis data for each phase produced the same pattern of results: (1) four trajectories produced a substantial degree of concordance among clinicians (61–80%) and (2) four trajectories produced a strong degree of concordance among clinicians (81–100%).
Conclusions
It is possible to achieve a strong degree of concordance among neonatal experts’ interpretations of newborn trajectories. Thus, using the degree of concordance as an approximation of the neonate’s true physiological state in resuscitation after birth may be a promising direction to explore for cognitive aid design.
Impact
-
Differential diagnoses with a good degree of concordance among expert neonatal clinicians could potentially substitute in part for the direct measurement of key physiological and anatomical variables of the neonatal transition, which is currently unavailable.
-
The concordance of clinicians’ judgements or inferences with regards to the true physiological state of the newborn during resuscitation after birth has never been explored.
-
The findings provide a crucial first step toward using consensus of neonatal experts’ judgements in the design of a cognitive aid to support clinicians’ management of the newborns who require resuscitation after birth.
Similar content being viewed by others
Log in or create a free account to read this content
Gain free access to this article, as well as selected content from this journal and more on nature.com
or
References
Hillman, N. H., Kallapur, S. G. & Jobe, A. H. Physiology of transition from intrauterine to extrauterine life. Clin. Perinatol. 39, 769–783 (2012).
Hooper, S., Kitchen, J. M., Polglase, R. G., Roehr, C. C. & Te Pas, B. A. The physiology of neonatal resuscitation. Curr. Opin. Pediatr. 30, 187–191 (2018).
Askin, D. F. Complications in the transition from fetal to neonatal life. J. Obstet. Gynecol. Neonatal Nurs. 31, 318–327 (2002).
Schmölzer, G. M., Morley, C. J. & Kamlin, O. C. O. F. Enhanced monitoring during neonatal resuscitation. Semin. Perinatol. 43, 151177 (2019).
Zestic, J., Sanderson, P., Dawson, J. & Liley, H. Defining information needs in neonatal resuscitation with work domain analysis. J. Clin. Monit. Comput. 13, 1–22 (2020).
Crossley, K. J. et al. Dynamic changes in the direction of blood flow through the ductus arteriosus at birth. J. Physiol. 587, 4695–4704 (2009).
Hooper, S., Polglase, G. R. & Roehr, C. C. Cardiopulmonary changes with aeration of the newborn lung. Paediatr. Respir. Rev. 16, 147–150 (2015).
Polglase, G. R. et al. Physiologically based cord clamping stabalises cardiac output and reduces cerebrovascular injury in asphyxiated near-term lambs. Arch. Dis. Child. Fetal Neonatal Ed. 103, F530 (2018).
Blank, D. A. et al. Respiratory changes in term infants immediately after birth. Resuscitation 130, 105–110 (2018).
Jeroen, Jv. V. et al. Noninvasive measurements of hemodynamic transition directly after birth. Pediatr. Res. 75, 448–452 (2013).
van Vonderen, J., Roest, A., Klumper, F., Hooper, S. & Pas, A. The effect of breathing on ductus arteriosus blood flow directly after birth. Eur. J. Pediatr. 176, 1581–1585 (2017).
Hou, M., Burns, C. M. & Banbury, S. Advances and challenges in intelligent adaptive interface design. In Contemporary Issues in Systems Science and Engineering (Zhou, M., Li, H.-X. & Weijnen, M., eds) 367–424 (Wiley, New Jersey, 2015).
Vicente, K. J. Coherence-and correspondence-driven work domains: Implications for systems design. Behav. Inform. Technol. 9, 493–502 (1990).
Baig, M. M., Gholam Hosseini, H., Kouzani, A. & Harrison, M. J. Anaesthesia monitoring using fuzzy logic. J. Clin. Monit. Comp. 25, 339–347 (2011).
Bolon-Canedo, V. et al. Dealing with inter-expert variability in retinopathy of prematurity: a machine learning approach. Comput. Meth. Prog. Biomed. 122, 1–15 (2015).
Miller, A., Scheinkestel, C. & Steele, C. The effects of clinical information presentation on physicians’ and nurses’ decision-making in ICUs. Appl. Ergon. 40, 753–761 (2009).
Grundgeiger, T. et al. Cognitive aids in acute care: investigating how cognitive aids affect and support in-hospital emergency teams. In Proc. 2019 CHI Conference on Human Factors in Computing Systems 1–14 (Association for Computing Machinery, 2019).
Marshall, S. The use of cognitive aids during emergencies in anesthesia: a review of the literature. Anesth. Analg. 117, 1162–1171 (2013).
Calder, L. A. et al. Healthcare providers’ perceptions of a situational awareness display for emergency department resuscitation: a simulation qualitative study. Int. J. Qual. Health Care 30, 16–22 (2018).
Fuerch, J. H., Yamada, N. K., Coelho, P. R., Lee, H. C. & Halamek, L. P. Impact of a novel decision support tool on adherence to Neonatal Resuscitation Program algorithm. Resuscitation 88, 52–56 (2015).
Gonzales, M., Henry, J., Calhoun, A. & Riek, L. Visual TASK: a collaborative cognitive aid for acute care resuscitation. In 10th EAI International Conference on Pervasive Computing Technologies for Healthcare (Pervasive Health) 1–8 (Cornell University Library, 2016).
Roitsch, C., Patricia, K., Hagan, J., Arnold, J. & Sundgren, N. Tablet-based decision support tool improves performance of neonatal resuscitation: a randomized trial in simulation. Simul. Health 15, 243–250 (2020).
Schild, S. et al. A digital cognitive aid for anesthesia to support intraoperative crisis management: results of the user-centered design process. JMIR mHealth uHealth. 7, e13226 (2019).
Klüber, S. et al. Experience matters: design and evaluation of an anesthesia support tool guided by user experience theory. In Proc. 2020 ACM Designing Interactive Systems Conference 1523–1535 (Association for Computing Machinery, 2020).
Nielsen, J. Usability inspection methods. In Computer Human Interaction 413–414 (Computer Human Interaction Conference Companion, 1994).
Dawson, J. A. et al. Defining the reference range for oxygen saturation for infants after birth. Pediatrics 125, e1340–e1347 (2010).
Cohen, J. A coefficient of agreement for nominal scales. Educ. Psychol. Meas. 20, 37–46 (1960).
Fleiss, J. L. Measuring nominal scale agreement among many raters. Psychol. Bull. 76, 378–382 (1971).
Landis, J. R. & Koch, G. G. The measurement of observer agreement for categorical data. Biometrics 33, 159–174 (1977).
Ericsson, K. A. & Lehmann, A. C. Expert and exceptional performance: Evidence of maximal adaptation to task constraints. Annu. Rev. Psychol. 47, 273–305 (1996).
Klein, G. In Advances in Man-Machine Systems (ed. Rouse, W. B.) 47–92 (JAI Press, 1989).
Faust, O., Hagiwara, Y., Hong, T. J., Lih, O. S. & Acharya, U. R. Deep learning for healthcare applications based on physiological signals: a review. Comput. Meth. Prog. Biol. 161, 1–13 (2018).
Pickup, L. et al. Development of a clinical interface for a novel newborn resuscitation device: human factors approach to understanding cognitive user requirements. J. Med. Internet Res. 6, e12055 (2019).
Acknowledgements
We gratefully acknowledge the contributions of Jennifer Dawson for providing us with access to the neonatal database, and Isaac Salisbury for assisting in the extraction of the neonatal trajectories from the database. Support for this research was provided by J.Z.’s research higher degree (HDR) support funds at The University of Queensland and her Australian Government Research Training Programme (RTP) Scholarship. The project was also supported by The University of Queensland School of Psychology Strategic funds allocation to P.S.
Author information
Authors and Affiliations
Contributions
Substantial contributions to conception and design, acquisition of data or analysis and interpretation of data: J.Z., H.L. and P.S. Drafting the article or revising it critically for important intellectual content: J.Z., H.L. and P.S. Final approval of the version to be published: J.Z., H.L. and P.S.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Consent statement
Patient consent was not required for this study. Clinician participants provided written informed consent. The study was given ethical approval by Mater Misericordiae Ltd (approval 53861) and by the Human Research Ethics Committee at The University of Queensland (approval 2019002697).
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Zestic, J., Liley, H. & Sanderson, P. Concordance of expert clinicians’ interpretations of the newborn’s true physiological state. Pediatr Res 91, 1222–1230 (2022). https://doi.org/10.1038/s41390-021-01565-9
Received:
Revised:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41390-021-01565-9