Abstract
Study design:
An experimental, cross-sectional study.
Objectives:
To investigate effects of using a visuotemporal cue on the walking ability of independent ambulatory subjects with spinal cord injury (SCI) as compared with healthy subjects.
Setting:
A tertiary rehabilitation center, Thailand.
Methods:
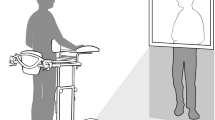
Forty independent ambulatory subjects with SCI and healthy subjects participated in the study (20 subjects per group). All of them were assessed for their walking speed, stride length, cadence and percents of step symmetry under two conditions, including walking at their fastest speed with and without a visuotemporal cue along a 10 m walkway.
Results:
When walking with a visuotemporal cue, walking speed, stride length and cadence of the subjects were significantly increased from the uncued condition (P<0.01). However, the healthy subjects showed a significantly greater increase in walking speed and cadence, whereas, subjects with SCI demonstrated significantly higher improvement in stride length as compared with the other group (P<0.001). In addition, the effects of the visuotemporal cue were significantly greater in those with less severity of SCI (P<0.01).
Conclusion:
The findings confirm the benefits of using a visuotemporal cue to improve variables relating to walking ability in subjects with intact integrative capability of the brain but with different levels of sensorimotor deterioration. The findings suggest the use of a visuotemporal cue to improve the effectiveness of programs in sport and exercise sciences, and rehabilitation treatments.
Similar content being viewed by others
Log in or create a free account to read this content
Gain free access to this article, as well as selected content from this journal and more on nature.com
or
References
Field-Fote EC . Spinal cord control of movement: implications for locomotor rehabilitation following spinal cord injury. Phys Ther 2000; 80: 477–484.
Lapointe R, Lajoie Y, Serresse O, Barbeau H . Functional community ambulation requirements in incomplete spinal cord injured subjects. Spinal Cord 2001; 39: 327–335.
Van Hedel H . Gait speed in relation to categories of functional ambulation after spinal cord injury. Neurorehabil Neural Repair 2009; 23: 343–350.
Amatachaya S, Keawsutthi M, Amatachaya P, Manimmanakorn N . Effects of external cues on gait performance in independent ambulatory incomplete spinal cord injury patients. Spinal Cord 2009; 47: 668–673.
Field-Fote E, Tepavac D . Improved intralimb coordination in people with incomplete spinal cord injury following training with body weight support and electrical stimulation. Phys Ther 2002; 82: 707–715.
Zorner B, Blanckenhorn WU, Dietz V, Curt A . Clinical algorithm for improved prediction of ambulation and patient stratification after incomplete spinal cord injury. J Neurotrauma 2010; 27: 241–252.
Majsak M, Kaminski T, Gentile A, Flanagan J . The reaching movements of patients with Parkinson's disease under self-determined maximal speed and visually cued conditions. Brain 1998; 121: 755–766.
Suteerawattananon M, Morrisb G, Etnyrec B, Jankovicd J, Protas E . Effects of visual and auditory cues on gait in individuals with Parkinson’s disease. J Neurol Sci 2004; 219: 63–69.
Thaut M, Leins A, Rice R, Argstatter H, Kenyon G, McIntosh G et al. Rhythmic auditory stimulation improves gait more than NDT/Bobath training in near-ambulatory patients early poststroke: a single-blind, randomized trial. Clin Rehabil 2007; 21: 455–459.
Beek P, van Wieringen P . Perspectives on the relation between information and dynamics: an epilogue. Hum Mov Sci 1994; 13: 519–533.
Bach-y-Rita P, Kercel S . Sensory substitution and the human-machine interface. Trends Cogn Sci 2003; 7: 541–546.
Amatachaya S, Amatachaya P, Keawsutthi M . External cues benefit walking ability of ambulatory patients with spinal cord injury. J Spinal Cord Med 2013; 36: 638–644.
Said C, Goldie P, Patla A, Sparrow W . Effect of stroke on step characteristics of obstacle crossing. Arch Phys Med Rehabil 2001; 82: 1712–1719.
Kirtley C . The temporal-spatial parameters. In: Clinical Gait Analysis: Theory and Practice. Livingstone: Edinburgh, Scotland. 2006 pp 20–21.
Van Hedel H, Dietz V, Curt A . Assessment of walking speed and distance in subjects with an incomplete spinal cord injury. Neurorehabil Neural Repair 2007; 21: 295–301.
Gibson J . The Ecological Approach to Visual Perception. Houghton Mifflin company: Boston, MA, USA. 1979.
Tanawongsuwan R, Bobick A . Performance analysis of time-distance gait parameters under different speeds. Proceedings of the 4th International Conference on Audio- and Video-Based Biometric Person Authentication; 2003. Guildford, UK, pp 715–724.
Capo-Lugo CE, Mullens CH, Brown DA . Maximum walking speeds obtained using treadmill and overground robot system in persons with post-stroke hemiplegia. J Neuroeng Rehabil 2012; 9: 80.
Teixeira da Cunha Filho I, Lim PA, Qureshy H, Henson H, Monga T, Protas EJ . A comparison of regular rehabilitation and regular rehabilitation with supported treadmill ambulation training for acute stroke patients. J Rehabil Res Dev 2001; 38: 245–255.
Hausdorff JM, Edelberg HK, Mitchell SL, Goldberger AL, Wei JY . Increased gait unsteadiness in community-dwelling elderly fallers. Arch Phys Med Rehabil 1997; 78: 278–283.
Acknowledgements
This study was funded by a grant from Thammasat University, Bangkok, Thailand, and the Improvement of Physical Performance and Quality of Life (IPQ) research group, Khon Kaen University, Khon Kaen, Thailand. We sincerely thank Mr Ian Thomas for his contribution in preparing this manuscript. We also thank Faculty of Associated Medical Sciences, and Graduate School, Khon Kaen University.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Pramodhyakul, N., Amatachaya, P., Sooknuan, T. et al. Effects of a visuotemporal cue on walking ability of independent ambulatory subjects with spinal cord injury as compared with healthy subjects. Spinal Cord 52, 220–224 (2014). https://doi.org/10.1038/sc.2013.160
Received:
Revised:
Accepted:
Published:
Issue date:
DOI: https://doi.org/10.1038/sc.2013.160