Abstract
Study design:
Retrospective study.
Objectives:
The objective of this study was to investigate the clinical risk factors for febrile urinary tract infection (UTI) in spinal cord injury-associated neurogenic bladder (NB) patients who perform routine clean intermittent catheterization (CIC).
Setting:
Rehabilitation Hospital, Kobe, Japan.
Methods:
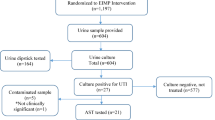
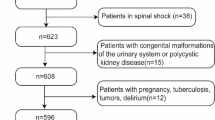
Over a 3-year period, we retrospectively assessed the clinical risk factors for febrile UTI in 259 spinal cord injury patients diagnosed as NB and performing routine CIC with regard to the factors such as gender, the presence of pyuria and bacteriuria, and the categories of the American Spinal Injury Association (ASIA) impairment scale.
Results:
A total of 67 patients had febrile UTI in the follow-up period, with 57 cases of pyelonephritis, 11 cases of epididymitis and 2 cases of prostatitis, including the patients with plural infectious diseases. The causative bacteria were ranked as follows: Escherichia coli (74 cases), Pseudomonas aeruginosa (17 cases), Enterococcus faecalis (14 cases) and Klebsiella pneumoniae (12 cases). Antibiotic-resistant E. coli were seen, with 10.5% instances of extended-spectrum β-lactamase (ESBL) production and 23.8% of fluoroquinolone resistance. Multivariate analyses of clinical risk factors for febrile UTI showed that gender (male, P=0.0431), and ASIA impairment scale C or more severe (P=0.0266) were significantly associated with febrile UTI occurrence in NB patients with routine CIC.
Conclusion:
Our data demonstrated gender (male) and ASIA impairment scale C or more severe were significantly associated with febrile UTI occurrence in NB patients using routine CIC. Further prospective studies are necessary to define the full spectrum of possible risk factors for febrile UTI in these patients.
Similar content being viewed by others
Log in or create a free account to read this content
Gain free access to this article, as well as selected content from this journal and more on nature.com
or
References
Igawa Y, Wyndaele JJ, Nishizawa O . Catheterization: Possible complications and prevention and treatment. Int J Urol 2008; 15: 481–485.
Kakizaki H, Igawa Y, Gotou M, Takeda M, Hasegawa T, Koyanagi T et al. Clinical practice guideline for lower urinary tract dysfunction in patients with chronic spinal cord injury. J Jpn Med Soc Spinal Cord Lesion 2005; 16: 253–259.
Tanaka K, Hattori K, Hayashi H . Long-term follow up of intermittent catheterization by patient with spinal cord injury. J Jpn Med Soc Spinal Cord Lesion 2006; 19: 32–33.
Ozawa H, Nishiyama Y . Correlation between catheterization frequency and complication in spinal cord injured patients. J Jpn Med Soc Spinal Cord Lesion 2007; 20: 194–195.
Gerridzen RG, ThijssenAM, Dehoux E . Risk factors for upper tract deterioration inchronic spinal cord injury patients. J Urol 1992; 147: 416–418.
American Spinal Injury Association International Standards for Neurological Classification of Spinal Cord Injury, Revised 2002. American Spinal Injury Association: Chicago, IL, USA,. 2002.
Schurch B, Schmid DM, Karsenty G, Reitz A . Can neurologic examination predict type of detrusor sphincter-dyssynergia in patients with spinal cord injury? Urology 2005; 65: 243–246.
Takaba K, Shigemura K, Osawa K, Nomi M, Fujisawa M, Arakawa S . Emergence of extended-spectrum β-lactamase-producing Escherichia coli in catheter-associated urinary tract infection in neurogenic bladder patients. Am J Infect Control 2014; 42: e29–e31.
Beraldo PS, Neves EG, Alves CM, Khan P, Cirilo AC, Alencar MR . Pyrexia in hospitalised spinal cord injury patients. Paraplegia 1993; 31: 186–191.
Schaeflfer AJ, Schaeffer EM. Infections and inflammations. In: Wein AJ, Kavoussi LR, Novick AC, Partin AW, Peters CA (eds). Campbell-Walsh Urology, 10th edn. Elsevier-Saunders: Philadelphia, PA, USA, 2011, pp 257–326.
Everaert K, Oostra C, Delanghe J, Vande Walle J, Van Laere M, Oosterlinck W . Diagnosis and localization of a complicated urinary tract infection in neurogenic bladder disease by tubular proteinuria and serum prostate specific antigen. Spinal Cord 1998; 36: 33–38.
Hooton TM, Bradley SF, Cardenas DD, Colgan R, Geerlings SE, Rice JC et al. Diagnosis, prevention, and treatment of catheter-associated urinary tract infection in adults: 2009 International Clinical Practice Guidelines from the Infectious Diseases Society of America. Clin Infect Dis 2010; 50: 625–663.
Nicolle LE . AMMI Canada Guidelines Committee. Complicated urinary tract infection in adults. Can J Infect Dis Med Microbiol 2005; 16: 349–360.
Kikkawa K, Mitsuda M, Yamasaki K, Uekado Y . Evaluation of urinary tract infection in patients treated with clean intermittent catheterization. Jpn J Environ Infect 2010; 25: 73–78.
Furuse A, Nagano K, Komaki S, Mochinaga H, Saitou M . Clinical analysis of childhood urinary tract infection due to extended-spectrum β-lactamase producing Escherichia coli and Klebsiella pneumoniae. J Pediatr Infect Dis Immunol 2014; 5: 403–406.
Quale JM, Landman D, Bradford PA, Visalli M, Ravishankar J, Flores C et al. Molecular epidemiology of a citywide outbreak of extended-spectrum -lactamase-producing Klebsiella pneumoniae infection. Clin Infect Dis 2002; 35: 834–841.
Kurtaran B, Candevir A, Tasova Y, Kibar F, Inal AS, Komur S et al. Antibiotic resistance in community-acquired urinary tract infections: prevalence and risk factors. Med Sci Monit 2010; 16: CR246–CR251.
Chong Y, Shimoda S, Yakushiji H, Ito Y, Miyamoto T, Kamimura T et al. Community spread of extended spectrum β -lactamase-producing Escherichia coli Klebsiella pneumoniae and Proteus mirabilis: a long-term study in Japan. J Med Microbiol 2013; 62: 1038–1043.
Pena C, Pujol M, Ardanuy C, Ricart A, Pallares R, Liñares J et al. Epidemiology and successful control of a large outbreak due to Klebsiella pneumoniae producing extended-spectrum β-lactamases. Antimicrob Agents Chemother 1998; 42: 53–58.
Rahal JJ, Urban C, Horn D, Freeman K, Segal-Maurer S, Maurer J et al. Class restriction of cephalosporin use to control total cephalosporin resistance in nosocomial Klebsiella. JAMA 1998; 280: 1233–1237.
Sauerwein D . Urinary tract infection in patients with neurogenic bladder dysfunction. Int J Antimicrob Agents 2002; 19: 592–597.
Massa LM, Hoffman JM, Cardenas DD . Validity, accuracy and predictive value of urinary tract infection signs and symptoms in individuals with spinal cord injury on intermittent catheterization. J Spinal Cord Med 2009; 32: 568–573.
Jayawardena V, Midha M . Significance of bacteriuria in neurogenic bladder. J Spinal Cord Med 2004; 27: 102–105.
Cardenas DD, Hoffman JM, Kelly E, Mayo ME . Impact of a urinary tract infection educational program in persons with spinal cord injury. J Spinal Cord Med 2004; 27: 47–54.
Cespedes RD, Gerboc JL. Other therapies for storage and emptying failure. In: Wein AJ, Kavoussi LR, Novick AC, Partin AW, Peters CA (eds). Campbell-Walsh Urology, 10th edn. Elsevier-Saunders: Philadelphia, CA, USA, 2011, pp 2186–2203.
Kovindha A, Na Chiang Mai W, Madersbacher H . Reused silicone catheter for clean intermittent catheterization (CIC): is it safe cord-injured (SCI) men? Spinal Cord 2004; 42: 638–642.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Mukai, S., Shigemura, K., Nomi, M. et al. Retrospective study for risk factors for febrile UTI in spinal cord injury patients with routine concomitant intermittent catheterization in outpatient settings. Spinal Cord 54, 69–72 (2016). https://doi.org/10.1038/sc.2015.170
Received:
Revised:
Accepted:
Published:
Issue date:
DOI: https://doi.org/10.1038/sc.2015.170
This article is cited by
-
Hydrophilic catheters for intermittent catheterization and occurrence of urinary tract infections. A retrospective comparative study in patients with spinal cord Injury
BMC Urology (2024)
-
Clinical Characteristics of Uncomplicated Acute Pyelonephritis Caused by Escherichia coli and Klebsiella pneumoniae
Infectious Diseases and Therapy (2024)
-
Urinary tract infections and intermittent catheterization among patients with spinal cord injury in Chinese community
Scientific Reports (2023)
-
Behandlung rezidivierender Harnwegsinfekte bei PatientInnen mit neurogener Blasenfunktionsstörung
Journal für Urologie und Urogynäkologie/Österreich (2022)
-
Behandlung rezidivierender Harnwegsinfekte bei PatientInnen mit neurogener Blasenfunktionsstörung
Urologie in der Praxis (2021)