Abstract
Esophageal adenocarcinoma (EAC) has increased substantially to become the most common type of esophageal cancer in the United States, surpassing esophageal squamous cell carcinoma (ESCC). Whether the increasing incidence of EAC is linked to trends in esophageal cancer mortality is unclear. We analyzed esophageal cancer data from the Surveillance, Epidemiology, and End Results-12 cancer registry program, using Joinpoint regression for trend analysis and a decomposition method to attribute changes to population growth, population aging, and epidemiological changes. Age–period–cohort models were employed to estimate incidence and mortality through 2044. Between 1992 and 2019, 39,700 individuals were diagnosed with esophageal cancer, and 35,259 deaths were recorded from 1993 to 2019. The overall incidence of esophageal cancer declined [average annual percent change (AAPC), − 0.7%], but the incidence of EAC increased by an AAPC of 1.6% per year (P < 0.001) from 1992 to 2019. The overall mortality rates decreased by an annual percentage change of 1.0% [95% confidence intervals − 1.2% to − 0.7%] from 1998 to 2019, primarily related to decline in ESCC in 1996–2019. The mortality of EAC increased by an AAPC of 2.2% per year (P < 0.001) over the study period and increased for all demographic characteristic groups. Population aging and growth largely explain the increase in esophageal cancer over the last 3 decades. Future projections (2019–2044) suggest a 31% increase in incidence and deaths, with EAC rates continuing to rise (AAPC, 0.25; 95% CI 0.23–0.28). The number of esophageal cancer cases and deaths have significantly increased and projections indicate that this trend will continue. Effective measures must be taken to address the burden of esophageal cancer.
Similar content being viewed by others
Introduction
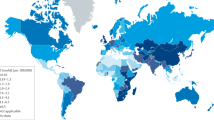
Esophageal cancer is the 11th most commonly diagnosed cancer and the seventh leading cause of cancer death in 2022, representing 4.6% of the total cancer deaths worldwide1. The burden of esophageal cancer demonstrates substantial regional and demographic disparities. For instance, many Asian, South American, and North American countries have shown declining trends, while some European regions, especially those with aging populations, experience stable or increasing rates2. Despite a reduction in overall esophageal cancer incidence and mortality rates in the United States, the disease remains a significant public health challenge, with an estimated 22,370 new cases and 16,130 deaths projected in 20243. Historically, esophageal squamous cell carcinoma (ESCC) was the predominant subtype, but its incidence has declined significantly due to public health interventions and lifestyle modifications4,5,6,7. In contrast, esophageal adenocarcinoma (EAC) incidence has shown an upward trend, surpassing ESCC around 1997 to become the predominant subtype of esophageal cancer8. However, while recent research suggests a stabilization in EAC incidence, particularly among cohorts born after 1955, the trajectory of EAC mortality remains ambiguous9.
The unique epidemiological trends of esophageal cancer in the United States are influenced by genetic, environmental, and lifestyle factors, resulting in distinct distributions across demographic groups and tumor subtypes. The divergent trends between ESCC and EAC, coupled with the evolving demographic landscape, underline the imperative for detailed epidemiological analyses to direct precision prevention and treatment efforts for high-risk groups. With rising obesity rates and the growing aging population, the burden of esophageal cancer is likely to intensify, highlighting the necessity for predictive analyses to foresee future incidence and mortality patterns10,11. Furthermore, cancer incidence and mortality are interconnected, with increases in the former often portending rises in the latter. Most previous studies have examined esophageal cancer incidence and mortality independently, and integrating the two in the analysis helps focus attention on solutions to the combined challenge and allows policymakers to recognize the importance of prioritizing upstream solutions.
Thus, the study aims to: (1) describe the trends in incidence and incidence-based mortality of esophageal cancer within U.S. populations, considering demographics and tumor characteristics; (2) decompose the changes in terms of population growth, aging, and epidemiological shifts; and (3) project the incidence and incidence-based mortality through 2044.
Methods
This study was analyzed from March 1, 2022 to June 1, 2023 and followed the strengthening the reporting of observational studies in epidemiology (STROBE) reporting guideline. The Institutional Review Board of Shantou University School of Medicine deemed the research exempt due to the use of public data, waiving informed consent requirements.
Data sources
Esophageal cancer incidence file during 1992–2019 and incidence-based mortality file during 1993–2019 were obtained from Surveillance, Epidemiology, and End Results–12 (SEER-12) registry, a database that includes data from 12 high-quality, population-based registries representing approximately 12.2% of the U.S. population12. The SEER program of the National Cancer Institute (NCI) provides information on cancer statistics, including patient demographics, tumor characteristics, treatment, and vital status from population-based cancer-registries12. To ensure that most deaths in the incidence-based mortality analysis occurred in patients diagnosed with esophageal cancer after 1992, we excluded the year 1992, in line with the median survival of proximal esophageal cancer (8 months)13,14. Incidence-based mortality, superior to mortality data, includes information on disease onset and can be examined by variables recorded at diagnosis. Cases were augmented with demographic, tumor features, and diagnostic details. U.S. population projections for 2020–2044 were obtained from the International Database web tool programmed by the US Census Bureau15, adjusted for the 12.2% ratio of SEER-12.
Characteristics
Diagnoses were confirmed microscopically according to the International Classification of Oncological Diseases (ICD-O) Third Revision, EAC (codes 8140-8573), EAC site (codes 8050-8082). Analyzed demographic variables included sex, age at diagnosis (< 60, 60–69 and 70+ years) and race (black, white, American Indian and Asian or Pacific Islander). This information was originally abstracted from medical records and submitted to regional or state cancer registries. Cancer staging was categorized by SEER historical stage A (1973–2015) (used from 1992 to 2015) and combined summary stage (2004+) (used from 2016 to 2019), encompassing localized (limited to esophageal cancer), regional (involving tumour spread beyond regional lymph nodes) and distant (indicating tumour metastasis).
Statistical analysis
For each SEER case of esophageal cancer, we selected only the first matching record and microscopically confirmed cases, and excluded cases that were reported only from autopsy records or death certificates. Age-standardized incidence and incidence-based mortality rates (per 100,000 person-years) and 95% CIs were calculated using SEER*Stat, adjusted to the 2000 U.S. standard population16.
To quantify trends and assess changes in incidence and mortality, we used the NCI’s Joinpoint regression program (version 4.9.1.0) to calculate annual percentage change (APC), average annual percentage change (AAPC), and 95% CIs, fitting trends to a maximum of five join points17. One advantage of Joinpoint analysis is its ability to detect significant shifts in trends, providing a nuanced view of temporal variations. This helps us identify and study temporal trends in esophageal cancer. Furthermore, we employed Das Gupta’s decomposition methodology to analyze the relative contributions of population growth, population aging, and changes in incidence or mortality to these variations18. Decomposition analysis helps identify key drivers by quantifying the independent contributions of different factors, such as population aging, population growth, and changes in disease prevalence, to the variation in disease burden. This can guide the development of public health policies19,20,21. While this method effectively highlights the relative impact of demographic and epidemiologic factors, it assumes independence among these components and may not fully account for overlapping influences in real-world scenarios. To predict the numbers of new cases and deaths due to esophageal cancer from 2020 to 2044 by sex and histological types, a log-linear age–period–cohort model via NORDPRED, taking into account the changing rates and changing population structure22. Moreover, we performed a sensitivity analysis using a Bayesian age–period–cohort (BAPC) model in addition to the NORDPRED model to ensure the robustness of our projections. The BAPC model, implemented using the same dataset stratified by sex and histological subtype, provided an alternative methodological framework to evaluate the impact of modeling assumptions on our forecasts23. Data management and analyses were performed using R software (version 4.3.0). Statistical significance was assessed at an α level of P < 0.05, and all hypotheses were 2-sided.
Results
Overall esophageal cancer
There were 39,700 esophageal cancer cases and 35,259 deaths in SEER-12 for the entire study period. Among the cases, the majority were males (76.29%) and White individuals (82.29%). EAC presented higher incidence and mortality rates (2.25 and 1.94 per 100,000 person-years, respectively) compared to ESCC (1.50 and 1.38 per 100,000 person-years, respectively). The incidence (4.30 per 100,000 person-years) and mortality (3.80 per 100,000 person-years) rates among males in EAC were approximately twice as high as those for ESCC (2.11 and 2.00 per 100,000 person-years, respectively). Whites accounted for the majority of cases and deaths (82.29% and 82.04%, respectively); however, Blacks showed the highest incidence and mortality rates of esophageal cancer. Specifically, the incidence was highest among Black individuals for ESCC (3.73 per 100,000 person-years), while for EAC, the highest incidence was observed among Whites (2.68 per 100,000 person-years). Consistent with the incidence data, the incidence-based mortality showed similar racial disparities in EAC and ESCC (Table 1).
Incidence trends of esophageal cancer (1992–2019)
The overall trend of esophageal cancer incidence showed an insignificant increase during 1992–2004, followed by a rapid decrease with an APC of 1.3% (95% CI − 1.7% to − 1.0%) from 2004 to 2019. The rates declined for all sexes, races and age groups from 2004 to 2019, with the most significant decreases observed in Black individuals (AAPC, − 4.6% [95% CI − 4.9% to − 4.3%]) and in patients with tumors located in the middle part of esophagus (AAPC, − 2.7% [95% CI − 3.0% to − 2.5%]). However, those with advanced stage and tumor located at the lower part of esophagus showed increasing trends with AAPC of 1.6% (95% CI 1.0–2.2%) and 0.6% (95% CI 0.2–1.1%), respectively (Fig. 1 and Table S1).
Trends in the incidence (1992–2019) and incidence-based mortality rates (1993–2019) of esophageal cancer stratified by sex, age, and race. Note: (A) Incidence and incidence-based mortality rates stratified by sex. (B) Incidence and incidence-based mortality rates stratified by age group. (C) Incidence rates stratified by race. (D) Incidence-based mortality rates stratified by race.
The incidence rates in EAC differed from the overall incidence trends, statistically increasing by 5.2% (95% CI 3.2–7.1%) from 1992 to 2000 and then plateauing from 2000 to 2019 (APC, 0.1% [95% CI − 0.2% to 0.5%]) (Fig. 2). The most substantial increase was observed in those diagnosed at the distant stage (AAPC, 3.2% [95% CI 2.4–4.0%]), followed by females, Whites, diagnoses at the regional stage, and tumor located at lower and upper esophagus (Figs. 3 and 4; Table S2). The tumor location at the lower part of esophagus showed a significant rise (AAPC, 1.9% [95% CI 1.3–2.5%] during the study period. Although the AAPC of most of the variables of EC indicated an upper trend during the study period, they tended to decrease or plateau to varying degrees at the start of the twenty-first century. ESCC incidence rates showed a decreasing trend for all variables in the study, with the largest decrease being black (AAPC, − 5.5% [95% CI − 5.9% to − 5.2%]), followed by having a localized tumor, age < 60, and tumor location in middle or lower esophagus (Figs. 3 and 4; Table S3).
Trends in the incidence (1992–2019) and incidence-based mortality rates (1993–2019) of esophageal adenocarcinoma (EAC) and esophageal squamous cell carcinoma (ESCC) stratified by sex. Note: (A) Incidence rates of EAC and ESCC stratified by sex. (B) Incidence-based mortality rates of EAC and ESCC stratified by sex.
Trends in the incidence (1992–2019) and incidence-based mortality rates (1993–2019) of esophageal adenocarcinoma (EAC) and esophageal squamous cell carcinoma (ESCC) stratified by age. Note: (A) Incidence rates of EAC and ESCC stratified by age group. (B) Incidence-based mortality rates of EAC and ESCC stratified by age group.
Trends in the incidence (1992–2019) and incidence-based mortality rates (1993–2019) of esophageal adenocarcinoma (EAC) and esophageal squamous cell carcinoma (ESCC) stratified by race. Note: (A) Incidence rates of EAC and ESCC stratified by race. (B) Incidence-based mortality rates of EAC and ESCC stratified by race.
Incidence-based mortality trends of esophageal cancer (1993–2019)
From 1993 to 1998, we observed an increasing trend in overall incidence-based mortality rates for esophageal cancer, with an APC of 4.8% (95% CI 2.4–7.1%), followed by a significant annual decline from 1998 to 2019 (APC, − 1.0% [95% CI − 1.2% to − 0.7%]) (Fig. 1). The most pronounced decline occurred among Black individuals (AAPC, − 4.2% [95% CI − 4.6% to − 3.9%]). Conversely, patients diagnosed with distant metastasis (AAPC, 1.7% [95% CI 1.2–2.1%]), patients with tumor in the lower esophagus (AAPC, 1.1% [95% CI 0.4–1.8%]) and Whites (AAPC, 0.9% [95% CI 0.4–1.5%]) experienced a considerable growth in incidence-based mortality during the study period (Table S1).
EAC showed an upward trend across all sexes, age groups and racial groups with an APC of 8.2% (95% CI 5.4–11.1%) from 1993 to 1999, and then slightly rising from 1999 to 2019 (APC, 0.5% [95% CI 0.2–0.8%]). The most significant increases were observed in individuals age 60–69 years (AAPC, 3.7% [95% CI 0.9–6.5%]), patients diagnosed with regional (AAPC, 3.5% [95% CI 0.6–6.5%]) or distant (AAPC, 3.1% [95% CI 2.4–3.8%]), Whites (AAPC, 2.6% [95% CI 2.0–3.2%]) and those with tumors in the lower esophagus (AAPC, 2.3% [95% CI 1.6–3.0%]) (Figs. 3 and 4; Table S2). ESCC mortality rates, however, showed a decline of 2.1% (95% CI − 2.9% to − 1.2%) from 1993 to 2019, with the largest decrease observed in patients with a decreasing trend for all variables in the study (Figs. 3 and 4; Table S3).
Decomposition analysis
Population ageing has been a significant factor in the increase of esophageal cancers of various histological subtypes over the study period. Specifically, it has been the main driver of the rise in ESCC, while changes in epidemiology have largely contributed to the increase in EAC. Between 1992 to 2019, the incidence of esophageal cancer increased by 52.04%, from 1124 cases in 1992 to 1709 in 2019, influenced by aging (41.56%), population growth (29.97%), and a slight decrease in incidence (− 19.49%). The total change in EAC was 163.94%, with contributions of 55.39% from aging, 40.75% from population growth, and 67.8% from changes in incidence. Conversely, the total change in ESCC was − 20.12%, with contributions from aging (32.78%), population growth (23.04%), and a substantial decrease in incidence (− 75.94%). And the overall changes in mortality for both EAC and ESCC have also shown an upward trend, with increases of 246.97% and 5.49%, respectively. In the decomposition analysis of the changes in mortality, we found that for esophageal cancer and EAC, aging, population growth and epidemiological change in mortality all contributed to the increase. However, for ESCC, the change due to epidemiological change in mortality showed a decrease (− 56%) (Table 2).
Forecast of esophageal cancer incidence and mortality trends (2020–2044)
Predictions from 2020 to 2044 indicate a 31.0% increase in new esophageal cancer cases, from 1719 in 2019 to 2252 in 2044, and a 31.1% increase in deaths, from 1615 to 2117. EAC is projected to experience the most significant rise in both cases and deaths, nearly 50%, with an AAPC of 1.59 (95% CI 1.52–1.65) for cases and 1.54 (95% CI 1.42–1.65) for deaths. Despite the absolute increase in the number of esophageal cancer cases and deaths, age-standardized rates are predicted to decline, with AAPCs of − 0.35 (95% CI − 0.39 to − 0.31) for incidence and − 0.80 (95% CI − 0.85 to − 0.76) for mortality from 2019 to 2044. The predicted incidence and mortality rates, stratified by sex, show a more pronounced decrease observed in men than in women. Moreover, a similar decrease is expected in mortality rates for both EAC and ESCC, but the estimated trend for EAC incidence rates is forecasted to increase, with an AAPC of 0.25 (95% CI 0.23–0.28), rising from 2.38 in 2019 to 2.54 in 2044 (Fig. 5). The results from the BAPC model aligned closely with those of NORDPRED, both models indicated a steady decline in overall incidence and mortality rates (Fig. S1).
Discussion
This study found that although the incidence and mortality rates of esophageal cancer among Americans have significantly improved over the past several decades, the number of esophageal cancer cases has substantially increased. This increase is primarily attributed to population aging and growth, illustrating the significance of comprehending how aging influences future health requirements. Furthermore, our projections suggest a continued rise in the number of esophageal cancer cases. Therefore, American policymakers should be conscious of the fact that the number of incidence and mortality rates of esophageal cancer represent the disease burden that the U.S. healthcare system must address.
During the study period, the age-standardized overall incidence and mortality rates of esophageal cancer decreased. However, distinct trends emerged when comparing the two main histologic subtypes. The incidence rate of EAC showed a stable pattern since 2000, consistent with findings in previous reports9. Important risk factors for EAC include tobacco use, high body mass index, gastroesophageal reflux disease symptoms (GERD) and low fruit and vegetable consumption5,24,25. The observed plateau in EAC incidence may be explained by declining smoking rates and the widespread use of proton pump inhibitors to manage GERD symptoms26,27,28. However, despite these advancements, our study found that EAC mortality continues to rise by 0.5% annually since 1999, contrasting with a SEER study reporting a plateau in 201229. According to our decomposition analysis, the increase in EAC deaths (135.38%) was largely due to epidemiological changes, suggesting that ongoing exposure to risk factors such as an unhealthy diet, high body mass index and GERD may be perpetuating this upward trend5,10,24,30,31. By contrast, the incidence and mortality rates of ESCC have significantly improved, likely owing to more effective smoking control and reductions in heavy alcohol consumption5,9,25. This improvement underscores the critical role of behavioral modifications in reducing disease burden. Common risk factors for ESCC include excessive use of alcohol, tobacco use, and low fruit and vegetable intake5,25,32. Despite these divergent trends, the overall burden of esophageal cancer may continue to rise from 2019 through 2044 in terms of incidence and mortality based on our predictions. The BAPC results were consistent with NORDPRED, providing robust support for the reliability of our findings. Although declining smoking rates have helped to reduce the burden of esophageal cancer, the balance may be upset as obesity and other risk factors rise5,24,30,31,33. As such, esophageal cancer remains a significant challenge for the American healthcare system, underscoring the need for further research on its risk factors, particularly those driving EAC. This study provides evidence-based insights for policymakers in healthcare planning, emphasizing the importance of integrating demographic and lifestyle trends into future strategies.
Age is a significant factor in the development of esophageal cancer7. The incidence rate of esophageal cancer accounted for 46.34%, and 49.28% of the deaths were patients over 70 years old. Our decomposition analysis revealed a strong correlation between aging and both EAC and ESCC. Notably, the incidence and mortality rates of EAC in the elderly continue to rise significantly, highlighting the need for targeted interventions. Due to the aging of society, the disease burden of esophageal cancer is still increasing, even though other risk factors are effectively controlled34. Emerging technologies like cytosponge provide promising, minimally invasive approaches for early detection of Barrett’s esophagus, the precursor to EAC, and have demonstrated effectiveness in improving diagnosis rates35,36. Therefore, policies should promote regular physical examinations and screening while encouraging healthy lifestyles among the elderly.
Sex differences and racial disparities have been also observed. Consistent with prior research, males have two to four fold higher incidence rate of esophageal cancer than females37,38, and the rise in mortality rates for EAC can be attributed to an increase in male EAC cases. The higher susceptibility of males to esophageal cancer may be due to hormone levels and gender differences in gene expression biology39. Additionally, chronic GERD is more prevalent in males, which increases the risk of esophageal cancer40. High-risk behaviours such as excessive alcohol consumption and smoking are also more common in males41. In accordance with previous studies, it has been found that EAC is more commonly found in whites, while ESCC is more commonly found in blacks42. However, our study found that the epidemiologic trend of EAC in Blacks is significantly increasing, while the incidence of ESCC is significantly decreasing. This disparity may reflect differences in GERD prevalence, obesity rates, or genetic predispositions among racial groups43,44. Further studies are necessary to explore the mechanisms underlying sex differences and racial disparities in order to develop targeted health policies.
Furthermore, our study revealed a more significant decrease in morbidity and mortality rates for localized stages of esophageal cancer, regardless of histologic subtype, when compared to regional and distant stages. After comparing incidence and mortality rates, the decrease in localized mortality was primarily due to a decline in localized-stage cancer diagnoses. In addition, advancements in immunotherapy and surgical techniques have contributed to the declining trend in early mortality45,46. It is essential to note that socioeconomic status plays a critical role in the prognosis of esophageal cancer47. Individuals in lower socioeconomic groups are more likely to be diagnosed at advanced stages due to unequal healthcare access48. Disparities in treatment accessibility, such as patients with higher household incomes being more likely to receive endoscopic resection treatment for EAC49, further underscore the impact of socioeconomic factors on esophageal cancer outcomes. Moreover, the adoption and enhancement of early detection techniques, including imaging and molecular biomarker testing29,50, may explain the increasing proportion of deaths from advanced EAC and ESCC over time in our study. Policy measures should focus on improving health coverage and access to ensure early detection and timely intervention.
Our study provided a comprehensive assessment of the incidence and mortality of esophageal cancer. However, there are several limitations to our study. First, although the SEER-12 database is highly regarded for its stringent quality standards, it represents only about 12.2% of the U.S. population and lacks certain key data, including detailed treatment histories, lifestyle factors, and clinical characteristics. This constraint limits the generalizability of our findings and our ability to perform more nuanced subgroup or causal analyses. Second, while Joinpoint regression effectively detects significant shifts in trends, it may not capture highly complex or non-linear patterns; Besides, it should be acknowledged that changes in staging classifications and diagnostic practices over the 27-year study period may have influenced the observed trends to some extent. Das Gupta’s decomposition offers clear distinctions among demographic contributions but treats them as largely independent; and the log-linear age–period–cohort model via NORDPRED reliably forecasts future burdens based on historical data, yet may be sensitive to unforeseen changes in risk profiles or clinical interventions. These methodologies enable a comprehensive analysis of esophageal cancer trends and future trajectories. Future research could expand coverage to additional registries, incorporate richer clinical and behavioral data, and refine modeling approaches to better capture evolving patterns of esophageal cancer and inform targeted prevention and treatment strategies.
Conclusions
In summary, esophageal cancer incidence and mortality rates have effectively improved in the United States from 1992 to 2019, although EAC mortality rates are still slowly and significantly increasing. In addition, the number of incidence and mortality of esophageal cancer is still increasing, which is mainly due to aging and population growth. Increasing aging requires effective measures to address esophageal cancer in the elderly and further control of risk factors for esophageal cancer.
Data availability
The data used in this study are publicly available. The Surveillance, Epidemiology, and End Results (SEER) Program data can be accessed from the SEER website: https://seer.cancer.gov/. Demographic data from the U.S. Census Bureau can be obtained from: https://www.census.gov/.
Abbreviations
- AAPC:
-
Average annual percent change
- APC:
-
Annual percentage change
- BAPC:
-
Bayesian age–period–cohort
- CI:
-
Confidence intervals
- EAC:
-
Esophageal adenocarcinoma
- ESCC:
-
Esophageal squamous cell carcinoma
- GERD:
-
Gastroesophageal reflux disease symptoms
- ICD-O:
-
International Classification of Oncological Diseases
- NCI:
-
National Cancer Institute
- SEER:
-
Surveillance, Epidemiology, and End Results
- STROBE:
-
Strengthening the reporting of observational studies in epidemiology
References
Bray, F. et al. Global cancer statistics 2022: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J. Clin. 74, 229–263 (2024).
Zhou, B. et al. Global burden and temporal trends in incidence and mortality of oesophageal cancer. J. Adv. Res. 50, 135–144 (2023).
Siegel, R. L., Giaquinto, A. N. & Jemal, A. Cancer statistics, 2024. CA Cancer J. Clin. 74, 12–49 (2024).
Paiji, C. & Sedarat, A. Endoscopic management of esophageal cancer. Cancers (Basel) 14, 3583 (2022).
Wang, S.-M. et al. Population attributable risks of subtypes of esophageal and gastric cancers in the United States. Am. J. Gastroenterol. 116, 1844–1852 (2021).
He, H. et al. Trends in the incidence and survival of patients with esophageal cancer: A SEER database analysis. Thorac. Cancer 11, 1121–1128 (2020).
Pennathur, A., Gibson, M. K., Jobe, B. A. & Luketich, J. D. Oesophageal carcinoma. Lancet 381, 400–412 (2013).
Pohl, H. & Welch, H. G. The role of overdiagnosis and reclassification in the marked increase of esophageal adenocarcinoma incidence. J. Natl. Cancer Inst. 97, 142–146 (2005).
Liu, K. S., Raza, S. A., El-Serag, H. B. & Thrift, A. P. Trends in esophageal adenocarcinoma and esophageal squamous cell carcinoma incidence in the United States from 1992 to 2019. Cancers 14, 6049 (2022).
Wang, Y. et al. Has the prevalence of overweight, obesity and central obesity levelled off in the United States? Trends, patterns, disparities, and future projections for the obesity epidemic. Int. J. Epidemiol. 49, 810–823 (2020).
Weir, H. K., Thompson, T. D., Soman, A., Møller, B. & Leadbetter, S. The past, present, and future of cancer incidence in the United States: 1975 through 2020. Cancer 121, 1827–1837 (2015).
National Cancer Institute. Surveillance, Epidemiology, and End Results Program. https://seer.cancer.gov/. Accessed 28 Feb 2023.
Wu, W. et al. Rising trends in pancreatic cancer incidence and mortality in 2000–2014. Clin. Epidemiol. 10, 789–797 (2018).
de Vos-Geelen, J. et al. Trends in treatment and overall survival among patients with proximal esophageal cancer. World J. Gastroenterol. 25, 6835–6846 (2019).
U.S. Census Bureau. International Database. https://www.census.gov/data-tools/demo/idb/. Accessed 13 Feb 2024.
Klein, R. J. & Schoenborn, C. A. Age Adjustment Using the 2000 Projected U.S. Population. https://doi.org/10.1037/e583772012-001 (2001).
National Cancer Institute. Joinpoint Regression Program. https://surveillance.cancer.gov/joinpoint/. Accessed 28 Feb 2023.
Das Gupta, P. A general method of decomposing a difference between two rates into several components. Demography 15, 99–112 (1978).
GBD 2017 Causes of Death Collaborators. Global, regional, and national age-sex-specific mortality for 282 causes of death in 195 countries and territories, 1980–2017: A systematic analysis for the global burden of disease study 2017. Lancet 392, 1736–1788 (2018).
GBD 2019 Dementia Forecasting Collaborators. Estimation of the global prevalence of dementia in 2019 and forecasted prevalence in 2050: An analysis for the global burden of disease study 2019. Lancet Public Health 7, e105–e125 (2022).
Bai, Z. et al. The global, regional, and national patterns of change in the burden of non-malignant upper gastrointestinal diseases from 1990 to 2019 and the forecast for the next decade. Int. J. Surg. 111, 80–92. https://doi.org/10.1097/JS9.0000000000001902 (2025).
Møller, B. et al. Prediction of cancer incidence in the Nordic countries: Empirical comparison of different approaches. Stat. Med. 22, 2751–2766 (2003).
Schmid, V. J. & Held, L. Bayesian age-period-cohort modeling and prediction—BAMP. J. Stat. Softw. 21, 1–15 (2007).
Abnet, C. C. et al. A prospective study of BMI and risk of oesophageal and gastric adenocarcinoma. Eur J Cancer. 44, 465–471 (2008).
Engel, L. S. et al. Population attributable risks of esophageal and gastric cancers. J. Natl. Cancer Inst. 95, 1404–1413 (2003).
Rodriguez, G. M. et al. Trends in epidemiology of esophageal cancer in the US, 1975–2018. JAMA Netw. Open 6, e2329497 (2023).
Wang, Q.-L., Xie, S.-H., Li, W.-T. & Lagergren, J. Smoking cessation and risk of esophageal cancer by histological type: Systematic review and meta-analysis. J. Natl. Cancer Inst. 109, 12 (2017).
Mishuk, A. U. et al. National trends in prescription proton pump inhibitor use and expenditure in the United States in 2002–2017. J. Am. Pharm. Assoc. 61, 87-94.e7 (2021).
Corona, E. et al. Trends in esophageal cancer mortality and stage at diagnosis by race and ethnicity in the United States. Cancer Causes Control 32, 883–894 (2021).
Kröner, P. T., Cortés, P. & Lukens, F. J. The medical management of gastroesophageal reflux disease: A narrative review. J. Prim. Care Community Health 12, 21501327211046736 (2021).
El-Serag, H. B., Sweet, S., Winchester, C. C. & Dent, J. Update on the epidemiology of gastro-oesophageal reflux disease: A systematic review. Gut 63, 871–880 (2014).
Freedman, N. D. et al. A prospective study of tobacco, alcohol, and the risk of esophageal and gastric cancer subtypes. Am. J. Epidemiol. 165, 1424–1433 (2007).
Hales, C. M., Fryar, C. D., Carroll, M. D., Freedman, D. S. & Ogden, C. L. Trends in obesity and severe obesity prevalence in US youth and adults by sex and age, 2007–2008 to 2015–2016. JAMA 319, 1723 (2018).
Li, H. et al. Age–period–cohort analysis of incidence, mortality and disability-adjusted life years of esophageal cancer in global, regional and national regions from 1990 to 2019. BMC Public Health 24, 212 (2024).
Shaheen, N. J. et al. Diagnosis and management of Barrett’s esophagus: An updated ACG guideline. Am. J. Gastroenterol. 117, 559–587 (2022).
Deboever, N., Jones, C. M., Yamashita, K., Ajani, J. A. & Hofstetter, W. L. Advances in diagnosis and management of cancer of the esophagus. BMJ 385, e074962 (2024).
Li, B., Liu, Y., Peng, J., Sun, C. & Rang, W. Trends of esophageal cancer incidence and mortality and its influencing factors in China. Risk Manag. Healthc. Policy 14, 4809–4821 (2021).
Li, S. et al. Changing trends in the disease burden of esophageal cancer in China from 1990 to 2017 and its predicted level in 25 years. Cancer Med. 10, 1889–1899 (2021).
Mathieu, L. N., Kanarek, N. F., Tsai, H.-L., Rudin, C. M. & Brock, M. V. Age and sex differences in the incidence of esophageal adenocarcinoma: Results from the Surveillance, Epidemiology, and End Results (SEER) registry (1973–2008). Dis. Esophagus 27, 757–763 (2014).
Houston, T. & Sharma, P. Volumetric laser endomicroscopy in Barrett’s esophagus: Ready for primetime. Transl. Gastroenterol. Hepatol. 5, 27 (2020).
Mchembe, M. D. et al. Endoscopic and clinicopathological patterns of esophageal cancer in Tanzania: Experiences from two tertiary health institutions. World J. Surg. Oncol. 11, 257 (2013).
Cook, M. B., Chow, W.-H. & Devesa, S. S. Oesophageal cancer incidence in the United States by race, sex, and histologic type, 1977–2005. Br. J. Cancer 101, 855–859 (2009).
Xie, S.-H., Rabbani, S., Petrick, J. L., Cook, M. B. & Lagergren, J. Racial and ethnic disparities in the incidence of esophageal cancer in the United States, 1992–2013. Am. J. Epidemiol. 186, 1341–1351 (2017).
Kim, A., Ashman, P., Ward-Peterson, M., Lozano, J. M. & Barengo, N. C. Racial disparities in cancer-related survival in patients with squamous cell carcinoma of the esophagus in the US between 1973 and 2013. PLoS ONE 12, e0183782 (2017).
Demarest, C. T. & Chang, A. C. The landmark series: Multimodal therapy for esophageal cancer. Ann. Surg. Oncol. 28, 3375–3382 (2021).
Rogers, J. E., Sewastjanow-Silva, M., Waters, R. E. & Ajani, J. A. Esophageal cancer: Emerging therapeutics. Expert Opin. Ther. Targets 26, 107–117 (2022).
Wang, N. et al. The effect of socioeconomic status on health-care delay and treatment of esophageal cancer. J. Transl. Med. 13, 241 (2015).
Macdonald, S., Macleod, U., Campbell, N. C., Weller, D. & Mitchell, E. Systematic review of factors influencing patient and practitioner delay in diagnosis of upper gastrointestinal cancer. Br. J. Cancer 94, 1272–1280 (2006).
Geng, C. X. et al. Socioeconomic disparities affect outcomes in early-stage esophageal adenocarcinoma: A SEER analysis. Clin. Gastroenterol. Hepatol. 21, 2797-2806.e6 (2023).
Januszewicz, W. & Fitzgerald, R. C. Early detection and therapeutics. Mol. Oncol. 13, 599–613 (2019).
Funding
Guangdong Basic and Applied Basic Research Foundation (No. 2022A1515012623); Science and Technology Special Fund of Guangdong Province of China (190829105556145); Strategic and Special Fund for Science and Technology Innovation of Guangdong Province of China (180918114960704); Guangdong Provincial Medical Science and Technology Research Fund Project (No. A2021255); Guangdong Basic and Applied Basic Research Foundation (No. 2023A1515010616).
Author information
Authors and Affiliations
Contributions
ZX conceptualized the study and JL collaborated in the design of the study. ZX and JL designed survey, acquired the data and analyzed the data. ZL contributed to the interpretation of the data. ZX and JL wrote the main manuscript text. HS, KH, DL and YX prepared tables and figure. DZ and CL critically reviewed and improved the manuscript. All authors substantially contributed to the study and approved its submission. The author(s) read and approved the final manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethics approval and consent to participate
The Institutional Review Board of Shantou University School of Medicine deemed the research exempt due to the use of public data, waiving informed consent requirements.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Xie, Z., Lin, J., Li, Z. et al. Esophageal cancer trends in the US from 1992 to 2019 with projections to 2044 using SEER data. Sci Rep 15, 22423 (2025). https://doi.org/10.1038/s41598-025-01674-z
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-025-01674-z