Abstract
Background
Early developmental intervention seeks to enhance functional outcomes in preterm infants by leveraging neuroplasticity. We investigated the relationship between early intervention and neurodevelopmental outcomes in early childhood among preterm infants without severe brain injury.
Methods
This prospective cohort study enrolled very-low-birth-weight infants (23+0–32+6 weeks’ gestation) registered in the Korean Neonatal Network. Neurodevelopment was evaluated at corrected ages 18-24 months and chronological ages 33-45 months using the Bayley Scales of Infant and Toddler Development (Second or Third Edition), the Korean Developmental Screening Test, or both. Infants who began motor-based or language therapy prior to 18–24 months of corrected age were defined as the early intervention group.
Results
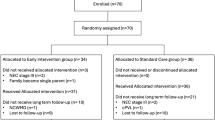
Of the 1797 infants who completed follow-up, 518 (28.8%) received early intervention. Compared to infants without early intervention, those with early intervention had lower gestational age and higher rates of prematurity-related complications and post-discharge rehospitalizations. The interaction between the intervention group and assessment time was statistically significant, indicating that early intervention was associated with a reduced risk of motor developmental delays over time (adjusted odds ratio 0.669, 95% confidence interval 0.472–0.949).
Conclusion
Early intervention was associated with more favorable motor outcomes, highlighting the importance of timely support for high-risk preterm infants.
Impact
-
Preterm infants with greater medical complexity more commonly received early intervention.
-
Early intervention mitigated the progression of motor developmental delays over time.
-
An enriched early environment may help offset the negative developmental impact of preterm complications.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 14 print issues and online access
$259.00 per year
only $18.50 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
Data availability
The Korean Neonatal Network (KNN) Publication Ethics Policy conforms to the following guidelines for managing and accessing research data: All information regarding patients and participating NICUs is confidential. Access to the data is limited to individuals with approved research purposes. Institutions or individuals not affiliated with the KNN must submit an official request to the KNN publication-Ethics Committee and obtain network approval to access the data.
References
Younge, N. et al. Survival and Neurodevelopmental Outcomes among Periviable Infants. N. Engl. J. Med. 376, 617–628 (2017).
Serenius, F. et al. Neurodevelopmental Outcome in Extremely Preterm Infants at 2.5 Years after Active Perinatal Care in Sweden. JAMA 309, 1810–1820 (2013).
Lee, H. C., Liu, J., Profit, J., Hintz, S. R. & Gould, J. B. Survival without major morbidity among very low birth weight infants in California. Pediatrics 146, e20193865 (2020).
Cheong, J. L. Y. et al. Changing neurodevelopment at 8 years in children born extremely preterm since the 1990s. Pediatrics 139, e20164086 (2017).
Haga, M. et al. Changes in in-hospital survival and long-term neurodevelopmental outcomes of extremely preterm infants: a retrospective study of a Japanese tertiary center. J. Pediatr. 255, 166–174.e164 (2023).
Kolb, B. & Gibb, R. Brain Plasticity and Behaviour in the Developing Brain. J. Can. Acad. Child Adolesc. Psychiatry 20, 265–276 (2011).
Orton, J. et al. Early developmental intervention programmes providedpost hospital discharge to prevent motor and cognitive impairment in preterm infants. Cochrane Database Syst. Rev. 2, CD005495 (2024).
Kelly, L. E. et al. Perinatal health services organization for preterm births: a multinational comparison. J. Perinatol. 37, 762–768 (2017).
Swearingen, C., Simpson, P., Cabacungan, E. & Cohen, S. Social disparities negatively impact neonatal follow-up clinic attendance of premature infants discharged from the neonatal intensive care unit. J. Perinatol. 40, 790–797 (2020).
Chin-Lun Hung, G. et al. Socioeconomic disadvantage and neural development from infancy through early childhood. Int. J. Epidemiol. 44, 1889–1899 (2015).
Huhtala, M. et al. Parental psychological well-being and behavioral outcome of very low birth weight infants at 3 years. Pediatrics 129, e937–e944 (2012).
Spittle, A. & Treyvaud, K. The role of early developmental intervention to influence neurobehavioral outcomes of children born preterm. Semin. Perinatol. 40, 542–548 (2016).
Rees, P. et al. Preterm brain injury and neurodevelopmental outcomes: a meta-analysis. Pediatrics 150, e2022057442 (2022).
Tréluyer, L. et al. Intraventricular hemorrhage in very preterm children: mortality and neurodevelopment at age 5. Pediatrics 151, e2022059138 (2023).
Pascal, A. et al. The impact of intraventricular hemorrhage and periventricular leukomalacia on mortality and neurodevelopmental outcome in very preterm and very low birthweight infants: a prospective population-based cohort study. J. Pediatr. 262, 113600 (2023).
Cizmeci, M. N. et al. Periventricular hemorrhagic infarction in very preterm infants: characteristic sonographic findings and association with neurodevelopmental outcome at age 2 years. J. Pediatr. 217, 79–85.e71 (2020).
Chang, Y. S., Park, H. Y. & Park, W. S. The Korean Neonatal Network: An Overview. J Korean Med Sci. 30, S3–S11 (2015).
Hyun, S. E. et al. Early Neurodevelopmental Assessments of Neonates Discharged from the Neonatal Intensive Care Unit: A Physiatrist’s Perspective. Ann. Rehabil. Med. 47, 147–161 (2023).
Chung, H. J. et al. Development of the Korean Developmental Screening Test for Infants and Children (K-Dst). Clin. Exp. Pediatr. 63, 438–446 (2020).
Jang, C. H. et al. Clinical Usefulness of the Korean Developmental Screening Test (K-Dst) for Developmental Delays. Ann. Rehabil. Med. 43, 490–496 (2019).
Johnson, S., Moore, T. & Marlow, N. Using the Bayley-III to assess neurodevelopmental delay: which cut-off should be used?. Pediatr. Res 75, 670–674 (2014).
Jary, S., Whitelaw, A., Walløe, L. & Thoresen, M. Comparison of Bayley-2 and Bayley-3 Scores at 18 Months in Term Infants Following Neonatal Encephalopathy and Therapeutic Hypothermia. Dev. Med. Child Neurol. 55, 1053–1059 (2013).
Gerull, R. et al. Association of growth with neurodevelopment in extremely low gestational age infants: a population-based analysis. Eur. J. Pediatr. 181, 3673–3681 (2022).
Wyckoff, M. H. et al. Part 13: Neonatal Resuscitation: 2015 American Heart Association Guidelines Update for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Circulation 132, S543–S560 (2015).
Kono, Y. Neurodevelopmental Outcomes of Very Low Birth Weight Infants in the Neonatal Research Network of Japan: Importance of Neonatal Intensive Care Unit Graduate Follow-Up. Clin. Exp. Pediatr. 64, 313–321 (2021).
Lugli, L. et al. Neuroprem 2: An Italian Study of Neurodevelopmental Outcomes of Very Low Birth Weight Infants. Front. Pediatr. 9, 697100 (2021).
Hille, E. T. et al. Is Attrition Bias a Problem in Neonatal Follow-Up?. Early Hum. Dev. 81, 901–908 (2005).
Guillén, U. et al. Relationship between attrition and neurodevelopmental impairment rates in extremely preterm infants at 18 to 24 months: a systematic review. Arch. Pediatr. Adolesc. Med. 166, 178–184 (2012).
Spittle, A. J., Treyvaud, K., Lee, K. J., Anderson, P. J. & Doyle, L. W. The role of social risk in an early preventative care programme for infants born very preterm: a randomized controlled trial. Dev. Med. Child Neurol. 60, 54–62 (2018).
Lambiase, C. V. et al. The financial burden experienced by families during NICU hospitalization and after discharge: a single center, survey-based study. Eur. J. Pediatrics 183, 903–913 (2024).
Doyle, L. W. et al. Developmental disability at school age and difficulty obtaining follow-up data. Pediatrics 141, e20173102 (2018).
Yaari, M., Treyvaud, K., Lee, K. J., Doyle, L. W. & Anderson, P. J. Preterm Birth and Maternal Mental Health: Longitudinal Trajectories and Predictors. J. Pediatr. Psychol. 44, 736–747 (2019).
Pace, C. C. et al. Evolution of depression and anxiety symptoms in parents of very preterm infants during the newborn period. JAMA Pediatr. 170, 863–870 (2016).
Neri, E. et al. Developmental dimensions in preterm infants during the 1st year of life: the influence of severity of prematurity and maternal generalized anxiety. Front Psychol. 11, 455 (2020).
Loccoh, E. C. et al. Prevalence and Risk Factors Associated with Non-Attendance in Neurodevelopmental Follow-up Clinic among Infants with CHD. Cardiol. Young. 28, 554–560 (2018).
Bailes, A. F., Reder, R. & Burch, C. Development of guidelines for determining frequency of therapy services in a pediatric medical setting. Pediatr. Phys. Ther. 20, 194–198 (2008).
McManus, B. M., Richardson, Z., Schenkman, M., Murphy, N. & Morrato, E. H. Timing and Intensity of Early Intervention Service Use and Outcomes among a Safety-Net Population of Children. JAMA Netw. Open 2, e187529 (2019).
Fourdain, S. et al. Impacts of an Interdisciplinary Developmental Follow-up Program on Neurodevelopment in Congenital Heart Disease: The Cinc Study. Front. Pediatr. 8, 539451 (2020).
Whitehouse, A. J. O. et al. Effect of preemptive intervention on developmental outcomes among infants showing early signs of autism: a randomized clinical trial of outcomes to diagnosis. JAMA Pediatrics 175, e213298 (2021).
Pritchard, M. A. et al. Risk Determinants in early intervention use during the first postnatal year in children born very preterm. BMC Pediatr. 13, 201 (2013).
Mills, I. S., Doyle, L. W., Cheong, J. L. & Roberts, G. Rates of early intervention services in children born extremely preterm/extremely low birthweight. J. Paediatr. Child Health 54, 74–79 (2018).
Pascal, A. et al. Neurodevelopmental outcome in very preterm and very-low-birthweight infants born over the past decade: a meta-analytic review. Dev. Med. Child Neurol. 60, 342–355 (2018).
Acknowledgements
This research was supported by the National Institute of Health (NIH) research project (2025-ER0601-00#).
Funding
This study was supported by the Soonchunhyang University Research Fund (grant number 2025-0026), which covered publication costs. The funder did not participate in (1) the study design, (2) the data collection, analysis, or interpretation, (3) the manuscript preparation, or (4) the decision to submit the manuscript for publication.
Author information
Authors and Affiliations
Contributions
JY and SPB conceptualized and designed the study. SPB and SYP were responsible for data acquisition and analysis. JY and SPB drafted the manuscript. DHK and WRL critically revised the manuscript. All authors approved the final version before submission.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Consent statement
Participation of the infant in the registration of data in the KNN was approved by the Institutional Review Board (IRB) of each participating center. Written informed consent was obtained from the parents of each participant in the study.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Yun, J., Bae, S.P., Kim, D.H. et al. Early developmental intervention and neurodevelopmental trajectories in preterm infants without severe brain injury. Pediatr Res (2026). https://doi.org/10.1038/s41390-026-04825-8
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41390-026-04825-8