Abstract
Background
Weight stigma causes significant physical and psychological harm to its targets.
Objective
This review aims to determine when identifying as a member of the higher-weight group exacerbates versus mitigates the adverse effects of weight stigma.
Methods
Searches were conducted on 10 January, 2025, using PsycInfo, Medline, Scopus, Web of Science, Embase, and CINAHL. Evidence was synthesised in terms of exacerbating versus protective effects of higher-weight social identity (as moderator/mediator) in the relationship between weight stigma and 18 distinct health outcomes. This review is registered on PROSPERO (ID: CRD42023415639).
Results
Fourteen studies met the inclusion criteria. Studies employing weight status measures to assess higher-weight social identity identified actual and self-perceived higher-weight as risk factors for anticipated rejection, dietary control challenges, increased physiological stress and greater functional disability following stigmatisation. Conversely, studies measuring individual connection with the higher-weight group revealed that stronger identification had protective effects on self-esteem and distress, but only for specific individuals (e.g., those with low internalised weight bias).
Limitations
Grey literature and unpublished studies were not reviewed.
Conclusions
Initial evidence suggests that higher-weight social identity functions as both risk and protective factor in the relationship between weight stigma and well-being.
Implications
Future research should explore the emotional and evaluative components of higher-weight social identity to enhance understanding of how and when group membership influences the adverse effects of weight stigma. This knowledge can inform targeted interventions designed to improve the well-being of higher-weight individuals.
Similar content being viewed by others
People with obesity are frequent targets of weight stigma (i.e., social devaluation due to body weight)Footnote 1 across various settings including education, employment, health care, the media, and within the family home [1]. Weight stigma is manifested through negative stereotypes (e.g., lazy, incompetent, ill-disciplined) which may result in prejudice (e.g., negative attitudes) and discrimination toward the target [2]. The psychological and physical consequences of weight stigma include depression, anxiety, low self-esteem, and weight gain [3]. Interventions targeted at reducing bias against higher-weight people have had limited success to date [4]. Research has, therefore, shifted toward understanding psychosocial factors that can mitigate the negative impact of weight stigma on the targets. Two lines of research—weight-based social identity threat (WBSIT) [5], and the social cure [6, 7]—have emerged that identify weight-based social identity as a major factor in the relationship between stigma and well-being. As depicted in Fig. 1, the WBSIT model views higher-weight social identity—the part of the self-concept that comes from identifying as a member of the higher-weight social group (i.e., the ingroup) [8]—as a risk factor, while the social cure framework suggests it can be protective under specific circumstances.
Note. WBSIT model denoted by dotted pathways: Higher-weight social identity is hypothesised to moderate the relationship between weight stigma and health outcomes (link A). Specifically, higher-weight social identity is predicted to exacerbate the negative effects of weight stigma on health. Higher-weight social identity is expected to mediate the relationship between weight stigma (links B and Ca, where higher-weight social identity is negatively related to well-being). Social Cure model denoted by solid pathways: Higher-weight social identity as a detrimental mediator of the relationship between weight stigma and health outcomes (links B and Cb−) or as a protective factor (links B and Cb+), depending on certain circumstances (e.g., the perceived illegitimacy of stigma) and individual factors (e.g., low levels of internalised weight bias; see link D).
Identifying what constitutes risk versus protective factors is crucial as such knowledge can help inform interventions and policies aimed at reducing the adverse impacts of weight stigma on its targets and is, therefore, the general aim of this review.
Weight-based social identity threat model, weight stigma, and health outcomes
The WBSIT model examines the adverse effects of a higher-weight social identity. As depicted by link A in Fig. 1, this model proposes that when individuals categorise themselves as higher-weight or believe others regard them as member of this social category, weight stigma increases the vulnerability to experiencing weight-based social identity threat due to fear of the association of weight stigma with the ingroup [8]. This in turn activates stress processes that can be associated with self-control resources required for regulating healthy behaviours [9]. These effects, when experienced persistently, further undermine mental and physical health and, ironically, contribute to weight gain and increase the likelihood of ongoing stigmatisation [5]. Research applying this model has also examined whether the negative impact of weight stigma on well-being is mediated by higher-weight social identification (see links B and Ca, Fig. 1) [10].
Numerous studies support the WBSIT model. For instance, research assessing higher-weight social identity using objective weight measures like body mass index (BMI; i.e., assigned group membership), demonstrates that individuals with higher body weight experience more adverse psychological (e.g., stress emotions) [11] and physical (e.g., greater cortisol reactivity) [12] outcomes following exposure to weight stigmatisation, compared to those with lower body-weight. Other researchers suggest that self-categorisation (i.e., psychological group membership) as higher-weight is a necessary condition to elicit WBSIT and, consequently, have operationalised higher-weight social identity by measuring individuals’ self-perceived weight status in addition to BMI. For instance, Hunger et al. found that among higher-weight women and those who perceived themselves as higher-weight, exposure to weight stigma led to significantly greater anticipation of being socially rejected because of their weight compared to their average-weight counterparts [13].
Although the WBSIT perspective provides useful insights into the mechanisms connecting weight stigma and adverse health outcomes among higher-weight individuals, this approach is limited by its conceptualisation of higher-weight social identity as an individual’s mere awareness of belonging to the higher-weight group. Evidence suggests that the emotional and evaluative significance of group membership to an individual is also likely to have important implications for health outcomes [14]. This evidence is consistent with influential definitions of social identity, which includes both knowing one belongs to a group and feeling attached to it through emotions and/or values [15].
In addition to these methodological and conceptual issues, WBSIT research may also be limited by the assumption that higher-weight individuals universally internalise weight stigma [16, 17] and do not display ingroup favouritism (see Crandall [18]), a well-documented tendency among ingroup members [19]. However, recent studies show that many individuals actively resist weight stigma (e.g., “Big is Beautiful” reframing strategies), and that ingroup identification is an important predictor of this resistance [20]. To address these limitations, some researchers have turned to the social cure approach to examine weight stigma and health outcomes.
The social cure approach, weight stigma, and health outcomes
Informed by social identity theory [21], and self-categorisation theory [22], the social cure approach [6, 7] proposes that although some social identities (particularly low status social identities) may be a potential source of distress (i.e., a social curse—see Cruwys and Gunaseelan [23], Kyprianides et al. [24]), they may also act as a buffer against adverse consequences of stigma (i.e., a social cure; see links B and Cb, Fig. 1). In contrast to the WBSIT model, which limits its focus on group membership awareness, this approach considers the broader definition of social identity (see Postmes et al. [14]) that includes an individual’s evaluative and emotional connection to the ingroup (which may vary in strength and be positive/negative/neutral). Drawing from the rejection-identification model (RIM) [25], the social cure approach proposes that stigmatised individuals, who perceive group boundaries as impermeable and discrimination toward the ingroup as unfair, are likely to respond to stigma by identifying with ingroup members to reduce feelings of rejection, which in turn, protects well-being by increasing perceived social support [26]. Members may also pursue collective social strategies that provide an additional basis for social support and promote hope and optimism [27].
In the context of weight, the pervasive discrimination and perceived impermeability of group boundaries, due to the challenge of achieving long-term weight loss [28], are likely to move stigmatised higher-weight people closer to their ingroup [20]. In this vein, the RIM asserts that higher-weight social identification plays a mediating role in the relationship between weight stigma and well-being with a positive effect on well-being (see links B and Cb+, Fig. 1). However, the highly negative content of weight stigma is commonly endorsed by group members [28]. For those members, the social cure approach predicts that ingroup identification may lead to a social curse rather than to a social cure (see links B and Cb−, Fig. 1).
Given these complexities, and the current lack of research examining protective factors [2], researchers have recently sought to clarify when and for whom identification with the higher-weight group is likely to buffer against the harmful effects of weight stigma (e.g., Curll and Brown [29]; Magallares et al. [30]). Internalised weight bias (IWB), which is strongly associated with negative mental health outcomes [31] and research shows, for example, that individuals with high IWB are more likely to legitimise weight stigma [32]. Curll and Brown [29] tested the role of IWB within the social cure model and predicted that the social cure effect would depend on individual differences in IWB. They operationalised higher-weight social identification as the degree to which being higher-weight was central to a participant’s identity (identity centrality). Results indicated that stronger higher-weight social identification was associated with lower psychological distress (i.e., improved well-being; see links B and D, Fig. 1), but only among individuals with low IWB. This study is important as it provides a more nuanced understanding of the factors influencing the relationship between weight stigma and the mental and physical health of higher-weight individuals by considering both group (i.e., social identity) and individual-level (i.e., IWB) factors.
Rationale and objectives
Thus far, interventions on weight stigma have mostly focused on reducing stigmatisation (i.e., focus on the stigmatisers), and have generally been unsuccessful [4]. Because weight stigma produces highly detrimental health effects on targets, it is important to investigate risk and resilience factors that may exacerbate or prevent/reduce the harmful impact of stigma. To date, no synthesis of this literature exists.
Taken together, the literature reviewed above suggests that social identity can be both a cure and curse depending on context, and that individual factors can play a role in determining the outcome (e.g., IWB). Therefore, this review will not test the validity of the WBSIT or the social cure models. Instead, it aims to test the two models together and review studies that have explored how higher-weight social identity moderates and/or mediates the relationship between weight stigma and psychological and physical well-being (i.e., WBSIT model). In addition, it also aims to investigate whether the mediating effect of higher-weight social identity is moderated by individual factors (such as perceived il/legitimacy of stigma, or IWB; i.e., the social cure model). The ultimate goal is to understand whether and when higher-weight social identity exacerbates versus reduce weight stigma harm. As such, this review will provide a synthesis of the state-of-the art in this field, contribute with suggestions for future research, and offer evidence-based recommendations for targeted interventions and policies aimed at improving health outcomes for higher-weight individuals.
Methods
The preferred reporting items for systematic review and meta-analyses (PRISMA) statement [33] were followed for this review. Methods were established prior to data extraction and pre-registered in PROSPERO (ID: CRD42023415639).
Search strategy
Systematic searches were performed on January 10, 2025, using PsycINFO, CINAHL, Web of Science Core Collection, Medline Complete, Scopus, and Embase databases with no date limitations on studies. Search results were imported into Covidence via Endnote for screening. A combination of search terms using Boolean phrasing (see Table 1 in Supplementary Materials) were used to identify papers relevant to weight stigma, social identity, and health outcomes. Additional studies were identified via a search of reference lists of included papers.
Eligibility criteria
To be eligible, studies had to be peered reviewed and meet the following criteria: there had to be (1) a measure of experienced or perceived weight stigma as an independent variable, (2) a measure of higher-weight social identity/identification (as a mediator or a moderator variable), and (3) a physical or psychological health outcome measure. Studies were excluded if they: (1) were reports, reviews, book chapters, abstracts, dissertations, were not peer reviewed, or provided insufficient data, (2) were unpublished studies, (3) included the wrong independent variable, mediator or moderator, or outcome measure, and (4) were not written in English, due to interpretation limitations.
Screening and data extraction
Studies were independently screened by two reviewers (AH and LB) at both the title and abstract, and full-text screening stages using Covidence. Any disagreements were resolved through discussion. The data from eligible studies were extracted by AH and included (if reported): author name(s), country, year of publication, sample characteristics (sample size, source, percentage of females), age, BMI (mean and standard deviation), study design (i.e., cross-sectional, longitudinal, or experimental), and measure(s) of the independent variable, the mediator/moderator, and the physical and/or mental health outcome variables. Inferential statistics and standardised effects sizes were extracted for all statistical analyses. Guidelines published by Cohen [34] were used for assessing effect sizes.
Risk of bias assessment
A risk of bias assessment was conducted by AH and LB using the Centre for Evidence-Based Management (CEBMa) checklist for surveys, irrespective of study design. This approach was adopted in a recent systematic review for weight stigma effects (see Hill et al. [35]) to allow comparison across studies with a single tool (all eleven criteria are displayed in Table 2 in Supplementary Materials). Each criterion was assessed as “yes,” “no,” or “can’t tell.” Overall quality rating (i.e., good, fair, or poor) was assessed independently by AH and LB based on the critical appraisal of the risk of potential for selection, information bias, measurement, or confounding. Any conflicts were discussed and resolved between AH and LB.
Results
Study search
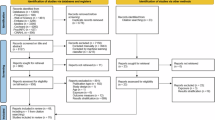
Following a search of six databases, the studies were entered into Covidence, which identified duplicates and automatically removed them before they were screened by title and abstract. Of the initial 1855 studies 57 remained to be screened against the full-text eligibility criteria, which resulted in 14 studies left for inclusion in the review (see Fig. 1 in Supplementary Materials and Appendix A in Supplementary Materials).
Higher-weight social identity as a risk factor
Study characteristics
Table 1 shows a summary of the characteristics for each of the 10 included studies examining higher-weight social identity as a risk factor (N = 5955). That is, studies that evaluated link A, as well as links B and Ca in Fig. 1. All studies were published between 2011 and 2025, with nine studies conducted in the United States of America, and one in China. Four studies recruited only women. Study designs were mixed, with seven using between-subjects, two using cross-sectional single sample (correlational), and one using a longitudinal design.
Weight stigma measures
Most studies (n = 7) utilised different weight stigma manipulation paradigms to experimentally induce weight stigma (see Table 3 in Supplementary Materials) and examine its impact on individuals’ well-being. One study used an author-created questionnaire to measure perceived weight stigma, one used the original version of the Perception of Teasing Scale [36], and one used a 2-item composite validated measure of daily anticipated and experienced weight stigma [37].
Higher-weight social identity measures
Four studies measured BMI as an indicator of higher-weight social identity, and three measured self-perceived weight. Only three studies measured both assigned and psychological membership (i.e., BMI and self-perceived weight, respectively).
Outcome measures
Twelve different psychological outcomes and two physical outcomes were examined. The most common psychological outcome was executive functioning (n = 3). Each of the following were examined in two studies: self-regulation, rejection expectations, self-conscious emotions, state self-esteem, stress emotions, and disordered eating. Each of the following were examined in one study only: self-efficacy for dietary control, weight stigma concerns, anxiety, post-interaction rumination, and alcohol use. Cortisol reactivity was examined in two studies and functional disability (i.e., change in mobility over a 10-year period) in one.
Synthesis of results
As displayed in Tables 2–4, there were 31 unique findings resulting from the nine studies that examined higher-weight social identity as a moderator (i.e., tested link A in Fig. 1). One study (see Table 5) examined the mediating role of higher-weight social identity (i.e., tested links B and Ca in Fig. 1). All moderating/mediating effects were in line with the studies’ hypothesised direction, with two exceptions in Lee et al.’s [37] study (see below), and 50% were statistically significant.
Psychological outcomes
Outcomes related to consumption behaviours
As shown in Table 2, outcomes relating to calorie consumption behaviours were the most affected by weight stigma and higher-weight social identity. Specifically, compared to a control group, following exposure to weight stigma, only participants who were higher-weight, or perceived they were, consumed more calories and felt less capable of dietary control. Interestingly, weight stigma was associated with greater restrictive eating among lower compared to higher-weight individuals [38], and Lee et al. [37] found that the positive relationships between weight stigma and (1) disordered eating and (2) alcohol use were weaker when identification was stronger.
Other psychological outcomes
Table 3 shows results for other psychological outcomes. Two out of three findings from studies that assessed rejection expectations indicated that higher-weight social identity exacerbated the negative impact of weight stigma. Results were mixed for stress emotions and executive functioning. Higher-weight social identity did not significantly moderate the relationships between weight stigma and self-conscious emotions, state self-esteem, weight stigma concerns, post-interaction rumination, and anxiety.
Physical outcomes
As shown in Tables 4 and 5, there were four unique findings across all studies for physical outcomes. Across the two studies that examined cortisol reactivity, higher-weight social identity was found to significantly increase the harmful effects of weight stigma on this outcome (see Table 4). Lastly, Schafer and Ferraro [10] found that perceived weight discrimination was positively associated with self-perceived higher-weight, which significantly mediated the harmful effect of perceived weight stigma on functional disability (see Table 5).
Higher-weight social identity as a protective factor
Study characteristics
Table 6 summarises the characteristics for each of the four studies that examined higher-weight social identity as a protective factor (N = 3017). That is, studies that tested links B, Cb, and D in Fig. 1. One study was conducted in Spain, one in Australia, and two in the USA. All studies used a cross- sectional, correlational design.
Weight stigma measures
The studies used different measures of weight stigma. One used the Everyday Discrimination Scale [39], one used the Obesity Related Problems Scale [40], and two used the Perceived Discrimination Scale [41].
Higher-weight social identity measures
Different measures were also used to assess higher-weight social identification. These included the centrality subscale of the 5-factor Group Identification Scale [42], the centrality subscale of the Group Identification Scale [43], and the Fat-Group Identification Scale [41].
Outcome measures
Across the four studies, self-esteem, satisfaction with life, stress, psychological distress, disordered eating, and general health were assessed as outcomes.
Synthesis of results
As shown in Table 7, there were seven unique findings across the four studies. Four findings were in line with the authors’ predictions [29, 30, 44] and two were in the opposite direction (see below; Wellman et al. [45]). Six of the seven findings were statistically significant. These inconsistencies in results highlight the complexity of the relationship between higher-weight social identification and well-being among higher-weight individuals.
Psychological outcomes
There were six unique findings across all studies for psychological outcomes. As shown in Table 7, findings were mixed for self-esteem. Results from Magallares et al.’s [30] path analysis provided support for the RIM model, revealing a negative link between weight stigma and self-esteem but a positive link between higher-weight group identification and this outcome (see links B and Cb in Fig. 1). In contrast, Wellman et al. [45] found that weight stigma was associated with lower self-esteem, and higher-weight social identification significantly mediated this relationship. Similarly, Araiza et al. [44] demonstrated that weight stigma was positively associated with higher-weight social identification, which in turn, was linked to increased stress and disordered eating (see links B and Cb in Fig. 1). Curll and Brown [29] found a significant, positive indirect effect of weight stigma on psychological distress through higher-weight social identification. However, this indirect effect was found to be moderated by IWB. That is, for participants with low IWB, higher-weight social identification was associated with lower distress; but the opposite was found for those with higher IWB (supporting links B and D in Fig. 1).
Physical outcomes
As shown in Table 7, higher weight stigma was negatively related to general health and the indirect pathway from weight stigma to general health through group identification was also negative and significant (see links B and Cb in Fig. 1).
Risk of bias assessment
A risk of bias assessment was performed by AH and LB using the CEBMa checklist. All studies were given an overall quality rating of good, with the exception of one (i.e., Wang et al. [46]; see Table 3 in Supplementary Materials), based on the critical appraisal of the risk of potential for selection bias, information bias, measurement or confounding bias. As such, the pattern of findings in this review were not biased by the methodological rigour of the included studies.
Discussion
This review explored the role of higher-weight social identity as both a risk and protective factor in the effects of weight stigma on physical and psychological well-being. Given the difficulty of combating weight stigma at the societal level [4], understanding these factors is crucial for developing targeted interventions that effectively reduce the harmful effects of weight stigma for higher-weight individuals. This review synthesised 13 studies. Across the 13 studies, seven different measures of weight stigma were used, higher-weight social identity was operationalised in five different ways, and 18 outcome variables were assessed. Thus, the research question was not suitable for a meta-analysis. Ten studies were informed by the WBSIT model and three by the social cure perspective. A general conclusion that can be drawn is that the studies support both the WBSIT and the social cure models, but results were contingent on the outcomes measured and the inclusion of moderators when evaluating the link between higher- weight social identity and well-being.
Higher-weight social identity as a risk factor
Psychological outcomes
Studies informed by WBSIT theory showed mixed results. Major et al. [11] found that higher-weight women experienced greater stress emotions after weight stigmatisation, unlike their lower-weight counterparts. However, another study [47] found no significant impact of higher-weight social identity on this relationship. Moreover, higher-weight social identity, when accompanied by weight stigma, did not exacerbate the negative emotions experienced, such as reduced self-esteem, increased anxiety, post-interaction rumination, and self-consciousness. Similarly, this social identity did not consistently exacerbate the negative impact of weight stigma on executive functioning, as observed by Blodorn et al. [47] and Hunger et al. [13].
Interestingly, two of three findings indicated that higher-weight social identity played an exacerbating role in the link between weight stigma and expectations of weight-based social rejection, while only one finding showed no impact on this outcome. Anticipated rejection has been identified as a mediator between weight stigma and psychological stress, negative emotions and reduced executive performance [13, 47]. Thus, interventions targeting rejection expectations could be implemented to prevent significant downstream psychological issues for higher-weight individuals. For instance, therapies addressing anxiety symptoms may incorporate cognitive bias modification training to address weight-based rejection expectations [48].
Furthermore, in three studies, all findings demonstrated that higher-weight social identity, combined with weight stigma, detrimentally affects outcomes related to consumption behaviours, such as individuals’ belief in their ability to control their diet and their actual tendency to do so. Notably, higher-weight women consumed more high-calorie snacks after weight stigma exposure compared to average-weight individuals [49, 50]. Since self-efficacy is crucial for long-term behavioural self-regulation among higher-weight individuals [51], interventions should prioritise promoting dietary self-efficacy. However, one study found that weight stigma’s negative consequences on alcohol use and disordered eating were worse for lower-weight individuals [37]. Given the prominence of behavioural responses to weight stigmatisation among higher-weight individuals in the WBSIT model, further research assessing these outcomes is necessary, as this study alone is insufficient.
Physical outcomes
The current review revealed that all findings from the three studies that assessed physical outcomes indicated that stigma and WBSIT can get “under the skin” to undermine a person’s physical health and their ability to fully participate in life [52]. Specifically, higher-weight social identity was found to significantly increase the harmful effects of weight stigma on physiological stress and partly explained weight stigma’s impact on functional disability among individuals identifying as higher-weight. However, as research is limited, further research in this area is needed.
Higher-weight social identity as a protective factor
Psychological outcomes
Studies informed by the social cure also showed mixed results. One study found that identification protected against the negative impact of weight stigma on self-esteem [30]. In contrast, Wellman et al. [45] reported that higher-weight social identity exacerbated the harmful impact of stigma on self-esteem, and Araiza et al. [44] similarly identified detrimental effects, linking higher-weight social identity to increased stress and unhealthy eating behaviours. Methodological differences may explain these discrepancies. Wellman et al. and Araiza et al. both used large community samples (n = 739 and n = 1257, respectively), whereas Magallares et al. [30] included 95 participants exclusively from higher-weight associations, possibly influencing their tendency to positively identify with the higher-weight group. Wellman et al. found no evidence that higher-weight social identity exacerbates the negative relationship between weight stigma and life satisfaction. However, this is one study and further research is required.
Importantly, Curll and Brown [29] found that higher perceived weight stigma was associated with stronger identification that, in turn, was associated with higher psychological distress. However, in line with their predictions, this indirect relationship was moderated by IWB. Increased identification was shown to be an effective strategy for coping with the distress associated with stigma, but only when IWB was low. This study provides valuable insights into individual factors that determine when higher-weight social identification can buffer against the harmful effects of weight stigma. It also provides support for strategies (such as, participation in online size acceptance communities) and psychosocial interventions (including group-based treatments) that aim to harness the benefits of a higher-weight social identity.
Physical outcomes
One study unexpectedly found that higher-weight social identification exacerbated the harmful effects of weight stigma on general health. However, given the limited research in this area, further studies should examine the influence of individual factors, such as levels of IWB, on these relationships.
Limitations of the studies
Most studies in this review that were guided by the WBSIT model assessed higher-weight social identity using either psychological group membership (i.e., self-perceived weight; n = 3), or sociological/assigned group membership (i.e., BMI; n = 4). Although both forms of identity are important to assess, they are conceptually and operationally different. Whereas psychological group membership reflects self-perception, sociological group membership denotes an assigned membership that may or may not correspond to one’s identity. Psychological membership is more likely to impact outcomes [8] compared to an externally assigned identity that may or may not be internalised. Acknowledging these issues, three studies [13, 37, 53] used self-perceived weight alongside BMI to assess the impact of higher-weight social identity on the harmful effects of weight stigma, all of which found significant moderation effects for both BMI and self-perceived weight. However, it remains uncertain whether mere awareness of group membership is a true measure of social identity, since social identity theory also emphasises the evaluative and affective aspects of identity [19]. Thus, it raises questions about whether a more comprehensive measure of social identity would yield different results.
To comprehensively capture higher-weight social identity, it is necessary to assess both the extent to which group membership contributes to one’s self-concept and to the positive emotional valuation of that membership [14]. Although the former was assessed in the social cure studies through measures of identity centrality, individuals’ positive feelings towards and attachment to (e.g., embracing, rejecting or neutral) the ingroup were not assessed. To better understand the complexity of the higher-weight experience and how to minimise negative outcomes of stigma, research should employ a multidimensional operationalisation of social identity that incorporates affective components, such as satisfaction with and attachment to the ingroup, in addition to identity centrality (see Leach et al. [42]). By doing so, researchers can explore the psychosocial resources available to individuals and determine how they can either facilitate effective coping with stigma or potentially intensify its negative consequences. It is essential to explore the possibility that some individuals may embrace a higher-weight identity, which is likely to result in positive psychological outcomes [54].
Furthermore, the four studies that employed the social cure approach used a correlational design, which restricted the ability to draw causal conclusions. Although the social cure approach is theoretically strong, it is possible that psychological well-being might also influence social identification and weight stigma [29]. Moreover, perceived weight stigma was assessed by reference to participants’ past stigma experiences, and so may have been vulnerable to recall bias [29]. Future research should consider longitudinal methods, such as ecological momentary assessment [55], to measure stigma experiences in real-time, reducing the potential for recall bias.
Risk of bias
In this review, 13 out of the 14 included studies were of good quality. Therefore, results were not impacted by discrepancies in quality, suggesting there was no bias in the results. However, areas for improvement by researchers include reporting response rates (n = 5 studies achieved a satisfactory response rate), and confidence intervals for main results (n = 7). None of the studies reported conducting an a priori power analysis. If studies were underpowered this could explain non-significant findings present. Future studies should report adequate information for meaningful conclusions to be drawn.
Limitations of this review
This review has some limitations. Firstly, whilst revealing important directions for future research, the heterogeneity of findings makes it challenging to conduct meta-analysis and draw definitive conclusions about the role of higher-weight social identity as a risk or protective factor in the relationship between weight stigma and well-being. Secondly, consistent reporting of effect sizes was observed for only three out of the 18 outcomes assessed (i.e., for dietary self-efficacy, cortisol reactivity, and psychological distress), limiting a comprehensive overview of the magnitude of the impact of higher-weight social identity on health outcomes. Thirdly, the scope of this review was limited by the exclusion of unpublished or grey literature, potentially introducing publication bias and excluding relevant information. Future review should include such literature to address these limitations.
Conclusion
This review aimed to investigate the role of higher-weight social identity as a risk and a protective factor in the relationship between weight stigma and psychological and physical outcomes. Studies that examined higher-weight social identity as a risk factor showed that individuals aware of their higher-weight social categorisation were more likely to expect to be rejected due to their weight, perceive a lack of control over their diet, and engage in increased eating in response to stigma. However, research on other outcomes was limited and inconclusive and prevented more robust conclusions from being drawn. A major limitation of these studies was the lack of assessment of the evaluative and emotional components of higher-weight social identity, opening up new avenues for research. This review also highlighted the strengths of the social cure approach, which revealed that stronger identification with the higher-weight group could mitigate distress and improve self-esteem for certain individuals (e.g., those with low IWB). However, limited research informed by this approach and mixed results impeded definitive conclusions about the buffering role of social identification.
Overall, whilst the impact of a higher-weight social identity requires further investigation, this review suggests promising directions for future research. Researchers should use more comprehensive measures of higher-weight social identity and conduct experimental or longitudinal studies that measure actual weight stigma experiences to validate the predictive power of the social cure approach within the higher-weight group. Additionally, exploring individual factors that influence the social cure effect should be a continued focus of research. In the absence of much needed societal changes to eliminate weight stigma, such research is crucial for the development of effective strategies and psychosocial treatments that can foster a positive social identity and boost the well-being of individuals affected by weight stigma.
Methodological statement
In compliance with the established guidelines and regulations for conducting systematic reviews, we confirm that all methods utilised in this manuscript were rigorously performed in alignment with the PRISMA (Preferred Reporting Items for Systematic Reviews and Meta-Analyses) guidelines. This includes thorough literature searches, eligibility assessments, data extraction, and quality assessments, all of which adhered to the accepted standards in the field. We are committed to maintaining the integrity and transparency of our research, ensuring that our systematic review contributes meaningfully to the body of knowledge in this area.
Notes
Note that in this review, weight stigma refers to “public stigma”, including experienced, anticipated, and perceived stigma (see Emmer et al. [2]) and not to “private stigma” (i.e., internalised weight stigma or self-stigma).
References [References marked with an asterisk indicate studies included in the systematic review]
Ata RN, Thompson JK. Weight bias in the media: a review of recent research. Obes Facts. 2010;3:41–6.
Emmer C, Bosnjak M, Mata J. The association between weight stigma and mental health: a meta‐analysis. Obes Rev. 2020;21:e12935.
Schvey NA, Puhl RM, Brownell KD. The stress of stigma: exploring the effect of weight stigma on cortisol reactivity. Psychosom Med. 2014;76:156–62.
Lee M, Ata RN, Brannick MT. Malleability of weight-biased attitudes and beliefs: a meta-analysis of weight bias reduction interventions. Body Image. 2014;11:251–9.
Hunger JM, Major B, Blodorn A, Miller CT. Weighed down by stigma: how weight‐based social identity threat contributes to weight gain and poor health. Soc Personal Psychol Compass. 2015;9:255–68.
Jetten J, Haslam SA, Cruwys T, Greenaway KH, Haslam C, Steffens NK. Advancing the social identity approach to health and well‐being: progressing the social cure research agenda. Eur J Soc Psychol. 2017;47:789–802.
Haslam SA, Jetten J, Postmes T, Haslam C. Social identity, health and well-being: an emerging agenda for applied psychology. Appl Psychol. 2009;58:1–23.
Major B, O’Brien LT. The social psychology of stigma. Annu Rev Psychol. 2005;56:393–421.
Muraven M, Baumeister RF. Self-regulation and depletion of limited resources: does self-control resemble a muscle? Psychol Bull. 2000;126:247–59.
*Schafer MH, Ferraro KF. The stigma of obesity: Does perceived weight discrimination affect identity and physical health? Soc Psychol Q. 2011;74:76–97.
*Major B, Eliezer D, Rieck H. The psychological weight of weight stigma. Soc Psychol Personal Sci. 2012;3:651–8.
Himmelstein M, Tomiyama AJ. It’s not you, it’s me: self-perceptions, antifat attitudes, and stereotyping of obese individuals. Soc Psychol Personal Sci. 2015;6:749–57.
*Hunger JM, Blodorn A, Miller CT, Major B. The psychological and physiological effects of interacting with an anti-fat peer. Body Image. 2018;27:148–55.
Postmes T, Haslam SA, Jans L. A single‐item measure of social identification: reliability, validity, and utility. Br J Soc Psychol. 2013;52:597–617.
Tajfel H, editor. Differentiation between groups: studies in the social psychology of group interactions. London: Academic Press; 1978.
Tomiyama AJ. Weight stigma is stressful: a review of evidence for the cyclic obesity/weight-based stigma model. Appetite. 2014;82:8–15.
Wang SS, Brownell KD, Wadden TA. The influence of the stigma of obesity on overweight individuals. Int J Obes. 2004;28:1333–7.
Crandall CS. Prejudice against fat people: ideology and self-interest. J Pers Soc Psychol. 1994;66:882.
Tajfel H, Turner JC, Austin WG. Social psychology of intergroup relations. Annu Rev Psychol. 1982;33:1–39.
Meadows A, Higgs S. Challenging oppression: a social identity model of stigma resistance in higher-weight individuals. Body Image. 2022;42:237–45.
Tajfel H, Turner JC. An integrative theory of intergroup conflict. In: Austin WG, Worchel S, editors. Organizational identity. London: Academic Press; 1979. pp. 56–65.
Turner J, Hogg M, Oakes P, Reicher S, Wetherell M. Rediscovering the social group: a self-categorization theory. New York: Blackwell; 1987.
Cruwys T, Gunaseelan S. “Depression is who I am”: mental illness identity, stigma and wellbeing. J Affect Disord. 2016;189:36–42.
Kyprianides A, Easterbrook MJ, Cruwys T. “I changed and hid my old ways”: how social rejection and social identities shape well‐being among ex‐prisoners. J Appl Soc Psychol. 2019;49:283–94.
Branscombe NR, Schmitt MT, Harvey RD. Perceiving pervasive discrimination among African Americans: implications for group identification and well-being. J Personal Soc Psychol. 1999;77:135.
Schmitt MT, Branscombe NR, Kobrynowicz D, Owen S. Perceiving discrimination against one’s gender group has different implications for well-being in women and men. Pers Soc Psychol Bull. 2002;28:197–210.
Haslam C, Jetten J, Cruwys T, Dingle G, Haslam SA. The new psychology of health: unlocking the social cure. United Kingdom: Routledge; 2018.
Pearl RL, Puhl RM, Lessard LM, Himmelstein MS, Foster GD. Prevalence and correlates of weight bias internalization in weight management: a multinational study. SSM Popul Health. 2021;13:100755.
*Curll SL, Brown PM. Weight stigma and psychological distress: a moderated mediation model of social identification and internalised bias. Body Image. 2020;35:207–16.
*Magallares A, Morales JF, Rubio MÁ. Group identification, discrimination and psychological health in an obese sample. Int J Psychol Psychol Ther. 2014;14:421–31.
Pearl RL, Puhl RM. Weight bias internalization and health: a systematic review. Obes Rev. 2018;19:1141–63.
Cruwys T, Haslam SA, Dingle GA, Haslam C, Jetten J. Depression and social identity: an integrative review. Pers Soc Psychol Rev. 2014;18:215–38.
Page MJ, McKenzie JE, Bossuyt PM, Boutron I, Hoffmann TC, Mulrow CD, et al. The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ. 2021;372:1–35.
Cohen J. Statistical power analysis for the behavioral sciences. New York: Routledge; 2013.
Hill B, Bergmeier H, Incollingo Rodriguez AC, Barlow FK, Chung A, Ramachandran D, et al. Weight stigma and obesity‐related policies: a systematic review of the state of the literature. Obes Rev. 2021;22:e13333.
Thompson JK, Cattarin J. The perception of teasing scale. Behav Ther. 1992;15:230.
*Lee KM, Hunger JM, Tomiyama AJ. Weight stigma and health behaviors: evidence from the Eating in America Study. Int J Obes. 2021;45:1499–509.
*Wang Z, Wang B, Hu Y, Cheng L, Zhang S, Chen Y, et al. Relationships among weight stigma, eating behaviors and stress in adolescents in Wuhan, China. Glob Health Res Policy. 2020;5:8–20.
Williams DR, Yu Y, Jackson JS, Anderson NB. Racial differences in physical and mental health: socio-economic status, stress and discrimination. J Health Psychol. 1997;2:335–51.
Bilbao A, Mar J, Mar B, Arrospide A, Martínez de Aragón G, Quintana JM. Validation of the Spanish translation of the questionnaire for the obesity-related problems scale. Obes Surg. 2009;19:1393–400.
Lindly OJ, Nario-Redmond MR, Noel JG. Creatively re-defining fat: identification predicts strategic responses to stigma, ingroup attitudes, and well-being. Fat Stud. 2014;3:179–95.
Leach CW, Van Zomeren M, Zebel S, Vliek ML, Pennekamp SF, Doosje B, et al. Group-level self-definition and self-investment: a hierarchical (multicomponent) model of in-group identification. J Pers Soc Psychol. 2008;95:144–60.
Luhtanen R, Crocker J. A collective self-esteem scale: self-evaluation of one’s social identity. Pers Soc Psychol Bull. 1992;18:302–18.
Araiza AM, Vieira Zaidan AC, Wijayatunga NN, Wellman JD. Weight discrimination as a predictor of stress and eating: the role of identifying as “fat”. Appetite. 2025;206:107772.
*Wellman JD, Araiza AM, Nguyen T-VC, Beam AJ, Pal S. Identifying as fat: examining weight discrimination and the rejection-identification model. Body Image. 2022;41:46–51.
Wang Z, Wang B, Hu Y, Cheng L, Zhang S, Chen Y, et al. Relationships among weight stigma, eating behaviors and stress in adolescents in Wuhan, China. Glob Health Res Policy. 2020;5:1–9.
*Blodorn A, Major B, Hunger J, Miller C. Unpacking the psychological weight of weight stigma: a rejection-expectation pathway. J Exp Soc Psychol. 2016;63:69–76.
Rowlands K, Beaty T, Simic M, Grafton B, Hirsch C, Treasure J, et al. Cognitive bias modification training of attention and interpretation to reduce expectations of social rejection in adolescents with eating disorders: a small efficacy randomized controlled trial. Int J Eat Disord. 2022;55:1506–20.
*Brochu PM, Dovidio JF. Would you like fries (380 calories) with that? menu labeling mitigates the impact of weight-based stereotype threat on food choice. Soc Psychol Personal Sci. 2014;5:414–21.
*Major B, Hunger JM, Bunyan DP, Miller CT. The ironic effects of weight stigma. J Exp Soc Psychol. 2014;51:74–80.
Teixeira PJ, Silva MN, Coutinho SR, Palmeira AL, Mata J, Vieira PN, et al. Mediators of weight loss and weight loss maintenance in middle‐aged women. Obesity. 2010;18:725–35.
Muennig P, Jia H, Lee R, Lubetkin E. I think therefore I am: perceived ideal weight as a determinant of health. Am J Public Health. 2008;98:501–6.
*McCleary-Gaddy AT, Miller CT, Grover KW, Hodge JJ, Major B. Weight stigma and hypothalamic-pituitary-adrenocortical axis reactivity in individuals who are overweight. Ann Behav Med. 2019;53:392–8.
Decker KM, Philip SR, Thurston IB. Measuring weight-and shape-based social identity threat vulnerability in young adults. Body Image. 2022;42:136–44.
Vartanian LR, Pinkus RT, Smyth JM. The phenomenology of weight stigma in everyday life. J Context Behav Sci. 2014;3:196–202.
*Himmelstein MS, Belsky ACI, Tomiyama AJ. The weight of stigma: cortisol reactivity to manipulated weight stigma. Obesity. 2015;23:368–74.
Clark PA, Detterman DK. Performance of mentally retarded and nonretarded persons on a lifted-weight task with strategies reduced or eliminated. Am J Ment Defic. 1981;85:530–8.
Funding
Open Access funding enabled and organized by CAUL and its Member Institutions.
Author information
Authors and Affiliations
Contributions
Alice Hudson: conceived and designed the study, extracted the data, conducted the analysis, and drafted the initial manuscript. Responsible for critical revisions and ensuring the accuracy of the published work. Luisa Batalha: assisted in conceiving and designing the study, assisted in the development of the research methodology, participated in the data extraction. Participated in the drafting and revision of the manuscript. Joseph Ciarrochi: provided theoretical expert guidance and participated in the drafting of the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethical approval
This systematic review did not require ethical approval or informed consent as it involved the analysis of previously published studies and does not involve direct interaction with human participants or the collection of primary data. All studies included in this review adhered to ethical guidelines set forth by their respective institutions and ethics committees. The findings and conclusions drawn are based solely on existing literature.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
41366_2025_1755_MOESM1_ESM.docx
Higher-Weight Social Identity as a Risk and Protective Factor in the Negative Health Consequences of Weight Stigma: A Systematic Review
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Hudson, A., Batalha, L. & Ciarrochi, J. Higher-weight social identity as a risk and protective factor in the negative health consequences of weight stigma: a systematic review. Int J Obes 49, 1209–1228 (2025). https://doi.org/10.1038/s41366-025-01755-z
Received:
Revised:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41366-025-01755-z