Abstract
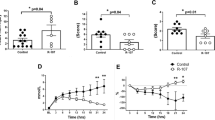
Although vessel-sealing systems have been shown useful for dissection of small-diameter vessels, no studies to date have evaluated the optimal angle of dissection. Lateral thermal damage to a canine pulmonary artery was assessed microscopically. Burst pressure was compared in swine carotid arteries undergoing orthogonal and oblique dissections to determine the safer dissection technique. Histological analysis of a canine model revealed a thermal spread of approximately 1.3 mm. Burst pressure comparison showed no significant differences between orthogonal and oblique dissection angles (829.2 mmHg [range 608–1214 mmHg] vs. 949.1 mmHg [range, 593–1306 mmHg], P = 0.206). In a surrogate arterial model, burst pressure did not differ between orthogonal and oblique cuts. Given histologically limited lateral thermal spread on PA, angle may be less critical than avoiding vessel tension. These findings may contribute to the safer application of vessel-sealing systems in patients undergoing minimally invasive thoracic surgery.
Similar content being viewed by others
Data availability
The datasets used and/or analysed during the current study are available from the corresponding author on reasonable request.
References
Yoshida, K. et al. Feasibility of using a vessel sealing system in a human pulmonary lobectomy: a retrospective comparison of this procedure with or without a vessel sealing system. Ann. Thorac. Cardiovasc. Surg. 20, 353–358 (2014).
Miyajima, M. et al. Vessel sealing system for video-assisted lung resection for cancer reduces chylothorax and bleeding. J. Thorac. Dis. 13, 3458–3466 (2021).
Timm, R. W. et al. Sealing vessels up to 7 mm in diameter solely with ultrasonic technology. Med. Devices (Auckl). 7, 263–271 (2014).
Toishi, M. et al. Usefulness of vessel-sealing devices for ≤ 7 mm diameter vessels: a randomized controlled trial for human thoracoscopic lobectomy in primary lung cancer. Interact. Cardiovasc. Thorac. Surg. 19, 448–455 (2014).
Oyama, S. et al. A new method using a vessel-sealing system provides coagulation effects to various types of bleeding with less thermal damage. Surg. Endosc. 35, 1453–1464 (2021).
Hefermehl, L. J. et al. Lateral temperature spread of monopolar, bipolar and ultrasonic instruments for robot-assisted laparoscopic surgery. BJU Int. 114, 245–252 (2014).
Smith, C. T., Zarebczan, B., Alhefdhi, A. & Chen, H. Infrared thermographic profiles of vessel sealing devices on thyroid parenchyma. J. Surg. Res. 170, 64–68 (2011).
Družijanić, N., Pogorelić, Z., Perko, Z., Mrklić, I. & Tomić, S. Comparison of lateral thermal damage of the human peritoneum using monopolar diathermy, harmonic scalpel and LigaSure. Can. J. Surg. 55, 317–321 (2012).
Özyurtkan, M. O., Kaba, E. & Toker, A. Technological innovation in video-assisted thoracic surgery. J. Vis. Surg. 3, 20 (2017).
Miyajima, M. et al. Interlobar division using vessel-sealing system in robot-assisted pulmonary lobectomy. JTCVS Tech. 13, 211–216 (2022).
Okada, M. et al. Prospective feasibility study of sealing pulmonary vessels with energy in lung surgery. J. Thorac. Cardiovasc. Surg. 157, 388–395 (2019).
Hayami, M. et al. Lateral thermal spread induced by energy devices: a Porcine model to evaluate the influence on the recurrent laryngeal nerve. Surg. Endosc. 33, 4153–4163 (2019).
Hayami, M. et al. Steam induced by the activation of energy devices under a wet condition May cause thermal injury. Surg. Endosc. 34, 2295–2302 (2020).
Lesser, T. G., Wolfram, F. & Boltze, C. Sealing of pulmonary arteries with ligasure: in vivo and ex vivo examinations. J. Thorac. Cardiovasc. Surg. 145, 1525–1528 (2013).
Voegele, A. C., Korvick, D. L., Gutierrez, M., Clymer, J. W. & Amaral, J. F. Perpendicular blood vessel seals are stronger than those made at an angle. J. Laparoendosc. Adv. Surg. Tech. 23, 669–672 (2013).
Acknowledgements
The authors wish to thank Takahisa Orita, Yukihiro Suzuki and Taichi Orikasa for contributing to the analysis and assisting with the preparation of the experiment.
Funding
The authors have no funding sources to disclose.
Author information
Authors and Affiliations
Contributions
Yuichiro Ueda conceived and designed the study, performed the experiments, analyzed the data, and drafted the manuscript. Jun-ichi Wakahara, So Miyahara, Hiroyasu Nakajima, and Yoshiko Masuda contributed to data acquisition and interpretation. Fumihiro Shoji and Takeshi Shiraishi provided critical revisions for important intellectual content. Toshihiko Sato supervised the study and approved the final version of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Supplementary Material 1
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Ueda, Y., Wakahara, Ji., Miyahara, S. et al. Optimizing the dissection of small-diameter pulmonary vessels using vessel-sealing systems. Sci Rep (2026). https://doi.org/10.1038/s41598-026-39741-8
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-026-39741-8