Abstract
Interleukin-33 (IL-33) is a pleiotropic molecule that plays various roles in the body. However, how exogenous IL-33 changes the tumor immune microenvironment remains unclear. Our study revealed that exogenous IL-33 exerts anti-tumor effects and effectively suppresses the progression of subcutaneous melanoma. scRNA-seq analysis revealed that exogenous IL-33 reduced neutrophils accumulation, thereby improving the inhibitory immune environment. Flow cytometry analysis revealed that exogenous IL-33 significantly increased the proportion of eosinophils and group 2 innate lymphoid cells (ILC2s). In addition, we identified genes encoding major histocompatibility complex (MHC) class II molecules in this group of ILC2s, suggesting that ILC2s may play a role in antigen presentation. In Il7rCreArg1flox/flox mice, the decrease of ILC2s led to a reduction in the proportion of eosinophils. Furthermore, we found that exogenous IL-33 effectively promoted the differentiation of ILC2s and their accumulation in tumors, thereby enhancing the anti-tumor immune response. These findings may pave the way for developing new cancer immunotherapies that use IL-33 as an activator to enhance anti-tumor immune responses.
Similar content being viewed by others
Introduction
Interleukin-33 (IL-33) is a pleiotropic molecule that plays crucial roles in various physiological processes, including immunity, tissue development, homeostasis, and repair, and has drawn increasing attention in the field of tumor immunology1. IL-33, a multifunctional cytokine2, plays a significant role in the occurrence, progression, and immune response of tumors3,4. Studies have shown that IL-33 is expressed in various types of tumor tissues and that its expression level is closely related to the degree of malignancy and invasiveness of tumors5. For example, the expression of IL-33 is generally higher in breast, lung, and liver cancer6,7,8,9. In addition, IL-33 promotes the proliferation and activation of immune cells and infiltrates various tissues, thereby inhibiting lung tumor metastasis10,11,12,13. These results demonstrate the important role of IL-33 in carcinogenesis.
IL-33, through its receptor suppressor of tumorigenicity 2 (ST2), activates downstream signaling pathways and participates in tumorigenesis14. And it promotes anti-tumor immune responses by activating immune cells such as natural killer (NK) cells, T cells, and macrophages10,11,12,13,15. These immune cells inhibit tumor growth and metastasis by releasing cytokines and chemokines. In contrast, IL-33 may suppress anti-tumor immune responses by promoting the proliferation and invasion of tumor cells, thereby promoting tumor progression16,17,18,19,20. This dual mechanism of action allows IL-33 to play a complex role in tumor immune responses. Therefore, reasonable utilization of the dual mechanism of IL-33 in tumor therapy has become a key research topic.
The tumor microenvironment (TME) is an important site for tumor growth and development. Group 2 innate lymphoid cells (ILC2s) have recently attracted attention21. ILC2s not only exist as immune regulators but also participate in multiple processes such as the growth, differentiation, and metastasis of tumor cells22,23,24. ILC2s can inhibit antitumor immune responses and promote tumor growth and metastasis25. For example, in some types of tumors, ILC2s can be activated to recruit myeloid-derived suppressor cells (MDSCs) with inhibitory antitumor immune abilities, which in turn inhibit the function of antitumor T cells, thereby promoting the occurrence and progression of tumors26,27. In addition, cytokines such as IL-25 can activate ILC2s and promote tumor growth through a similar mechanism28.
Although ILC2s may promote tumor growth in some cases, they also play an indispensable role in anti-tumor immunity29. For example, ILC2s can activate and recruit other immune cells, such as eosinophils and NK cells, to jointly resist tumor cells21,30. In addition, ILC2s can secrete cytokines, such as IL-13, to induce tumor cells to express MHC class II molecules, thereby increasing the sensitivity of tumor cells to CD4+ T cells and enhancing the anti-tumor immune response31,32,33. Given the dual nature of IL-33 and ILC2s in the occurrence and progression of tumors, it is imperative to understand the combined role of IL-33 and ILC2s.
In this study, we present evidence that exogenous IL-33 can effectively inhibit the progression of B16-F10 melanoma by affecting the proportion and number of tumor-infiltrating immune cells. Our findings highlight that ILC2s play a positive role in antitumor immune responses. In the Il7rCreArg1flox/flox conditional knockout model, we found that the number of ILC2s affected the proportion of eosinophils and neutrophils. Moreover, we detected genes encoding MHC class II molecules on the surface of ILC2s. This also led us to hypothesize that ILC2s might play a role in antigen presentation. In summary, this study reveals a novel role for exogenous IL-33 in orchestrating the activity of various immune cells within the tumor microenvironment to exert anti-tumor effects.
Results
Exogenous IL-33 plays a role in inhibiting tumor growth
We aimed to determine whether IL-33 could play a role in anti-tumor immunity and identify the cells that it targets. We subcutaneously injected B16-F10 cells into C57BL/6 mice and began treating them with IL-33 on the fourth day post-inoculation for ten consecutive days (Fig. 1A). The results indicate that IL-33 effectively protects the host and reduce the effects of tumor, with an increasingly stronger effect starting on day six of treatment (Fig. 1B). This suggests that IL-33 administration may effectively activate an anti-tumor response. On day 14 post-inoculation, we removed the draining lymph nodes on the inoculated side of the mice and the tumor tissues from their bodies, photographed them, and weighed them. These results further verify our findings. After IL-33 treatment, the tumor tissues were significantly smaller than those in the control group, and their quality decreased significantly (Fig. 1C). We also monitored weight changes in the mice during the treatment period (Fig. 1D). The body weight of the treatment group increased, which may be related to the production of a certain amount of ascites after treatment.
IL−33 can effectively inhibit tumor growth. (A) Design of the suppression experiment. Mice were inoculated with tumor cells, followed by intraperitoneal injections of either recombinant IL-33 (rIL-33) or PBS for 10 days (blue arrow). (B, C) Cumulative tumor curve (B) and tumor weight (C) of B16-F10 melanoma tumors in C57BL/6 N mice with different treatments (n = 7). Tumor size was monitored every 2 days. (D) The weight changes of B16-F10 melanoma bearing mice under two treatment methods. (E-H) Representative flow cytometry plot of the percentage of CD4+ T cells (E), CD8+ T cells (E), ILCs (F), ILC2s (G) and DCs (H) in draining lymph nodes. (I-K) The number of ILCs (I), ILC2s (J) and DCs (K) contained in each lymph node in draining lymph nodes. The data is from one of three identical experiments (day 14 takedown). The outcomes of the two remaining experiments are presented in Fig. S2. Two-way analysis of variance (ANOVA) was used to determine statistical significance for time points when all mice were viable for tumor measurement. The value marked in the figure is the proportion of this cell population to CD45+ cells. Graphs shown represent data summarized as means ± SEM and were analyzed by unpaired two-tailed Student’s t test. Data were presented as the means ± SD and p values are indicated. *p < 0.05, **p < 0.01, ***p < 0.001, and ****p < 0.0001. ILCs, innate lymphoid cells; ILC2s, type 2 innate lymphoid cells; DCs, dendritic cells.
Exogenous IL-33 can change proportion and number of cells in secondary lymphoid organs
Given the antitumor effects of IL-33, we sought to investigate the pathways via which it exerts these effects. We obtained draining lymph nodes from the sides of tumor-bearing mice and performed flow cytometry analysis. The results show that IL-33 did not significantly affect the ratio of CD4+ T cells and CD8+ T cells in the draining lymph nodes (Fig. 1E). The proportions of these two cell types remained relatively unchanged after treatment. However, when analyzing the lineage negative (Lin−) cells, we observed an increase in the proportion and number of innate lymphoid cells (ILCs; gate on Lin− CD90.2+ CD127+) following IL-33 treatment (Fig. 1F, I). Further analysis revealed that the proportion of ILC2s (gate on KLRG1+ ST2+ of ILCs) increased by approximately 100 times and the cell number increased by approximately 150 times (Fig. 1G, J). We speculated that most of the increased ILCs in the treatment group were ILC2s. As for dendritic cells (DCs; gate on CD45+ CD11c+ I-A/I-E+) in the lymph nodes, although the proportion increased after treatment, there was no significant difference in cell number (Fig. 1H, K).
Exogenous IL-33 regulates TME to promote antitumor effects
To understand how exogenous IL-33 affects the antitumor function of tumor-infiltrating immune cells, single-cell suspensions isolated from B16-F10 melanoma cells were analyzed by flow cytometry. The results show that the proportion of CD8+ T cells in the tumors increased significantly, whereas the proportion of CD4+ T cells did not change. However, when normalized to the number of cells per gram of tumor, the number of both cell types increased significantly after treatment (Fig. 2A). Regulatory T (Treg) cells (gate on CD4+ Foxp3+) play a crucial role in maintaining peripheral tolerance and preventing systemic autoimmune diseases34,35. However, they appear to play a dual role in mediating antitumor immunity36. Evidence indicates that Treg cells can promote a suppressive tumor microenvironment, thereby suppressing anti-tumor immunity. However, some studies have indicated that Treg cells develop a fragile phenotype in the presence of inflammatory signals, which could alter the suppressive function of Treg cells37,38. Our analysis of Treg cell-infiltrating tumors revealed that, although the proportion of Treg cells in the treatment group was comparable to that in the control, the cell count doubled (Fig. 2B, G). Further analysis revealed that a significant proportion of the increased Treg cells were ST2+ Treg cells (Fig. 2C). At the same time, the number of ST2+ Treg in the treatment group was significantly higher than that in the control group (Fig. 2H).
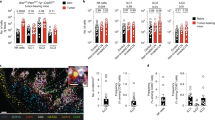
The changes of myeloid and lymphoid compartments in the TME. (A) Representative flow cytometry plot and quantitative plot of the percentage of CD4+ T cells and CD8+ T cells. (B-F) Representative flow cytometry plot of the percentage of Treg cells (B), ST2+ Treg cells (C), ILCs (D), ILC2s (E) and I-A/I-E+ ILC2s (F) in TME. (G-K) The number of Treg cells (G), ST2+ Treg cells (H), ILCs (I), ILC2s (J) and I-A/I-E+ ILC2s (K) per gram of tumor. (L, M) Representative flow cytometry plot of the percentage of eosinophils (L), neutrophils (L) and NK cells (M) in TME. (N-P) The number of eosinophils (N), neutrophils (O) and NK cells (P) per gram of tumor. The data is from one of three identical experiments (day 14 takedown). The outcomes of the two remaining experiments are presented in Fig. S2. The value marked in the figure is the proportion of this cell population to CD45+ cells. The graphs shown represent data analyzed as means ± SD and were analyzed by unpaired two-tailed Student’s t-test. *p < 0.05, **p < 0.01, ***p < 0.001, and ****p < 0.0001.
Subsequently, we analyzed cells lacking the immune cell lineage marker within the tumor, and the results were similar to those obtained in the draining lymph nodes. The proportion and number of tumor-infiltrating ILCs increased (Fig. 2D, I), and most of these cells were ILC2s (Fig. 2E, J). Additionally, we observed that a large amount of I-A/I-E (a marker of MHC II) was expressed in tumor-infiltrating ILC2s in the treatment group (Fig. 2F, K), suggesting that these ILC2s may also play a role in antigen presentation.
We focused on eosinophils (gate on CD11b+ Siglec-F+ Ly-6G−) and neutrophils (gate on CD11b+ Siglec-F− Ly-6G+) in tumor-infiltrating myeloid cells. We found that the proportion and cell count of eosinophils increased (Fig. 2L, N), whereas those of neutrophils decreased (Fig. 2L, O). This indicates that exogenous IL-33 can promote the recruitment of eosinophils to tumors to a certain extent, thereby exerting anti-tumor effects. NK cells are important human immune cells. Although we did not observe any changes in the proportion of NK cells in the tumors of the treatment group (Fig. 2M), the cell count per gram of tumor increased three to four times (Fig. 2P). This may also explain the smaller tumors in the treatment group.
Exogenous IL-33 can promote aggregation of ILC2s in tumors
We used scRNA-seq data to detect infiltrating immune cells other than T cells in B16-F10 tumors. Using t-SNE analysis, we identified nine different clusters of immune cells corresponding to B cells, neutrophils, eosinophils, basophils, DCs, NK cells, natural killer T (NKT) cells, ILCs, and monocytes (Fig. 3A). We divided the clusters into two groups. There were a large number of neutrophils, monocytes, and some NK cells in the tumor tissues of the control group. In the treatment group, most of the cells were ILCs, followed by eosinophils (Fig. 3B). At the same time, we also measured the proportion of each cluster, and the results were similar to the above (Fig. 3C). This indicates that IL-33 enhances the infiltration of ILCs into tumor tissues.
The regulation of IL−33 on tumor-infiltrating immune cells. (A) t-SNE dimensionality reduction projects other tumor-infiltrating immune cells except T cells from B16-F10 tumor-bearing WT mice to two dimensions showing nine subclusters differentiated by color. Each point represents a single cell, with cells of similar gene expression profiles positioned closer together in the projection. (B) Two dimensions spatial projection of tumor-infiltrating immune cells across control groups (green) and IL-33 treatment groups (red). (C) The proportion of tumor-infiltrating immune cell clusters in the two different groups. (D) Dot plot showing the gene expression profiles of nine cell clusters, based on tumor scRNA-seq analysis. The genes expressed as features on the ILCs are indicated within the box. (E) Spatial clustering of gene expression intensities. DCs, dendritic cells; ILCs, innate lymphoid cells; NKT, natural killer T cells.
By ranking the expression levels of genes in different immune cell clusters, we found that NK cells expressed highly related genes, including Klre1, Nkg7, and Granzyme A. B cells prominently expressed CD79a, Mzb1, and Iglc3. Basophils expressed high levels of Gata2, CD200r3, and Cpa3 (Fig. 3D). Meanwhile, we found that ILCs expressed a large number of ILC2s-related markers, such as Rorα, Gata3, and Arg1. This finding is consistent with the results of our previous study. In our previous study, we found that ILC2s were the only lymphoid cell type that could express the Arg1 gene. Reportedly, ST2, the co-receptor of IL-33, is highly expressed on ILC2s11,13,39. Therefore, we conducted a cluster analysis of specific markers and transcription factors in ILCs. Among these ILCs, the expression of the ILC2s-related marker ST2 and its transcription factor Gata3 was significantly higher than that in the other types of ILCs (Fig. 3E). These data suggest that exogenous IL-33 enhances the aggregation of ILCs, especially ILC2s, in tumors.
Exogenous IL-33 can induce differentiation of ILC2s
Studies have shown that Il7r can be used as a characteristic marker of ILC2s in lymphoid cells40,41,42,43,44. Further, the Arg1 gene plays an important role in the regulation of cell proliferation. We constructed a conditional knockout mouse model using the Cre-loxP system to simulate the absence of ILC2s (Fig. 4A). As in previous experiments, B16-F10 cells were subcutaneously inoculated into the mice. We found that in the absence of ILC2s, the anti-tumor effect of IL-33 was affected. Moreover, under natural conditions, the absence of ILC2s further increased the size of the tumor (Fig. 4B). After removing the tumors, we photographed and weighed them and found that the tumors in Il7rCreArg1flox/flox (CKO) mice were larger than those in Il7rCreArg1+/+ (CON) mice under natural conditions (Fig. 4C, D). In the IL-33 treatment group, the spleens of mice were enlarged (Fig. 4E), which was consistent with that of wild-type mice, indicating that IL-33 can enhance the immune response in vivo. We analyzed the draining lymph nodes on the side of inoculation and found that IL-33 did not significantly alter the proportion of CD4+ T cells and CD8+ T cells in the lymph nodes of either mouse type (Fig. 4F, G). In contrast, IL-33 increased the proportions of ILCs and ILC2s, although these proportions were reduced in the CKO model compared to CON model (Fig. 4H–J). We speculated that exogenous IL-33 could induce the further differentiation of ILC2s.
IL−33 possesses the capacity to induce the differentiation of ILC2s. (A) Strategy of generation of Il7rCreArg1flox/flox mice. (B-D) B16-F10 tumor cells were inoculated intradermally into the right flank of the female CON (Il7rCreArg1+/+) and CKO (Il7rCreArg1flox/flox) mice. Tumor size was monitored every 2 days. Cumulative tumor curve (B), tumor size (C) and tumor weight (D) of B16-F10 tumor-bearing CON and CKO mice with different treatments (n = 4 to 6). (E) The spleen weights of tumor-bearing CON and CKO mice. (F, G) The proportion of CD4+ T cells (F) and CD8+ T cells (G) in draining lymph nodes. (H) Representative flow cytometry plot of the percentage of ILC2s. (I, J) The proportion of ILCs (I) and ILC2s (J) in draining lymph nodes. The data is from one of four identical experiments (day 14 takedown). The outcomes of the three remaining experiments are presented in Fig. S3-5. Two-way analysis of variance (ANOVA) was used to determine statistical significance for time points when all mice were viable for tumor measurement. The value marked in the figure is the proportion of this cell population to CD45+ cells. Graphs shown represent data summarized as means ± SEM and were analyzed by unpaired two-tailed Student’s t test. Data were presented as the means ± SD and p values are indicated. *p < 0.05, **p < 0.01, ***p < 0.001, and ****p < 0.0001.
Furthermore, we conducted flow cytometric analysis of single-cell suspensions isolated from B16-F10 melanoma cells. In myeloid cells, the proportion of neutrophils significantly increased in the absence of ILC2s, whereas that of eosinophils was relatively low (Fig. 5A–C). IL-33 effectively reverses this effect. Subsequently, we analyzed the lymphoid cells. The results found no significant difference in the proportion of tumor-infiltrating CD4+ T cells and CD8+ T cells between the two models (Fig. 5D, E). The increase in ST2+ Treg cells observed in wild-type mouse models still existed after IL-33 treatment. At the same time, in the absence of ILC2s, Treg cells infiltration in tumor tissue was relatively reduced (Fig. 5F, G). In addition, the proportion of tumor infiltrating ILC2s still increased after IL-33 stimulation, although the increase in CKO model was limited (Fig. 5H–J). This indicates that the CKO model can inhibit the transformation of ILC2s to a certain extent and that IL-33 can reverse this process.
IL-33 altered immune cells population in the TME. (A) Representative flow cytometry plot of the percentage of eosinophils and neutrophils. (B, C) The proportion of tumor-infiltrating eosinophils (B) and neutrophils (C). (D-G) The proportion of tumor-infiltrating CD4+ T cells (D), CD8+ T cells (E), Treg cells (F) and ST2+ Treg cells (G). (H) Representative flow cytometry plot of the percentage of tumor-infiltrating ILC2s. (I, J) The proportion of tumor-infiltrating ILCs (I) and ILC2s (J). The data is from one of four identical experiments (day 14 takedown). The outcomes of the three remaining experiments are presented in Fig. S3-5. The value marked in the figure is the proportion of this cell population to CD45+ cells. The graphs shown represent data analyzed as means ± SD and were analyzed by unpaired two-tailed Student’s t-test. *p < 0.05, **p < 0.01, ***p < 0.001, and ****p < 0.0001.
Discussion
IL-33 can recruit and activate CD8+ T and NK cells, which play a key role in anti-tumor immunity and help inhibit tumor cell metastasis15. Given the positive role of IL-33 in anti-tumor immunity, it is considered a potential target for immunotherapy1. In this study, we determined the effectiveness of IL-33 and verified that exogenous IL-33 administration inhibited the progression of B16-F10 melanoma. Further evidence has shown that IL-33 can increase the proportion of eosinophils and decrease that of neutrophils, which provides a macroscopic mechanism for the anti-tumor immunity of IL-33 and may improve the immunosuppressive TME.
The relationship between ILC2s and tumor immunity is complex. In some tumors, such as lung cancer and breast cancer45,46, ILC2s have been reported to promote cancer progression by coordinating an immunosuppressive tumor microenvironment, which may be related to the immune checkpoint receptors expressed by ILC2s, such as PD-1, as well as recruiting macrophages and MDSCs under specific signals, such as IL-4 and IL-1326. However, in other types of tumors, such as intestinal cancer47, ILC2s exhibit an anti-tumor immune effect48,49,50. In our study, we found that exogenous IL-33 could effectively stimulate an increase in infiltrating immune cells in draining lymph nodes and tumors. Further analysis revealed that most of the increased cells were ILC2s in tumors with significantly reduced volumes. This is consistent with our hypothesis and scRNA-seq results.
To further clarify the potential source of tumor-infiltrating ILC2s, we used a conditional knockout model. Our data demonstrate that, under natural conditions, the proportion of ILC2s in the CKO model was reduced, indicating that the model effectively suppressed the natural differentiation of ILC2s. Previous studies have demonstrated that ILC2s can influence tumor prognosis by secreting type 2 cytokines such as GM-CSF and IL-527,50. IL-5 is a key cytokine in eosinophil production, and its concentration affects the number of eosinophils. We observed a reduction in the proportion of eosinophils in the CKO model under the treatment of IL-33, further validating its efficacy. As we and others previously found, exogenous but not endogenous IL-33 increases the proportion and number of ST2+ Treg cells in the spleen, inflamed lung tissues, and tumors51,52,53. We use this model to test our hypotheses. The results show that under stimulation by IL-33, the proportions of ILCs and ILC2s in the CKO model increased to some extent, although there was still a significant difference compared to the CON model. Moreover, we found that most of the newly added ILCs were ILC2s, indicating that exogenous IL-33 effectively induces the differentiation of ILC2s.
Our results reveal an important tumor-suppressive role for exogenous IL-33, potentially opening new avenues in cancer immunology. Il7rCreArg1flox/flox conditional knockout model can also effectively inhibit the differentiation of ILC2s under natural conditions. This makes it become a good model for studying ILC2s. Moreover, we also demonstrated the rationality of IL-33 in tumor immunotherapy by promoting the differentiation of ILC2. However, further studies are needed to investigate how IL-33 immunotherapy can be effectively combined with conventional treatments to optimize outcomes. Although strategies that utilize ILC2s-based immunotherapy show great promise, further research and clinical trials are necessary to confirm their safety and efficacy. Because in the course of our experiments, we found that mice stimulated with IL-33 developed varying degrees of splenomegaly and ascites. We analyzed these adverse events that may be related to the way we administer the drug. So, further experiments are needed to explore ways to reduce these adverse events. At the same time, we also need to further explore the synergistic effect of IL-33 and PD-1 on tumors to play a better anti-tumor effect.As research advances and technology improves, we anticipate that IL-33 will play a significant role in the future of cancer treatment.
Methods
Mice
C57BL/6 mice were purchased from Jackson Labs and bred in-house.Il7rCre, and Arg1flox/flox mice were generated by Shanghai Model Organisms. To obtain Il7rCreArg1flox/flox mice, we crossed Arg1flox/flox mice with Il7rCre mice. Il7rCreArg1flox/flox mice and controls were generated by breeding Arg1flox/flox mice with Il7rCreArg1flox/+ mice (Fig. S1A). All mice were maintained under specific pathogen-free conditions. For all experiments, unless stated otherwise, 8 to 12-week-old mice were used by age and sex-matched. Mice with the same genotypes were randomly assigned to different treatment groups. All animal experiments performed in this study were approved by the Institutional Animal Care and Use Committee (IACUC) of the Southern University of Science and Technology. All animal experiments were conducted in accordance with the ARRIVE guidelines 2.0. All methods were performed in accordance with the relevant guidelines and regulations.
Cell lines
Cell line of B16-F10 melanoma was purchased from ATCC. B16-F10 was cultured in DMEM (ATCC) containing 10% heat-inactivated FBS (Gibco), 2 mM L-glutamine (Gibco), 100 mg/ml streptomycin (Gibco), and 100 U/ml penicillin (Gibco). Before using, cells for injections were passaged at least three times after being thawed. All cell lines were tested negative for mycoplasma by PCR.
Tumor growth in vivo
Syngeneic female C57BL/6 wild-type mice or genetically modified mice were shaved and anesthetized using isoflurane. 1 × 105 B16-F10 cells were prepared in 50 µl of 50:50 Matrigel (Corning) and 1 × PBS (Gibco) and then subcutaneously injected into the right flank. PBS or 1 µg per mouse daily of carrier-free recombinant mouse IL-33 (Biolegend) in sterile PBS was intraperitoneally injected into mice for 10 days since the day we discovered the appearance of the tumor. A caliper was used to measure the tumor length and width every 2 days, and tumor volumes were calculated by the formula volume = length×width2/2. For the termination of the experiment, the time was determined by a tumor length > 15 mm or tumor volume > 1000 mm3 or other situations requiring euthanasia as defined by institutional IACUC guidelines.
Tumor-infiltrating immune cell isolation
Mice were euthanized by cervical dislocation and dissected the tumors with surgical scissors and forceps. After recording the tumor weight, the tumors were minced and digested by 1 mg/ml Collagenases IV (Sigma) and 0.25 mg/ml DNase I (Sigma) in Hank’s balanced salt solution (Gibco, with Ca2+ and Mg2+) containing 0.5% BSA (Sigma) and 10mM HEPES (Gibco) for 45 min at 37℃ with gentle agitation. Digestion was quenched by adding 5 times of buffer which consists of PBS with 0.3% BSA and 2 mM EDTA (Invitrogen). Digested tissue was then meshed through a 70-µm cell strainer to collect single cells, and cells were washed in FACS buffer (PBS containing 0.3% BSA and 0.3% sodium azide). Tumor-infiltrating immune cells were recovered from the interface after centrifugation on a 40–80% Percoll (GE Healthcare) density gradient media. In some situations, the cells were further lysed with ACK buffer (Lonza) to remove red blood cells and washed with FACS buffer.
Flow cytometry
Single-cell suspensions were blocked with anti-CD16/32 (clone 93) and stained with fixable viability dye Zombie NIR (Biolegend) for 10–20 min, then stained with fluorescently conjugated antibodies for 30 min on ice in FACS buffer54. CD90 (clone 53 − 2.1), CD11b (clone M1/70), CD11c (clone N418), CD45 (clone 30-F11), TCRβ (clone H57-597), CD4 (clone RM4-5), CD8 (clone 53 − 6.7), CD127 (clone A7R34), KLRG1 (clone 2F1/KLRG1), ST2 (clone DJ8), SiglecF (clone E50-2440), Ly-6G (clone 1A8), Ly-6 C (clone HK1.4), I-A/I-E (clone M5/114.15.2), F4/80 (clone BM8), CD80 (clone 16-10A1), FcεRI (clone MAR-1), CD335 (clone 29A1.4), Gr1 (clone RB6-8C5), NK1.1 (clone PK136), Foxp3 (clone FJK-16s) were purchased from BD Bioscience, eBiosciences, or BioLegend. For transcription factor staining, cells were fixed and permeabilized by Foxp3/Transcription Factor Staining Buffer Set (Invitrogen) for 45–60 min at room temperature. After being washed twice, the cells were then stained for 45–60 min with anti-Foxp3 antibodies. Stained cells were analyzed on a FACSAriaIII (BD). The acquired data were then analyzed using Flowjo software (V.10.8.1). The gating strategy of each cell group is shown in Fig. S1B-C.
scRNA-seq data processing
Cells were purified by fluorescence-activated cell sorting and washed twice in PBS with BSA (300 µg/ml) and then resuspended with the concentration of 1000 cells/µl. During the library preparation process, a single Gel Bead and a single cell are encapsulated in separate oil in water droplets to form a GEM. Each Gel Bead has unique Barcode and UMI sequences, as well as Poly-dT primer sequences for initiating reverse transcription reactions. In this GEM reaction system, cells undergo fragmentation and lysis, while releasing mRNA and initiating a reverse transcription reaction with Poly-dT primer sequences under the action of reverse transcriptase. The final Full cDNA was obtained. Libraries were sequenced on an Illumina HiSeq/Nocaseq platform with 40,000 reads per cell on average. t-SNE dimensionality reduction methods using the R package were implemented to classify and visualize the subpopulations of tumor-infiltrating immune cells according to the markers.
Statistical analysis
All statistical analyses were conducted using GraphPad Prism 9. All data are presented as mean ± SD or mean ± SEM unless otherwise stated. Statistical significance was calculated by unpaired 2-tailed Student’s t-test, ordinary one-way ANOVA followed by a Tukey’s multiple comparisons test, and ordinary two-way ANOVA with *p < 0.05; **p < 0.01; ***p < 0.001; ****p < 0.0001; ns = not significant.
Data availability
Sequence data that support the findings of this study have been deposited in National Center for Biotechnology Information (NCBI) and freely available following publication (https://www.ncbi.nlm.nih.gov/sra/PRJNA1173306). The other data that support the findings of this study are available from the corresponding author upon reasonable request.
References
Liew, F. Y., Girard, J. P. & Turnquist, H. R. Interleukin-33 in health and disease. Nat. Rev. Immunol. 16(11), 676–689. https://doi.org/10.1038/nri.2016.95 (2016).
Carriere, V. et al. IL-33, the IL-1-like cytokine ligand for ST2 receptor, is a chromatin-associated nuclear factor in vivo. P Natl. Acad. Sci. USA. 104(1), 282–287. https://doi.org/10.1073/pnas.0606854104 (2006).
Dwyer, G. K., D’Cruz, L. M. & Turnquist, H. R. Emerging functions of IL-33 in homeostasis and immunity. Annu. Rev. Immunol. 40, 15–43. https://doi.org/10.1146/annurev-immunol-101320-124243 (2022).
Martin, N. T. & Martin, M. U. Interleukin 33 is a guardian of barriers and a local alarmin. Nat. Immunol. 17(2), 122–131. https://doi.org/10.1038/ni.3370 (2016).
Palmer, G., Moulin, D., Donzé, O., Talabot-Ayer, D. & Gabay, C. IL-33: a novel cytokine with proinflammatory properties. Arthritis Res. Ther. 9, P9. https://doi.org/10.1186/ar2235 (2007).
Perri, G. et al. Interleukin 33 supports squamous cell carcinoma growth via a dual effect on tumour proliferation, migration and invasion, and T cell activation. Cancer Immunol. Immun. 73(6), 110. https://doi.org/10.1007/s00262-024-03676-8 (2024).
He, P. Y. et al. Interleukin-33/serum stimulation-2 pathway: Regulatory mechanisms and emerging implications in immune and inflammatory diseases. Cytokine Growth F R. 76, 112–126. https://doi.org/10.1016/j.cytogfr.2023.12.001 (2023).
Mok, M. Y., Luo, C. Y., Huang, F. P., Kong, W. Y. & Chan, G. C. F. IL-33 orchestrated the interaction and immunoregulatory functions of alternatively activated macrophages and regulatory T cells in vitro. J. Immunol. 211(7), 1134–1143. https://doi.org/10.4049/jimmunol.2300191 (2023).
Holgado, A. et al. A20 is a master switch of IL-33 signaling in macrophages and determines IL-33-induced lung immunity. J. Allergy Clin. Immun. 152(1), 244–256. https://doi.org/10.1016/j.jaci.2023.02.026 (2023).
Dominguez, D. et al. Exogenous IL-33 restores dendritic cell activation and maturation in established cancer. J. Immunol. 198(3), 1365–1375. https://doi.org/10.4049/jimmunol.1501399 (2016).
Wan, J. et al. ILC2-derived IL-9 inhibits colorectal cancer progression by activating CD8 + T cells. Cancer Lett. 502, 34–43. https://doi.org/10.1016/j.canlet.2021.01.002 (2021).
Hollande, C. et al. Inhibition of the dipeptidyl peptidase DPP4 (CD26) reveals IL-33-dependent eosinophil-mediated control of tumor growth. Nat. Immunol. 20(3), 257–264. https://doi.org/10.1038/s41590-019-0321-5 (2019).
Jacquelot, N. et al. Blockade of the co-inhibitory molecule PD-1 unleashes ILC2-dependent antitumor immunity in melanoma. Nat. Immunol. 22(7), 851–864. https://doi.org/10.1038/s41590-021-00943-z (2021).
Yeoh, W. J., Vu, V. P. & Krebs, P. IL-33 biology in cancer: An update and future perspectives. Cytokine. 157, 155961. https://doi.org/10.1016/j.cyto.2022.155961 (2022).
Che, K. et al. Macrophages reprogramming improves immunotherapy of IL-33 in peritoneal metastasis of gastric cancer. Embo Mol. Med. 16(2), 251–266. https://doi.org/10.1038/s44321-023-00012-y (2024).
Saranchova, I. et al. A novel type-2 innate lymphoid cell-based immunotherapy for cancer. Front. Immunol. 15, 1317522. https://doi.org/10.3389/fimmu.2024.1317522 (2024).
Park, J. H. et al. Nuclear IL-33/SMAD signaling axis promotes cancer development in chronic inflammation. Embo J. 40(7), e106151. https://doi.org/10.15252/embj.2020106151 (2021).
Zhao, M. et al. IL-33/ST2 signaling promotes constitutive and inductive PD-L1 expression and immune escape in oral squamous cell carcinoma. Brit J. Cancer 128(5), 833–843. https://doi.org/10.1038/s41416-022-02090-0 (2022).
Dai, J. Z. et al. Obesity-mediated upregulation of the YAP/IL33 signaling axis promotes aggressiveness and induces an immunosuppressive tumor microenvironment in breast cancer. J. Cell. Physiol. 238(5), 992–1005. https://doi.org/10.1002/jcp.30985 (2023).
Faas, M. et al. IL-33-induced metabolic reprogramming controls the differentiation of alternatively activated macrophages and the resolution of inflammation. Immunity. 54(11), 2531–2546. https://doi.org/10.1016/j.immuni.2021.09.010 (2021).
Lu, H. F. et al. ILC2s: Unraveling the innate immune orchestrators in allergic inflammation. Int. Immunopharmaccol. 131, 111899. https://doi.org/10.1016/j.intimp.2024.111899 (2024).
Li, Z. et al. Therapeutic application of human type 2 innate lymphoid cells via induction of granzyme B-mediated tumor cell death. Cell. 187(3), 624–641. https://doi.org/10.1016/j.cell.2023.12.015 (2024).
Howard, E. et al. PD-1 blockade on tumor microenvironment-resident ILC2s promotes TNF-α production and restricts progression of metastatic melanoma. Front. Immunol. 12, 733136. https://doi.org/10.3389/fimmu.2021.733136 (2021).
Yuan, X., Rasul, F., Nashan, B. & Sun, C. Innate lymphoid cells and cancer: Role in tumor progression and inhibition. Eur. J. Immunol. 51(9), 2188–2205. https://doi.org/10.1002/eji.202049033 (2021).
Spits, H. & Mjösberg, J. Heterogeneity of type 2 innate lymphoid cells. Nat. Rev. Immunol. 22(11), 701–712. https://doi.org/10.1038/s41577-022-00704-5 (2022).
Trabanelli, S. et al. Tumour-derived PGD2 and NKp30-B7H6 engagement drives an immunosuppressive ILC2-MDSC axis. Nat. Commun. 8(1), 593. https://doi.org/10.1038/s41467-017-00678-2 (2017).
Konjević, G. M., Vuletić, A. M., Mirjačić Martinović, K. M. & Larsen, A. K. & Jurišić, V. B. The role of cytokines in the regulation of NK cells in the tumor environment. Cytokine. 117, 30–40. https://doi.org/10.1016/j.cyto.2019.02.001 (2019).
Jou, E. et al. An innate IL-25-ILC2-MDSC axis creates a cancer-permissive microenvironment for Apc mutation-driven intestinal tumorigenesis. Sci. Immunol. 7(72), abn0175. https://doi.org/10.1126/sciimmunol.abn0175 (2022).
Schwartz, C. et al. ILC2s regulate adaptive Th2 cell functions via PD-L1 checkpoint control. J. Exp. Med. 214(9), 2507–2521. https://doi.org/10.1084/jem.20170051 (2017).
Jarick, K. J. et al. Non-redundant functions of group 2 innate lymphoid cells. Nature. 611(7937), 794–800. https://doi.org/10.1038/s41586-022-05395-5 (2022).
Ercolano, G. et al. PPARɣ drives IL-33-dependent ILC2 pro-tumoral functions. Nat. Commun. 12(1), 2538. https://doi.org/10.1038/s41467-021-22764-2 (2021).
Schuijs, M. J. et al. ILC2-driven innate immune checkpoint mechanism antagonizes NK cell antimetastatic function in the lung. Nat. Immunol. 21(9), 998–1009. https://doi.org/10.1038/s41590-020-0745-y (2020).
Qi, J. et al. Single-cell transcriptomic landscape reveals tumor specific innate lymphoid cells associated with colorectal cancer progression. Cell. Rep. Med. 2(8), 100353. https://doi.org/10.1016/j.xcrm.2021.100353 (2021).
Vignali, D. A., Collison, L. W. & Workman, C. J. How regulatory T cells work. Nat. Rev. Immunol. 8(7), 523–532. https://doi.org/10.1038/nri2343 (2008).
Wing, K., & Sakaguchi, S. Regulatory T cells exert checks and balances on self tolerance and autoimmunity. Nat. Immunol. 11(1), 7–13. https://doi.org/10.1038/ni.1818 (2009).
Whiteside, T. L. What are regulatory T cells (Treg) regulating in cancer and why? Semin Cancer Biol. 22(4). https://doi.org/10.1016/j.semcancer.2012.03.004 (2012). 327 – 34.
Deng, Y. et al. CD122-selective IL-2 complexes treat ovarian carcinomas, induce Treg fragility and promote T cell stem cells. J. Immunother Cancer. 8, A729–A731. https://doi.org/10.1136/jitc-2020-sitc2020.0690 (2020).
Lucca, L. E. & Dominguez-Villar, M. Modulation of regulatory T cell function and stability by co-inhibitory receptors. Nat. Rev. Immunol. 20(11), 680–693. https://doi.org/10.1038/s41577-020-0296-3 (2020).
Moral, J. A. et al. ILC2s amplify PD-1 blockade by activating tissue-specific cancer immunity. Nature. 579(7797), 130–135. https://doi.org/10.1038/s41586-020-2015-4 (2020).
Barata, J. T., Durum, S. K. & Seddon, B. Flip the coin: IL-7 and IL-7R in health and disease. Nat. Immunol. 20(12), 1584–1593. https://doi.org/10.1038/s41590-019-0479-x (2019).
Kaech, S. M. et al. Selective expression of the interleukin 7 receptor identifies effector CD8 T cells that give rise to long-lived memory cells. Nat. Immunol. 4(12), 1191–1198. https://doi.org/10.1038/ni1009 (2003).
Silva, A. et al. IL-7 contributes to the progression of human T-cell acute lymphoblastic leukemias. Cancer Res. 71(14), 4780–4789. https://doi.org/10.1158/0008-5472.CAN-10-3606 (2011).
Krzystek-Korpacka, M. et al. Elevated systemic interleukin-7 in patients with colorectal cancer and individuals at high risk of cancer: association with lymph node involvement and tumor location in the right colon. Cancer Immunol. Immun. 66(2), 171–179. https://doi.org/10.1007/s00262-016-1933-3 (2016).
Seol, M. A. et al. Interleukin-7 contributes to the invasiveness of prostate cancer cells by promoting epithelial-mesenchymal transition. Sci. Rep. 9(1), 6917. https://doi.org/10.1038/s41598-019-43294-4 (2019).
Bennstein, S. B. & Uhrberg, M. Biology and therapeutic potential of human innate lymphoid cells. Febs J. 289(14), 3967–3981. https://doi.org/10.1111/febs.15866 (2021).
Akimoto, M. et al. Hypoxia induces downregulation of the tumor-suppressive sST2 in colorectal cancer cells via the HIF-nuclear IL-33-GATA3 pathway. Proc. Natl. Acad. Sci. USA. 120(18), e2218033120. https://doi.org/10.1073/pnas.2218033120 (2023).
Maric, J. et al. Prostaglandin E2 suppresses human group 2 innate lymphoid cell function. J. Allergy Clin. Immun. 141(5), 1761–1773. https://doi.org/10.1016/j.jaci.2017.09.050 (2017).
Ercolano, G., Falquet, M., Vanoni, G., Trabanelli, S. & Jandus, C. ILC2s: new actors in tumor immunity. Front. Immunol. 10, 2801. https://doi.org/10.3389/fimmu.2019.02801 (2019).
Ruf, B., Greten, T. F. & Korangy, F. Innate lymphoid cells and innate-like T cells in cancer - at the crossroads of innate and adaptive immunity. Nat. Rev. Cancer. 23(6), 351–371. https://doi.org/10.1038/s41568-023-00562-w (2023).
Blomberg, O. S. et al. IL-5-producing CD4 + T cells and eosinophils cooperate to enhance response to immune checkpoint blockade in breast cancer. Cancer Cell. 41(1), 106–123. https://doi.org/10.1016/j.ccell.2022.11.014 (2022).
Turnquist, H. R. et al. IL-33 expands suppressive CD11b + Gr-1(int) and regulatory T cells, including ST2L + Foxp3 + cells, and mediates regulatory T cell-dependent promotion of cardiac allograft survival. J. Immunol. 187(9), 4598–4610. https://doi.org/10.4049/jimmunol.1100519 (2011).
Liu, Q. et al. IL-33-mediated IL-13 secretion by ST2 + Tregs controls inflammation after lung injury. Jci Insight. 4(6). https://doi.org/10.1172/jci.insight.123919 (2019).
Halvorsen, E. C. et al. IL-33 increases ST2 + Tregs and promotes metastatic tumour growth in the lungs in an amphiregulin-dependent manner. Oncoimmunology. 8(2), 1527497. https://doi.org/10.1080/2162402X.2018.1527497 (2018).
Džopalić, T. et al. Effects of galectin-1 on immunomodulatory properties of human monocyte-derived dendritic cells. Growth Factors. 38(5–6), 235–246. https://doi.org/10.1080/08977194.2021.1947267 (2021).
Acknowledgements
We extend our gratitude to Ph.D. Quan Liu and Ph.D. Jie Liu for their invaluable support of this study. We acknowledge the Laboratory Animal Center for their exemplary care of the animals. We extend our appreciation to the Southern University of Science and Technology Core Research Facilities for their invaluable training and meticulous maintenance of the equipment.
Funding
This study was supported by the special fund of the basic research support program for outstanding young teachers in Heilongjiang Province (Grant No. YQJH2023032 to Xi Chen).
Author information
Authors and Affiliations
Contributions
Zhenchu Feng: Writing - review & editing, Writing - original draft, Data curation, Visualization. Ye Kuang: Writing - original draft, Formal analysis, Methodology. Yuan Qi: Writing - original draft, Investigation, Software. Xi Wang: Validation, Supervision. Peng Xu: Resources, Conceptualization. Xi Chen: Writing - review & editing, Funding acquisition, Project administration. All authors reviewed the manuscript.
Corresponding authors
Ethics declarations
Ethics approval
The animal study was approved by Institutional Animal Care and Use Committee of Southern University of Science and Technology. The study was conducted in accordance with the local legislation and institutional requirements.
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic Supplementary Material
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Feng, Z., Kuang, Y., Qi, Y. et al. Exogenous IL-33 promotes tumor immunity via macroscopic regulation of ILC2s. Sci Rep 14, 26140 (2024). https://doi.org/10.1038/s41598-024-77751-6
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41598-024-77751-6