Abstract
Introduction:
Spinal epidural abscess (SEA) is a rare but serious cause of back pain in the critical care setting. It occurs most commonly in adults in their fifth and sixth decades of life. Risk factors include diabetes mellitus, alcoholism, AIDS or other immunocompromised states, cancer, intravenous drug use, trauma and spinal surgery. The clinical presentation can be non-specific but the classical triad includes back pain, fever and neurological deficits. Magnetic resonance imaging (MRI) with gadolinium is the diagnostic imaging modality of choice.
Case presentation:
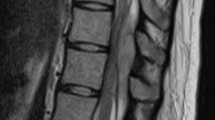
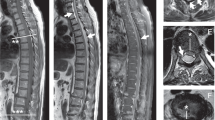
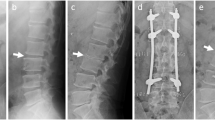
Here we report a case of SEA in a 63-year-old man with type II diabetes who presented with severe low back pain. He was found to have SEA likely secondary to a hip joint injection. The diagnosis was delayed due an earlier non-gadolinium-enhanced MRI of the spine showing no epidural abscess.
Discussion:
This case stresses the need for the definitive diagnostic study, MRI with gadolinium, in patients whose SEA is high on the list of differential diagnoses.
Similar content being viewed by others
Log in or create a free account to read this content
Gain free access to this article, as well as selected content from this journal and more on nature.com
or
References
Reihsaus E, Waldbaur H, Seeling W . Spinal epidural abscess: a meta-analysis of 915 patients. Neurosurg Rev 2000; 23: 175–204, discussion 205.
Martin RJ, Yuan HA . Neurosurgical care of spinal epidural, subdural, and intramedullary abscesses and arachnoiditis. Orthop Clin North Am 1996; 27: p 125–136.
Chao D, Nanda A . Spinal epidural abscess: a diagnostic challenge. Am Fam Physician 2002; 65: 1341–1346.
Vilke GM, Honingford EA . Cervical spine epidural abscess in a patient with no predisposing risk factors. Ann Emerg Med 1996; 27: 777–780.
Baker AS, Ojemann RG, Swartz MN, Richardson EP . Spinal epidural abscess. N Engl J Med 1975; 293: 463–468.
Kabbara A, Rosenberg SK, Untal C . Methicillin-resistant Staphylococcus aureus epidural abscess after transforaminal epidural steroid injection. Pain Physician 2004; 7: 269–272.
Sendi P, Bregenzer T, Zimmerli W . Spinal epidural abscess in clinical practice. QJM 2008; 101: 1–12.
Tang HJ, Lin HJ, Liu YC, Li CM . Spinal epidural abscess--experience with 46 patients and evaluation of prognostic factors. J Infect 2002; 45: 76–81.
Darouiche RO, Hamill RJ, Greenberg SB, Weathers SW, Musher DM . Bacterial spinal epidural abscess. Review of 43 cases and literature survey. Medicine 1992; 71: 369–385.
Teman AJ . Spinal epidural abscess. Early detection with gadolinium magnetic resonance imaging. Arch Neurol 1992; 49: 743–746.
Sadato N, Numaguchi Y, Rigamonti D, Kodama T, Nussbaum E, Sato S et al. Spinal epidural abscess with gadolinium-enhanced MRI: serial follow-up studies and clinical correlations. Neuroradiology 1994; 36: 44–48.
Rigamonti D, Liem L, Sampath P, Knoller N, Namaguchi Y, Schreibman DL et al. Spinal epidural abscess: contemporary trends in etiology, evaluation, and management. Surg Neurol 1999; 52: 189–196, discussion 197.
Pilkington SA, Jackson SA, Gillett GR . Spinal epidural empyema. Br J Neurosurg 2003; 17: 196–200.
Numaguchi Y, Rigamonti D, Rothman MI, Sato S, Mihara F, Sadato N . Spinal epidural abscess: evaluation with gadolinium-enhanced MR imaging. Radiographics 1993; 13: 545–559, discussion 559–60.
Sandhu FS, Dillon WP . Spinal epidural abscess: evaluation with contrast-enhanced MR imaging. AJNR Am J Neuroradiol 1991; 12: 1087–1093.
Pradilla G, Ardila GP, Hsu W, Rigamonti D . Epidural abscesses of the CNS. Lancet Neurol 2009; 8: 292–300.
Acknowledgements
CC-M takes responsibility for the content of the manuscript, including the case compilation, description and literature review. MP and MS provided mentorship and constructive review during the writing of this case.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Chima-Melton, C., Pearl, M. & Scheiner, M. Diagnosis of spinal epidural abscess: a case report and literature review. Spinal Cord Ser Cases 3, 17013 (2017). https://doi.org/10.1038/scsandc.2017.13
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/scsandc.2017.13