Abstract
Background/Objectives
Northeastern Indian region has a high density of marginalised populations with a concerning quality of health services. We observed the trends in prevalence of infectious diseases and nutritional disorders among children under-five years from 2006 to 2020 in the Northeastern states. We also assessed the distribution of their burden by place of residence.
Methods
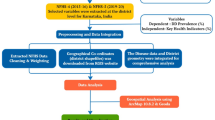
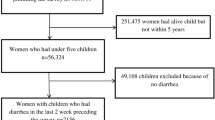
A secondary data analysis of select indicators on infectious diseases and nutritional disorders in seven Northeastern states across three rounds of the National Family Health Survey (2005–06, 2015–16, 2019–20) was undertaken. We calculated outcome indicator mean prevalence, relative change and average annual rates of reduction of the indicators.
Results
A significant relative reduction between 2006–2020 in the prevalence of diarrhoea (0.4 [95CI:0.7,0.1]) at p < 0.05; acute respiratory illness (ARI) (0.7 [95CI:0.1,0.4]), stunting (0.3 [95CI: 0.3,0.12]) and underweight (0.3 [95CI:0.5,0.2]) at p < 0.001 were noted. However, overweight prevalence increased (10.1[95CI:4.3,16.0, p < 0.001]) due to a low annual reduction rate. The highest annual reduction rates were observed in Sikkim and Tripura for diarrhoea and ARI respectively (>10.0%), and in Meghalaya for wasting and severely wasting (6.3%). Rural areas had a higher burden of stunting, wasting (including severe), underweight, anaemia and diarrhoea; overweight was seen in both rural and urban settings.
Conclusion
Significant reductions were observed in ARI, diarrhoea, stunting and underweight prevalence between 2006–2020, with sub-regional variations and a greater burden in rural areas. During this period, overweight prevalence worsened; and anaemia showed a large increase from 2016. To reduce the equity-gap, programmes should be adapted to meet the differential needs of the Northeastern states.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
Data availability
The data supporting the findings of this study are publicly available from NFHS at http://rchiips.org/nfhs/index.shtml; NFHS-3 and NFHS-4 data were obtained from the state reports and NFHS-5 was obtained from the state factsheets.
References
UNICEF, World Health Organization, World Bank. Levels and Trends in Child malnutrition. Key findings of the 2018 edition. 2018.
UNICEF. One is too many- Ending child deaths from pneumonia and Diarrhoea. 2016. Available from: https://data.unicef.org/wp-content/uploads/2016/11/UNICEF-Pneumonia-Diarrhoea-report2016-web-version_final.pdf
UNICEF. Children, food and nutrition-Growing well in a changing world. 2019.
Dandona R, Anil Kumar G, Henry NJ, Joshua V, Ramji S, Gupta SS, et al. Subnational mapping of under-5 and neonatal mortality trends in India: the Global Burden of Disease Study 2000-17. Lancet 2020;395:1640–58.
World Health Organization. Children: improving survival and well-being. 2020. Available from: https://www.who.int/news-room/fact-sheets/detail/children-reducing-mortality
UNICEF. WHO. World Bank: UN DESA. Levels & Trends in Child Mortality 2019. UN IGME Rep. 2019;52.
2020 Global Nutrition Report—Global Nutrition Report. 2020. Available from: https://globalnutritionreport.org/reports/2020-global-nutrition-report/
World Health Organisation. Ending preventable deaths from pneumonia and diarrhoea by 2025. 2013. Available from: https://www.who.int/news/item/10-04-2013-ending-preventable-deaths-from-pneumonia-and-diarrhoea-by-2025
Sachs J, Schmidt-Traub, Kroll G, Fuller G The Sustainable Development Goals and COVID-19. Sustainable Development Report 2020. 2020. Available from: www.pica-publishing.com
Global Hunger Index Scores by 2021 GHI Rank - Global Hunger Index (GHI). 2021. Available from: https://www.globalhungerindex.org/ranking.html
Liu L, Chu Y, Oza S, Hogan D, Perin J, Bassani DG, et al. National, regional, and state-level all-cause and cause-specific under-5 mortality in India in 2000–15: a systematic analysis with implications for the Sustainable Development Goals. Lancet Glob Heal. 2019;7:e721–34.
Ministry of Health and Family Welfare (MoHFW), Government of India, UNICEF, Population Council. Comprehensive National Nutrition Survey (CNNS) National Report 2016-2018. New Delhi; 2109.
Press Information Bureau., Government of India., Ministry of Health and Family Welfare. Nutritional Rehabilitation Centres. 2018. Available from: https://pib.gov.in/newsite/PrintRelease.aspx?relid=186712
National food security Portal. Dept. of food and public distribution. Governement of India. National Food Security Act, (NFSA) 2013. 2013. Available from: https://nfsa.gov.in/portal/NFSA-Act
International Institute for Population Sciences. National Family Health Survey. Mumbai; Available from: http://rchiips.org/nfhs/
Office of the Registrar General & Census Commissioner. India. Census 2011 India. 2011. Available from: https://www.census2011.co.in/
Reserve Bank of India. Handbook of Statistics on Indian States. 2021. Available from: https://m.rbi.org.in/scripts/AnnualPublications.aspx?head=Handbook of Statistics on Indian States
Das TK, Das Gupta I, Haldar SK, Mitra S Conflicts and Socioeconomic Consequences in Northeast India. Asian Journal of Humanities and Social Studies. 2015. Available from: https://www.researchgate.net/publication/279200696
Singh KD, Alagarajan M, Ladusingh L. What explains child malnutrition of indigenous people of Northeast India? PLoS ONE. 2015;10:e0130567.
National Family Health Survey 2019-20: DATA QUALITY ASSURANCE AND QUALITY CONTROL MECHANISMS. 2021.
StataCorp. Stata Statistical Software: Release 16. College Station, TX: StataCorp LLC; 2019.
Statistics and Monitoring Section. Division of Policy and Practice. UNICEF. Technical Note: How to calculate average annual rate of reduction (AARR) of underweight prevalence—UNICEF DATA. 2007. Available from: https://data.unicef.org/resources/technical-note-calculate-average-annual-rate-reduction-aarr-underweight-prevalence/
Swaminathan S, Hemalatha R, Pandey A, Kassebaum NJ, Laxmaiah A, Longvah T, et al. The burden of child and maternal malnutrition and trends in its indicators in the states of India: the Global Burden of Disease Study 1990–2017. Lancet Child Adolesc Heal. 2019;3:855–70.
WHO/UNICEF. WHO/UNICEF discussion paper: The extension of the 2025 maternal, infant and young child nutrition targets to 2030—UNICEF DATA. 2019. Available from: https://data.unicef.org/resources/who-unicef-discussion-paper-nutrition-targets/
Press Information Bureau, Government of India., Ministry of Women and Child Development. PM launches National Nutrition Mission, and pan India expansion of Beti Bachao Beti Padhao, at Jhunjhunu in Rajasthan. 2018. Available from: https://pib.gov.in/newsite/PrintRelease.aspx?relid=177166
Emergency Nutrition Network. Undersized Indian children: nutrients-starved or hungry for development. Field Exchange 59. Emergency Nutrition Network (ENN); 2019. p. 41. Available from: www.ennonline.net/fex/59/undersizedindianchildren. Accessed Feb 2021
Drèze J, Gupta A, Parashar SA, Sharma K. Pauses and Reversals of Infant Mortality Decline in India in 2017 and 2018. SSRN Electronic Journal. 2020. Available from: https://www.ssrn.com/abstract=3727001. Accessed Feb 2022
FAO UN, WFP, WHO, UNICEF, IFAD. Transforming Food Systems for Affordable Healthy Diets. The State of Food Security and Nutrition in the World 2020. 2020.
Jith JR, Bedamatta R. Child undernutrition in the states of india: an analysis based on change in composite index of anthropometric failure from 2006 to 2016. Rev Dev Chang. 2021;26:104–26.
Loukrakpam B, Rajendran A, Madhari RS, Boiroju NK, Longvah T. Dietary adequacy and nutritional status of Meitei community of Manipur, Northeast India. Matern Child Nutr. 2020;16(S3):1–12.
Chyne DAL, Meshram II, Rajendran A, Kodali V, Getti N, Roy P, et al. Nutritional status, food insecurity, and biodiversity among the Khasi in Meghalaya, North-East India. Matern Child Nutr. 2017;13:e12557.
Longvah T, Khutsoh B, Meshram II, Krishna S, Kodali V, Roy P, et al. Mother and child nutrition among the Chakhesang tribe in the state of Nagaland, North-East India. Matern Child Nutr. 2017;13:1–12.
Rajbangshi PR, Nambiar D. “who will stand up for us?” the social determinants of health of women tea plantation workers in India. Int J Equity Health. 2020;19:1–10.
Myatt M, Khara T, Schoenbuchner S, Pietzsch S, Dolan C, Lelijveld N, et al. Children who are both wasted and stunted are also underweight and have a high risk of death: a descriptive epidemiology of multiple anthropometric deficits using data from 51 countries. Arch Public Heal. 2018;76:28.
Ganesan L, Kashyap A. Problems and prospects of implementing ICDS in the States of Tamil Nadu and Assam. Shanlax. Int J Econ. 2016;4:53–63.
Barua K, Baruah R. Application of growth monitoring charts by health care providers in Village Health and Nutrition Day (VHND) setting in rural Kamrup. Indian J Community Heal. 2015;26:322–6.
Ministry of Health and Family Welfare. Ministry of Health and Family Welfare Government of India Programme for Promotion of Breastfeeding. 2016. Available from: https://nhm.gov.in/MAA/Operational_Guidelines.pdf
Stegmuller AR, Self A, Litvin K, Roberton T. How is the Lives Saved Tool (LiST) used in the global health community? Results of a mixed-methods LiST user study. BMC Public Health 2017;17(Suppl 4):773.
UNICEF, World Health Organization, World Bank. Levels and trends in child malnutrition. 2018.
Monasta L, Batty GD, Cattaneo A, Lutje V, Ronfani L, Van Lenthe FJ, et al. Early-life determinants of overweight and obesity: a review of systematic reviews. Obes Rev. 2010;11:695–708.
Weng SF, Redsell SA, Swift JA, Yang M, Glazebrook CP. Systematic review and meta-analyses of risk factors for childhood overweight identifiable during infancy. Arch Dis Child. 2012;97:1019–26.
Salam N, Azam S. Prevalence and distribution of soil-transmitted helminth infections in India. BMC Public Health. 2017;17:201.
Pasricha SR, Black J, Muthayya S, Shet A, Bhat V, Nagaraj S, et al. Determinants of anemia among young children in rural India. Pediatrics 2010;126:140.
Ngui R, Lim YAL, Chong Kin L, Sek Chuen C, Jaffar S. Association between anaemia, iron deficiency anaemia, neglected parasitic infections and socioeconomic factors in rural children of West Malaysia. de Silva N, editor. PLoS Negl Trop Dis. 2012;6:e1550.
Molla E, Mamo H. Soil-transmitted helminth infections, anemia and undernutrition among schoolchildren in Yirgacheffee, South Ethiopia. BMC Res Notes. 2018;11:585.
Douglas NM, Lampah DA, Kenangalem E, Simpson JA, Poespoprodjo JR, Sugiarto P, et al. Major Burden of Severe Anemia from Non-Falciparum Malaria Species in Southern Papua: A Hospital-Based Surveillance Study. Hviid L, editor. PLoS Med. 2013;10:e1001575.
Baranwal A, Baranwal A, Roy N. Association of household environment and prevalence of anemia among children under-5 in India. Front Public Heal. 2014;2:196.
Adolescent Division. Ministry of Health and Family Welfare. Government of India. Guidelines for Control of Iron Deficiency Anaemia. 2018. Available from: http://nhm.gov.in/images/pdf/programmes/wifs/guidelines/Guidelines_for_Control_of_Iron_Deficiency_Anaemia.pdf
Poshan Abhiyan. National Health Mission. An introduction to Anemia Mukt Bharat. 2019. Available from: https://anemiamuktbharat.info/wp-content/uploads/2019/09/INFO-sheet-3-About-Anemia-Mukt-Bharat.pdf
Susan K, Guy P, Grace E, Bart van den B. Determinants of stunting and overweight among young children and adolescents in sub-Saharan Africa. Food Nutr Bull. 2014;35:167–78.
Acknowledgements
The authors thank NFHS for their data. The authors also appreciate the support of Solomon Salve from Oxford Policy Management for reviewing the manuscript. No funding was sought for this study.
Author information
Authors and Affiliations
Contributions
A.M. was responsible for conceiving and designing the study. She drafted the manuscript, extracted the data, conducted the analyses, and wrote the Results and Discussion sections. She coordinated with co-authors and integrated the feedback, and revised the manuscript. R.R. was responsible for rechecking the data analyses and writing the initial Introduction. She also reviewed the complete manuscript. R.P. was responsible for conceiving and designing the study. He reviewed the draft, provided feedback and revised the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Mukherjee, A., Rizu & Parashar, R. Longitudinal trends in the health outcomes among children of the North Eastern States of India: a comparative analysis using national DHS data from 2006 to 2020. Eur J Clin Nutr 76, 1528–1535 (2022). https://doi.org/10.1038/s41430-022-01147-w
Received:
Revised:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41430-022-01147-w