Abstract
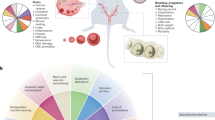
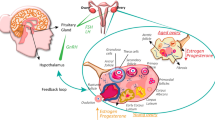
People today are choosing to have children later in life, often in their thirties and forties, when their fertility is in decline. We sought to identify and compile effective methods for improving either male or female fertility in this context of advanced reproductive age. We found few clinical studies with strong evidence for therapeutics that mitigate reproductive aging or extend fertility; however, this Perspective summarizes the range of emerging experimental strategies under development. Preclinical studies, in mouse models of aging, have identified pharmaceutical candidates that improve egg and sperm quality. Further, a diverse array of medically assisted reproduction methodologies, including those that stimulate rare ovarian follicles and rejuvenate egg quality using mitochondria, may have future utility for older patients. Finally, we highlight the many knowledge gaps and possible future directions in the field of therapeutics to extend the age of healthy human reproduction.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$32.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 digital issues and online access to articles
$119.00 per year
only $9.92 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Morse, A. Fertility rates: declined for younger women, increased for older women. Stable Fertility Rates 1990–2019 Mask Distinct Variations by Age https://www.census.gov/library/stories/2022/04/fertility-rates-declined-for-younger-women-increased-for-older-women.html (2022).
Fitzpatrick, K. E., Tuffnell, D., Kurinczuk, J. J. & Knight, M. Pregnancy at very advanced maternal age: a UK population-based cohort study. BJOG 124, 1097–1106 (2017).
Shan, D. et al. Pregnancy outcomes in women of advanced maternal age: a retrospective cohort study from China. Sci. Rep. 8, 12239 (2018).
Australian Institute of Health and Welfare. Australia’s mothers and babies. https://www.aihw.gov.au/reports/mothers-babies/australias-mothers-babies/contents/about (2023).
Martin, J. A., Hamilton, B. E. & Osterman, M. J. K. Births in the United States, 2015 NCHS Data Brief https://stacks.cdc.gov/view/cdc/41352 (2016).
Office for National Statistics. Birth characteristics in England and Wales: 2022. ONS https://www.ons.gov.uk/peoplepopulationandcommunity/birthsdeathsandmarriages/livebirths/bulletins/birthcharacteristicsinenglandandwales/2022 (2024).
Broekmans, F. J., Soules, M. R. & Fauser, B. C. Ovarian aging: mechanisms and clinical consequences. Endocr. Rev. 30, 465–493 (2009).
Heffner, L. J. Advanced maternal age–how old is too old? N. Engl. J. Med. 351, 1927–1929 (2004).
Mathieu, C., Ecochard, R., Bied, V., Lornage, J. & Czyba, J. C. Cumulative conception rate following intrauterine artificial insemination with husband’s spermatozoa: influence of husband’s age. Hum. Reprod. 10, 1090–1097 (1995).
Fitzgerald, O., Harris, K., Paul, R. C. & Chambers, G. M. Assisted reproductive technology in Australia and New Zealand 2015 (National Perinatal Epidemiology and Statistics Unit, the University of New South Wales Sydney, Sydney, 2017).
Slama, R. et al. Influence of paternal age on the risk of spontaneous abortion. Am. J. Epidemiol. 161, 816–823 (2005).
du Fosse, N. A., van der Hoorn, M. P., van Lith, J. M. M., le Cessie, S. & Lashley, E. Advanced paternal age is associated with an increased risk of spontaneous miscarriage: a systematic review and meta-analysis. Hum. Reprod. Update 26, 650–669 (2020).
van Noord-Zaadstra, B. M. et al. Delaying childbearing: effect of age on fecundity and outcome of pregnancy. BMJ 302, 1361–1365 (1991).
Mishra, G. D. et al. Optimising health after early menopause. Lancet 403, 958–968 (2024).
Laven, J. S. E., Visser, J. A., Uitterlinden, A. G., Vermeij, W. P. & Hoeijmakers, J. H. J. Menopause: genome stability as new paradigm. Maturitas 92, 15–23 (2016).
Ruth, K. S. et al. Genetic insights into biological mechanisms governing human ovarian ageing. Nature 596, 393–397 (2021).
Ruth, K. S. et al. Events in early life are associated with female reproductive ageing: a UK Biobank study. Sci. Rep. 6, 24710 (2016).
Roman Lay, A. A., do Nascimento, C. F., Horta, B. L. & Dias Porto Chiavegatto Filho, A. Reproductive factors and age at natural menopause: a systematic review and meta-analysis. Maturitas 131, 57–64 (2020).
Baker, T. G. A quantitative and cytological study of germ cells in human ovaries. Proc. R. Soc. Lond. B Biol. Sci. 158, 417–433 (1963).
Richards, J. S. & Pangas, S. A. The ovary: basic biology and clinical implications. J. Clin. Invest. 120, 963–972 (2010).
Kinnear, H. M. et al. The ovarian stroma as a new frontier. Reproduction 160, R25–R39 (2020).
Kerr, J. B., Myers, M. & Anderson, R. A. The dynamics of the primordial follicle reserve. Reproduction 146, R205–R215 (2013).
Richardson, S. J., Senikas, V. & Nelson, J. F. Follicular depletion during the menopausal transition: evidence for accelerated loss and ultimate exhaustion. J. Clin. Endocrinol. Metab. 65, 1231–1237 (1987).
Faddy, M. J., Gosden, R. G., Gougeon, A., Richardson, S. J. & Nelson, J. F. Accelerated disappearance of ovarian follicles in mid-life: implications for forecasting menopause. Hum. Reprod. 7, 1342–1346 (1992).
Hainaut, M. & Clarke, H. J. Germ cells of the mammalian female: a limited or renewable resource? Biol. Reprod. 105, 774–788 (2021).
Babayev, E. & Duncan, F. E. Age-associated changes in cumulus cells and follicular fluid: the local oocyte microenvironment as a determinant of gamete quality. Biol. Reprod. 106, 351–365 (2022).
Morimoto, A. et al. Granulosa cell metabolism at ovulation correlates with oocyte competence and is disrupted by obesity and aging. Hum. Reprod. 39, 2053–2066 (2024).
Centers for Disease Control and Prevention. 2019 Assisted Reproductive Technology Fertility Clinic and National Summary Report (CDC, 2021).
Charalambous, C., Webster, A. & Schuh, M. Aneuploidy in mammalian oocytes and the impact of maternal ageing. Nat. Rev. Mol. Cell Biol. 24, 27–44 (2023).
Nagaoka, S. I., Hassold, T. J. & Hunt, P. A. Human aneuploidy: mechanisms and new insights into an age-old problem. Nat. Rev. Genet. 13, 493–504 (2012).
Adhikari, D., Lee, I. W., Yuen, W. S. & Carroll, J. Oocyte mitochondria-key regulators of oocyte function and potential therapeutic targets for improving fertility. Biol. Reprod. 106, 366–377 (2022).
May-Panloup, P. et al. Ovarian ageing: the role of mitochondria in oocytes and follicles. Hum. Reprod. Update 22, 725–743 (2016).
Pasquariello, R. et al. Alterations in oocyte mitochondrial number and function are related to spindle defects and occur with maternal aging in mice and humans. Biol. Reprod. 100, 971–981 (2019).
Wilding, M. et al. Mitochondrial aggregation patterns and activity in human oocytes and preimplantation embryos. Hum. Reprod. 16, 909–917 (2001).
Morimoto, N. et al. Mitochondrial oxygen consumption rate of human embryos declines with maternal age. J. Assist Reprod. Genet. 37, 1815–1821 (2020).
Al-Zubaidi, U. et al. Mitochondria-targeted therapeutics, MitoQ and BGP-15, reverse aging-associated meiotic spindle defects in mouse and human oocytes. Hum. Reprod. 36, 771–784 (2021).
Wang, H. et al. Rejuvenation of aged oocyte through exposure to young follicular microenvironment. Nat. Aging https://doi.org/10.1038/s43587-024-00697-x (2024).
Mihalas, B. P., De Iuliis, G. N., Redgrove, K. A., McLaughlin, E. A. & Nixon, B. The lipid peroxidation product 4-hydroxynonenal contributes to oxidative stress-mediated deterioration of the ageing oocyte. Sci. Rep. 7, 6247 (2017).
Ben-Meir, A. et al. Coenzyme Q10 restores oocyte mitochondrial function and fertility during reproductive aging. Aging Cell 14, 887–895 (2015).
Zhang, Y. et al. Polyamine metabolite spermidine rejuvenates oocyte quality by enhancing mitophagy during female reproductive aging. Nat. Aging 3, 1372–1386 (2023).
Bertoldo, M. J. et al. NAD+ Repletion rescues female fertility during reproductive aging. Cell Rep. 30, 1670–1681 (2020).
McCloskey, C. W. et al. Metformin abrogates age-associated ovarian fibrosis. Clin. Cancer Res. 26, 632–642 (2020).
Amargant, F. et al. Ovarian stiffness increases with age in the mammalian ovary and depends on collagen and hyaluronan matrices. Aging Cell 19, e13259 (2020).
Umehara, T. et al. Female reproductive life span is extended by targeted removal of fibrotic collagen from the mouse ovary. Sci. Adv. https://doi.org/10.1126/sciadv.abn4564 (2022).
Wang, S. et al. Single-cell transcriptomic atlas of primate ovarian aging. Cell 180, 585–600 (2020).
Mara, J. N. et al. Ovulation and ovarian wound healing are impaired with advanced reproductive age. Aging 12, 9686–9713 (2020).
Zhou, C. et al. Single-Cell atlas of human ovaries reveals the role of the pyroptotic macrophage in ovarian aging. Adv. Sci. 11, e2305175 (2024).
Wu, M. et al. Spatiotemporal transcriptomic changes of human ovarian aging and the regulatory role of FOXP1. Nat. Aging 4, 527–545 (2024).
Ben Yaakov, T., Wasserman, T., Aknin, E. & Savir, Y. Single-cell analysis of the aged ovarian immune system reveals a shift towards adaptive immunity and attenuated cell function. Elife https://doi.org/10.7554/eLife.74915 (2023).
Ansere, V. A. et al. Cellular hallmarks of aging emerge in the ovary prior to primordial follicle depletion. Mech. Ageing Dev. https://doi.org/10.1016/j.mad.2020.111425 (2021).
Isola, J. V. V. et al. A single-cell atlas of the aging mouse ovary. Nat. Aging https://doi.org/10.1038/s43587-023-00552-5 (2024).
Briley, S. M. et al. Reproductive age-associated fibrosis in the stroma of the mammalian ovary. Reproduction 152, 245–260 (2016).
West, E. R., Xu, M., Woodruff, T. K. & Shea, L. D. Physical properties of alginate hydrogels and their effects on in vitro follicle development. Biomaterials 28, 4439–4448 (2007).
Appiah, D., Nwabuo, C. C., Ebong, I. A., Wellons, M. F. & Winters, S. J. Trends in age at natural menopause and reproductive life span among US women, 1959–2018. JAMA 325, 1328–1330, (2021).
Chatzidaki, E. E. et al. Ovulation suppression protects against chromosomal abnormalities in mouse eggs at advanced maternal age. Curr. Biol. 31, 4038–4051 (2021).
Brown, A. M. & McCarthy, H. E. The effect of CoQ10 supplementation on ART treatment and oocyte quality in older women. Hum. Fertil. 26, 1544–1552 (2023).
Gat, I. et al. The use of coenzyme Q10 and DHEA during IUI and IVF cycles in patients with decreased ovarian reserve. Gynecol. Endocrinol. 32, 534–537 (2016).
Reiter, R. J. et al. Melatonin as an antioxidant: biochemical mechanisms and pathophysiological implications in humans. Acta Biochim. Pol. 50, 1129–1146 (2003).
Hu, K. L., Ye, X. H., Wang, S. W. & Zhang, D. Melatonin application in assisted reproductive technology: a systematic review and meta-analysis of randomized trials. Front. Endocrinol. https://doi.org/10.3389/fendo.2020.00160 (2020).
Zhang, J. et al. Efficacy of dehydroepiandrosterone priming in women with poor ovarian response undergoing IVF/ICSI: a meta-analysis. Front. Endocrinol. 14, 1156280 (2023).
Chu, Q., Yu, Y. X., Zhang, J. Z., Zhang, Y. T. & Yu, J. P. Effects of flaxseed oil supplementation on metaphase II oocyte rates in IVF cycles with decreased ovarian reserve: a randomized controlled trial. Front. Endocrinol. https://doi.org/10.3389/fendo.2024.1280760 (2024).
Hart, R. J. Nutritional supplements and IVF: an evidence-based approach. Reprod. Biomed. Online 48, 103770 (2024).
Umehara, T. et al. The acceleration of reproductive aging in Nrg1flox/flox;Cyp19-Cre female mice. Aging Cell 16, 1288–1299 (2017).
Flurkey, K., Currer, J. M. & Harrison, D. E. In The Mouse in Biomedical Research (eds. J. G. Fox et al.) 637–672 (Academic Press, 2007).
Lliberos, C. et al. Evaluation of inflammation and follicle depletion during ovarian ageing in mice. Sci. Rep. 11, 278 (2021).
Kanda, A., Nobukiyo, A. & Sotomaru, Y. Effect of cetrorelix administration on ovarian stimulation in aged mice. Exp. Anim. 70, 31–36 (2021).
Qin, X. S. et al. TrkB agonist antibody ameliorates fertility deficits in aged and cyclophosphamide-induced premature ovarian failure model mice. Nat. Commun. https://doi.org/10.1038/s41467-022-28611-2 (2022).
Zhang, H. et al. C-type natriuretic peptide improves maternally aged oocytes quality by inhibiting excessive PINK1/Parkin-mediated mitophagy. Elife https://doi.org/10.7554/eLife.88523 (2023).
Tarin, J. J., Perez-Albala, S. & Cano, A. Oral antioxidants counteract the negative effects of female aging on oocyte quantity and quality in the mouse. Mol. Reprod. Dev. 61, 385–397 (2002).
Murphy, M. P. & Smith, R. A. Targeting antioxidants to mitochondria by conjugation to lipophilic cations. Annu. Rev. Pharmacol. Toxicol. 47, 629–656 (2007).
Sumegi, K. et al. BGP-15 protects against oxidative stress- or lipopolysaccharide-induced mitochondrial destabilization and reduces mitochondrial production of reactive oxygen species. PLoS ONE 12, e0169372 (2017).
Lin, H. Y. et al. 2,3,5,4′-tetrahydroxystilbene-2-β-d-glucoside improves female ovarian aging. Front. Cell Dev. Biol. https://doi.org/10.3389/fcell.2022.862045 (2022).
Li, C. et al. Melatonin ameliorates the advanced maternal age-associated meiotic defects in oocytes through the SIRT2-dependent H4K16 deacetylation pathway. Aging 12, 1610–1623 (2020).
Novelle, M. G., Ali, A., Dieguez, C., Bernier, M. & de Cabo, R. Metformin: a hopeful promise in aging research. Cold Spring Harb. Perspect. Med. 6, a025932 (2016).
Dou, X. W. et al. Short-term rapamycin treatment increases ovarian lifespan in young and middle-aged female mice. Aging Cell 16, 825–836 (2017).
Qin, X. et al. Metformin prevents murine ovarian aging. Aging 11, 3785–3794 (2019).
Miao, Y. L., Cui, Z. K., Gao, Q., Rui, R. & Xiong, B. Nicotinamide mononucleotide supplementation reverses the declining quality of maternally aged oocytes. Cell Rep. https://doi.org/10.1016/j.celrep.2020.107987 (2020).
Huang, P. et al. Long-term treatment of nicotinamide mononucleotide improved age-related diminished ovary reserve through enhancing the mitophagy level of granulosa cells in mice. J. Nutr. Biochem. https://doi.org/10.1016/j.jnutbio.2021.108911 (2022).
Yang, Q. L. et al. Increasing ovarian NAD+ levels improve mitochondrial functions and reverse ovarian aging. Free Radic. Biol. Med. 156, 1–10 (2020).
Yang, Q. L. et al. NADase CD38 is a key determinant of ovarian aging. Nat. Aging https://doi.org/10.1038/s43587-023-00532-9 (2024).
Nehra, D. et al. Prolonging the female reproductive lifespan and improving egg quality with dietary omega-3 fatty acids. Aging Cell 11, 1046–1054 (2012).
Amargant, F., Magalhaes, C., Pritchard, M. T. & Duncan, F. E. Systemic low-dose anti-fibrotic treatment attenuates ovarian aging in the mouse. Geroscience https://doi.org/10.1007/s11357-024-01322-w (2024).
Navarro-Pando, J. M. et al. Inhibition of the NLRP3 inflammasome prevents ovarian aging. Sci. Adv. https://doi.org/10.1126/sciadv.abc7409 (2021).
Landry, D. A. et al. Metformin prevents age-associated ovarian fibrosis by modulating the immune landscape in female mice. Sci. Adv. https://doi.org/10.1126/sciadv.abq1475 (2022).
Esencan, E., Simsek, B. & Seli, E. Analysis of female demographics in the United States: life expectancy, education, employment, family building decisions, and fertility service utilization. Curr. Opin. Obstet. Gynecol. 33, 170–177 (2021).
Adamson, G. D. et al. International Committee for Monitoring Assisted Reproductive Technology: world report on assisted reproductive technology, 2011. Fertil. Steril. 110, 1067–1080 (2018).
Chambers, G. et al. International Committee for Monitoring Assisted Reproductive Technologies world report: assisted reproductive technology, 2014. Hum. Reprod. 36, 2921–2934 (2021).
Human Fertilisation and Embryology Authority. Fertility treatment 2018: trends and figures. HFEA https://www.hfea.gov.uk/about-us/publications/research-and-data/fertility-treatment-2018-trends-and-figures/ (2020).
Devesa, M. et al. Cumulative live birth rates and number of oocytes retrieved in women of advanced age. A single centre analysis including 4500 women ≥38 years old. Hum. Reprod. 33, 2010–2017 (2018).
Cimadomo, D. et al. Impact of maternal age on oocyte and embryo competence. Front. Endocrinol. 9, 327 (2018).
Wu, Z., Liu, K. & Zhang, C. Clinical applications of in vitro primordial follicle activation. Curr. Opin. Endocr. Metab. Res. 18, 194–200 (2021).
Song, Y. et al. The remodeling of ovarian function: targeted delivery strategies for mesenchymal stem cells and their derived extracellular vesicles. Stem Cell Res. Ther. 15, 90 (2024).
Esfandyari, S. et al. Mesenchymal stem cells as a bio organ for treatment of female infertility. Cells https://doi.org/10.3390/cells9102253 (2020).
Zafardoust, S. et al. The effects of intraovarian injection of autologous menstrual blood-derived mesenchymal stromal cells on pregnancy outcomes in women with poor ovarian response. Stem Cell Res. Ther. 14, 332 (2023).
Tian, C. et al. Bone marrow mesenchymal stem cells derived from juvenile macaques reversed ovarian ageing in elderly macaques. Stem Cell Res. Ther. 12, 460 (2021).
Herlihy, N. S. et al. Effect of intraovarian platelet-rich plasma injection on IVF outcomes in women with poor ovarian response: the PROVA randomized controlled trial. Hum. Reprod. https://doi.org/10.1093/humrep/deae093 (2024).
Yildirim, R. M. & Seli, E. Mitochondria as therapeutic targets in assisted reproduction. Hum. Reprod. https://doi.org/10.1093/humrep/deae170 (2024).
Cohen, J. et al. Ooplasmic transfer in mature human oocytes. Mol. Hum. Reprod. 4, 269–280 (1998).
Tilly, J. L. & Sinclair, D. A. Germline energetics, aging, and female infertility. Cell Metab. 17, 838–850 (2013).
Zhang, C. et al. Mitochondrial transfer from induced pluripotent stem cells rescues developmental potential of in vitro fertilized embryos from aging females. Biol. Reprod. 104, 1114–1125 (2021).
Craven, L., Tang, M. X., Gorman, G. S., De Sutter, P. & Heindryckx, B. Novel reproductive technologies to prevent mitochondrial disease. Hum. Reprod. Update 23, 501–519 (2017).
Tang, M. et al. Germline nuclear transfer in mice may rescue poor embryo development associated with advanced maternal age and early embryo arrest. Hum. Reprod. 35, 1562–1577 (2020).
Greenfield, A. Making sense of heritable human genome editing: scientific and ethical considerations. Prog. Mol. Biol. Transl. Sci. 182, 1–28 (2021).
Herbert, M., Choudhary, M. & Zander-Fox, D. Assisted reproductive technologies at the nexus of fertility treatment and disease prevention. Science 380, 164–167 (2023).
Saitou, M. & Hayashi, K. Mammalian in vitro gametogenesis. Science 374, eaaz6830 (2021).
Qu, J., Hu, H., Niu, H., Sun, X. & Li, Y. Melatonin restores the declining maturation quality and early embryonic development of oocytes in aged mice. Theriogenology 210, 110–118 (2023).
Cao, Y. et al. Quercetin promotes in vitro maturation of oocytes from humans and aged mice. Cell Death Dis. 11, 965 (2020).
Ma, L. et al. Coenzyme Q10 supplementation of human oocyte in vitro maturation reduces postmeiotic aneuploidies. Fertil. Steril. 114, 331–337 (2020).
Yang, Q. et al. Rapamycin improves the quality and developmental competence of in vitro matured oocytes in aged mice and humans. Aging 14, 9200–9209 (2022).
Dong, S. et al. Testicular aging, male fertility and beyond. Front. Endocrinol. 13, 1012119 (2022).
Stone, B. A., Alex, A., Werlin, L. B. & Marrs, R. P. Age thresholds for changes in semen parameters in men. Fertil. Steril. 100, 952–958 (2013).
Yao, S. Y. et al. Nestin-dependent mitochondria–ER contacts define stem Leydig cell differentiation to attenuate male reproductive ageing. Nat. Commun. https://doi.org/10.1038/s41467-022-31755-w (2022).
Zhang, C. et al. FOXO4-DRI alleviates age-related testosterone secretion insufficiency by targeting senescent Leydig cells in aged mice. Aging 12, 1272–1284 (2020).
Fujii, J., Iuchi, Y., Matsuki, S. & Ishii, T. Cooperative function of antioxidant and redox systems against oxidative stress in male reproductive tissues. Asian J. Androl. 5, 231–242 (2003).
Koksal, I. T., Usta, M., Orhan, I., Abbasoglu, S. & Kadioglu, A. Potential role of reactive oxygen species on testicular pathology associated with infertility. Asian J. Androl. 5, 95–99 (2003).
Eskenazi, B. et al. Antioxidant intake is associated with semen quality in healthy men. Hum. Reprod. 20, 1006–1012 (2005).
Schmid, T. E. et al. Micronutrients intake is associated with improved sperm DNA quality in older men. Fertil. Steril. 98, 1130–1137 (2012).
Gueven, N., Ravishankar, P., Eri, R. & Rybalka, E. Idebenone: when an antioxidant is not an antioxidant. Redox Biol. https://doi.org/10.1016/j.redox.2020.101812 (2021).
Nikitaras, V., Zander-Fox, D. & McPherson, N. O. Improving sperm oxidative stress and embryo quality in advanced paternal age using idebenone in vitro–a proof-of-concept study. Antioxidants https://doi.org/10.3390/antiox10071079 (2021).
Gonzalez, M. B. et al. BGP-15 mitigates adverse impacts of aging on sperm quality, fertility, and offspring health in male mice. Reproduction https://doi.org/10.1530/REP-24-0105 (2024).
Hassan, H. M. et al. Men with idiopathic oligoasthenoteratozoospermia exhibit lower serum and seminal plasma melatonin levels: comparative effect of night-light exposure with fertile males. Exp. Ther. Med. 20, 235–242 (2020).
Muratoglu, S., Dizakar, O. S. A., Aktan, A. K., Ömeroglu, S. & Akbulut, K. G. The protective role of melatonin and curcumin in the testis of young and aged rats. Andrologia https://doi.org/10.1111/and.13203 (2019).
Sokanovic, S. J., Capo, I., Medar, M. M., Andric, S. A. & Kostic, T. S. Long-term inhibition of PDE5 ameliorates aging-induced changes in rat testis. Exp. Gerontol. 108, 139–148 (2018).
Butkiewicz, A. F., Amaral, A., Cerveira-Pinto, M. & Kordowitzki, P. Assessing the influence of maternal age in bovine embryos and oocytes: A model for human reproductive aging. Aging Dis. https://doi.org/10.14336/AD.2024.0305 (2024).
Duncan, F. E. et al. Age-associated dysregulation of protein metabolism in the mammalian oocyte. Aging Cell 16, 1381–1393 (2017).
Adhikari, D., Risal, S., Liu, K. & Shen, Y. Pharmacological inhibition of mTORC1 prevents over-activation of the primordial follicle pool in response to elevated PI3K signaling. PLoS ONE 8, e53810 (2013).
Zhang, X. M. et al. Rapamycin preserves the follicle pool reserve and prolongs the ovarian lifespan of female rats via modulating mTOR activation and sirtuin expression. Gene 523, 82–87 (2013).
Selesniemi, K., Lee, H. J., Muhlhauser, A. & Tilly, J. L. Prevention of maternal aging-associated oocyte aneuploidy and meiotic spindle defects in mice by dietary and genetic strategies. Proc. Natl Acad. Sci. USA 108, 12319–12324 (2011).
Selesniemi, K., Lee, H. J. & Tilly, J. L. Moderate caloric restriction initiated in rodents during adulthood sustains function of the female reproductive axis into advanced chronological age. Aging Cell 7, 622–629 (2008).
Snider, A. P. & Wood, J. R. Obesity induces ovarian inflammation and reduces oocyte quality. Reproduction 158, R79–R90 (2019).
Lane, M., Zander-Fox, D. L., Robker, R. L. & McPherson, N. O. Peri-conception parental obesity, reproductive health, and transgenerational impacts. Trends Endocrinol. Metab. 26, 84–90 (2015).
Gonzalez, M. B., Robker, R. L. & Rose, R. D. Obesity and oocyte quality: significant implications for ART and emerging mechanistic insights. Biol. Reprod. 106, 338–350 (2022).
Service, C. A., Puri, D., Al Azzawi, S., Hsieh, T. C. & Patel, D. P. The impact of obesity and metabolic health on male fertility: a systematic review. Fertil. Steril. 120, 1098–1111 (2023).
Dong, L., Teh, D. B. L., Kennedy, B. K. & Huang, Z. Unraveling female reproductive senescence to enhance healthy longevity. Cell Res. 33, 11–29 (2023).
Yang, Y. et al. The potent antioxidant mitoq protects against preeclampsia during late gestation but increases the risk of preeclampsia when administered in early pregnancy. Antioxid. Redox Signal. 34, 118–136 (2021).
Wilkinson, J. E. et al. Rapamycin slows aging in mice. Aging Cell 11, 675–682 (2012).
Ochiai, A. et al. Influence of resveratrol supplementation on IVF-embryo transfer cycle outcomes. Reprod. Biomed. Online 39, 205–210 (2019).
Acknowledgements
We acknowledge the many researchers whose primary works on the mechanisms of reproductive aging could not be included due to space constraints and restrictions on the number of references.
Author information
Authors and Affiliations
Contributions
T.U., Y.E.W., J.S.S., M.B.G. and R.L.R. reviewed the literature and compiled the studies to be included. Y.E.W. and J.S.S. wrote the sections about female reproductive aging. M.B.G. wrote the sections about male reproductive aging. R.J.N. provided clinical expertise and critical review. R.L.R. wrote the conclusions section with input from all authors. Y.E.W. prepared the figures with input from all authors. J.S.S. compiled the tables with input from all authors. All authors reviewed multiple drafts of the manuscript. R.L.R. supervised and coordinated all aspects of the literature review and manuscript preparation.
Corresponding author
Ethics declarations
Competing interests
M.B.G. and R.L.R. are inventors on a patent related to the actions of BGP-15 to improve gamete quality filed by The University of Adelaide and owned by Mitochon Technologies. R.L.R. is a consultant for Vitaleon Pharma. The other authors declare no competing interests.
Peer review
Peer review information
Nature Aging thanks Shweta Dipali, Zhi Zhou, Bo Xiong, and the other, anonymous, reviewer(s) for their contribution to the peer review of this work.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Winstanley, Y.E., Stables, J.S., Gonzalez, M.B. et al. Emerging therapeutic strategies to mitigate female and male reproductive aging. Nat Aging 4, 1682–1696 (2024). https://doi.org/10.1038/s43587-024-00771-4
Received:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s43587-024-00771-4
This article is cited by
-
Crosstalk between H3K4me3 and oxidative stress is a potential target for the improvement of ART-derived embryos
Nature Communications (2025)
-
Germ cells and the aging niche: a systems approach to reproductive longevity
Journal of Assisted Reproduction and Genetics (2025)