Abstract
Background
Children 10–20 years old in the US have suboptimal hydration status. Hydration is best assessed using an objective marker, such as urine specific gravity (USG) from a 24-h urine collection. There are limited studies associating hydration from an objective marker with intake assessed from 24-h recalls in children. The objective of the study was to evaluate which foods or beverages are significantly associated with an objective marker of hydration (USG) in a sample of children and adolescents.
Methods
Intake was assessed from three 24-h dietary recalls and analyzed using the Nutrition Data System for Research (NDSR). Hydration status was objectively measured using USG via 24-h urine collection. Associations were assessed with logistic regressions.
Results
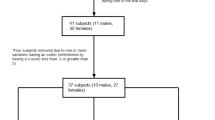
A total of 68 children and adolescents were recruited (50% females). Average overall USG score was 1.020 ± 0.011 uG with 39.7% categorized as dehydrated. After adjusting for age and sex, fruit juice (1.009, 95% CI: 1.001, 1.018) and all beverages (1.001, 95% CI: 1.000, 1.002) were significantly associated with higher odds of being euhydrated.
Conclusions
The main predictors of hydration were fruit juice and all beverages intake. Future research should be conducted to explore differences in dietary patterns in a larger, more generalizable sample.
Impact
-
Findings showed that the main predictors of hydration were water and fruit juice intake in children and water intake in adolescents in southern Florida.
-
This is the first study to examine which type of beverages and foods are associated with USG, an objective marker of hydration status, in US children and adolescents.
-
Provides further insight into the use of objective markers to assess hydration status, while providing data to assist epidemiological studies that may have limited resources to examine beverages and foods that contribute to hydration.
Similar content being viewed by others
Log in or create a free account to read this content
Gain free access to this article, as well as selected content from this journal and more on nature.com
or
Data availability
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Suh, H. G. & Kavouras, S. A. Water intake and hydration state in children. Eur. J. Nutr. 58, 475–496 (2019).
Chang, T., Ravi, N., Plegue, M. A., Sonneville, K. R. & Davis, M. M. Inadequate hydration, BMI, and obesity among US adults: NHANES 2009-2012. Ann. Fam. Med. 14, 320–324 (2016).
Maffeis, C. et al. Fluid intake and hydration status in obese vs normal weight children. Eur. J. Clin. Nutr. 70, 560–565 (2016).
García, A. I. L. et al. Association between hydration status and body composition in healthy adolescents from Spain. Nutrients 11, https://doi.org/10.3390/nu11112692 (2019).
Vieux, F., Maillot, M., Rehm, C. D., Barrios, P., Drewnowski, A. Trends in tap and bottled water consumption among children and adults in the United States: analyses of NHANES 2011–16 data. Nutr. J. 19, https://doi.org/10.1186/S12937-020-0523-6 (2020).
Institute of Medicine (U.S.). Panel on Dietary Reference Intakes for Electrolytes and Water. DRI, Dietary Reference Intakes for Water, Potassium, Sodium, Chloride, and Sulfate (National Academies Press, 2004).
Kenney, E. L., Long, M. W., Cradock, A. L. & Gortmaker, S. L. Prevalence of inadequate hydration among US children and disparities by gender and race/ethnicity: National Health and Nutrition Examination Survey, 2009–2012. Am. J. Public Health 105, e113–e118 (2015).
Baron, S., Courbebaisse, M., Lepicard, E. M. & Friedlander, G. Assessment of hydration status in a large population. Br. J. Nutr. 113, 147–158 (2015).
Palacios, C. et al. Effect of Soluble Corn Fiber supplementation for 1 year on bone metabolism in children, the MetA-Bone Trial: Rationale and Design. Contemp. Clin. Trials 95, 106061 (2020).
Hess, J. M., Cifelli, C. J. & Fulgoni, V. L. Energy and nutrient intake of americans according to meeting current dairy recommendations. Nutrients 12, 1–14 (2020).
Center for Health Statistics N. Anthropometry Procedures Manual. Published online 2017.
Growth Charts - Individual Growth Charts. Accessed May 4, 2022. https://www.cdc.gov/growthcharts/charts.htm.
Craig, C. L. et al. International physical activity questionnaire: 12-country reliability and validity. Med. Sci. Sports Exerc 35, 1381–1395 (2003).
Burrows, T. L., Martin, R. J. & Collins, C. E. A systematic review of the validity of dietary assessment methods in children when compared with the method of doubly labeled water. J. Am. Diet. Assoc. 110, 1501–1510 (2010).
Foster, E. et al. Validity and reliability of an online self-report 24-h dietary recall method (Intake24): A doubly labelled water study and repeated-measures analysis. J Nutr Sci. https://doi.org/10.1017/JNS.2019.20 (2019).
Ma, Y. et al. Number of 24-hour diet recalls needed to estimate energy intake. Ann. Epidemiol. 19, 553 (2009).
Shamah-Levy, T. et al. Three 24-hour recalls in comparison with one improve the estimates of energy and nutrient intakes in an Urban Mexican population. J. Nutr. 146, 1043–1050 (2016).
Logan-Sprenger, H. M. & Spriet, L. L. The acute effects of fluid intake on urine specific gravity and fluid retention in a mildly dehydrated state. J. Strength Cond. Res 27, 1002–1008 (2013).
Sawka, M. N. et al. American College of Sports Medicine position stand. Exercise and fluid replacement. Med Sci. Sports Exerc 39, 377–390 (2007).
Scientific Opinion on Dietary Reference Values for water. EFSA J. 8, https://doi.org/10.2903/J.EFSA.2010.1459 (2016).
Willett, W. Nature of Variation in Diet. Nutritional Epidemiology. Published online November 7, 2012. https://doi.org/10.1093/ACPROF:OSO/9780199754038.003.0003
Feferbaum, R., de Abreu, L. C. & Leone, C. Fluid intake patterns: an epidemiological study among children and adolescents in Brazil. BMC Public Health 12, 1005 (2012).
Stookey, J. D., Brass, B., Holliday, A. & Arieff, A. What is the cell hydration status of healthy children in the USA? Preliminary data on urine osmolality and water intake. Public Health Nutr. 15, 2148–2156 (2012).
Bougatsas, D. et al. Fluid consumption pattern and hydration among 8-14 years-old children. Eur. J. Clin. Nutr. 72, 420–427 (2018).
Montenegro-Bethancourt, G., Johner, S. A. & Remer, T. Contribution of fruit and vegetable intake to hydration status in schoolchildren. Am. J. Clin. Nutr. 98, 1103–1112 (2013).
Liang, J. et al. Associations of weight-adjusted body fat and fat distribution with bone mineral density in chinese children aged 6–10 years. Int. J. Environ. Res. Public Health 17, https://doi.org/10.3390/IJERPH17051763 (2020).
Adams, W. M., Hevel, D. J., Maher, J. P., McGuirt, J. T. Racial and sex differences in 24h urinary hydration markers among male and female emerging adults: a pilot study. Nutrients 12, https://doi.org/10.3390/NU12041068 (2020).
Moshfegh, A. J. et al. The US Department of Agriculture Automated Multiple-Pass Method reduces bias in the collection of energy intakes. Am. J. Clin. Nutr. 88, 324–332 (2008).
Acknowledgements
We would like to thank Julia Leone from the Department of Dietetics and Nutrition, Stempel School of Public Health, at Florida International University for their contribution in the data collection.
Funding
This study was funded in part by the National Institutes of Health (Eunice Kennedy Shriver National Institute of Child Health and Human Development, NICHD), grant number 1R01HD098589-01.
Author information
Authors and Affiliations
Contributions
P.C. and C.P. facilitated and conducted the study, wrote the manuscript. M.A.T.F., R.G., and P.C. collected all questionnaires, biospecimens, and anthropometrics. C.P.: project oversight and was responsible for the final content of the manuscript; and all authors critically reviewed the manuscript and approved the final version.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Consent to participate
All participants enrolled in the study were required to provide written consent prior to participation.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Clayton, P., Trak-Fellermeier, M.A., Macchi, A. et al. The association between hydration status and total fluid intake in healthy children and adolescents. Pediatr Res 94, 796–802 (2023). https://doi.org/10.1038/s41390-023-02506-4
Received:
Revised:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41390-023-02506-4