Abstract
Study design:
Cross-sectional study.
Objective:
To evaluate the long-term effect of the sacral anterior root stimulator (SARS) on neurogenic bowel dysfunction in a large, well defined spinal cord injury (SCI) cohort.
Setting:
Department of Neuro-Urology, Bad Wildungen, Germany.
Methods:
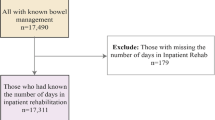
Subjects undergone surgery at for SARS-SDAF (sacral deafferentation) between September 1986 and July 2011 (n=587) answered a questionnaire. In total, 277 SARS subjects were available for the baseline (recall) and follow-up comparison.
Results:
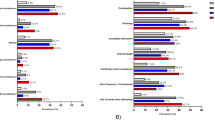
Median age was 49 years (range: 19–80), time from SCI to surgery was 10 years (range: 0–49) and from surgery to follow-up 13 (range: 1–25). Of the responders 73% used SARS for bowel emptying. On visual analog scale (VAS) ranging from 0–10 (best), satisfaction with SARS was 10. Baseline and follow-up comparison showed a decline in the median VAS score 0–10 (worst) for bowel symptoms from 6 (range: 4–8) to 4 (range: 2–6), P<0.0001; median neurogenic bowel dysfunction score from 17 (range: 11–2) to 11 (range: 9–15), P<0.0001; median St Marks score from 4 (range: 0–7) to 4 (range: 0–5), P=0.01; and median Cleveland constipation score from 7 (range: 6–10) to 6 (range: 4–8), P<0.0001. Use of suppositories, digital evacuation and mini enema and subjects totally dependent on assistance during defecation were significantly lower after SARS.
Conclusions:
The SARS has the potential to be one of the few treatment methods targeting multiple organ dysfunctions following SCI.
Similar content being viewed by others
Log in or create a free account to read this content
Gain free access to this article, as well as selected content from this journal and more on nature.com
or
References
Kutzenberger J . Surgical therapy of neurogenic detrusor overactivity (hyperreflexia) in paraplegic patients by sacral deafferentation and implant driven micturition by sacral anterior root stimulation: methods, indications, results, complications, and future prospects. Acta Neurochir Suppl 2007; 97: 333–339.
Krogh K, Perkash I, Stiens SA, Biering-Sorensen F . International bowel function basic spinal cord injury data set. Spinal Cord 2009; 47: 230–234.
Krogh K, Perkash I, Stiens SA, Biering-Sorensen F . International bowel function extended spinal cord injury data set. Spinal Cord 2009; 47: 235–241.
Krogh K, Christensen P, Sabroe S, Laurberg S . Neurogenic bowel dysfunction score. Spinal Cord 2006; 44: 625–631.
Vaizey CJ, Carapeti E, Cahill JA, Kamm MA . Prospective comparison of faecal incontinence grading systems. Gut 1999; 44: 77–80.
Agachan F, Chen T, Pfeifer J, Reissman P, Wexner SD . A constipation scoring system to simplify evaluation and management of constipated patients. Dis Colon Rectum 1996; 39: 681–685.
Kirshblum SC, Burns SP, Biering-Sorensen F, Donovan W, Graves DE, Jha A et al. International standards for neurological classification of spinal cord injury (revised 2011). J Spinal Cord Med 2011; 34: 535–546.
Krogh K, Olsen N, Christensen P, Madsen JL, Laurberg S . Colorectal transport during defecation in patients with lesions of the sacral spinal cord. Neurogastroenterol Motil 2003; 15: 25–31.
Rasmussen MM, Krogh K, Clemmensen D, Bluhme H, Rawashdeh Y, Christensen P . Colorectal transport during defecation in subjects with supraconal spinal cord injury. Spinal Cord 2013; 51: 683–687.
Krogh K, Mosdal C, Laurberg S . Gastrointestinal and segmental colonic transit times in patients with acute and chronic spinal cord lesions. Spinal Cord 2000; 38: 615–621.
Lombardi G, Del Popolo G, Cecconi F, Surrenti E, Macchiarella A . Clinical outcome of sacral neuromodulation in incomplete spinal cord-injured patients suffering from neurogenic bowel dysfunctions. Spinal Cord 2010; 48: 154–159.
Varma JS, Binnie N, Smith AN, Creasey GH, Edmond P . Differential effects of sacral anterior root stimulation on anal sphincter and colorectal motility in spinally injured man. Br J Surg 1986; 73: 478–482.
Valles M, Rodriguez A, Borau A, Mearin F . Effect of sacral anterior root stimulator on bowel dysfunction in patients with spinal cord injury. Dis Colon Rectum 2009; 52: 986–992.
Binnie NR, Smith AN, Creasey GH, Edmond P . Constipation associated with chronic spinal cord injury: the effect of pelvic parasympathetic stimulation by the Brindley stimulator. Paraplegia 1991; 29: 463–469.
Brindley GS . Sacral root and hypogastric plexus stimulators and what these models tell us about autonomic actions on the bladder and urethra. Clin Sci (Lond) 1986; 70: 41s–44s.
Moller FV, Buntzen S, Rijkhoff NJ, Laurberg S . Rectal evacuation and antegrade colonic luminal transport by sacral anterior root stimulation in pigs. Dis Colon Rectum 2009; 52: 1650–1656.
Andersen IS, Rijkhoff NJ, Vukovic A, Buntzen S, Djurhuus JC, Laurberg S . Anorectal motility responses to selective stimulation of the ventral sacral nerve roots in an experimental model. Br J Surg 2005; 92: 1513–1519.
Juul T, Bazzocchi G, Coggrave M, Johannesen IL, Hansen RB, Thiyagarajan C et al. Reliability of the international spinal cord injury bowel function basic and extended data sets. Spinal Cord 2011; 49: 886–891.
Worsoe J, Rasmussen M, Christensen P, Krogh K . Neurostimulation for neurogenic bowel dysfunction. Gastroenterol Res Pract 2013; 2013: 563294.
George AT, Dudding TC, Gurmany S, Kamm MA, Nicholls RJ, Vaizey CJ . Pudendal nerve stimulation for bowel dysfunction in complete cauda equina syndrome. Ann Surg 2014; 259: 502–507.
Acknowledgements
The authors thank Professor Soren Laurberg for help and support with the study. Further, we thank the Lundbeck foundation for financial support.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Rasmussen, M., Kutzenberger, J., Krogh, K. et al. Sacral anterior root stimulation improves bowel function in subjects with spinal cord injury. Spinal Cord 53, 297–301 (2015). https://doi.org/10.1038/sc.2015.2
Received:
Revised:
Accepted:
Published:
Issue date:
DOI: https://doi.org/10.1038/sc.2015.2
This article is cited by
-
Impact of Neurogenic Lower Urinary Tract Dysfunction on Bowel Symptoms
Current Bladder Dysfunction Reports (2023)
-
Guideline for the management of neurogenic bowel dysfunction in spinal cord injury/disease
Spinal Cord (2022)
-
Effects of highly selective sympathectomy on neurogenic bowel dysfunction in spinal cord injury rats
Scientific Reports (2021)
-
Guideline for the management of pre-, intra-, and postpartum care of women with a spinal cord injury
Spinal Cord (2020)
-
Leitlinie: Neurogene Darmfunktionsstörung bei Querschnittlähmung (Langfassung)
coloproctology (2020)