Abstract
Study design
Cross-sectional.
Objective
Identify the association between secondary health conditions (SHC) and the indirect costs of traumatic spinal cord injury (SCI) based on the pre-injury and post-injury changes in employment and earnings.
Setting
Medical university in the southeastern United States (US).
Methods
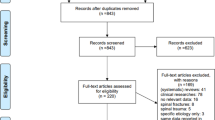
A population-based cohort of 304 participants met the following eligibility criteria: received treatment for acute SCI within the state, residual effects resulting from traumatic SCI, at least 1-year post injury, age between 23 and 64 years at the time of injury onset, and younger than 65 years at the time of study measurement. The indirect costs estimate was measured by the annual forgone earnings and fringe benefits calculated as the difference in the sum of earnings and benefits between before injury and after injury adjusting for inflation in 2019 US dollars. We considered seven SHC in this study: bowel accidents, urine accidents, urinary tract infections, pressure sores, unintentional injury, severe pain, and depressive disorder. We used multivariate ordinary least squares regression models to examine their relationship controlling for age, sex, race/ethnicity, marital status, years of education, injury level, and ambulatory status.
Results
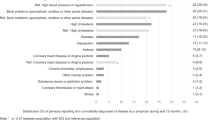
The indirect costs were significantly associated with the total number of SHC and with the individual conditions of bowel accidents, urine accidents, pressure sores, and depressive disorder after controlling for age, sex, race/ethnicity, marital status, years of education, injury level, and ambulatory status.
Conclusions
Preventing SHC relates to better economic consequences for individuals, their families, and society, even after accounting for differences in severity of SCI.
Similar content being viewed by others
Log in or create a free account to read this content
Gain free access to this article, as well as selected content from this journal and more on nature.com
or
Data availability
The data sets generated and/or analyzed during the current study are not publicly available due to the privacy concerns of study participants and are not standardized to be in a publicly interpretable format.
References
Cao Y, Krause JS. Estimation of indirect costs based on employment and earnings changes after spinal cord injury: an observational study. Spinal Cord. 2020. https://doi.org/10.1038/s41393-020-0447-1.
McDaid D, Park AL, Gall A, Purcell M, Bacon M. Understanding and modelling the economic impact of spinal cord injuries in the United Kingdom. Spinal Cord. 2019;57:778–88.
Berkowitz M, Harvey C, Greene C, Wilson S. The economic consequences of traumatic spinal cord injury. New York: Demos Medical Publications; 1992.
DeVivo M, Whiteneck G, Charles E. The economic impact of spinal cord injury. In: Stover S, DeLisa J, Whiteneck G, editors. Spinal cord injury: clinical outcomes from the model systems. Gaithersburg, MD: Aspen Publishers; 1995. p. 234–71.
Stover SL, DeLisa JA, Whiteneck GG. Spinal cord injury: clinical outcomes from the model systems. Gaithersburg, MD: Aspen Publications; 1995.
Krueger H, Noonan VK, Trenaman LM, Joshi P, Rivers CS. The economic burden of traumatic spinal cord injury in Canada. Chronic Dis Inj Can. 2013;33:113–22.
Hammell KW, Miller WC, Forwell SJ, Forman BE, Jacobsen BA. Fatigue and spinal cord injury: a qualitative analysis. Spinal Cord. 2009;47:44–9.
Leduc BE, Lepage Y. Health-related quality of life after spinal cord injury. Disabil Rehabil. 2002;24:196–202.
Lidal IB, Veenstra M, Hjeltnes N, Biering-Sorensen F. Health-related quality of life in persons with long-standing spinal cord injury. Spinal Cord. 2008;46:710–5.
Cao Y, Krause JS, Dipiro N. Risk factors for mortality after spinal cord injury in the USA. Spinal Cord. 2013;51:413–8.
Krause JS, DeVivo MJ, Jackson AB. Health status, community integration, and economic risk factors for mortality after spinal cord injury. Arch Phys Med Rehabil. 2004;85:1764–73.
Meade MA, Forchheimer M, Krause JS, Charlifue S. The influence of secondary conditions on job acquisition and retention in adults with spinal cord injury. Arch Phys Med Rehabil. 2011;92:425–32.
Krause JS, Dismuke-Greer CE, Reed KS, Li C. Employment status, hours working, and gainful earnings after spinal cord injury: relationship with pain, prescription medications for pain, and nonprescription opioid use. Spinal Cord. 2020;58:275–83.
Krause JS, Reed KS, McArdle JJ. A structural analysis of health outcomes after spinal cord injury. J Spinal Cord Med. 2010;33:22–32.
Krause JS, Saunders LL. Risk and protective factors for secondary conditions: A 15-year longitudinal study. Top Spinal Cord Inj Rehabil. 2010;16:22–9.
Cleeland CS. The brief pain inventory: user guide. 2009. http://www.mdanderson.org/education-and-research/departments-programs-and-labs/departments-and-divisions/symptom-research/symptom-assessment-tools/BPI_UserGuide.pdf.
CDC. Behavioral risk factor surveillance system. 2010. http://www.cdc.gov/brfss/questionnaires/pdf-ques/2010brfss.pdf.
Braddom RL. Physical medicine and rehabilitation. 4th ed. Philadelphia: Saunders, an Imprint of Elsevier, Inc; 2010.
McCulloch JM, Kloth LC. Wound healing: evidence-based management. 4th ed. Philadelphia: F.A. Davis Company; 2010.
Krause JS, Dismuke-Greer CE, Jarnecke M, Reed KS. Differential odds of employment and estimation of earnings among those with spinal cord injury. Rehabiitation Couns Bull. 2020;63:67–78.
Krause JS, Dismuke CE, Acuna J, Sligh-Conway C, Walker E, Washington K, et al. Race-ethnicity and poverty after spinal cord injury. Spinal Cord. 2014;52:133–8.
Krause JS, Reed KS. Barriers and facilitators to employment after spinal cord injury: underlying dimensions and their relationship to labor force participation. Spinal Cord. 2011;49:285–91.
Cao Y, DiPiro N, Li C, Roesler J, Krause JS. Behavioral factors and unintentional injuries after spinal cord injury. Arch Phys Med Rehabil. 2020;101:412–7.
Funding
The contents of this publication were developed under grants from the South Carolina Spinal Cord Injury Research Fund (SCSCIRF) grants SCIRF 11-006, SCIRF 09-001, and SCIRF 2017 SI-02. However, those contents do not necessarily represent the policy of the SCSCIRF, and you should not assume endorsement by the state of SC.
Author information
Authors and Affiliations
Contributions
YC was the principal investigator and was responsible for the introduction, analyses, and research methods sections, as well as contributing to the results, discussion, and conclusion. JK was responsible for the discussion and contributed to the overall development and editing of the paper.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
We certify that all applicable institutional and governmental regulations concerning the ethical use of human volunteers were followed during the course of this research.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Cao, Y., Krause, J.S. The association between secondary health conditions and indirect costs after spinal cord injury. Spinal Cord 59, 306–310 (2021). https://doi.org/10.1038/s41393-020-00567-4
Received:
Revised:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41393-020-00567-4
This article is cited by
-
Heart rate variability biofeedback in adults with chronic spinal cord injury: a randomised feasibility study
BMC Neurology (2025)
-
Incidence and mortality of spinal cord injury from 2008 to 2020: a retrospective population-based cohort study in the Piedmont Region, Italy
Spinal Cord (2023)
-
Socioeconomic consequences of traumatic and non-traumatic spinal cord injuries: a Danish nationwide register-based study
Spinal Cord (2022)