Key Points
-
GDPs are the principle dental care providers for patients with complex medical conditions.
-
There are patient groups viewed as at risk from procedural bacteraemia that are not specifically covered by any standard clinical guideline and physicians may view them as being excepted from standard guidance on antimicrobial prophylaxis.
-
Physicians' opinions and prescribing practice are often determined locally and require consideration.
Abstract
Background Concern that some catheter related bloodstream infections (CRBSI) arise from dental treatment in home parenteral nutrition (HPN) patients results in recommendation of antibiotic prophylaxis. Clinical guideline 64 is widely recognised and observed. There is a lack of consistent guidance for other patient groups viewed at risk from procedural bacteraemia.
Methods 1. An email survey of the British Association for Parenteral and Enteral Nutrition (BAPEN) HPN group, requesting physicians' opinions, observations and practises relating to oral health and CRBSI prevention; 2. Comparison of oral health parameters and dental treatment in relation to patient reported 12 month CVC infection history, using chi-square analysis to assess associations in 52 HPN patients.
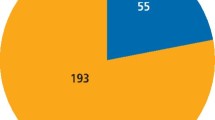
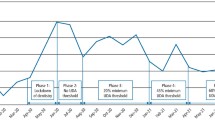
Results 1. Sixty-eight percent of the UK HPN Group responded. Fifty percent linked oral health/dental treatment with the possibility of CRBSI, 39% were unsure. Sixty-one percent had recommended parenteral prophylactic antibiotics (82% IV, 18% IM), mainly following the historic infective endocarditis (IE) dental prophylaxis guidelines. Infection with streptococci, prevotella and fusobacteria caused most concern. Amoxicillin, metronidazole, co-amoxyclav and gentamycin were the most prescribed antibiotics. Thirty-six percent might delay HPN if oral health was poor; 57% had recommended dental examination and 25% dental extractions, to prevent or treat CRBSI. 2. Associations between patient recalled CVC infection and their current dental status, the interval since dental treatment or the prophylaxis received over the previous 12 months did not achieve significance.
Conclusions Opinion varies among UK HPN providers on the role of dental treatment and oral health in CRBSI and on prescribing prophylactic antibiotics for dental treatment. Prophylaxis guidance specific to this patient group is required.
Similar content being viewed by others
Log in or create a free account to read this content
Gain free access to this article, as well as selected content from this journal and more on nature.com
or
References
Lee A M . The oral health of people receiving home parenteral nutrition. London: University of London, 2009. MSc thesis.
NICE. Nutrition support in adults: oral nutrition support, enteral tube feeding and parenteral nutrition. Clinical guideline 32. London: National Institute for Health and of Clinical Excellence, 2006. Online article available at http://www.nice.org.uk/CG32 (accessed September 2010).
NICE. Antimicrobial prophylaxis against infective endocarditis. Clinical guideline 64. London: National Institute for Health and Clinical Excellence, 2008. Online article available at http://www.nice.org.uk/CG64 (accessed December 2011).
Roberts G J . Dentists are innocent! 'Everyday' bacteraemia is the real culprit: a review and assessment of the evidence that dental surgical procedures are a principle cause of bacterial endocarditis in children. Paediatr Cardiol 1999; 20: 317–325.
Ireton-Jones C, DeLegge M . Home parenteral nutrition registry: a five-year retrospective evaluation of outcomes of patients receiving home parenteral nutrition support. Nutrition 2005; 21: 156–160.
Rannem T, Ladefoged K, Hegnhøj J, Møller E H, Bruun B, Jarnum S . Catheter related sepsis in long term parenteral nutrition with Broviac catheters. An evaluation of different disinfectants. Clin Nutr 1990; 9: 131–136.
Messing B . Catheter-related sepsis during home parenteral nutrition. Clin Nutr 1995; 14(Suppl 1): 46–51.
Johnston D A, Richards J, Pennington C R . Auditing the effect of experience and change on home parenteral nutrition related complications. Clin Nutr 1994; 13: 341–344.
George R L, Cornel G . Subendocardial abscess as a complication of prolonged central venous assess for parenteral nutrition. Can J Surg 1992; 35: 91–93.
Yared G, Seidner D L, Steiger E, Hall P M, Nally J V . Tunnelled right atrial catheter infection presenting as renal failure. JPEN J Parenter Enteral Nutr 1999; 23: 363–365.
Corso F A, Shaul D B, Wolfe B M . Spinal osteomyelitis after TPN catheter-induced septicemia. JPEN J Parenter Enteral Nutr 1995; 19: 291–295.
Nightingale J M, Simpson A J, Towler H M, Lennard-Jones J E. Fungal feeding-line infections beware: the eyes and the teeth. J R Soc Med 1995; 88: 258–263.
Culkin A, Gabe S M, Bjarnason I, Grimble G, Madden A M, Forbes A . A double-blind, randomized, controlled crossover trial of glutamine supplementation in home parenteral nutrition. Eur J Clin Nutr 2008; 62: 575–583.
Pennington C R . Parenteral nutrition. In Nightingale J (ed) Intestinal failure. pp 497–511. London: Greenwich Medical Media Limited, 2001.
Spuller R L . The central indwelling venous catheter in the paediatric patient – dental treatment considerations. Spec Care Dentist 1988; 8: 74–76.
French G L . How should prophylactic antibiotics be used during dental work or bacteraemia associated procedures? Paed Nephrol 1993; 7: 346.
Aptekar A, Sandor G K B . Point of Care. What precautions do I need to take when providing dental treatment to a patient with a central venous catheter? JCDA 2006; 72: 619–628.
Chambers A, Hennessey E, Powell-Tuck J. Longitudinal trends in quality of life after starting home parenteral nutrition: a randomised control study of telemedicine Clin Nutr 2006; 25: 505–514.
The Oley Foundation. HPN complication chart. 2009. Online article available at http://www.oley.org/charts/newHPN.pdf (accessed December 2011).
Wylie I . Oral healthcare for older people: 2020 vision. Gerodontology 2003; 20: 60–62.
Machuca G, Nieves E, Sanchez A F, Machuca C, Bullon P . Descriptive study factors modifying the periodontal status of a population of people with a learning disability in Spain. J Disabil Oral Health 2007; 8: 73–80.
Tiller S, Wilson K I, Gallagher J E . Oral health status and dental service use of adults with learning disabilities living in residential institutions and in the community. Community Dent Health 2001; 18: 167–171.
Ellervall E, Brehmer B, Knutsson K . How confident are general dental practitioners in their decision to administer antibiotic prophylaxis? A questionnaire study. BMC Med Inform Decis Mak 2008; 8: 57.
Kiyak H A . Impact of patients' and dentists' attitudes on older persons' use of dental services. Gerodontics 1988; 4: 331–335.
Kelly M, Steele J, Nuttall N et al. Adult dental health survey: oral health in the UK 1998. London: The Stationery Office, 2000.
British Association for Parenteral and Enteral Nutrition. Annual BANS report 2010. Artificial nutrition support in the UK 2000–2009. Redditch: BAPEN, 2010. Online article available at http://www.bapen.org.uk/pdfs/bans_reports/bans_report_10.pdf (accessed December 2010).
Scolapio J S, Fleming C R, Kelly D G, Wick D M, Zinsmeister A R . Survival of home parenteral nutrition patients: 20 years of experience at the Mayo Clinic. Mayo Clin Proc 1999; 74: 217–222.
Lloyd D A J, Vega R, Bassett P, Forbes A, Gabe S M . Survival and dependence on home parenteral nutrition: experience over a 25-year period in a UK referral centre. Aliment Pharmacol Ther 2006; 24: 1231–1240.
Jeejeebhoy K N . Treatment of intestinal failure: transplantation or home parenteral nutrition? Gastroenterology 2008; 135: 303–305.
Irving M H . An intestinal failure unit. In Nightingale J (ed) Intestinal failure. pp 469–473. London: Greenwich Medical Media Limited, 2001.
Gould F K, Elliott T S, Foweraker J et al. Guidelines for the prevention of endocarditis: report of the Working Party of the British Society for Antimicrobial Chemotherapy. J Antimicrob Chemother 2006; 57: 1035–1042.
Dajani A S, Taubert K A, Wilson W et al. Prevention of bacterial endocarditis. Recommendations by the American Heart Association. JAMA 1997; 277: 1794–1804.
Arendorf T M, Walker D M . The prevalence and intra-oral distribution of Candida albicans in man. Arch Oral Biol 1980; 25: 1–10.
Wilson J . The aetiology, diagnosis and manage-ment of denture stomatitis. Br Dent J 1998; 185: 380–384.
Acknowledgements
The authors would like to express appreciation for the help of the UK HPN Group membership, in particular Janet Baxter PhD, Clinical Network Manager, Dr Emma Greig PhD MRCP (BAPEN Medical), the contribution and guidance of Dr Janice Fiske OBE MPhil and statistical support from Ron Wilson, KCL Dental Institute. Alison Lee is grateful for the facilitation of this study by Hillingdon Community Health Dental Referral Service.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Lee, A., Gabe, S., Nightingale, J. et al. Oral health, dental prophylaxis and catheter related bloodstream infections in home parenteral nutrition patients: results of a UK survey and cohort study. Br Dent J 212, E4 (2012). https://doi.org/10.1038/sj.bdj.2012.50
Accepted:
Published:
Issue date:
DOI: https://doi.org/10.1038/sj.bdj.2012.50