Abstract
Serum protein electrophoresis can sometimes reveal polyclonal hypergammaglobulinemia. This electrophoretic abnormality can be caused by a variety of conditions and can be difficult to investigate. We sought to investigate screening practices in patients with hypergammaglobulinemia in order to establish diagnostic guidance strategies. We selected all patients with polyclonal hypergammaglobulinemia greater than or equal to 20 g/L over one year to identify the etiologies causing a significant increase in gammaglobulins in the absence of a monoclonal abnormality. We then selected patients who presented with this abnormality for the first time, with no known etiology. Clinical, medication, biological and imaging data were collected. In our study population with polyclonal hypergammaglobulinemia (n = 155), the main etiologies identified were infections (56%), autoimmune and autoinflammatory diseases (20%), liver diseases (18%) and hematological and non-hematological malignancies (6%). Once hypergammaglobulinemia was identified, the clinical examination provided diagnostic orientation but was not sufficient to make the diagnosis. The initial assessment must investigate the most common pathologies including analysis of liver function, viral status, the search for signs of intravascular haemolysis, inflammatory markers, and blood cell count. At the second time point (unless there were suggestive clinical signs at presentation), more specific biological and imaging analyses were required. Finally, we propose a diagnostic guideline for a current, rational and optimal medical practice to assist clinicians in the management of patients with hypergammaglobulinemia.
Similar content being viewed by others
Introduction
In normal serum, protein electrophoresis (SPE) yields a broad gamma fraction with Gaussian distribution due to the millions of plasma cell clones that secrete immunoglobulins (Ig) into the serum1. Polyclonal gammopathy is characterized by a broad diffuse increase of the gammaglobulin zone caused by one or more heavy chains and both kappa and lambda light chains2. Symmetric/Gaussian hypergammaglobulinemia is generally associated with elevated levels of IgG1, 2 or 3, or IgM. In contrast, hypergammaglobulinemia characterized by beta-gamma bridging is usually due to a polyclonal increase in IgA, often linked to liver disease, or IgG4, frequently associated with IgG4-related diseases (IgG4-RD)3. It is worth noting that a relatively high serum concentration of IgG4 may give rise to a focal band, irrespective of whether it is polyclonal or monoclonal IgG42. With the emergence of IgG4-RD4, awareness and correct interpretation of the specific electrophoretic migration of IgG4 are important. Interpretation of SPE is not obvious. However, it can have a significant diagnostic impact.
While the “French National Health Authority” codifies the indications for prescribing SPE to search for a monoclonal abnormality and outlines the steps to be taken if a monoclonal Ig is found5, the detection of polyclonal hypergammaglobulinemia does not give rise to any recommendations, either for interpretation or for prescribing additional tests. However, the situations described as requiring the prescription of a SPE to search for the presence of a monoclonal protein are numerous and often non-specific, and may lead to the discovery of a polyclonal abnormality: recurrent infections, non-traumatic bone pain without abnormalities on standard radiological examination, unexplained polyarthritis, adenopathies, splenomegaly, hemogram abnormalities without obvious cause (anemia, isolated lymphopenia or hyperlymphocytosis), etc.
Polyclonal hypergammaglobulinemia has a wide variety of causes: liver diseases such as chronic viral hepatitis, autoimmune diseases, infections6,7,8, also some rare pathologies such as Eosinophilic granulomatosis with polyangiitis formerly known as Churg-Strauss syndrome9 and Rosai-Dorfman-Destombes disease10,11. The detection of this electrophoretic characteristic may be part of the diagnostic criteria in some pathologies, such as Castleman disease12, autoimmune lymphoproliferative syndrome13.
There is no consensus γ-globulin threshold to define polyclonal hypergammaglobulinemia. Standards for γ-globulin levels vary depending on supplier data and laboratory standards. From a practical point of view, it is recommended to consider a moderate polyclonal increase in γ-globulins for values between 15 and 20 g/L. A value greater than or equal to 20 g/L can be defined as a significant polyclonal increase in γ-globulins, requiring a search for an etiology14. Given the multitude of pathologies leading to polyclonal hypergammaglobulinemia and the lack of consensus on a strategy for investigating this anomaly, we established a diagnostic aid algorithm based on a study of the patient population at the University Hospital of Bordeaux.
Methodology
Population of patients
Our study is monocentric, retrospective, cross-sectional and descriptive, including patients with a polyclonal hypergammaglobulinemia on SPE (CAPILLARYS 3 SYSTEM, SEBIA) greater than or equal to 20 g/L (Fig. 1) and excluding patients who received intravenous or subcutaneous polyclonal Ig in the prior month. Thus, the study population was determined by extracting SPE performed at the University Hospital of Bordeaux between January 2017 and January 2018 using the Laboratory Information Management System software: GLIMS (CLINISYS - MIPS) (n = 483). For all enrolled patients, demographic, clinical and paraclinical data were collected during their hospital stay in dedicated health records (DXCARE, DEDALUS France). We restricted ourselves to collecting data corresponding to the same day or the closest day (within a maximum of three days) of the performance of the SPE in these patients. We then selected patients who had undergone a primary diagnosis (n = 170) and whose disease had not yet been investigated.
Illustration of polyclonal hypergammaglobulinemia on SPE (CAPILLARYS 3 SYSTEM, SEBIA). (A) Beta-gamma bridging for a patient with ethylic cirrhosis, beta-2 globulin 5.6 g/L, gammaglobulin 23.4 g/L; (B) Gaussian gammaglobulin for a patient with autoimmune cirrhosis, beta-2 globulin 2.3 g/L, gammaglobulin 55.5 g/L. Normal values for beta-2 and gammaglobulins: 2.0–4.9 g/L and 6.0–15.0 g/L respectively.
The study was conducted in accordance with the Declaration of Helsinki. It complies with the framework for the protection of personal data and privacy provided for in Article 65 − 2 of the amended Data Protection Act and the General Regulation on the protection of personal data. The Institutional Ethics Committee (CHU Bordeaux, France) approved it. All methods were carried out in accordance with relevant guidelines and regulations, and informed consent was obtained from all subjects and/or their legal guardian(s).
Clinical and paraclinical data
We focused our exploratory work by selecting clinical data that allowed us to establish the patient’s situation (first visit, monitored patient), symptoms and chronic or hospitalized drug treatments. Biological data were selected on the basis of frequently prescribed general parameters and more specific parameters that may vary according to the pathologies found to cause polyclonal hypergammaglobulinemia, based on the etiological prevalence reported in the literature (viral serologies, liver tests, CRP, lactate dehydrogenase (LDH), autoimmunity test, β2-microglobulin (β2-m), angiotensin-converting enzyme (ACE), IgG4)6,15. Finally, the imaging data obtained during the patients’ hospitalization was recorded to highlight any abnormalities suggestive of specific pathologies.
We determined the distribution of etiologies causing polyclonal hypergammaglobulinemia and studied variations in several clinico-biological parameters to highlight diagnostic exploration profiles. The etiological classes were identified as Infections, Autoimmune and autoinflammatory diseases, Liver diseases, Hematological and non-hematological malignancies, pathologies of Mixed origin, Other classification and Undetermined origin. Given the low inclusion of patients in these latter classifications, the Mixed (n = 6), Undetermined (n = 8) and Other groups (n = 1) were excluded from the rest of the study.
Statistical analysis
Descriptive results were expressed as percentages for qualitative variables and means ± standard deviations for quantitative variables. IBM SPSS Statistic 25.0 software was used for statistical analysis. The Kolmogorov-Smirnov test was used to determine that the variables studied did not follow a normal distribution. As a result, non-parametric tests were performed. The Kruskal-Wallis H test was used for group comparisons and the Mann-Whitney U test for within-group comparisons. Statistical significance was accepted at p < 0.05.
Results
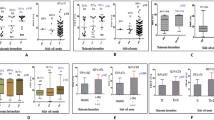
Figure 2 shows the repartition of etiologies among hypergammaglobulinemia detected in our study patients (n = 155). Infectious diseases were the most common etiology, followed by autoimmune and autoinflammatory diseases, liver, then hematological and non-hematological malignancies. Infections (n = 86) were dominated by bacterial etiologies (n = 59, 68.6%) mainly represented by sepsis, spondylodiscitis, tuberculosis, while viral infections were less frequent (n = 14, 16.3%) and mainly represented by acute HAV hepatitis, primary HIV infection. Autoimmune and autoinflammatory diseases (n = 31) were very heterogenous, mainly immunological thrombocytopenic purpura (n = 5, 16.1%), vasculitis (n = 3, 9.7%), sarcoidosis (n = 3, 9.7%), systemic lupus erythematosus, Sjögren syndrome, ankylosing spondylitis. Liver diseases (n = 28) were mainly represented by alcoholic cirrhosis (n = 10, 35.7%). Hematological and non-hematological malignancies (n = 10) included myelodysplastic syndrome (n = 3, 30%), carcinoma (n = 3, 30%), lymphoma (n = 2, 20%) and acute myeloid leukemia (n = 2, 20%).
Table 1 shows the distribution of gammaglobulin levels between the different etiologies, which did not differ significantly (p > 0.05). The mean values were between 23.6 and 26.4 g/L and the max values between 34.2 and 55.9 g/L, showing a great impact of the pathologies on the gammaglobulin production.
Table 2 summarises the results of liver parameters, LDH and CRP assay. Liver tests were widely prescribed in all etiological classes. The overall results showed an average prevalence of cytolysis, cholestasis, and jaundice. As expected, these disorders were more frequently found in liver diseases. In autoimmune and autoinflammatory diseases, and hematological and non-hematological malignancies, these tests have been performed to check the integrity of liver function before treatment and during follow-up16,17,18,19,20. Bilirubin measurement is also recommended in hematological and non-hematological malignancies to monitor the intravascular haemolysis that may occur with some treatments21.
In our population, LDH was frequently elevated in liver diseases, infections, and hematological and non-hematological malignancies. Because LDH is so ubiquitous in cells, the practical roles played by this enzyme are numerous. LDH can be increased in many phenomena such as intravascular hemolytic anemia, hepatic cytolysis, proliferation of a tumour mass, tumour lysis syndrome22. Therefore, recommendations for prescribing this parameter are rare. In autoimmune and autoinflammatory diseases, the only one is for the diagnosis of autoimmune hemolytic anemia23. Prescriptions for LDH testing in liver disease do not appear to follow any recommendation, either for diagnosis or for initiation or monitoring of drug therapy. Because of the hepatocyte tropism of LDH, it can be used in practice to assess liver damage, which explains the high positivity of the tests (62.5%) in this part of our population24. Finally, in the field of infections, LDH tests have been reported to be useful for some practical purposes: to assess liver damage or for the differential diagnosis of lymphoma in the presence of suggestive clinical findings (persistent fever, adenopathy) in cases of primary EBV or CMV infection25.
C-reactive protein (CRP) measurement was performed in almost 90% of baseline tests. The results indicated that CRP was elevated in 83.9% of investigations. It appears that CRP levels were higher in infectious diseases (80.2 ± 70.8 mg/L) and hematological and non-hematological malignancies (63 ± 80.9 mg/L) than in other diagnostic categories. Conversely, autoimmune and autoinflammatory diseases, and liver diseases appeared to be less inflammatory (24.8 ± 39.9 mg/L and 23.5 ± 29.1 mg/L, respectively).
Other parameters were analysed (data not shown). The study of viral serology prescriptions revealed that a few viruses can be grouped together in the same panel because they are frequently included in the same work-up: HIV, chronic and acute hepatitis viruses. A total of 113 serologies (72.9%) were performed. In detail, 90.3% of the tests included at least one serology related to HIV, HBV, HCV, HAV and/or HEV. The prescription of these serologies appeared to be of even greater importance when one considers that this panel was involved in 77.8% of diagnosed active viral infections, representing 14 out of a total of 18 infections.
A total of 78 autoimmunity tests were conducted. The screening for antinuclear antibodies (ANA) was positive in 59% of tests and anti-hepatocyte autoantibodies in 53% of tests. However, only a few targets were identified meaning a considerable number of tests were prescribed for various pathologies not related to immune damage.
A limited number of β2-m assays was prescribed. It increased in 84.2% of tests. β2-m can be used for many applications such as multiple myeloma prognosis, therapeutic monitoring of HIV infections, prognostic marker for lymphoma progression in Sjögren syndrome26,27,28. On the other hand, no recommendations have been identified for the interpretation of β2-m in liver diseases. From an analytical perspective, serum levels of this protein are sensitive to renal failure and inflammation, making it difficult to interpret this marker in pathologies leading to these organic disorders. A total of 13 prescriptions for ACE assays were observed. The pathologies associated with elevated ACE levels are primarily sarcoidosis and tuberculosis. This enzyme is used as a prognostic marker and for therapeutic follow-up in sarcoidosis29. This marker presents a moderate sensitivity diagnostic strength (50–75%) thus moderating its contribution as a diagnostic test30. Moreover, the specificity of this enzyme is not absolute in sarcoidosis, as elevated ACE levels may be found in a variety of other conditions (granulomatosis, primary biliary cholangitis, cholestasis, renal failure, hyperthyroidism). No specific results were identified on the basis of CBC (Complete Blood Count) tests. Only 4 patients had IgG4 tested in our population. Serum IgG4 levels, evaluated by immunonephelemetry and expressed as mean ± SD as other Ig, were not elevated: IgG4 = 0.5 ± 0.2 g/L (laboratory standards: 0.072–0.642 g/L). In the meantime, serum levels of the other IgG subclasses (IgG1, 2, 3) all increased in these patients: IgG1 = 12.5 ± 1.9 g/L (laboratory standards: 4.559–8.750 g/L); IgG2 = 7.1 ± 0.7 g/L (laboratory standards: 1.889–4.586 g/L); IgG3 = 1.8 ± 0.5 g/L (laboratory standards: 0.200–0.908 g/L). Apart from biological tests, 81 medical imaging studies were conducted. The objective was to identify the imaging techniques that provided a significant diagnostic advance, as they revealed an organic abnormality suggestive of the pathology. Forty-eight imaging contributed to the diagnosis, mostly in liver diseases. Signs suggestive of autoimmune and infectious diseases were less obvious, with a lesser contribution from imaging. Conversely, few imaging techniques have been used in the context of hematological and non-hematological malignancies in our population. The abnormalities identified on imaging are predominantly hepatosplenomegaly, hepatic dysmorphia, multiple cervical or mediastinal adenopathies, pulmonary or hepatic nodules, abscesses, ground-glass lung opacities, and signs of bone hypermetabolism.
Suggested diagnostic work-up
Based on these etiological, biological and imaging findings, we propose a diagnostic algorithm when polyclonal hypergammaglobulinemia is discovered (Figure 3). In addition, our results seem to show an over-prescription of some biological tests, especially autoimmune and β2-m explorations. With this suggested approach, a more rational way of prescribing biological tests could be adopted to optimize patient care: less risk of misinterpretation, more efficient costs.
Discussion
The present study was based on an analysis of the etiological distribution of pathologies inducing significant polyclonal hypergammaglobulinemia (≥ 20 g/L) and the determination of the involvement of clinical and paraclinical parameters in establishing the diagnosis. The main result of our study was to propose a decision-making algorithm for the prescription of complementary biological and medical imaging examinations to help the diagnostic approach. To date, few studies have provided guidelines for the investigation of polyclonal hypergammaglobulinemia3,11,31.The first question was about the target value of gammaglobulins (≥ 20 g/L) from which we wanted to propose a decision-making algorithm. The 20 g/L threshold was selected in order to eliminate ethnic factors32, ensure sufficient population inclusion for the study, and avoid the exclusion of potential etiologies. Dispenzieri A et al.6. and Simon N et al.15. selected higher thresholds, 30 and 25 g/L respectively. As a result, the proportion of the different main etiologies differed. In these two respective studies compared to ours, liver diseases represented 54 and 46.5% vs. 18%, autoimmune and autoinflammatory diseases 22 and 15.5% vs. 20%, infections 6 and 22.5% vs. 56%, hematological and non-hematological malignancies 5 and 8.9% vs. 6%. The main difference is the inversion of the proportions between the representativeness of liver diseases and infections. This may also be due to recruitment bias. Indeed, in our monocentric study, 25% of the patients came from internal medicine, 17% from infectious disease department, 13% from emergencies, 6% from hepatogastroenterology, the others at a rate less than or equal to 5% from various clinical services (data not shown). No mention of the type of clinical services was reported in these other studies6,15. Finally, a recent study led by Baillou et al. in three French hospital centers defined the threshold for polyclonal hypergammaglobulinemia on the 95th percentile at around 19 g/L, the lowest one at 16.8 g/L and the highest one at 22.2 g/L33, nevertheless without including other biological or clinical characteristics. However, their approach reinforced the choice of the cut-off of 20 g/L in our study.
Overall, our results allowed us to establish the place of the different clinical and biological tests in the diagnostic exploration and to establish an algorithm to help clinicians. This algorithm can be applied to any exploration of polyclonal hypergammaglobulinemia as our findings apply to all levels of gammaglobulin. Whether or not mild polyclonal hypergammaglobulinemia warrants further investigation is left to the discretion of the individual clinician. A complete hepatic blood test, including aminotransferases, γ-GT, alkaline phosphatase and bilirubin, is essential in the etiological search for significant polyclonal hypergammaglobulinemia. As evidenced by our findings, an impaired liver function will typically lead the clinician towards liver disease or, alternatively, infection. In the other hand, LDH is of particular interest in assessing tumour proliferation22. When combined with a hepatic test and a haptoglobin assay (a collapsed haptoglobin indicates intravascular haemolysis), an isolated increase would be indicative of a hematological or non-hematological malignancy. In this context, it is a marker that should be prescribed in the first instance. If transaminases are elevated in parallel with LDH, the clinician should be more inclined towards liver diseases, given the prevalence of the etiologies we highlighted, without formally ruling out a hematological or non-hematological etiology. To support our reasoning, in our population of cancer patients, we observed an elevation of LDH without any associated cytolysis.Viral infections, whether acute or chronic, play an important role in the etiology of polyclonal hypergammaglobulinemia. As such, the prescription of viral serologies is an essential part of the investigative work-up. In our population, we showed that the main agents found in viral infections are HIV, HBV, HCV, and HAV. The prescription panel comprising HIV and hepatotropic viruses was sufficient to cover 75% of diagnosed active viral infections. Since 10.6% of patients in the study were infected with one of these viruses (n = 18), this panel should be part of the first-line test for patients with polyclonal hypergammaglobulinemia. Other viruses (EBV, CMV, parvovirus B19, etc.) should be specifically investigated as second-line tests, depending on the patient’s clinical situation34. CRP is a robust indicator of inflammation, yet it lacks the specificity to serve as a diagnostic tool. In our study, all the pathologies under investigation exhibited elevated CRP levels, indicating a proinflammatory state. CRP is a highly sensitive marker, but its specificity is limited by the influence of various factors, including the reduction of levels by anti-inflammatory drugs, liver failure, … It is therefore only one factor contributing to the diagnostic process. A markedly elevated CRP may support an infectious hypothesis or a disease with an inflammatory component (e.g., aggressive lymphoma). Conversely, a low CRP level in the absence of any concurrent event may indicate liver disease (such as cirrhosis or primary biliary cholangitis) or autoimmune and autoinflammatory disease3. Consequently, it would be wise to interpret low CRP levels as indicating the absence of infectious and inflammatory pathologies, while high CRP levels do not appear to provide a definitive indication of the underlying etiology.There is a widespread tendency to prescribe autoimmunity tests for the patients in our study. However, establishing autoimmune status is not recommended as part of a patient’s initial test. The diagnosis of autoimmune diseases is based on a combination of clinical and biological signs. The presence of autoantibodies, which are both actors and markers of autoimmune disease, corroborates the diagnosis when the clinical picture is typical, or at least guides it when it is atypical. In practice, ANA testing should be carried out when the patient’s clinical picture is particularly suggestive of Sjögren syndrome, inflammatory muscle disease, scleroderma, mixed connective tissue disease or autoimmune hepatitis35. Screening for ANA will therefore be carried out as a second intention. The search for autoantibodies of autoimmune liver diseases can also be carried out as a second intention when the etiological causes of the most common liver diseases have been ruled out (viruses, alcohol, or even drugs). β2-m plays an important role in the assessment of tumor burden, making it a highly useful marker in the diagnosis and prognosis of hematological and non-hematological malignancies. It should therefore be prescribed in cases of suspicion of these pathologies. ACE was showed to be a low sensitivity marker, with many situations affecting serum ACE levels. Thus, it should not be measured as a first-line indicator of polyclonal hypergammaglobulinemia, but only when there is a strong suspicion of sarcoidosis.
The CBC is an integral part of the standard analysis for any patient. Its interest is more particular in the demonstration of anemia (hemolytic autoimmune? ), or hyperleukocytosis/hyperlymphocytosis with atypical cells (blasts, atypical lymphocytes, etc.), or even cytopenias.Finally, despite the interest of IgG436, our study population had no patients with IgG4-RD and very few prescriptions for this IgG isotype. Our immunological laboratory is very restrictive for the IgG subclass testing. We need to justify the context of the prescription (immunodeficiency or any suggestive symptoms of Ig4-RD) to obtain the analysis. In the main time, we restricted the data collection to the same day or the closest day (within a maximum of three days) of the performance of the SPE. Many patients were issued from the emergency department or other units that are not familiar with this prescription and not aware of the prevalence of IgG4-RD. This could explain the underestimated rate of IgG4-RD in our study. By referring to the literature, it is highlighted that it is an underestimated pathology, whose warning signs are polymorphic (damages to pancreas, bile ducts, salivary glands, …). The determination of IgG subclasses will be a major diagnostic orientation to label this pathology and should be performed as a first-line test for this type of clinical abnormality. In the literature, the guidelines developed by Zhao et al. were mainly based on IgG subclasses and CRP3. This approach comes from a center where IgG subclasses have been extensively studied, as IgG4-RD is an important investigative pathology for this center. As IgG subclasses tests are restrictive in our hospital, our study therefore focused on other parameters and provided new insights into the investigation of polyclonal hypergammaglobulinemia. Besides biological tests, medical imaging could provide important information necessary for diagnosis in all the pathologies reported in our study. The signs found on imaging are never specific to a pathology but they are diagnostic indications: hepatic dysmorphia, hepatosplenomegaly, lymphadenopathy, etc. These examinations require time and organization, and should only be carried out in the presence of clinical signs already pointing to organic damage: suspected deep-seated infection, lymphadenopathy, etc….
Conclusion
Polyclonal hypergammaglobulinemia, mainly at a rate greater than or equal to 20 g/L, should be investigated because of the clinical importance of the pathologies underlying this electrophoretic abnormality, which may require immediate treatment. A clinical examination may provide some clues but is not sufficient to establish the diagnosis. There are many etiologies, and the clinical manifestations are sometimes confused and non-specific, requiring further investigation. We propose a diagnostic aid algorithm based on clinical and biological data from a large population of patients.
Data availability
The datasets used and/or analysed during the current study available from the corresponding author on reasonable request.
References
Turner, K. A. et al. An international multi-center serum protein electrophoresis accuracy and M-protein isotyping study. Part I: factors impacting limit of quantitation of serum protein electrophoresis. Clin. Chem. Lab. Med. (CCLM). 58 (4), 533–546 (2020).
Jacobs, J. F. M., Van Der Molen, R. G. & Keren, D. F. Relatively restricted Migration of polyclonal IgG4 may mimic a monoclonal gammopathy in IgG4-Related disease. Am. J. Clin. Pathol. 142 (1), 76–81 (2014).
Zhao, E. J., Cheng, C. V., Mattman, A. & Chen, L. Y. C. Polyclonal hypergammaglobulinaemia: assessment, clinical interpretation, and management. Lancet Haematol. 8 (5), e365–e375 (2021).
Zhao, E. J., Carruthers, M. N., Li, C. H., Mattman, A. & Chen, L. Y. C. Conditions associated with polyclonal hypergammaglobulinemia in the IgG4-related disease era: a retrospective study from a hematology tertiary care center. Haematologica 105 (3), e121–e123 (2020).
Muriel, D. Quand prescrire une électrophorèse des protéines sériques (EPS) et conduite à tenir en cas d’une immunoglobuline monoclonale. Fiche mémo, HAS. (2017).
Dispenzieri, A., Gertz, M. A., Therneau, T. M. & Kyle, R. A. Retrospective cohort study of 148 patients with polyclonal gammopathy. Mayo Clinic Proceedings. ;76(5):476–87. (2001).
Paricaud, K., Moulis, G., Combis, M. S., Sailler, L. & Arlet, P. Causes of protidemia above 100 g/L. Eur. J. Intern. Med. 25 (10), e123 (2014).
Beuvon, C., Martin, M., Baillou, C., Roblot, P. & Puyade, M. Etiologies of polyclonal hypergammaglobulinemia: a scoping review. Eur. J. Intern. Med. 90, 119–121 (2021).
Vaglio, A. et al. IgG4 immune response in Churg–Strauss syndrome. Ann. Rheum. Dis. 71 (3), 390–393 (2012).
Henrie, R. et al. Inflammatory diseases in hematology: a review. Am. J. Physiology-Cell Physiol. 323 (4), C1121–C1136 (2022).
Zhao, E. J., Gauiran, D. T. V., Slack, G. W., Dutz, J. P. & Chen, L. Y. C. A 54-Year-old woman with cutaneous nodules. NEJM Evid. 1 (5), EVIDmr2200035 (2022).
Fajgenbaum, D. C. et al. International, evidence-based consensus diagnostic criteria for HHV-8–negative/idiopathic multicentric Castleman disease. Blood 129 (12), 1646–1657 (2017).
Rao, V. K. & Oliveira, J. B. How I treat autoimmune lymphoproliferative syndrome. Blood 118 (22), 5741–5751 (2011).
Szymanowicz, A. et al. [A proposal of ready-made interpretative comments applicable to serum protein electrophoresis]. Ann. Biol. Clin. (Paris). 64 (4), 367–380 (2006).
Simon, N., Bouillet, L. & Deroux, A. Étiologies Des hypergammaglobulinémies polyclonales dans un CHU. La. Revue De Médecine Interne. 38, A133–A134 (2017).
Larrey, D. Hépatotoxicité Des immunosuppresseurs. Conduite diagnostique. Gastroentérologie Clinique et Biol. 32 (5), S194–204 (2008).
De Martin, E., Michot, J. M., Rosmorduc, O., Guettier, C. & Samuel, D. Liver toxicity as a limiting factor to the increasing use of immune checkpoint inhibitors. JHEP Rep. 2 (6), 100170 (2020).
Rhyner, G. Revue Médicale Suisse: Hépatotoxicité médicamenteuse due aux antibiotiques. Zahedi K, editor. Revue Médicale Suisse. ;6(271):2180–7. (2010).
Ramadori, G. & Cameron, S. Effects of systemic chemotherapy on the liver. Ann. Hepatol. 9 (2), 133–143 (2010).
Dominique, L. Liver toxicity of TNFα antagonists. Joint Bone Spine. 75 (6), 636–638 (2008).
Anastasiou, M. Revue Médicale Suisse: Anémie hémolytique dans le contexte de cancer. Chalandon Y, editor. Revue Médicale Suisse. ;14(607):1021–7. (2018).
Forkasiewicz, A. et al. The usefulness of lactate dehydrogenase measurements in current oncological practice. Cell. Mol. Biol. Lett. 25 (1), 35 (2020).
Lauda-Maillen, M. et al. Diagnostic et prise en charge de l’anémie hémolytique auto-immune à L’exclusion Des formes secondaires à une cause néoplasique. Adéquation de la prise en charge Au PNDS Octobre 2009. La. Revue De Médecine Interne. 38 (10), 648–655 (2017).
Kotoh, K. et al. Lactate dehydrogenase production in hepatocytes is increased at an early stage of acute liver failure. Experimental Therapeutic Med. 2 (2), 195–199 (2011).
Qiu, L. et al. A retrospective analysis of EBV-DNA status with the prognosis of lymphoma. J. Cell. Mol. Medi. 26 (20), 5195–5201 (2022).
Kim, H. A., Jeon, J. Y., Yoon, J. M. & Suh, C. H. Beta2-Microglobulin can be a disease activity marker in systemic Lupus Erythematosus. Am. J. Med. Sci. 339 (4), 337–340 (2010).
Bongi, S. M., Campana, G., D’agata, A., Palermo, C. & Bianucci, G. The diagnosis value of β2-microglobulin and immunoglobulins in primary Sjögren’s syndrome. Clin. Rheumatol. 14 (2), 151–156 (1995).
Bergoin, C., Lamblin, C. & Wallaert, B. Manifestations biologiques Au cours de la sarcoïdose. Ann. Med. Interne. 152, 34–38 (2001).
Baudin, B. L’enzyme de conversion de L’angiotensine I (ECA) dans le diagnostic de la sarcoïdose. Pathol. Biol. (Paris). 53 (3), 183–188 (2005).
Finger, R., Rodrigues, R., Schönegg, R., Kluckert, T. & Brutsche, M. Sarcoïdose: aperçu clinique. Forum Med Suisse [Internet]. Mar 27 [cited 2023 Jun 17];13(1314). (2013). https://doi.emh.ch/fms.2013.01470
Chen, L. Y. C. et al. Case 30-2024: A 45-Year-Old Woman with Kidney Lesions and Lytic Bone Disease. Cabot RC, Rosenberg ES, Dudzinski DM, Baggett MV, Tran KM, Sgroi DC, editors. N Engl J Med. ;391(12):1140–51. (2024).
Buadi, F. et al. High prevalence of polyclonal hypergamma-globulinemia in adult males in Ghana, Africa. Am. J. Hematol. 86 (7), 554–558 (2011).
Baillou, C. et al. Polyclonal hypergammaglobulinaemia: towards definition of a threshold. Postgrad. Med. J. 99 (1170), 296–301 (2023).
Nomura, K. et al. Autoimmune lymphoproliferative syndrome mimicking chronic active Epstein–Barr virus infection. Int. J. Hematol. 93 (6), 760–764 (2011).
Pasquali, J. L. & Goetz, J. Que faire en présence d’anticorps antinucléaires chez l’adulte ? In: Lupus érythémateux [Internet]. Elsevier; 2013 [cited 2023 Jun 18]. pp. 103–8. https://linkinghub.elsevier.com/retrieve/pii/B9782294714474500131
Chen, L. Y. C., Mattman, A., Seidman, M. A. & Carruthers, M. N. IgG4-related disease: what a hematologist needs to know. Haematologica 104 (3), 444–455 (2019).
Author information
Authors and Affiliations
Contributions
M.A wrote the main manuscript text, prepared tables and figures. A.C and A.B contributed to the analysis, interpretation of data and reviewed the manuscript.All the authors approved the submitted version.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
ANDRE, M., CONTIS, A. & BERARD, A.M. Etiological study of polyclonal hypergammaglobulinemia in a French cohort of hospitalized patients and proposal of a diagnostic aid algorithm. Sci Rep 14, 31282 (2024). https://doi.org/10.1038/s41598-024-82735-7
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41598-024-82735-7