Abstract
Study design
Observational cross-sectional study.
Objectives
Due to weakened pelvic floor muscles, the risk of pelvic organ prolapse (POP) may increase after a spinal cord injury (SCI); hence, the aim of this study was to investigate the occurrence of POP after SCI and to evaluate the need for urogynecological consultations offered to women with SCI.
Setting
Clinic for Spinal Cord Injuries, Rigshospitalet, Denmark.
Methods
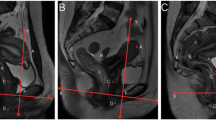
Women with SCI who visited our SCI-clinic during January 2013−January 2018 were offered a specialized urogynecological consultation. Any symptoms of POP, urinary/fecal incontinence, or bladder/bowel emptying problems were registered, and POP was classified according to the POP quantification system during a pelvic examination. Differences in baseline characteristics between women with POP stage 0−1 and POP stage ≥2 were investigated.
Results
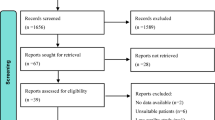
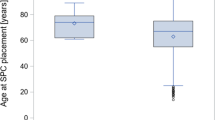
A total of 98 women were included in the study. Fourteen women (14%) reported POP symptoms and 21 women (21%) had anatomical POP stage ≥2. The group with POP stage ≥2 had a significantly higher age, higher parity, more with vaginal delivery, and more postmenopausal women, but the groups did not differ on median time after injury, neurological level, and completeness of injury. A total of 71% experienced urinary incontinence, 27% experienced fecal incontinence, 63% experienced bladder emptying problems, and 70% experienced bowel emptying problems. Consequently, 65% received treatment.
Conclusions
Women with SCI are not in increased risk of developing anatomical POP. Nonetheless, the high occurrence of other urogynecological issues and the high treatment-rate supports the need for specialized urogynecological consultations offered to women with SCI.
Similar content being viewed by others
Log in or create a free account to read this content
Gain free access to this article, as well as selected content from this journal and more on nature.com
or
References
Schopp LH, Sanford TC, Hagglund KJ, Gay JW, Coatney MA. Removing service barriers for women with physical disabilities: promoting accessibility in the gynecologic care setting. J Midwifery Women’s Health. 2002;47:74–9.
Swift SE. The distribution of pelvic organ support in a population of female subjects seen for routine gynecologic health care. Am J Obstet Gynecol. 2000;183:277–85.
Wan L, Liu X. Delayed-onset advanced pelvic organ prolapse after spinal cord injury in a young, nulliparous woman. Int Urogynecol J. 2016;27:825–7.
Ruffion A, Chartier-Kastler E. Specific features of genital prolapse in spinal cord injury patients. Prog Urol. 2007;17:440–1.
Fletcher S, Nosek MA, Rizk DE. Mobility impairments and pelvic health disorders in women: the need for innovative treatment and research. Int Urogynecol J. 2014;25:1003–4.
Elmelund M, Klarskov N, Biering-Sorensen F Prevalence of urinary incontinence in women with spinal cord injury. Spinal Cord 2018; e-pub ahead of print 2018; https://doi.org/10.1038/s41393-018-0157-0
Haylen BT, de Ridder D, Freeman RM, Swift SE, Berghmans B, Lee J, et al. An international urogynecological association (iuga)/international continence society (ics) joint report on the terminology for female pelvic floor dysfunction. Int Urogynecol J. 2010;21:5–26.
Avery K, Donovan J, Peters TJ, Shaw C, Gotoh M, Abrams P. Iciq: a brief and robust measure for evaluating the symptoms and impact of urinary incontinence. Neurourol Urodyn. 2004;23:322–30.
Price N, Jackson SR, Avery K, Brookes ST, Abrams P. Development and psychometric evaluation of the iciq vaginal symptoms questionnaire: the iciq-vs. BJOG. 2006;113:700–12.
Biering-Sorensen F, Craggs M, Kennelly M, Schick E, Wyndaele JJ. International lower urinary tract function basic spinal cord injury data set. Spinal Cord. 2008;46:325–30.
Swift S, Morris S, McKinnie V, Freeman R, Petri E, Scotti RJ, et al. Validation of a simplified technique for using the popq pelvic organ prolapse classification system. Int Urogynecol J Pelvic Floor Dysfunct. 2006;17:615–20.
Biering-Sorensen F, DeVivo MJ, Charlifue S, Chen Y, New PW, Noonan V, et al. International spinal cord injury core data set (version 2.0)-including standardization of reporting. Spinal Cord. 2017;55:759–64.
DeVivo M, Biering-Sorensen F, Charlifue S, Noonan V, Post M, Stripling T, et al. International spinal cord injury core data set. Spinal Cord. 2006;44:535–40.
Kirshblum SC, Burns SP, Biering-Sorensen F, Donovan W, Graves DE, Jha A, et al. International standards for neurological classification of spinal cord injury (revised 2011). J Spinal Cord Med. 2011;34:535–46.
Sundhedsstyrrelsen. Screening for cervical cancer - recommendations. Copenhagen: National Board of Health; 2012.
Horst W, do Valle JB, Silva JC, Gascho CLL. Pelvic organ prolapse: prevalence and risk factors in a brazilian population. Int Urogynecol J. 2017;28:1165–70.
Dillon BE, Seideman CA, Lee D, Greenberg B, Frohman EM, Lemack GE. A surprisingly low prevalence of demonstrable stress urinary incontinence and pelvic organ prolapse in women with multiple sclerosis followed at a tertiary neurogenic bladder clinic. J Urol. 2013;189:976–9.
Lynge E, Andersen B, Christensen J, Ejersbo D, Jochumsen K, Johansen T, et al. Cervical screening in denmark—a success followed by stagnation. Acta Oncol. 2018;57:354–61.
Cheng E, Myers L, Wolf S, Shatin D, Cui XP, Ellison G, et al. Mobility impairments and use of preventive services in women with multiple sclerosis: Observational study. BMJ. 2001;323:968–9.
Iezzoni LI, McCarthy EP, Davis RB, Harris-David L, O’Day B. Use of screening and preventive services among women with disabilities. Am J Med Qual. 2001;16:135–44.
Elmelund M, Oturai PS, Toson B, Biering-Sorensen F. Forty-five-year follow-up on the renal function after spinal cord injury. Spinal Cord. 2016;54:445–51.
Stohrer M, Blok B, Castro-Diaz D, Chartier-Kastler E, Del Popolo G, Kramer G, et al. Eau guidelines on neurogenic lower urinary tract dysfunction. Eur Urol. 2009;56:81–8.
Author contributions
ME was responsible for designing and planning the study, data analysis and interpretation, and writing the report. FB-S contributed to the design and planning of the study, interpretation of the results, and provided feedback on the report. MHB was responsible for data acquisition, contributed to interpretation of the results, and provided feedback on the report. NK contributed to the design and planning of the study, data analysis, interpretation of the results, and provided feedback on the report.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
ME and NK have received paid travel expenses from Contura travel expenses from Contura and MB has received paid travel expenses from Normedi. FB-S has no conflicts of interest to disclose.
Rights and permissions
About this article
Cite this article
Elmelund, M., Biering-Sørensen, F., Bing, M.H. et al. Pelvic organ prolapse and urogynecological assessment in women with spinal cord injury. Spinal Cord 57, 18–25 (2019). https://doi.org/10.1038/s41393-018-0181-0
Received:
Revised:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41393-018-0181-0
This article is cited by
-
Fortifying the foundation: assessing the role of uterine ligament integrity in uterine prolapse and beyond
Archives of Gynecology and Obstetrics (2024)
-
Knowledge Gaps in Urologic Care of Female Spinal Cord Injury Patients
Current Urology Reports (2019)