Abstract
Study design
A prospective observational study.
Objectives
To depict morphological and functional changes in the cervical nerve roots before and after spinal cord decompression surgery for degenerative cervical myelopathy (DCM).
Setting
A general hospital in Japan.
Methods
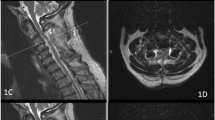
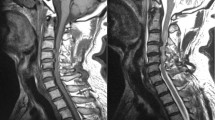
Thirteen DCM patients who underwent posterior spinal cord decompression surgery, laminoplasty or laminectomy, were included in this study. The neural foramen shown on MRI and the cross-sectional area (CSA) of the nerve roots on ultrasound were used to evaluate the C5 and C6 nerve roots. The compound muscle action potentials (CMAPs) of deltoid and biceps muscle were also recorded.
Results
All patients showed sensorimotor functional improvement without the postoperative C5 palsy after surgery. Foraminal stenosis and preoperative CSA of the nerve root: C4/5 foramen and C5 nerve root, C5/6 foramen and C6 nerve root, had no significant correlation (P = 0.53 and 0.08). CSA of the C5 nerve root displayed no significant change before and after surgery (P = 0.2), however, that of the C6 nerve root reduced significantly after surgery (P = 0.038). The amplitude of the deltoid and biceps CMAPs displayed no significant change before and after surgery (P = 0.05 and 0.05).
Conclusion
The C6 nerve root CSA change was observed after spinal cord decompression surgery with functional recovery. However, deltoid and biceps CMAPs amplitude showed no significant change. Independent CSA changes on ultrasound might be useful when conducting a functional evaluation of the postoperative nerve root.
Sponsorship
The Grant of Japan Orthopaedics and Traumatology Research Foundation No. 395.
Similar content being viewed by others
Log in or create a free account to read this content
Gain free access to this article, as well as selected content from this journal and more on nature.com
or
Data archiving
The datasets generated and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Nouri A, Tetreault L, Singh A, Karadimas SK, Fehlings MG. Degenerative cervical myelopathy: epidemiology, genetics, and pathogenesis. Spine. 2015;40:E675–93.
Meacock J, Schramm M, Selvanathan S, Currie S, Stocken D, Jayne D, et al. Systematic review of radiological cervical foraminal grading systems. Neuroradiology. 2021;63:305–16.
Reza Soltani Z, Sajadi S, Tavana B. A comparison of magnetic resonance imaging with electrodiagnostic findings in the evaluation of clinical radiculopathy: a cross-sectional study. Eur Spine J. 2014;23:916–21.
Takeuchi M, Wakao N, Hirasawa A, Murotani K, Kamiya M, Osuka K, et al. Ultrasonography has a diagnostic value in the assessment of cervical radiculopathy: a prospective pilot study. Eur Radio. 2017;27:3467–73.
Takeuchi M, Wakao N, Kamiya M, Hirasawa A, Murotani K, Takayasu M. Simple presurgical method of predicting C5 palsy after cervical laminoplasty using C5 nerve root ultrasonography. J Neurosurg Spine. 2018;29:365–70. https://doi.org/10.3171/2018.2.SPINE171363. Epub 2018 Jul 6.
Japanese Orthopaedic Association Scoring system (17-2) for cervical myelopathy. Nippon Seikeigeka Gakkai Zasshi. J Jpn Orthop Assoc. 1994;68:498.
Compston A. Aids to the investigation of peripheral nerve injuries. Medical Research Council: Nerve Injuries Research Committee. His Majesty’s Stationery Office: 1942; pp. 48 (iii) and 74 figures and 7 diagrams; with aids to the examination of the peripheral nervous system. By Michael O’Brien for the Guarantors of Brain. Saunders Elsevier: 2010; pp. [8] 64 and 94 Figures. Brain: a J Neurol. 2010;133:2838–44.
Koo TK, Li MY. A guideline of selecting and reporting intraclass correlation coefficients for reliability research. J Chiropr Med. 2016;15:155–63.
Kim S, Lee JW, Chai JW, Yoo HJ, Kang Y, Seo J, et al. A New MRI grading system for cervical foraminal stenosis based on Axial T2-Weighted Images. Korean J Radio. 2015;16:1294–302.
Kanda Y. Investigation of the freely available easy-to-use software ‘EZR’ for medical statistics. Bone Marrow Transpl. 2013;48:452–8.
Kadanka Z Jr., Adamova B, Kerkovsky M, Kadanka Z, Dusek L, Jurova B, et al. Predictors of symptomatic myelopathy in degenerative cervical spinal cord compression. Brain Behav. 2017;7:e00797.
Rydevik B, Lundborg G, Bagge U. Effects of graded compression on intraneural blood blow. An in vivo study on rabbit tibial nerve. J hand Surg. 1981;6:3–12.
Cheng X, Long H, Chen W, Xu J, Huang Y, Li F. Three-dimensional alteration of cervical anterior spinal artery and anterior radicular artery in rat model of chronic spinal cord compression by micro-CT. Neurosci Lett. 2015;606:106–12.
Wu S, Chandoo S, Zhu M, Huang K, Wang Y, Wang Z, et al. Is the cervical anterior spinal artery compromised in cervical spondylotic myelopathy patients? Dual-energy computed tomography analysis of cervical anterior spinal. Artery World Neurosurg. 2018;115:e152–9.
Lee YS, Choi E. Ultrasonographic changes after steroid injection in carpal tunnel syndrome. Skelet Radio. 2017;46:1521–30.
Wang JC, Lin KP, Liao KK, Chang YC, Wang KA, Huang YF, et al. Sonographic median nerve change after steroid injection for carpal tunnel syndrome. Muscle Nerve. 2018;58:402–6.
Cartwright MS, White DL, Demar S, Wiesler ER, Sarlikiotis T, Chloros GD, et al. Median nerve changes following steroid injection for carpal tunnel syndrome. Muscle Nerve. 2011;44:25–9.
Kim E, Yoon JS, Kang HJ. Ultrasonographic cross-sectional area of spinal nerve roots in cervical radiculopathy: a pilot study. Am J Phys Med rehabilitation/Assoc Academic Physiatrists. 2015;94:159–64.
Takeuchi M, Wakao N, Kamiya M, Osuka K, Matsuo N, Terasawa T, et al. Morphological distinction of cervical nerve roots associated with motor function in 219 healthy volunteers: a multicenter prospective study. Spine. 2014;39:E944–9.
McGillicuddy JE. Cervical radiculopathy, entrapment neuropathy, and thoracic outlet syndrome: how to differentiate? Invited submission from the Joint Section Meeting on Disorders of the Spine and Peripheral Nerves, March 2004. J Neurosurg Spine. 2004;1:179–87.
Imagama S, Matsuyama Y, Yukawa Y, Kawakami N, Kamiya M, Kanemura T, et al. C5 palsy after cervical laminoplasty: a multicentre study. J bone Jt Surg Br Vol. 2010;92:393–400.
Yoshihara H, Margalit A, Yoneoka D. Incidence of C5 Palsy: meta-analysis and potential etiology. World Neurosurg. 2019;122:e828–37.
Funding
This study was supported by the Grant of Japan Orthopaedics and Traumatology Research Foundation No. 395.
Author information
Authors and Affiliations
Contributions
NT was responsible for designing the study protocols, conducting the research, analysing data, interpreting results, and writing the paper. QH, YY, HM, and TS were involved in recruiting patients and editing the paper.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethics
We certify that all applicable institutional and governmental regulations concerning the ethical use of human volunteers were followed during the course of this research.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Tadokoro, N., Hashimoto, K., Yanagawa, Y. et al. Nerve root morphological and functional changes after degenerative cervical myelopathy surgery: preliminary study using ultrasound and electrophysiology. Spinal Cord 60, 301–305 (2022). https://doi.org/10.1038/s41393-021-00707-4
Received:
Revised:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41393-021-00707-4