Abstract
Study design:
This was a retrospective cohort study.
Objectives:
The objectives of this study were to determine clinical features of infection-related myelopathy (IRM) and functional outcomes compared with other nontraumatic and traumatic myelopathies.
Setting:
US academic inpatient rehabilitation unit.
Methods:
This was a 16-year retrospective review of patients with myelopathy discharged from inpatient rehabilitation between 1 January 1995 and 31 December 2010. Patients comprised three injury groups: IRM, nontraumatic myelopathy (NTM) and traumatic spinal cord injury (TSCI). Information collected includes demographic characteristics, functional data, length of stay, injury completeness and discharge destination. Primary outcome measures were change in Functional Independence Measure (FIM) and daily FIM change. For IRM, data were collected regarding injury characteristics, risk factors, presenting symptoms, neurologic impairment level and treatment.
Results:
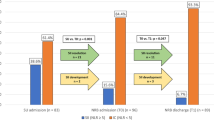
Of the 1601 patients, 40 (2.5%) had IRM, 1105 (69.0%) had NTM and 456 (28.5%) had TSCI. IRM mean (s.d.) age was 58.6 (15.7) years (male gender, 72.5%). The majority in each group had incomplete injuries. IRM had longer lengths of stay (P<0.001), lower admission (P=0.001) and discharge (P=0.005) FIM scores and lower FIM daily change (P=0.002) than NTM. Degree of functional improvement was similar in all groups, and most patients in each group were discharged home. Infectious pathogens were bacterial (80.0%, n=32), viral (7.5%, n=3), tuberculous (7.5%, n=3), parasitic (2.5%, n=1) and multiple types (2.5%, n=1). The most common bacterial cause (65.6%) was Staphylococcus aureus.
Conclusions:
Infectious etiologies comprise a small proportion of NTM but represent a unique entity with distinct recovery patterns and outcomes. These patients can achieve similar functional improvements as other NTM patients during inpatient rehabilitation, although over a longer period of time.
Similar content being viewed by others
Log in or create a free account to read this content
Gain free access to this article, as well as selected content from this journal and more on nature.com
or
References
McKinley WO, Seel RT, Hardman JT . Nontraumatic spinal cord injury: incidence, epidemiology, and functional outcome. Arch Phys Med Rehabil 1999; 80: 619–623.
New PW, Rawicki HB, Bailey MJ . Nontraumatic spinal cord injury: demographic characteristics and complications. Arch Phys Med Rehabil 2002; 83: 996–1001.
Vervoordeldonk JJ, Post MW, New P, Clin Epi M, Van Asbeck FW . Rehabilitation of patients with nontraumatic spinal cord injury in the Netherlands: etiology, length of stay, and functional outcome. Top Spinal Cord Inj Rehabil 2013; 19: 195–201.
New PW, Reeves RK, Smith E, Townson A, Eriks-Hoogland I, Gupta A et al. International retrospective comparison of inpatient rehabilitation for patients with spinal cord dysfunction epidemiology and clinical outcomes. Arch Phys Med Rehabil 2015; 96: 1080–1087.
Catz A, Goldin D, Fishel B, Ronen J, Bluvshtein V, Gelernter I . Recovery of neurologic function following nontraumatic spinal cord lesions in Israel. Spine (Phila Pa 1976) 2004; 29: 2278–2282.
New PW, Astrakhantseva I . Rehabilitation outcomes following infections causing spinal cord myelopathy. Spinal Cord 2014; 52: 444–448.
Connor DE Jr, Chittiboina P, Caldito G, Nanda A . Comparison of operative and nonoperative management of spinal epidural abscess: a retrospective review of clinical and laboratory predictors of neurological outcome. J Neurosurg Spine 2013; 19: 119–127.
Carey M . Infections of the spine and spinal cord. In: Youmans JR (ed). Neurological Surgery 4th edn. Saunders: Philadelphia, PA. 1996, pp 3275–3304.
Allen M, Flannery A, Fischer J . Spinal epidural and subdural abscesses. In: Wilkins RH, Rengachary SS (eds). Neurosurgery 2nd edn. McGraw-Hill: New York, NY, USA. 1996, pp 3327–3329.
Darouiche RO . Spinal epidural abscess. N Engl J Med 2006; 355: 2012–2020.
Yen HL, Kong KH, Chan W . Infectious disease of the spine: outcome of rehabilitation. Spinal Cord 1998; 36: 507–513.
Morillo-Leco G, Alcaraz-Rousselet MA, Diaz-Borrego P, Saenz-Ramirez L, Artime C, Labarta-Bertol C . Clinical characteristics of spinal cord injury caused by infection. Rev Neurol 2005; 41: 205–208.
Weingarden SI, Swarczinski C . Non-granulomatous spinal epidural abscess: a rehabilitation perspective. Paraplegia 1991; 29: 628–631.
Zafonte RD, Ricker JH, Hanks RA, Wood DL, Amin A, Lombard L . Spinal epidural abscess: study of early outcome. J Spinal Cord Med 2003; 26: 345–351.
Koo DW, Townson AF, Dvorak MF, Fisher CG . Spinal epidural abscess: a 5-year case-controlled review of neurologic outcomes after rehabilitation. Arch Phys Med Rehabil 2009; 90: 512–516.
McKinley W, Merrell C, Meade M, Brooke K, DiNicola A . Rehabilitation outcomes after infection-related spinal cord disease: a retrospective analysis. Am J Phys Med Rehabil 2008; 87: 275–280.
Ribeira T, Veiros I, Nunes R, Martins L . Spondilodyscitis: five years of experience in a department of rehabilitation. Acta Med Port 2008; 21: 559–566.
Draulans N, Kiekens C, Roels E, Peers K . Etiology of spinal cord injuries in Sub-Saharan Africa. Spinal Cord 2011; 49: 1148–1154.
Gupta A, Taly AB, Srivastava A, Murali T . Non-traumatic spinal cord lesions: epidemiology, complications, neurological and functional outcome of rehabilitation. Spinal Cord 2009; 47: 307–311.
Hart C, Williams E . Epidemiology of spinal cord injuries: a reflection of changes in South African society. Paraplegia 1994; 32: 709–714.
Shweikeh F, Saeed K, Bukavina L, Zyck S, Drazin D, Steinmetz MP . An institutional series and contemporary review of bacterial spinal epidural abscess: current status and future directions. Neurosurg Focus 2014; 37: E9.
Patel AR, Alton TB, Bransford RJ, Lee MJ, Bellabarba CB, Chapman JR . Spinal epidural abscesses: risk factors, medical versus surgical management, a retrospective review of 128 cases. Spine J 2014; 14: 326–330.
Curry WT Jr, Hoh BL, Amin-Hanjani S, Eskandar EN . Spinal epidural abscess: clinical presentation, management, and outcome. Surg Neurol 2005; 63: 364–371.
Kirshblum S, Waring W 3rd . Updates for the International Standards for Neurological Classification of Spinal Cord Injury. Phys Med Rehabil Clin N Am 2014; 25: 505–517.
Keith RA, Granger CV, Hamilton BB, Sherwin FS . The functional independence measure: a new tool for rehabilitation. Adv Clin Rehabil 1987; 1: 6–18.
Daniel WW . Biostatistics: A Foundation for Analysis in the Health Sciences 9th edn. John Wiley & Sons, Inc.: Hoboken, NJ. 2009.
New PW, Marshall R . International Spinal Cord Injury Data Sets for non-traumatic spinal cord injury. Spinal Cord 2014; 52: 123–132.
Nas K, Kemaloglu MS, Cevik R, Ceviz A, Necmioglu S, Bukte Y et al. The results of rehabilitation on motor and functional improvement of the spinal tuberculosis. Joint Bone Spine 2004; 71: 312–316.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Portions of this manuscript were presented at the Academy of Spinal Cord Injury Professionals annual meeting in New Orleans, Louisiana, 8 September 2015.
Rights and permissions
About this article
Cite this article
Brubaker, M., Luetmer, M. & Reeves, R. Clinical features and inpatient rehabilitation outcomes of infection-related myelopathy. Spinal Cord 55, 264–268 (2017). https://doi.org/10.1038/sc.2016.115
Received:
Revised:
Accepted:
Published:
Issue date:
DOI: https://doi.org/10.1038/sc.2016.115