Abstract
Objectives
To determine the near-term risk of stroke following a retinal artery occlusion (RAO).
Methods
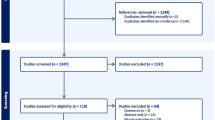
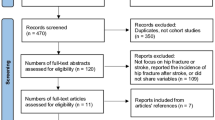
The risk of stroke was assessed in two manners; with a self-controlled case series (SCCS) and a propensity score (PS) matched cohort study using a US medical claims database. The date of RAO diagnosis was assigned as the index date. In the SCCS, incidence of stroke was compared in 30- and 7-day periods pre- and post-index date. In PS analysis, matched cohorts were created from patients with RAO or hip fracture. Cox proportional hazard regression assessed the hazard for stroke. Patients were censored at 1 year, upon leaving the insurance plan or if they had a qualifying event for the comparison group.
Results
The SCCS included 16,193 patients with RAO. The incidence rate ratio (IRR) of new stroke in the month after RAO was increased compared to all periods >2 months before and all months after the index date (IRRs: 1.68–6.40, p < 0.012). Risk was increased in the week immediately following the index date compared to most weeks starting 2 weeks prior to and all weeks immediately after the index date (IRRs: 1.93–29.00, p < 0.026). The PS study analysed 18,213 propensity-matched patients with RAO vs. hip fracture. The HR for having a stroke after RAO compared to a hip fracture was elevated in all analyses (All RAO HR: 2.97, 95% CI: 2.71–3.26, p < 0.001; CRAO HR: 3.24, 95% CI: 2.83–3.70, p < 0.001; BRAO HR: 2.76, 95% CI: 2.43–3.13, p < 0.001).
Conclusions
The highest risk for stroke occurs in the days following a CRAO or BRAO, supporting guidelines suggesting immediate referral to a stroke centre upon diagnosis.
Similar content being viewed by others
Log in or create a free account to read this content
Gain free access to this article, as well as selected content from this journal and more on nature.com
or
References
Brown GC. Systemic associations of retinal arterial obstructive disease. Int Ophthalmol Clin. 1991;31:1–14.
Park SJ, Choi NK, Seo KH, Park KH, Woo SJ. Nationwide incidence of clinically diagnosed central retinal artery occlusion in Korea, 2008 to 2011. Ophthalmology. 2014;121:1933–8.
Leavitt JA, Larson TA, Hodge DO, Gullerud RE. The incidence of central retinal artery occlusion in Olmsted County, Minnesota. Am J Ophthalmol. 2011;152:820–3.
Hayreh SS, Podhajsky PA, Zimmerman MB. Retinal artery occlusion: associated systemic and ophthalmic abnormalities. Ophthalmology. 2009;116:1928–36.
Recchia FM, Brown GC. Systemic disorders associated with retinal vascular occlusion. Curr Opin Ophthalmol. 2000;11:462–7.
Park SJ, Choi NK, Yang BR, Park KH, Lee J, Jung SY, et al. Risk and risk periods for stroke and acute myocardial infarction in patients with central retinal artery occlusion. Ophthalmology. 2015;122:2336–43.
Callizo J, Feltgen N, Pantenburg S, Wolf A, Neubauer AS, Jurklies B, et al. Cardiovascular risk factors in central retinal artery occlusion: results of a prospective and standardized medical examination. Ophthalmology. 2015;122:1881–8.
Chang YS, Jan RL, Weng SF, Wang JJ, Chio CC, Wei FT, et al. Retinal artery occlusion and the 3-year risk of stroke in Taiwan: a nationwide population-based study. Am J Ophthalmol. 2012;154:645–52.
Woo SC, Lip GY, Lip PL. Associations of retinal artery occlusion and retinal vein occlusion to mortality, stroke, and myocardial infarction: a systematic review. Eye. 2016;30:1031–8.
Lavin P, Patrylo M, Hollar M, Espaillat KB, Kirshner H, Schrag M. Stroke risk and risk factors in patients with central retinal artery occlusion. Am J Ophthalmol. 2018;196:96–100.
French DD, Margo CE, Greenberg PB. Ischemic stroke risk in medicare beneficiaries with central retinal artery occlusion: a Retrospective Cohort Study. Ophthalmol Ther. 2018;7:125–31.
Mir TA, Arham AZ, Fang W, Alqahtani F, Alkhouli M, Gallo J, et al. Acute vascular ischemic events in patients with central retinal artery occlusion in the United States: a Nationwide Study 2003–2014. Am J Ophthalmol. 2019;200:179–86.
Lee J, Kim SW, Lee SC, Kwon OW, Kim YD, Byeon SH. Co-occurrence of acute retinal artery occlusion and acute ischemic stroke: diffusion-weighted magnetic resonance imaging study. Am J Ophthalmol. 2014;157:1231–8.
Lauda F, Neugebauer H, Reiber L, Juttler E. Acute silent brain infarction in monocular visual loss of ischemic origin. Cerebrovasc Dis. 2015;40:151–6.
Golsari A, Bittersohl D, Cheng B, Griem P, Beck C, Hassenstein A, et al. Silent brain infarctions and leukoaraiosis in patients with retinal ischemia: a Prospective Single-Center Observational Study. Stroke. 2017;48:1392–6.
Rim TH, Han J, Choi YS, Hwang SS, Lee CS, Lee SC, et al. Retinal artery occlusion and the risk of stroke development: Twelve-Year Nationwide Cohort Study. Stroke. 2016;47:376–82.
Hong JH, Sohn SI, Kwak J, Yoo J, Ahn SJ, Woo SJ, et al. Retinal artery occlusion and associated recurrent vascular risk with underlying etiologies. PloS ONE. 2017;12:e0177663.
Flaxel CJ, Adelman RA, Bailey ST, Fawzi A, Lim JI, Vemulakonda GA, et al. Retinal and ophthalmic artery occlusions preferred practice pattern®. Ophthalmology. 2020;127:259–87.
Biousse V, Nahab F, Newman NJ. Management of acute retinal ischemia: follow the guidelines! Ophthalmology. 2018;125:1597–607.
Abel AS, Suresh S, Hussein HM, Carpenter AF, Montezuma SR, Lee MS. Practice patterns after acute embolic retinal artery occlusion. Asia Pac. Asia Pac J Ophthalmol. 2017;6:37–9.
Atkins EJ, Bruce BB, Newman NJ, Biousse V. Translation of clinical studies to clinical practice: survey on the treatment of central retinal artery occlusion. Am J Ophthalmol. 2009;148:172–3.
Cho KH, Kim CK, Woo SJ, Park KH, Park SJ. Cerebral small vessel disease in branch retinal artery occlusion. Invest Ophthalmol Vis Sci. 2016;57:5818–24.
Petersen I, Douglas I, Whitaker H. Self controlled case series methods: an alternative to standard epidemiological study designs. Bmj. 2016;354:i4515.
Porter J, Mondor L, Kapral MK, Fang J, Hall RE. How reliable are administrative data for capturing stroke patients and their care. Cerebrovasc Dis Extra. 2016;6:96–106.
Bearelly S, Mruthyunjaya P, Tzeng JP, Suner IJ, Shea AM, Lee JT, et al. Identification of patients with diabetic macular edema from claims data: a validation study. Arch Ophthalmol. 2008;126:986–9.
Muir KW, Gupta C, Gill P, Stein JD. Accuracy of international classification of diseases, ninth revision, clinical modification billing codes for common ophthalmic conditions. JAMA Ophthalmol. 2013;131:119–20.
Lau M, Prenner JL, Brucker AJ, VanderBeek BL. Accuracy of billing codes used in the therapeutic care of diabetic retinopathy. JAMA Ophthalmol. 2017;135:791–4.
Funding
National Institutes of Health K23 Award (1K23EY025729-01) and University of Pennsylvania Core Grant for Vision Research (2P30EY001583). The content is solely the responsibility of the authors and does not necessarily represent the official views of the NIH. Additional funding was provided by Research to Prevent Blindness, Karen & Herbert Lotman Fund for Macular Vision Research Foundation and the Paul and Evanina Mackall Foundation. None of the funding organizations had any role in the design or conduction of the study.
Author information
Authors and Affiliations
Contributions
Research design: Scoles, VanderBeek. Data collection: McGeehan, VanderBeek. Data analysis and interpretation: Scoles, McGeehan, VanderBeek. Obtaining funding: VanderBeek. Manuscript preparation: Scoles, McGeehan, VanderBeek. Brian VanderBeek had full access to all the data in the study and takes responsibility for the integrity of the data and the accuracy of the data analysis.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Scoles, D., McGeehan, B. & VanderBeek, B.L. The association of stroke with central and branch retinal arterial occlusion. Eye 36, 835–843 (2022). https://doi.org/10.1038/s41433-021-01546-6
Received:
Revised:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41433-021-01546-6
This article is cited by
-
Incidence and risk factors associated with ischemic cerebrovascular disease in patients with retinal artery occlusion: a systematic review and meta-analysis
Scientific Reports (2025)
-
Risks of stroke and myocardial infarction after retinal artery occlusion and their time dependence: a systematic review and meta-analysis
Journal of Neurology (2025)
-
Internistische Abklärung bei retinalen Gefäßverschlüssen
Die Ophthalmologie (2023)
-
Retinale arterielle Verschlüsse (RAV)
Die Ophthalmologie (2023)