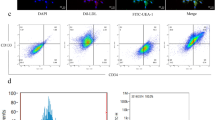
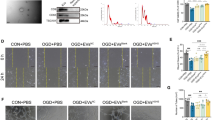
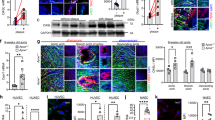
Abstract
Ischemic preconditioning (IPC) strongly protects against ischemia/reperfusion (I/R) injury; however, the molecular mechanism involved in delayed preconditioning-induced endothelial protection in peripheral arteries is unknown. Therefore, we examined using functional, morphologic and molecular biologic studies whether delayed IPC decreases formation of reactive oxygen species and upregulates endothelial nitric oxide synthase (eNOS) that in turn contributes to vascular endothelial protection. Adult male Sprague–Dawley rats were subjected to 30-min ischemia induced by mesenteric artery occlusion followed by 60-min reperfusion 24 h after sham surgery or preconditioning (three cycles of 5-min ischemia/5-min reperfusion). Delayed preconditioning prevented the I/R-induced impairment of endothelium-dependent relaxations to acetylcholine (maximal relaxation: sham 91.4±2.2%; I/R 54.0±4.0%; IPC 80.2±6.3%). This protective effect was abolished by NOS inhibitor NG-nitro-L-arginine methyl ester and not changed by ascorbic acid. Electron microscopy showed marked endothelial damage after I/R and the ultrastructural changes were prevented by delayed preconditioning. Following I/R, the impairment of eNOS phosphorylation and expression was observed in mesenteric vessels. Furthermore, phosphatidylinositol 3-kinase (PI3K) and Akt phosphorylation were reduced, although total PI3K and Akt remained unchanged. IPC restored I/R-induced impairment of eNOS expression and activity. This was possibly the result of the recovery of PI3K/Akt phosphorylation. Furthermore, I/R increased serum level of malondialdehyde, intravascular superoxide and nitrotyrosine generation, which were abrogated by IPC. These results suggest that delayed preconditioning prevented I/R-induced endothelial injury in peripheral resistance vasculature, both in terms of functional and structural changes. Endothelial protection afforded by delayed IPC is associated with inhibition of oxidative stress and upregulation of PI3K/Akt/eNOS pathway.
Similar content being viewed by others
Main
Ischemia followed by reperfusion leads to tissue injury in various pathophysiological conditions. The endothelium of blood vessel is the most directly exposed tissue to the deleterious consequences of ischemia/reperfusion (I/R). Substantial evidence has accumulated that I/R produces vascular endothelial dysfunction as defined by abrogated endothelium-dependent dilation.1, 2, 3, 4 Moreover, the arterial endothelial nitric oxide synthase (eNOS) protein expression is severely reduced after I/R injury.3 Given the well-known role of nitric oxide (NO) not only as a vasodilator but also as an inhibitor of neutrophil adhesion and platelet aggregation,5, 6, 7 the amelioration of the endothelial dysfunction associated with I/R through the maintenance of an adequate level of eNOS could be important. Reactive oxygen/nitrogen species (ROS/RNS) generation on reperfusion is also generally accepted as a contributing factor to I/R-induced vascular injury.2 Superoxide and NO can react to the powerful oxidant and nitrating agent peroxynitrite (ONOO−), reducing the bioavailability of NO and thus resulting in vascular dysfunction.8 Nitration of functional proteins further contributes to cellular injury, thus suggesting that oxygen radical formation acts as a triggering mechanism for endothelial dysfunction.
Ischemic preconditioning (IPC) is the phenomenon in which brief periods of ischemia followed by reperfusion increases resistance to a subsequent prolonged ischemic stress.9, 10 IPC is an important mechanism by which diverse tissues protect themselves from impending I/R damage. There are two phases of protection afforded by IPC, that is, the early phase and the late phase.11 This study focuses on the late phase of IPC, termed delayed preconditioning, because delayed IPC confers a longer window of cytoprotection and has greater significance for cardiovascular protection.12 The molecular mechanisms and mediators that account for delayed IPC have been extensively investigated, and it has emerged that eNOS has a key role in this phenomenon in the heart.9, 13 In addition, IPC was reported to reduce the generation of cardiac ROS/RNS after both the acute and late phase of postischemic reperfusion.14, 15
Most of the studies on preconditioning have focused on its capacity to protect cardiac myocytes. Although there is some evidence that the protective effects of both early and delayed IPC extend to endothelial cells,16, 17 the molecular signaling pathways that specifically mediate the effects of delayed IPC in the vascular endothelium have not been elucidated. In addition, disturbance in peripheral vascular resistance are basic contributors to different cardiovascular pathologies and mesenteric arteries are an essential constituent of peripheral resistance vessels.18, 19, 20 Therefore, the aim of this study was to investigate the effects of delayed IPC on endothelial function and morphology, as well as the involvement of ROS in mesenteric resistance arteries. The activation of phosphatidylinositol 3-kinase (PI3K)/Akt/eNOS signaling pathway as possible mechanism recruited by IPC in the peripheral arteries was also assessed.
MATERIALS AND METHODS
Animals
Adult male Sprague–Dawley rats (8–10 weeks old) were purchased from the Experimental Animal Center of Xi’an Jiaotong University. Animals were maintained under standard laboratory conditions, housed in cages in a room kept at 24 °C under a 12-h dark–light cycle and had unlimited access to water and standard rat chow. All experimental procedures were performed in accordance with the Guidelines for the Care and Use of Laboratory Animals issued by the Chinese Council on Animal Research and the Guidelines of Animal Care. This study was approved by the ethics committee of Xi’an Jiaotong University. All surgery was performed under sodium pentobarbital anesthesia, and all efforts were made to minimize suffering.
Experimental Protocol
Adult male Sprague–Dawley rats were randomly divided into three experimental groups (Figure 1). On day 1, rats were anesthetized with sodium pentobarbital (40 mg/kg, intraperitoneal injection) and subjected to abdominal surgery. Through a midline abdominal incision, the superior mesenteric artery was isolated meticulously at its origin. The rats were given 200 IU heparin intravenously. Rats from IPC group (group 3) were subjected to three cycles of 5-min mesenteric occlusion and 5-min reperfusion. The abdominal incision was closed. Rats from the sham group (group 1) and I/R group (group 2) were treated identically, omitting the superior mesenteric artery occlusion. All rats were closely monitored after recovering from anesthesia, and given free access to water.
Experimental groups and treatment protocols. Solid boxes indicate periods of ischemia induced by the mesenteric artery occlusion, and open boxes indicate periods of reperfusion. Ischemic preconditioning (IPC) was performed by occlusion of the artery for three cycles of 5-min ischemia followed by 5-min reperfusion. All animals were left 24 h before the ischemia/reperfusion (I/R) protocol. This consisted of 30-min artery occlusion followed by 60-min reperfusion.
Twenty-four hours after preconditioning or sham ischemia (day 2), rats were re-anesthetized. The abdomen was reopened and ischemia was induced as described above. Animals were subjected to 30-min ischemia followed by 60-min reperfusion. Sham animals (group 1) were treated identically except that the artery was not occluded. After the I/R protocol, rats were killed by cervical dislocation under anesthesia for dissection of mesenteric arteries.
Mesenteric Artery Preparation and Isometric Tension Measurement
The superior mesenteric artery was gently removed and immersed immediately in cold, oxygenated Krebs’ solution (in mmol/l: NaCl, 119; KCl, 4.7; CaCl2, 2.5; MgCl2, 1; NaHCO3, 25; KH2PO4, 1.2; and D-glucose, 11). Adherent fat and connective tissue were removed from the arteries, which were then cut into rings of approximately 2–3-mm length under a dissection microscope.19, 21 Care was taken during the dissecting procedure to protect the endothelium from inadvertent damage.
Isometric tension was measured as previously described.19, 20 Organ chambers (2-ml volume) were filled with the Krebs’ solution (37 °C and gassed with 95% air and 5% CO2; pH 7.4). Each ring was mounted on two L-shape stainless-steel holders, one of which was fix to the organ bath and the other connected to a force displacement transducer (Beijing Aeromedicine Engineering Research Institute, Beijing, China) attached to a Taimeng BL-420 biotic signal collection and analysis system (Taimeng Instruments, Chengdu, China) for continuous recording of isometric tension. Mesenteric arterial rings with endothelium were allowed to stabilize for 90 min under a resting tension of 0.5 g and the incubation solution was replaced every 15 min. At the end of the equilibration period, the contractile capacity of each ring was tested by exposure to a high-K+ Krebs’ solution (obtained by equimolar replacement of NaCl by KCl in the Krebs’ solution), and the ring was considered viable and used for experiments only if two reproducible high-K+ contractions were obtained.20, 22
Vascular Reactivity Studies
Endothelium-dependent and -independent relaxations were assessed by measuring the dilatory responses of mesenteric arteries to cumulative concentrations of acetylcholine (ACh; 10−10–10−5 mol/l) and sodium nitroprusside (SNP; 10−10–10−5 mol/l), respectively. All experiments were performed in vessels pre-contracted with phenylephrine (PE; 10 μmol/l). To avoid the possibility that PE might induce different contractility in vessels from sham-operated, I/R, or preconditioning-treated animals and to establish which PE concentration was capable of eliciting similar contractions among the groups, we performed a concentration-response analysis of PE effects (from 1 nmol/l to 100 μmol/l) in preliminary experiments. After the titration study, the dose of 10 μmol/l PE, which induced similar contractile responses in all of the groups, was selected. To evaluate NO availability, concentration-response curves to ACh were repeated after 30-min preincubation with the NOS inhibitor NG-nitro-L-arginine methyl ester (L-NAME; 100 μmol/l). To assess the influence of ROS on endothelial function, the responses to ACh were determined after 30-min incubation with ascorbic acid (100 μmol/l). After completing each concentration-response curve, rings were washed out three times with fresh Krebs’ solution and allowed a 45-min equilibration period in Krebs’ solution before exposure to the next agent.
Hematoxylin and Eosin Staining and Immunohistochemistry
Rat superior mesenteric arteries were carefully isolated, and then fixed with 4% paraformaldehyde for <48 h. Samples were dehydrated and embedded in paraffin, and 5 μm sections were cut with a Leica RM-2162 (Leica; Bensheim, Germany) for hematoxylin and eosin staining and immunohistochemistry for eNOS. Immunohistochemical detection of eNOS was performed as previously described.23 The arterial sections were incubated with blocking solutions (5% bovine serum albumin) and then with rabbit anti-eNOS antibody (1:200 dilution; Cell Signaling Technology, Beverly, MA, USA) overnight at 4 °C. The sections were then washed with phosphate-buffered saline (PBS; three times for 2 min each) and incubated at 37 °C in biotin-conjugated goat anti-rabbit immunoglobulin for 30 min. They were rinsed three times for 5 min each in fresh PBS and reacted with a streptavidin–biotin complex conjugated with peroxidase at 37 °C for 30 min. Visualization of the chromogen (horseradish peroxidase) was performed by incubating the sections with 3,3′-diaminobenzidine tetra-hydrochloride (Boster Bio-Engineering, Wuhan, China) for 4 min. Finally, slides were dehydrated, cleared and mounted for light microscopy.
Transmission Electron Microscopy
Rat superior mesenteric arteries were gently isolated and fixed with 2.5% glutaraldehyde in 0.1 mol/l phosphate buffer (pH 7.2–7.4) for 2 h at 4 °C. After washing in phosphate buffer, the arteries were postfixed in 1% osmium tetroxide in 0.1 mol/l phosphate buffer for 2 h. Tissues were dehydrated in a graded ethanol series, infiltrated with propylene oxide and embedded in Epon 812. Toluidine blue-stained sections (1 μm) were examined by light microscopy, and appropriate areas of tissues were selected for cutting thin sections (LKB-V). Thin sections were stained with uranyl acetate and lead citrate, and examined by a transmission electron microscope (H-7650; Hitachi, Tokyo, Japan).
Arterial RNA Extraction and Reverse Transcription-Polymerase Chain Reaction
Expression of mRNA for eNOS was assessed by reverse transcription (RT)-polymerase chain reaction (PCR). Specimens of mesenteric vessels were disrupted with cold glass pestles, and total RNA was isolated by RNAiso Plus reagent (Takara Bio, Shiga, Japan) and chloroform. Each sample was treated with RNase-free DNase. Total RNA purity and concentration were determined by measurement of spectrophotometric optical density (260 and 280 nm). A 1 μg sample of RNA was reverse-transcribed to first-strand cDNA using PrimeScript RT reagent kit (Takara Bio). The PCR system contained 2 μl template cDNA, 0.5 μl forward primer, 0.5 μl reverse primer, 10 μl Taq PCR Mix (Xi'an Runde Biotechnology, Xi'an, China) and 7 μl ddH2O to a total volume of 20 μl. To amplify specific gene products, the following primers were used: eNOS forward: 5′-GGAGAAGATGCCAAGGCTGCTG-3′, reverse: 5′-CTTCCAGTGTCCAGACGCACCA-3′, 224 bp; mouse glyceraldehyde 3-phospharte dehydrogenase (GAPDH) was co-amplified as an internal control using the following primer sequence: GAPDH forward: 5′-CGGAGTCAACGGATTTGGTCGTAT-3′, reverse: 5′-AGCCTTCTCCATGGTGGTGAAGAC-3′, 306 bp. Primers were synthesized by GenScript Biotechnology (Nanjing, China). For eNOS, amplification conditions were: 3 min at 95 °C, 30 s at 60 °C and 45 s at 72 °C for 35 cycles. PCR products were separated by 2% agarose gel electrophoresis (70 V, 60 min) and stained with ethidium bromide. The intensity of the bands was captured by an image analysis scanning system (Peiqing, Shanghai, China). Results were normalized against those of the housekeeping gene GAPDH. The specific primers used were designed by PRIMER PREMIER 5.0 version software (Premier Biosoft International, La Jolla, CA, USA).
Western Blotting
Mesenteric arteries were homogenized in RIPA lysis buffer (Beyotime Biotech, Haimen, China) containing 1 mmol/l phenylmethylsulfonyl fluoride. The lysates were centrifuged at 12 000 r.p.m. for 15 min at 4 °C, and the supernatants were collected as the tissue protein extracts and were stored at −80 °C. Total protein concentrations were determined using Bicinchoninic acid protein assay kit (Beyotime Biotech). Samples (20 μg) were separated electrophoretically by 8% SDS-poly-acrylamide gel electrophoresis, and then electrotransferred onto polyvinylidene difluoride membrane (Millipore, Billerica, MA, USA). After blocking with 3% bovine serum albumin in Tris-HCl-buffered saline with 0.1% Tween 20 for 30 min at room temperature, the membranes were incubated at 4 °C overnight with primary antibody against PI3K (1:1000 dilution; Millipore), Akt (1:1000 dilution; Cell Signaling Technology), eNOS (1:1000 dilution; Cell Signaling Technology), phospho-PI3K (p85; 1:1000 dilution; Cell Signaling Technology), phospho-Akt (Ser473; 1:1000 dilution; Cell Signaling Technology), and phospho-eNOS (Ser1177; 1:1000 dilution; Cell Signaling Technology). The blots were then washed before incubation with horseradish peroxidase-linked secondary antibody (1:5000; Cowin Biotech, Beijing, China) for 30 min at room temperature. GAPDH was also determined and used as the internal loading control. The bands were visualized with ECL-Plus reagent (Millipore) and graphs were analyzed by the Gel-Pro Analyzer (Media Cybernetics, Bethesda, MD, USA).
Determination of Serum NOx and MDA
Arterial blood samples were collected from the carotid artery at the end of the reperfusion period. Blood samples were centrifuged at 3000 r.p.m. for 10 min at 4 °C and serum was aliquoted and stored at –80 °C until assay. The contents of nitrate/nitrite (NOx, NO metabolite) and malondialdehyde (MDA) were determined using colorimetric assay with commercially available kits (Jiancheng Bioengineering Institute, Nanjing, China) according to the manufacturer’s instructions.
Briefly, total NOx, an index of NO production, was determined using nitrate reductase to specifically reduce nitrate to nitrite; the latter was quantified by a colorimetric assay. Absorbance was determined at 550 nm on a Stat Fax 2100 spectrophotometer (Awareness Technology, Palm City, FL, USA).19, 24 The MDA content in serum was measured using the thiobarbituric acid method, based on the formation of a red complex when MDA reacts with thiobarbituric acid. Absorbance was measured spectrophotometrically at 532 nm.19, 25
In situ Detection of Vascular Superoxide Anion Production
The oxidative fluorescent dye dihydroethidium (DHE) was used to evaluate in situ production of superoxide anion, as described previously.19, 26 In brief, frozen tissue segments were cut into 30 μm-thick sections in a cryostat (HM500 OM; Microm International, Walldorf, Germany) and placed on poly-L-lysine-coated slides. The sections were incubated in 2 μmol/l DHE (Beyotime Biotech) in Krebs-HEPES buffer (in mmol/l: NaCl, 99.01; KCl, 4.69; CaCl2, 1.87; MgSO4, 1.20; KH2PO4, 1.03; NaHCO3, 25.0; Na-HEPES, 20.0; and glucose, 11.1; PH 7.4) at 37 °C for 30 min in a light-protected humidified container. DHE is freely permeable to cells and in the presence of superoxide anion is oxidized to ethidium, which intercalates in DNA, thereby exhibiting a red fluorescence. Tissue sections were then visualized with an inverted fluorescence microscope (TE-2000U, Nikon, Japan), and images were collected and stored digitally. The mesenteric arteries from the sham-operated, I/R and IPC-treated rats were processed in parallel, and images were acquired with identical acquisition parameters. Quantitative analysis of superoxide anion production was performed with Image-Pro Plus 5.0 (Media Cybernetics, Silver Spring, MD, USA). The vascular tissue was manually defined for each image. A target definition was used to avoid reading background staining. All measurements were conducted blind. The integrated optical density (IOD) in the target region was calculated.
Determination of Nitrotyrosine by Immunofluorescence
Cryosections (14 μm) of mesenteric arteries embedded in Tissue-Tek OCT (Sakura Finetek Europe, Zoeterwoude, The Netherlands) were fixed with 4% paraformaldehyde in PBS. After blockade, sections were incubated overnight at 4 °C with a mouse monoclonal antibody against nitrotyrosine (1:100; Millipore) in antibody dilution buffer (Beyotime Biotech) in a humidified chamber. After three washes in PBS, rings were incubated with the secondary antibody, a goat anti-mouse conjugated to fluorescein isothiocyanate (Zhongshan Goldenbridge Biotechnology, Beijing, China), at a dilution of 1:200 for 1 h at 37 °C in a humid container. After washing, immunofluorescent signals were viewed using an inverted Nikon TE-2000U fluorescence microscope, using the same imaging settings in each case. The specificity of the immunostaining was evaluated by omission of the primary antibody and processed as described above. Under these conditions, no staining was observed in the vessel wall in any experimental situation. Quantitative analysis of nitrotyrosine fluorescence was performed with Image-Pro Plus 5.0 (Media Cybernetics). The IOD was calculated. All measurements were conducted blind.
Drugs
ACh, PE and SNP were obtained from Sigma (St Louis, MO, USA). All other reagents were of analytical reagent grade. All drugs were dissolved in distilled water. Drug concentrations are expressed as the final molar concentration within the organ chamber.
Statistical Analysis
Maximal ACh- and SNP-induced responses (Emax) are calculated as a percentage reduction of the PE (10 μmol/l) -induced maximum contraction. Results are presented as mean±s.e.m., and n indicates the number of rats. Statistical analysis was performed by Student’s t-test or one-way analysis of variance followed by Turkey post hoc test for multiple comparisons. P<0.05 was considered statistically significant. All figures were prepared with GraphPad Prism 5.0 (San Diego, CA, USA).
RESULTS
Effects of IPC Treatment on I/R-Induced Endothelial Dysfunction in Mesenteric Arteries
In mesenteric arteries isolated from sham animals, ACh elicited concentration-dependent relaxations that reached 91.4±2.2% at the highest dose (Figures 2a and b). Compared with sham animals, ACh-induced vasorelaxation was significantly attenuated in mesenteric arteries taken from animals subjected to I/R (Emax: 54.0±4.0%; P<0.001; Figures 2a and b). This impairment was prevented by IPC performed 24 h before prolonged ischemia (Emax: 80.2±6.3%; P<0.001 vs I/R; Figures 2a and b). Moreover, no significant differences in the vasorelaxing response to the exogenous NO donor SNP were observed between the different experimental groups, indicating that the function of smooth muscle was preserved (Figures 2c and d).
Delayed preconditioning prevents ischemia/reperfusion (I/R)-induced endothelial dysfunction. Representative traces and concentration-response curves to acetylcholine (ACh) (a, b) and sodium nitroprusside (SNP) (c, d) in phenylephrine (PE)-precontracted intact mesenteric artery rings obtained from the sham-operated group, I/R group and ischemic preconditioning (IPC)-treated group. Values are the mean±s.e.m. (n=8 in each group). *P<0.001 compared with the sham-operated group; #P<0.001 compared with the I/R group (ANOVA followed by Tukey’s test).
Administration of the NOS inhibitor L-NAME (100 μmol/l) reduced the vasodilatory responses to ACh compared with the sham-operated group (Emax: sham: 91.4±2.2%, sham+L-NAME: 53.9±2.5%, P<0.001; Figure 3a). In rats subjected to I/R without delayed preconditioning, the diminished relaxing responses were not further reduced by treatment with L-NAME. The maximal responses to ACh were 54.0±4.0% and 46.9±4.0% in arteries taken from I/R group in the absence and presence of L-NAME, respectively (P>0.05; Figure 3b). In addition, L-NAME abolished the protective effect of delayed preconditioning (Emax: IPC: 80.2±6.3%, IPC+L-NAME: 49.5±5.7%, P<0.001; Figure 3c).
The effect afforded by delayed ischemic preconditioning (IPC) was abolished by nitric oxide synthase (NOS) inhibitor and not changed by reactive oxygen species (ROS) scavenger. Effects of NG-nitro-L-arginine methyl ester (L-NAME; 100 μmol/l) and ascorbic acid (100 μmol/l) on concentration-response curves to acetylcholine (ACh) in phenylephrine (PE)-precontracted intact mesenteric artery rings from the sham-operated group (a), the ischemia/reperfusion (I/R) group (b) and the IPC-treated group (c). Data are the mean±s.e.m. (n=8 per group). *P<0.001 vs respective control by Student’s t-test.
To assess the influence of ROS on endothelial function, the responses to ACh were determined after 30-min incubation with ascorbic acid (100 μmol/l). In sham-operated animals, ascorbic acid failed to modify the relaxation to ACh (Emax: sham: 91.4±2.2%, sham+ascorbic acid: 95.8±1.7%, P>0.05; Figure 3a). In vessels from I/R rats, ascorbic acid normalized the ACh-induced relaxation (Emax: I/R: 54.0±4.0%, I/R+ascorbic acid: 84.2±4.0%, P<0.001; Figure 3b). In rats subjected to I/R with delayed preconditioning, relaxation to ACh was not affected by ascorbic acid (Emax: IPC: 80.2±6.3%, IPC+ascorbic acid: 92.3±2.1%, P>0.05; Figure 3c).
Effects of IPC Treatment on I/R-Induced Endothelial Structural Damage in Mesenteric Arteries
To examine whether IPC prevented the structural damage caused by I/R, we observed the microstructure and ultrastructure of mesenteric artery endothelial cells by hematoxylin and eosin staining and transmission electron microscopy, respectively. Compared with the sham-operated group, smooth muscle layers were directly exposed to the vessel lumen because of endothelial cell desquamation in the I/R group (Figure 4). The ultrastructure of the I/R group appeared that cytoplasm contained clear vacuoles, the membrane of the endothelial cells was not intact and the internal elastic membrane was ruptured (Figure 5). As shown in Figures 4 and 5, abnormal structure of endothelium was not found in the IPC group. In all mesenteric arteries studied, transmission electron microscopy showed normal smooth muscle cells.
The microstructural changes in mesenteric artery. Hematoxylin and eosin staining showed that in the sham-operated group (a), the microstructure of mesenteric artery endothelial cells was normal; in the ischemia/reperfusion (I/R) group (b), endothelial structure was damaged. Desquamation of endothelial cell was present; whereas in the ischemic preconditioning (IPC)-treated group (c), the damage of endothelial structure was not observed. Arrows indicate mesentery artery endothelial cells. Scale bar =10 μm.
The ultrastructural changes in mesenteric artery. Under transmission electron microscopy (uranyl acetate/lead citrate staining), it was observed that in rats in the sham-operated group (a, d), structure of endothelial cells was clearly observed; in the ischemia/reperfusion (I/R) group (b, e), cytoplasm contained clear vacuoles, the membrane of the endothelial cells was not intact, and the internal elastic membrane was ruptured; whereas in the ischemic preconditioning (IPC)-treated group (c, f), the ultrastructure of endothelial cells is similar to the sham-operated group. (a–c) Vessel cross sections. (d–f) Vessel longitudinal sections. Arrows indicate mesentery artery endothelial cells. Scale bar =1 μm.
Measurement of Serum NOx Content
As NO is believed to be a key mediator of IPC, we measured NO production by the nitrate reductase method. Figure 6a showed a significant reduction in serum NOx content (an indication of NO level) in the I/R group compared with the sham-operated group (P<0.01). In addition, an obvious reversal was achieved in the IPC group (P<0.01 vs I/R).
Delayed ischemic preconditioning (IPC) prevents decline in the expression and activation of endothelial nitric oxide synthase (eNOS) caused by ischemia/reperfusion (I/R) in arteries. (a) Effects of I/R and IPC on serum total nitrate/nitrite (NOx) content. (b) Immunostaining for eNOS in mesenteric arteries from the sham-operated, I/R and IPC-treated groups. Positive immunoreaction is observed as a brown precipitate (arrows). Scale bar =10 μm. (c) Upper panels, representative agarose gel showing RT-PCR products for eNOS in mesenteric vessels from the sham-operated, I/R and IPC-treated groups. Bottom panels, column graph referring to densitometric analysis of eNOS complementary DNA (cDNA) bands normalized to the expression of glyceraldehyde 3-phosphate dehydrogenase (GAPDH). (d) Effects of I/R and IPC on phosphorylation and protein expression of eNOS in mesenteric arteries. Left, representative western blots of phospho-eNOS (top), total eNOS (middle), and GAPDH (bottom). Right, bar graphs summarizing the western blot data. Data are the mean±s.e.m. (n=6 per group). *P<0.05, **P<0.01 vs the sham-operated group; ##P<0.01 vs the I/R group (ANOVA followed by Tukey’s test).
Effects of I/R and IPC Treatment on eNOS Expression and Activity in Mesenteric Arteries
eNOS has been shown to have a critical role in vasorelaxation. Therefore, in this study we examined the effects of I/R and IPC on eNOS expression. Immunohistostaining of non-I/R vessels with anti-eNOS antibody revealed prominent signals for eNOS only in arterial endothelium. In the I/R mesenteric arteries, a weak eNOS immunopositivity was detected. By contrast, in vessels subjected to IPC, a marked enhancement in eNOS immunostaining was observed (Figure 6b). The densitometry results of mRNA expression for eNOS controlling by GAPDH were shown in Figure 6c. Our data showed that I/R resulted in a significant decrease in eNOS mRNA expression in mesenteric arteries compared with the sham-operated rats, as determined with RT-PCR (P<0.05; Figure 6c). In addition, IPC enhanced eNOS mRNA expression as compared with the I/R group (P<0.01; Figure 6c). A marked decrease in the eNOS protein level was observed in mesenteric artery following I/R injury (P<0.05 vs sham; Figure 6d). Furthermore, I/R injury reduced phosphorylation/activation of eNOS at Ser1177 (P<0.01 vs sham; Figure 6d). IPC significantly reversed I/R-induced reduction in eNOS phosphorylation and total eNOS expression (P<0.01 vs I/R; Figure 6d). These results suggested that eNOS downregulation might be a potential mechanism in the impairment of NO-mediated vasodilation in I/R, and IPC conferred endothelial protection by upregulating eNOS expression and activity.
Effects of I/R and IPC Treatment on PI3K and Akt Expression and Activity in Mesenteric Arteries
We then focused our interest on the molecular pathway that regulates IPC-induced eNOS upregulation. Previous studies have demonstrated that eNOS is a novel substrate for Akt and Akt has a key role in promoting endothelial NO production and vasorelaxation.27, 28 Therefore, the phosphorylation of Akt was tested. The results of western blot analysis revealed that Akt phosphorylation was reduced after I/R, although total Akt showed equal protein levels in all samples (P<0.01 vs sham; Figure 7b). IPC resulted in increased phosphorylation of Akt (P<0.01 vs I/R; Figure 7b). Next, we explored PI3K, the upstream target of Akt. The present data showed that the phosphorylation of PI3K was diminished without changes in the total amount of PI3K (P<0.05 vs sham; Figure 7a). IPC strongly prevented the prominent reduction in PI3K phosphorylation caused by I/R injury (P<0.05; Figure 7a). Together these experiments indicated that IPC might activate PI3K/Akt signaling pathway, which, in turn, interact with and phosphorylate eNOS.
Delayed ischemic preconditioning (IPC) prevents decrease in the phosphatidylinositol 3-kinase (PI3K)/Akt phosphorylation. In the top trace of each panel, representative western blots of phospho-PI3K and total PI3K (a) or phospho-Akt and total Akt (b) are shown. In the bottom trace, a bar graph summarizing the western blot data are shown. Values are the means±s.e.m. (n=6 per group). *P<0.05, **P<0.01 vs the sham-operated group; #P<0.05, ##P<0.01 vs the I/R group (ANOVA followed by Tukey’s test).
Effects of I/R and IPC on Vascular Superoxide Anion Generation and Serum MDA Content
To characterize and localize vascular superoxide anion production within the vessels, ethidium red fluorescence was analyzed in sections incubated with DHE. Figure 8 showed an increased production of superoxide anion from mesenteric vessels in the I/R group compared with sham-operated group (P<0.001 vs sham). IPC abrogated superoxide production (P<0.001 vs I/R; Figure 8a). The I/R rats also displayed higher MDA serum content (P<0.001 vs sham), and such an increment was attenuated by IPC (P<0.001 vs I/R; Figure 8b).
Measurement of oxidative stress in mesenteric arteries. (a) Dihydroethidium (DHE) staining for superoxide detection. Representative fluorescence photomicrographs (top) and quantification (bottom) of microscopic sections of rat mesenteric arteries from sham-operated, ischemia/reperfusion (I/R) and ischemic preconditioning (IPC)-treated group. Vessels were labeled with the oxidative dye DHE, which produce a red fluorescence when oxidized to ethidium by superoxide anion. Scale bar =200 μm. (b) Effects of I/R and IPC on serum malondialdehyde (MDA) content. Data are presented as mean±s.e.m. (n=6 per group). *P<0.001 compared with the sham-operated group; #P<0.001 compared with the I/R group (ANOVA followed by Tukey’s test).
Effects of I/R and IPC on Nitrotyrosine Immunofluorescence
NO can react with superoxide anion, leading to ONOO−, which can induce protein nitration.29 As shown in Figure 9, weak fluorescence for nitrotyrosine was found on mesenteric arteries from the sham-operated animals. However, a marked increase in nitrotyrosine immunofluorescence was observed after I/R. IPC treatment normalized vascular nitrotyrosine staining. The negative control obtained with the secondary antibodies did not displayed fluorescence (data not shown). Nitrotyrosine staining, which reflects the endogenous formation of ONOO−, confirmed the results obtained with DHE.
Determination of nitrotyrosine by immunofluorescence in mesenteric arteries. Representative photomicrographs (top) and quantification (bottom) of nitrotyrosine immunofluorescence of microscopic sections of rat mesenteric arteries from sham-operated, ischemia/reperfusion (I/R) and ischemic preconditioning (IPC)-treated group. Scale bar =200 μm. Data are presented as mean±s.e.m. (n=6 per group). *P<0.001 compared with the sham-operated group; #P<0.001 compared with the I/R group (ANOVA followed by Tukey’s test).
DISCUSSION
The salient findings of this study are that delayed IPC prevented endothelial dysfunction and morphological injuries induced by I/R in peripheral vessels. We also found that IPC reduced serum level of MDA, intravascular superoxide and nitrotyrosine generation. Molecular evidence indicated that PI3K/Akt/eNOS pathway was significantly upregulated after IPC. These results suggest that delayed IPC initiates inhibition of ROS, which induces abrogation of protein tyrosine nitration and activation of PI3K/Akt/eNOS pathway, leading to endothelial protection. We believe that our findings provide further understanding of the mechanism(s) underlying endothelial protection afforded by delayed IPC.
The mechanisms of I/R injury are multifactorial and incompletely understood. The vascular endothelium is implicated in the pathogenesis of I/R injury; deterioration of endothelial dilator and anticoagulant function during I/R injury may aggravate vasospasm and encourage persistence and accumulation of cellular aggregates and thrombus within conduit and resistance vessels. These aspects of endothelial dysfunction may directly affect the extent of tissue reperfusion.16 In this study, vasodilatations to ACh but not to SNP were impaired in vessels from the I/R rats, indicating an endothelium-dependent impairment. Our electron-microscopic studies also showed severe endothelial injury characterized by marked cytoplasmic vacuolation and elastic membrane fragmentation. The observed endothelial dysfunction could be a consequence of a decrease in the synthesis or bioavailability of NO. Analysis of enzymes accounting for NO production showed decreased expression and phosphorylation of eNOS in mesenteric arteries from rats subjected to I/R. Moreover, L-NAME did not induce further abrogation of cholinergic relaxation in vessels from the I/R rats. These results further support that the observed endothelial dysfunction is characterized by a marked reduction in stimulated NO availability.
On the other hand, I/R is associated with large increases in the production of ROS.30 It is well known that oxidative stress has a crucial role in the pathogenesis of vascular dysfunction observed in vascular diseases.31, 32 In this study, DHE fluorescence microscopy showed that mesenteric arteries from the I/R rats presented an enhanced formation of superoxide anion. These findings were accompanied by a profound increase in serum level of MDA, a marker of lipid peroxidation that occurs as a result of the damaging effects of ROS. The fact that ascorbic acid reverted the observed impairment of the ACh vasodilatation induced by I/R further supports the participation of ROS on the observed endothelial dysfunction.
It is well established that superoxide radicals scavenge endothelium-derived NO and produce ONOO−.33 Breakdown of ONOO− produces highly toxic ROS/RNS, and these radicals promote the post-translational modification of tyrosine to nitrotyrosine, which affects the tertiary structure and conformation of target proteins and can compromise their function.29, 34 The presence of nitrated proteins has been implicated in many disease states including I/R injury.35, 36 Our data showed that the tissue protein levels of nitrotyrosine were much higher after I/R relative to the sham-operated rats. Therefore, we hypothesized that the nitrated proteins may experience a loss of function, which attenuates protective roles and contributes to I/R-associated vascular injury. It has been demonstrated that tyrosine nitration inactivates PI3K/Akt pathway.36, 37 Previous study has shown that p85 regulatory subunit of PI3K is a target for ONOO−-induced tyrosine nitration.38 In this study, we observed significant decreases in PI3K phosphorylation and Akt phosphorylation, indicating an inhibitory effect of the protein nitration. It has been convincingly reported that PI3K and Akt are important upstream regulators of eNOS activation.27, 28, 39, 40, 41, 42 eNOS-derived NO has been known to have a pivotal role in the modulation of vascular tone and function.6, 7 Taken together, our results allow us to propose that, ROS/RNS excess in peripheral resistance vessels during I/R injury may blunt PI3K/Akt/eNOS pathway, thus triggering endothelial dysfunction. A schematic representation of the proposed mechanism is shown in Figure 10.
Proposed schematic illustration of the mechanism by which ischemic preconditioning (IPC) exerts its endothelial protective effects against ischemia/reperfusion (I/R) injury in this study. IPC attenuates protein tyrosine nitration mediated by peroxynitrite through abrogating reactive oxygen species formation, thereby activating PI3K/Akt/eNOS pathway that in turn contributes to endothelial protection. cGMP, cyclic guanosine monophosphate; eNOS, endothelial nitric oxide synthase; GTP, guanosine triphosphate; NO, nitric oxide; O2−, superoxide anion; sGC, soluble guanylate cyclase.
The involvement of the endothelium in the pathogenesis of I/R injury has led to the investigation of strategies to prevent endothelial dysfunction. This study demonstrated that delayed preconditioning prevented I/R-induced endothelial dysfunction in peripheral resistance vasculature, and was consistent with previous data in the coronary arteries.43 The mechanisms by which delayed preconditioning confers vascular endothelial protection are not completely characterized. Several lines of evidence have shown that the late effect of IPC is mainly attributable to increased NO production during I/R.16, 43 In our experiment, after delayed IPC treatment, we observed a restoration of NO availability, as documented by the full inhibition by L-NAME on ACh-induced relaxation. The upregulation of eNOS expression and phosphorylation suggests that eNOS had a role. Our data appear to contrast with the reports documenting the absence of an NO protective role in delayed IPC-induced cytoprotective effect in endothelial cells.17 Several factors may contribute to these discrepancies. First, our experimental setting was different from that used by these authors, because we used in vivo experimental model that is a more complex biological system, whereas they used cell culture. Moreover, these authors exclusively explored the mechanism involved in cell survival, whereas we focused on vascular endothelial function. It should be noted that NO is the primary regulator of vascular function, because it induces vasodilatation, inhibits platelet adhesion and aggregation, and reduces leukocyte–endothelial cell interaction.5, 6, 7 This could explain the critical role of NO in IPC-induced endothelial protection.
IPC was reported to reduce the generation of ROS/RNS after myocardial I/R.14, 15 In this study, after IPC treatment, ACh-evoked relaxation was no longer sensitive to ROS scavenging. In conjunction with our functional data, the DHE analysis documented that the enhanced generation of vascular superoxide anion in the I/R rats was dramatically reduced by delayed IPC. In line with these results, the increases in serum MDA content and vascular levels of nitrotyrosine expression were abrogated by delayed IPC. As protein tyrosine nitration is known to affect protein function, recovery of PI3K and Akt phosphorylation in our results may be related to suppression of protein tyrosine nitration. Based on data from our current study and others, it is plausible to speculate that, beyond the restoration of NO availability, the abrogation of vascular ROS overproduction is a mechanism whereby delayed IPC was able to activate PI3K/Akt/eNOS pathway. However, we do not exclude the potential salutary role of low levels of ROS as triggers of delayed IPC.16, 44 Therefore, the normalized endothelium-dependent relaxation after IPC treatment likely results from an abrogation of ROS generation, which in turn accounts for the decreased protein nitration and thus activation of PI3K/Akt/eNOS pathway (Figure 10).
However, it should be noted that our data does not prove a direct causal relationship between increased PI3K/Akt phosphorylation and IPC-induced endothelial protection. The use of specific PI3K or Akt inhibitors would help to clarify the role of this pathway in protection in this setting. Nevertheless, the results from this study are promising and provide clear clues for future in depth study. Further studies of detailed mechanism by which delayed IPC induces suppression of pathological ROS formation and how this process correlates with other pathways of protection are warranted.
In summary, our present experiments provide the first evidence that delayed IPC is able to abrogate I/R-induced endothelial dysfunction in peripheral resistance vessels, in part, presumably by preventing ROS production and upregulating eNOS. Delayed preconditioning represents an attractive strategy for enhancing vascular endothelial protection in the setting of reperfusion injury. The present findings provide novel insights in this field in terms of understanding of the mechanism of delayed IPC. This knowledge may help us to apply remote IPC (elicited by ischemia of easily accessible tissues) to protect remote vital organs undergoing I/R in the clinical settings. The results of this study may contribute to the development of future therapeutic strategies and pharmacological manipulations aimed at exploiting this endogenous protective mechanism to prevent or alleviate I/R injury.
References
Ma H, Zhang HF, Yu L et al. Vasculoprotective effect of insulin in the ischemic/reperfused canine heart: role of Akt-stimulated NO production. Cardiovasc Res 2006;69:57–65.
Zhang C, Xu X, Potter BJ et al. TNF-alpha contributes to endothelial dysfunction in ischemia/reperfusion injury. Arterioscler Thromb Vasc Bio 2006;26:475–480.
Gao X, Xu X, Belmadani S et al. TNF-alpha contributes to endothelial dysfunction by upregulating arginase in ischemia/reperfusion injury. Arterioscler Thromb Vasc Bio 2007;27:1269–1275.
Ha SJ, Kim W, Woo JS et al. Preventive effects of exenatide on endothelial dysfunction induced by ischemia-reperfusion injury via KATP channels. Arterioscler Thromb Vasc Biol 2012;32:474–480.
Li H, Witte K, August M et al. Reversal of endothelial nitric oxide synthase uncoupling and up-regulation of endothelial nitric oxide synthase expression lowers blood pressure in hypertensive rats. J Am Coll Cardiol 2006;47:2536–2544.
Mulders AC, Mathy MJ, Meyer ZH et al. Activation of sphingosine kinase by muscarinic receptors enhances NO-mediated and attenuates EDHF-mediated vasorelaxation. Basic Res Cardiol 2009;104:50–59.
Zhang QJ, McMillin SL, Tanner JM et al. Endothelial nitric oxide synthase phosphorylation in treadmill-running mice: role of vascular signalling kinases. J Physiol 2009;587:3911–3920.
Feletou M, Vanhoutte PM . Endothelial dysfunction: a multifaceted disorder (The Wiggers Award Lecture). Am J Physiol Heart Circ Physiol 2006;291:H985–H1002.
Xuan YT, Guo Y, Zhu Y et al. Endothelial nitric oxide synthase plays an obligatory role in the late phase of ischemic preconditioning by activating the protein kinase C epsilon p44/42 mitogen-activated protein kinase pSer-signal transducers and activators of transcription1/3 pathway. Circulation 2007;116:535–544.
Talukder MA, Yang F, Shimokawa H et al. eNOS is required for acute in vivo ischemic preconditioning of the heart: effects of ischemic duration and sex. Am J Physiol Heart Circ Physiol 2010;299:H437–H445.
Hausenloy DJ, Yellon DM . The second window of preconditioning (SWOP) where are we now? Cardiovasc Drugs Ther 2010;24:235–254.
Kimura M, Ueda K, Goto C et al. Repetition of ischemic preconditioning augments endothelium-dependent vasodilation in humans: role of endothelium-derived nitric oxide and endothelial progenitor cells. Arterioscler Thromb Vasc Bio 2007;27:1403–1410.
Yin C, Salloum FN, Kukreja RC . A novel role of microRNA in late preconditioning: upregulation of endothelial nitric oxide synthase and heat shock protein 70. Circ Res 2009;104:572–575.
Zhu X, Liu B, Zhou S et al. Ischemic preconditioning prevents in vivo hyperoxygenation in postischemic myocardium with preservation of mitochondrial oxygen consumption. Am J Physiol Heart Circ Physiol 2007;293:H1442–H1450.
Csonka C, Csont T, Onody A et al. Preconditioning decreases ischemia/reperfusion-induced peroxynitrite formation. Biochem Biophys Res Commun 2001;285:1217–1219.
Laude K, Beauchamp P, Thuillez C et al. Endothelial protective effects of preconditioning. Cardiovasc Res 2002;55:466–473.
Bellis A, Castaldo D, Trimarco V et al. Cross-talk between PKA and Akt protects endothelial cells from apoptosis in the late ischemic preconditioning. Arterioscler Thromb Vasc Biol 2009;29:1207–1212.
Vila E, Salaices M . Cytokines and vascular reactivity in resistance arteries. Am J Physiol Heart Circ Physiol 2005;288:H1016–H1021.
He X, Zhang HL, Zhao M et al. Amlodipine ameliorates endothelial dysfunction in mesenteric arteries from spontaneously hypertensive rats. Clin Exp Pharmacol Physiol 2011;38:255–261.
Zhao M, He X, Wier WG et al. Endothelial dysfunction in rat mesenteric artery after regional cardiac ischaemia-reperfusion. Exp Physiol 2012;97:70–79.
Wang SP, Zang WJ, Kong SS et al. Vasorelaxant effect of isopropyl 3-(3, 4-dihydroxyphenyl)-2-hydroxypropanoate, a novel metabolite from Salvia miltiorrhiza, on isolated rat mesenteric artery. Eur J Pharmacol 2008;579:283–288.
Luo HL, Zang WJ, Lu J et al. The protective effect of captopril on nicotine-induced endothelial dysfunction in rat. Basic Clin Pharmacol Toxicol 2006;99:237–245.
Wang Y, Wang S, Wier WG et al. Exercise improves the dilatation function of mesenteric arteries in postmyocardial infarction rats via a PI3K/Akt/eNOS pathway-mediated mechanism. Am J Physiol Heart Circ Physiol 2010;299:H2097–H2106.
Sun L, Li DL, Zhao M et al. The role of muscarinic receptors in the beneficial effects of adenosine against myocardial reperfusion injury in rats. PLoS One 2011;6:e25618.
Zhao M, He X, Zhao M et al. Low-dose celecoxib improves coronary function after acute myocardial ischaemia in rabbits. Clin Exp Pharmacol Physiol 2012;39:233–240.
Somers MJ, Mavromatis K, Galis ZS et al. Vascular superoxide production and vasomotor function in hypertension induced by deoxycorticosterone acetate-salt. Circulation 2000;101:1722–1728.
Fulton D, Gratton JP, McCabe TJ et al. Regulation of endothelium derived nitric oxide production by the protein kinase Akt. Nature 1999;399:597–560.
Jiménez R, Sánchez M, Zarzuelo MJ et al. Endothelium-dependent vasodilator effects of peroxisome proliferator-activated receptor beta agonists via the phosphatidyl-inositol-3 kinase-Akt pathway. J Pharmacol Exp Ther 2010;332:554–561.
Radi R . Nitric oxide, oxidants, and protein tyrosine nitration. Proc Natl Acad Sci USA 2004;101:4003–4008.
Murphy E, Steenbergen C . Mechanisms underlying acute protection from cardiac ischemia-reperfusion injury. Physiol Rev 2008;88:581–609.
Cai H, Griendling KK, Harrison DG . The vascular NAD(P)H oxidases as therapeutic targets in cardiovascular diseases. Trends Pharmacol Sci 2003;24:471–478.
Szocs K . Endothelial dysfunction and reactive oxygen species production in ischemia/reperfusion and nitrate tolerance. Gen Physiol Biophys 2004;23:265–295.
Brandes RP, Weissmann N, Schröder K . NADPH oxidases in cardiovascular disease. Free Radic Biol Med 2010;49:687–706.
Starr ME, Ueda J, Yamamoto S et al. The effects of aging on pulmonary oxidative damage, protein nitration, and extracellular superoxide dismutase down-regulation during systemic inflammation. Free Radic Biol Med 2011;50:371–380.
Liu B, Tewari AK, Zhang L et al. Proteomic analysis of protein tyrosine nitration after ischemia reperfusion injury: mitochondria as the major target. Biochim Biophys Acta 2009;1794:476–485.
Pacher P, Beckman JS, Liaudet L . Nitric oxide and peroxynitrite in health and disease. Physiol Rev 2007;87:315–424.
el-Remessy AB, Bartoli M, Platt DH et al. Oxidative stress inactivates VEGF survival signaling in retinal endothelial cells via PI 3-kinase tyrosine nitration. J Cell Sci 2005;118:243–252.
Hellberg CB, Boggs SE, Lapetina EG . Phosphatidylinositol 3-kinase is a target for protein tyrosine nitration. Biochem Biophys Res Commun 1998;252:313–317.
Morello F, Perino A, Hirsch E . Phosphoinositide 3-kinase signalling in the vascular system. Cardiovasc Res 2009;82:261–271.
Hashiguchi A, Yano S, Morioka M et al. Up-regulation of endothelial nitric oxide synthase via phosphatidylinositol 3-kinase pathway contributes to ischemic tolerance in the CA1 subfield of gerbil hippocampus. J Cereb Blood Flow Metab 2004;24:271–279.
Fernández-Hernando C, Ackah E, Yu J et al. Loss of Akt1 leads to severe atherosclerosis and occlusive coronary artery disease. Cell Metab 2007;6:446–457.
Romano MR, Lograno MD . Epigallocatechin-3-gallate relaxes the isolated bovine ophthalmic artery: involvement of phosphoinositide 3-kinase-Akt nitric oxide/cGMP signalling pathway. Eur J Pharmacol 2009;608:48–53.
Laude K, Favre J, Thuillez C et al. NO produced by endothelial NO synthase is a mediator of delayed preconditioning-induced endothelial protection. Am J Physiol Heart Circ Physiol 2003;284:H2053–H2060.
Takano H, Tang XL, Qiu Y et al. Nitric oxide donors induce late preconditioning against myocardial stunning and infarction in conscious rabbits via an antioxidant-sensitive mechanism. Circ Res 1998;83:73–84.
Acknowledgements
This work is supported by the Major International (Regional) Joint Research Project of National Natural Science Foundation of China (No. 81120108002), National Natural Science Foundation of China (No. 30930105; No. 30873058), CMB Distinguished Professorships Award (No. F510000/G16916404) and Natural Science Foundation of Shaanxi Province (No. 2012JZ4001). We are grateful to Professor Withrow Gil Wier from the University of Maryland for discussion of the paper. We also appreciate the technical support and materials from the electron microscope center of Xi’an Jiaotong University.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
This paper describes the mechanism that mediates delayed preconditioninginduced endothelial protection against ischemia/reperfusion injury in peripheral arteries. Protection is associated with inhibition of oxidative stress and activation of the PI3K/Akt/eNOS pathway. Thus, remote ischemic preconditioning, elicited by ischemia of easily accessible tissues, may protect remote vital organs undergoing ischemia/reperfusion.
Rights and permissions
About this article
Cite this article
He, X., Zhao, M., Bi, XY. et al. Delayed preconditioning prevents ischemia/reperfusion-induced endothelial injury in rats: role of ROS and eNOS. Lab Invest 93, 168–180 (2013). https://doi.org/10.1038/labinvest.2012.160
Received:
Revised:
Accepted:
Published:
Issue date:
DOI: https://doi.org/10.1038/labinvest.2012.160
Keywords
This article is cited by
-
Choline ameliorates cardiovascular damage by improving vagal activity and inhibiting the inflammatory response in spontaneously hypertensive rats
Scientific Reports (2017)
-
H2S Prevents Cyclosporine A-Induced Vasomotor Alteration in Rats
Cardiovascular Toxicology (2017)
-
High oxygen modifies vasodilator effect of cysteine via enhanced oxidative stress and thromboxane production in the rat mesenteric artery
Pflügers Archiv - European Journal of Physiology (2016)
-
A Review on the Mechanisms of Blood-Flow Restriction Resistance Training-Induced Muscle Hypertrophy
Sports Medicine (2015)
-
Protective effects of Phyllanthus emblica against myocardial ischemia-reperfusion injury: the role of PI3-kinase/glycogen synthase kinase 3β/β-catenin pathway
Journal of Physiology and Biochemistry (2015)