Abstract
This study aims to evaluate the effectiveness of total hip arthroplasty (THA) with subtrochanteric femoral osteotomy in patients with Crowe type IV DDH in terms of functional outcomes, complication rates, and implant stability. The study was prospective, conducted in the University Clinical Center of Kosovo and Otrila Hospital from 2016 to 2022 and included 22 patients with Crowe type IV hip dysplasia who underwent the THA with a subtrochanteric femoral osteotomy procedure. The treatment was performed using the posterior approach, and the placement of the dual mobility acetabular cup was based on the anatomic hip center using a Quattro non-cemented endoprothesis. There were no reported hip dislocations, and all patients had a negative Trendelenburg sign at approximately 6 months post-surgery. Harris Hip Score (HHS) and Functional Independent Score (FIS) were significantly increased after the treatment (t = 21.342, p < 0.0001; and t = 83.331, p < 0.0001, respectively). The limb-length discrepancy decreased significantly after surgery (Mean = 0.7 cm) compared to pre-surgery (Mean = 3.5 cm) (p < 0.05). The study concludes that THA with subtrochanteric osteotomy is a safe and effective treatment option for Crowe type IV hip dysplasia. Using dual mobility acetabular components and compression in the osteotomy led to improved outcomes and faster recovery. It can restore the anatomic hip center and improve functional outcomes while reducing the risk of dislocation.
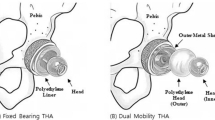
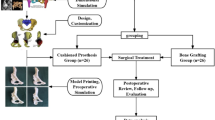
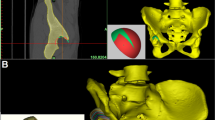
Similar content being viewed by others
Introduction
Crowe type IV Developmental Dysplasia of the Hip (DDH) is a severe form of hip dysplasia with a shallow acetabulum and a high degree of subluxation or dislocation. It causes excruciating pain, functional disability, and a low quality of life. Diagnosing Crowe Type IV DDH can be challenging and requires a comprehensive assessment involving clinical examination, radiographic imaging, and, laboratory investigations1,2.
Total hip arthroplasty (THA) is a widely accepted treatment option for patients with Crowe type IV DDH. THA is considered the best option for patients with Crowe type IV DDH who have failed conservative treatment or have severe hip joint degeneration3. However, achieving a stable, anatomic reduction in THA for Crowe Type IV DDH patients poses unique challenges due to the high risk of dislocation4.
Patients with Crowe type IV DDH who undergo THA are at a higher risk of complications compared to those with other forms of DDH or primary osteoarthritis5. Therefore, it is critical that these patients are managed by a skilled team that includes orthopedic surgeons, radiologists, and physical therapists to ensure comprehensive evaluation and treatment6.
Patients with high DDH have distinct and varied anatomical characteristics, with well-defined patterns observed in both the acetabulum and proximal femur. The acetabulum has deficits in the anterolateral and superior regions, resulting in challenges in achieving adequate bony coverage of the cup. Additionally, the proximal femur is hypoplastic with a limited intramedullary canal and increased anteversion. Muscles and soft tissues around the hip experience a reduction in length while the capsule becomes thicker7. The abductor insufficiency gives a Trendelenburg gait8. In cases where limb length exceeds 4 cm, the sciatic nerve becomes shorter and more susceptible to injury. In patients with hip dysplasia who have hip replacement, the occurrence of sciatic nerve palsy ranges from 0.8 to 13%9,10.
Due to these complexities, patients with severe osteoarthritis secondary to DDH often undergo total hip replacement (THR) at a younger age3,6,11. This kind of THA has been one of the most technically challenging procedures for orthopedic surgeons on both the femoral and acetabular sides because of severe anatomical abnormalities, especially in high-riding dislocations. Crowe Type IV developmental dysplasia of the hip (DDH), in particular, is among the most complex hip deformities to reconstruct12. Nevertheless, total hip arthroplasty (THA) has been shown to successfully reconstruct advanced DDH with a functional impairment that allows simultaneous shortening of the femur, correction of rotational abnormalities, and preservation of the proximal femoral metaphysic2,13. The main goal of Crowe IV DDH is to improve hip biomechanics and increase the subsequent survival rate of hip implants14. In Crowe IV DDH, THR is a challenging surgery, and the acetabulum is difficult to locate in these cases. Restoring the anatomical rotation center of the hip has been proven to yield good biomechanical results in THA for DDH patients.
Positioning the cup and reducing the hip joint are technically demanding steps that require precise techniques. This can be done by careful soft tissue dissection, capsule release from the proximal femur, the release of tight adductors and flexors, pi-crusting of abductors to gain length, and if needed, subtrochanteric shortening of the femur. Due to the altered anatomy in DDH, the femoral neurovascular bundle and sciatic nerve may not be found in their usual landmarks, necessitating particular caution15.
To overcome the contractures and reduce the hip without stretching the sciatic nerve, femoral shortening has been advocated as an adjunct to THR in Crowe Type IV DDH. To release the sciatic nerve, the piriformis muscle must be cut up to 5 cm on either side (curvature is reduced, the leg is extended more, and no paresthesia is experienced in the extremity). In such cases, cementless THR with a subtrochanteric femoral shortening osteotomy, rather than a proximal shortening osteotomy with distal advancement of the great trochanter to restore abductor muscle function, has been described as it avoids the risk of fibrous non-union of the great trochanter14.
The purpose of this study is to evaluate the effectiveness of total hip arthroplasty with subtrochanteric femoral osteotomy in patients with Crowe type IV DDH in terms of functional outcomes, complication rates, and implant stability.
Materials and methods
Study design
A prospective study was conducted at the University Clinical Center of Kosovo and Otrila Hospital between the months of January 2016 and December 2022. Twenty-two patients with Crowe type IV hip development dysplasia were included in our study (Subluxation > 100% or proximal dislocation > 20% of pelvic height)2,16.
Participants
22 patients (19 female and 3 male) underwent DM acetabular cup procedures, using a Quattro non-cemented endoprosthesis in all events.
Ethics approval
was obtained from the Faculty of Medicine “Fehmi Agani”, University of Gjakova ethics committee (Prot. no: 006/765). The procedures of this study complied fully with the provisions of the Declaration of Helsinki regarding Research on Human Participants, and all subjects provided informed consent prior to surgery. In all patients, preoperative planning was based on measurements taken from anteroposterior and oblique hip radiographs to determine the true acetabulum size and location. CT of the Pelvis was made; the purpose of this procedure was to determine the width of the femoral canal.
The inclusion criteria are: preoperative radiographic evidence of Crowe IV DDH, severe pain, accompanied by the abbreviation of the extremity, Unilateral Crowe IV, considerable difficulty in walking, low quality of life with functional impairment while performing life activities.
The exclusion criteria are: high dislocation of the hip secondary to septic arthritis, history of hip infections or tumors, Bilateral Crowe IV, patients less than 20 years of age, lumbar spine stiffness (lumbar spine lateral curve < 15°) or severe spinal deformity.
No patients had previously undergone proximal femoral or pelvic osteotomies.
The primary outcomes of this study include pre- and post-operative Harris Hip Score (HHS), Functional Independent Score (FIM), post-operative dislocation rate, the union of the osteotomized femoral subtrochanteric site, limb-length discrepancy (in cm), and Trendelenburg sign after surgery.
The amount of radiographic leg lengthening was calculated by the distance between the top of the greater trochanter preoperatively and one week postoperatively17. Osteolysis of the acetabulum and femur was assessed as previously described, as was measurement of radiolucent lines at the prosthesis-bone interface, as described by Gruen et al.18, and for the femur and acetabulum by DeLee and Charnley19. Femoral implant loosening and the stability of the femoral component was defined as bone-ingrown fixation, stable fibrous fixation, or unstable fixation according to Engh et al.20. Ectopic bone formation was evaluated according to the criteria described by Brooker et al.21.
Surgical procedures
All of the patients were treated using the posterior approach. The placement of the acetabular cup was based on the anatomic hip center. All patients received subtrochanteric osteotomies to shorten and derogate their femurs.
Subtrochanteric osteotomy can be performed in several ways, including transverse, oblique, double chevron (V-shaped), step-cut (Z-shaped), and sigmoid methods22,23,24. Among the subtrochanteric osteotomy types, transverse osteotomy has generally been favored due to its procedural simplicity, satisfactory clinical outcomes, and relatively high error tolerance. Step-cut and sigmoid osteotomies have been shown to provide greater rotational stability and bonier surface contact to support early bone tissue union than transverse osteotomies24. Nevertheless, further scientific evidence is required to substantiate the superior clinical outcomes of these osteotomies. The reduction can be maintained with a 3.5 mm compression plate. According to our experience, a wedge-shaped corrective osteotomy with apex (pressure) towards the medial part affects the formation of the callus faster.
THA used a Dual Mobility acetabular cup without cement in all cases, the non-cemented femoral component, and a femoral shortening osteotomy with a minimum follow-up of 6 months and records of patient-reported outcomes.
It was recorded whether there were any postoperative complications. A follow-up was performed on the 1st, 3rd, and 6th month after surgery.
Depending on the patient’s health, operations were performed under spinal or general anesthesia in the lateral decubitus position with a posterior approach to the hip. With the posterior approach, both the acetabulum and the femur are adequately visualized during the reconstructive procedure. After the skin incision, the fascia lata is incised over the gluteus maximus and the muscle is bluntly split into the short external rotators. This approach spares the abductors during surgical exposure of the acetabulum and femur. It also has the advantage of allowing stretchable exposure of the femur and acetabulum if needed.
The sciatic nerve is carefully protected as it pulls posteriorly to the short external rotators. After the piriformis is identified, the short external rotators and piriformis are anatomized at their attachment to the greater trochanter. They are then marked with a braided suture for identification, and we never repaired the sutured piriformis muscle after surgery. This exposes the posterior joint capsule, which is incised to expose the femoral neck and head.
Identification of the false acetabulum and the dysplastic true acetabulum was done after cutting and removing the femoral head and removing obscuring osteophytes. The true acetabulum was then debrided and reamed to expose healthy, bleeding bone in the required direction.
A dual-mobility acetabular cup was inserted with an anteversion of 10–25° and an inclination of 30–45° after the true acetabular cup was reamed. The extent of shortening was determined by moving the proximal part of the femur distally and osteotomizing the overlapping part of the distal femur. Each patient received a distally split and proximally HA -coated femoral stem (Group Lepine France).
In addition to the transection of the femoral neck and removal of the head, the femur was shortened to the correct size. The height of the transverse shortening osteotomy was set 1 cm distal to the lesser trochanter. A longitudinal marker was placed at the planned osteotomy site as a rotational reference for the femur (Fig. 1). The transverse osteotomy was then performed. A trial stem with a trial head was inserted into the proximal femur and provisionally reduced into the acetabulum. The distal femur was held with manual traction to establish the level for the second osteotomy. This was done to reduce the distal femur without excessive traction while reducing muscle tension and the position of the femur. The trial stem of the proximal femur was then reduced into the distal femoral segment. The most important factor in avoiding the nonunion of these fragments is the direction of the distal fragment osteotomy. This was performed so that the medial part remains in compression after fixation. Due to increased compression in the medial part of the site where the femur osteotomy was performed, we observed bone healing after the sixth month of follow-up as a result of the enhanced direction of the femoral osteotomy.
If the reduction of the hip joint is maintained after soft tissue decompression, resulting in leg lengthening of more than 4 cm, injury to the sciatic nerve may occur25. For this reason, we do not reattach the piriformis muscle. The curvature of the sciatic nerve through the piriformis muscle allows us to lengthen it in this manner.
To reduce traction forces on the sciatic nerve, the leg was positioned after surgery with the hip fully extended and the knee flexed. One day after surgery, the patient was able to walk with two crutches with partial weight bearing (15–20 kg).
Results
This study included 22 hips from 22 patients who underwent THR surgery and femoral shortening osteotomy for Crowe hip dysplasia type IV. Nineteen (86.3%) of the 22 patients were female, while three (13.6%) of them were male (Table 1). Fourteen out of the 22 patients had low back pain, and 16 out of 22 were overweight (BMI: 25.0–29.9 kg/m2). We had no dislocation of the hip after 6 months post surgery. The union of the osteotomized subtrochanteric femur site took about 3–5 months. Limb-length discrepancy decreased significantly after surgery (Mean = 0.7 cm) compared to pre surgery (Mean = 3.5 cm) (p < 0.05) (Fig. 2) (Table 2). Trendelenburg sign was negative in 100% of patients 6 months after surgery. Patients with femoral osteotomy were able to walk normally without assistance approximately 5 months after surgery.
HHS and FIS were significantly improved after the treatment (t = 21.342, p < 0.05; and t = 83.331, p < 0.05, respectively) (Table 2).
X-ray of the left femoral head: The sphericity of the left femoral head is irregular, the Shenton line is interrupted, more than 70% of the femoral head has fragmentation and signs of necrosis (A), X-ray after implantation of a total endoprosthesis (CROWE 4) with dual mobility component acetabular cup and a subtrochanteric osteotomy, which is more compressed in the medial part (B).
Discussion
Total hip arthroplasty (THA) is a common treatment for patients with Crowe type IV Developmental Dysplasia of the Hip (DDH). This study evaluates the efficacy of total hip arthroplasty along with subtrochanteric femoral osteotomy using a dual mobility acetabular cup procedure and a Quattro non-cemented endoprosthesis in patients with Crowe type IV developmental dysplasia of the hip. The key outcomes assessed include the dislocation rates, limb length correction, and osteotomy site union.
Crowe Type IV DDH presents significant challenges due to shorter and weaker abductor muscles increasing the risk of hip instability and abnormal gait post-surgery. Despite these challenges, our study reported no dislocations within six months post-surgery using the dual mobility acetabular cup and Quattro endoprosthesis. This contrasts with other studies conducted by Brooker et al., Sun et al., and Chen et al., that have reported high dislocation rates following THA in patients with Crowe type IV DDH, with rates ranging from 4 to 20%21,26,27.
Postoperative results showed an average limb length discrepancy reduction to 0.7 cm, and no positive Trendelenburg signs. Additionally, the Harris Hip Score (HHS) improved to an average of 89 points, and the Functional Independent Score (FIS) increased to 15.9 points after six months.
These findings are consistent with other studies, such as Guler et al., who observed similar HHS improvements using a press-fit cementless acetabular cup in overweight and obese patients28, and Hasegawa et al., who achieved comparable HHS scores in their study with a small cementless socket and posterolateral approach with the Crowe IV DDH patients in the lateral position. Additionally, Hasegawa et al. in their study had 2 hips (out of 20) with a positive Trendelenburg sign, and decreased the mean leg length discrepancy from 3.8 cm to 1.4 cm; however, they had a longer follow-up period29.
Achieving stable and anatomic hip reduction in Crowe Type IV DDH is difficult due to the shallow acetabulum and high degree of dislocation. Surgical techniques to address this include using larger diameter acetabular components, thicker acetabular liners, and the use of a constrained liner or cup30,31,32,33,34. Additionally, adequate placement of the patient on the operating table, the use of specialized instruments, and careful assessment of the position of the femoral component before final fixation are critical in establishing a stable and anatomical reduction and achieving better clinical outcomes35,36. Overall, THA for Crowe type IV DDH is a technically demanding procedure that requires a high level of surgical skill and experience.
Despite being technically demanding, THA for Crowe Type IV DDH can successfully restore the anatomic hip center, improve biomechanics, and enhance implant longevity. The use of dual mobility acetabular components reduces dislocation risk and supports early movement, while femoral osteotomy facilitates limb extension without nerve complications. However, challenges such as high dislocation rates and achieving stable reductions persist.
There are various limitations to this study. First of all, this study had a limited sample size. Which could not be expected due to the unpredictability of people seeking health care at the clinic. According to the G*power program, a sample size of 22 hips is considered statistically appropriate for analyzing data using the repeated measures t-test methodology. This analysis assumes an effect size of 0.8, a significance level (α) of 0.05, and a power (1-β) of 0.95. Second, we did not assess back pain or quality of life after surgery. Third, the follow-up evaluation was extended for up to six months. Other studies, however, have shown longer periods of follow-up for similar surgical treatments29. Further studies are needed to determine the long-term outcomes of total hip arthroplasty along with subtrochanteric femoral osteotomy using a dual mobility acetabular cup procedure and a Quattro non-cemented endoprosthesis for patients with Crowe type IV hip developmental dysplasia.
In conclusion, the total hip arthroplasty (THA) with subtrochanteric osteotomy for Crowe type IV hip dysplasia can restore the anatomic hip center and offer safe functional limb outcomes. The dual mobility acetabular component is a wise choice, because it offers a low dislocation risk, is biomechanically very compliant, and allows for early unsupported movement following surgery. In osteotomies with compression in the medial part, fragments fuse faster, resulting in faster walking without crutches. The cutting of the piriformis muscle and the release of the ischiatic nerve have enabled us to have the greatest possibility for extension of the extremity as well as not to have peroneal prolapse post-operatively. The use of a dual mobility acetabular component and compression in the medial part of the osteotomy can lead to faster recovery and better overall results, despite the inherent surgical challenges.
Data availability
The data that support the findings of this study are available from the corresponding author upon reasonable request.
References
Dezateux, C. & Rosendahl, K. Developmental dysplasia of the hip. Lancet 369, 1541–1552 (2007).
Crowe, J., Mani, V. & Ranawat, C. Total hip replacement in congenital dislocation and dysplasia of the hip. J. Bone Joint Surg. Am. Vol. 61, 15–23 (1979).
Harada, Y. et al. Anatomically designed prosthesis without cement for the treatment of osteoarthritis due to developmental dysplasia of the hip: 6-to 13-year follow-up study. J. Orthop. Sci. 12, 127–133 (2007).
Ding, Z. C. et al. Risk of dislocation after total hip arthroplasty in patients with Crowe Type IV Developmental Dysplasia of the hip. Orthop. Surg. 12, 589–600 (2020).
Zeng, W. N. et al. Total hip arthroplasty for patients with Crowe type IV developmental dysplasia of the hip: ten years results. Int. J. Surg. 42, 17–21 (2017).
Sochart, D. H. & Porter, M. L. The long-term results of Charnley low-friction arthroplasty in young patients who have congenital dislocation, degenerative osteoarthrosis, or rheumatoid arthritis. JBJS 79, 1599–1617 (1997).
Gustke, K. The dysplastic hip: not for the shallow surgeon. Bone Joint J. 95, 31–36 (2013).
Bailey, R., Selfe, J. & Richards, J. The role of the Trendelenburg Test in the examination of gait. Phys. Therapy Reviews. 14, 190–197 (2009).
Lewallen, D. G. Neurovascular injury associated with hip arthroplasty. Instr. Course Lect. 47, 275–283 (1998).
Lai, K. A., Shen, W. J., Huang, L. W. & Chen, M. Y. Cementless total hip arthroplasty and limb-length equalization in patients with unilateral Crowe type-IV hip dislocation. JBJS 87, 339–345 (2005).
Sochart, D. & Porter, M. The long term results of Charnley low-friction arthroplasty in patients with juvenile chronic rheumatoid arthritis. Hip Int. 10, 26–37 (2000).
Baz, A. B. et al. Treatment of high hip dislocation with a cementless stem combined with a shortening osteotomy. Arch. Orthop. Trauma Surg. 132, 1481–1486 (2012).
Karachalios, T. & Hartofilakidis, G. Congenital hip disease in adults: terminology, classification, pre-operative planning and management. J. Bone Joint Surg. Br. Volume. 92, 914–921 (2010).
Nagoya, S. et al. Cementless total hip replacement with subtrochanteric femoral shortening for severe developmental dysplasia of the hip. J. Bone Joint Surg. Br. Volume. 91, 1142–1147 (2009).
Jitesh Kumar, J., Agarwal, S. & Sharma, R. K. Total hip replacement in Crowe type IV dysplastic hips—average 5 year follow-up and literature review. Acta Orthop. Belg. 82, 539–548 (2016).
Hartofilakidis, G., Stamos, K. & Ioannidis, T. Low friction arthroplasty for old untreated congenital dislocation of the hip. J. Bone Joint Surg. Br. Volume. 70, 182–186 (1988).
Makita, H., Inaba, Y., Hirakawa, K. & Saito, T. Results on total hip arthroplasties with femoral shortening for Crowe’s group IV dislocated hips. J. Arthroplast. 22, 32–38 (2007).
Gruen, T. A., McNeice, G. M. & Amstutz, H. C. Modes of failure of cemented stem-type femoral components: a radiographic analysis of loosening. Clin. Orthop. Relat. Res. (1976–2007). 141, 17–27 (1979).
DeLee, J. G. & Charnley, J. Radiological demarcation of cemented sockets in total hip replacement. Clin. Orthop. Relat. Research®, 20–32 (1976).
ENGH, C. A., Massin, P. & SUTHERS, K. E. Roentgenographic assessment of the biologic fixation of porous-surfaced femoral components. Clin. Orthop. Relat. Res. (1976–2007). 257, 107–128 (1990).
Brooker, A. F., Bowerman, J. W., Robinson, R. A. & Riley, L. H. Jr Ectopic ossification following total hip replacement: incidence and a method of classification. Jbjs 55, 1629–1632 (1973).
Paavilainen, T., Hoikka, V. & Solonen, K. Cementless total replacement for severely dysplastic or dislocated hips. J. Bone Joint Surg. Br. Volume. 72, 205–211 (1990).
Çatma, M. F. et al. Femoral shortening osteotomy in total hip arthroplasty for severe dysplasia: a comparison of two fixation techniques. Int. Orthop. 40, 2271–2276 (2016).
Cascio, B. M., Thomas, K. A. & Wilson, S. C. A mechanical comparison and review of transverse, step-cut, and sigmoid osteotomies. Clin. Orthop. Relat. Research®. 411, 296–304 (2003).
Shi, X. et al. Total hip arthroplasty for Crowe type IV hip dysplasia: surgical techniques and postoperative complications. Orthop. Surg. 11, 966–973 (2019).
Sun, Q. C., Wang, X. H., Song, B. S., Zhu, F. B. & Yan, S. Total hip arthroplasty for crowe type IV developmental dysplasia of the hip with S-ROM prosthesis. Zhongguo Gu Shang = China J. Orthop. Traumatol. 26, 153–157 (2013).
Chen, M., Gittings, D. J., Yang, S. & Liu, X. Total hip arthroplasty for Crowe type IV developmental dysplasia of the hip using a titanium mesh cup and subtrochanteric femoral osteotomy. Iowa Orthop. J. 38, 191 (2018).
Güler, O., Öztürk, S., Özgezmez, F. T. & Çerçi, M. H. Comparison of supine and lateral decubitus positions for total hip arthroplasty with the direct lateral approach in overweight and obese patients. BioMed research international (2020). (2020).
Hasegawa, Y., Iwase, T., Kanoh, T., Seki, T. & Matsuoka, A. Total hip arthroplasty for Crowe type IV developmental dysplasia. J. Arthroplast. 27, 1629–1635 (2012).
Krych, A. J., Howard, J. L., Trousdale, R. T., Cabanela, M. E. & Berry, D. J. Total hip arthroplasty with shortening subtrochanteric osteotomy in Crowe type-IV developmental dysplasia. JBJS 91, 2213–2221 (2009).
Krych, A. J., Howard, J. L., Trousdale, R. T., Cabanela, M. E. & Berry, D. J. Total hip arthroplasty with shortening subtrochanteric osteotomy in Crowe type-IV developmental dysplasia: surgical technique. JBJS 92, 176–187 (2010).
Li, Y. et al. Equalisation of leg lengths in total hip arthroplasty for patients with Crowe type-IV developmental dysplasia of the hip: classification and management. bone Joint J. 99, 872–879 (2017).
Van Eecke, E., Vanbiervliet, J., Dauwe, J. & Mulier, M. Comparison of constrained acetabular components and dual mobility cups in revision total hip arthroplasty: a literature review. Hip Pelvis. 32, 59 (2020).
Alberton, G. M., High, W. A. & Morrey, B. F. Dislocation after revision total hip arthroplasty: an analysis of risk factors and treatment options. JBJS 84, 1788–1792 (2002).
Papalia, G. F. et al. The role of patient surgical positioning on hip arthroplasty component placement and clinical outcomes: a systematic re-view and meta-analysis. Orthop. Rev. 15 (2023).
Takada, R. et al. Supine versus lateral position for accurate positioning of acetabular cup in total hip arthroplasty using the modified Watson-Jones approach: a randomized single-blind controlled trial. Orthop. Traumatology: Surg. Res. 105, 915–922 (2019).
Acknowledgements
The authors would like to thank all the medical staff of the Clinic of Orthopedics of the University Clinical Center of Kosovo and Otrila Hospital for their support in conducting the present study.
Funding
There is no funding source.
Author information
Authors and Affiliations
Contributions
All the authors have contributed to the conception and design of the study, drafting the article or revising it, and approving the version to be submitted. Material preparation and data collection were performed by SU and DU. Data analysis and interpretation were performed by BT and SU. All the authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethics approval
Ethics approval was obtained from the Faculty of Medicine “Fehmi Agani”, University of Gjakova ethics committee (Prot. No: 006/765).
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Ukaj, S., Krasniqi, S., Ukaj, D. et al. Total hip arthroplasty for crowe type IV developmental dysplasia of the hip using a dual mobility acetabular cup. Sci Rep 15, 7982 (2025). https://doi.org/10.1038/s41598-024-81716-0
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41598-024-81716-0