Abstract
Effective management of osteoporosis requires individuals to take responsibility for following medication, exercise, and dietary guidelines. The aim of this study was to provide important insights into self-care behaviors and their determinants, especially dietary patterns related to vitamin D and calcium intake among elderly women, both healthy and those with osteoporosis. This cross-sectional descriptive-comparative study included 250 postmenopausal women aged 60 and above, consisting of 125 healthy women and 125 women with osteoporosis which conducted in Tabriz, Iran. The data collection instruments comprised a demographic questionnaire, Menopausal Self-Care Questionnaire, and Vitamin D and Calcium Food Frequency Questionnaire. Multivariate linear regression models were employed to identify predictors of self-care behaviors and dietary intakes. The mean (Standard deviation: SD) total self-care score (33–165) in healthy women was higher 118.97 ± 19.92 compared to osteoporotic women 84.7 ± 14.98 (p < 0.001). Healthy women also exhibited significantly higher daily dietary intakes of calcium (850.52 ± 147.92 mg vs. 546.71 ± 60.28 mg, p < 0.001) and vitamin D (3.38 ± 0.65 mg vs. 2.0 ± 0.34 mg, p < 0.001) than osteoporotic women. Multivariate analysis identified household income, age, education, exercise, and BMI as key predictors of self-care behaviors and dietary intakes (p < 0.05) in healthy and osteoporotic elderly women. Postmenopausal women with osteoporosis exhibited poorer self-care behaviors and lower calcium/vitamin D intake compared to healthy peers, with socioeconomic factors (income, education), exercise, age, and BMI as key predictors.
Similar content being viewed by others
Introduction
The increase in life expectancy and the decrease in fertility rates have led to an expanding elderly population worldwide, making population aging a pressing public health concern in modern society1,2,3. The phenomenon of aging is associated with a progressive decline of biological tissues, which negatively impacts the structural integrity and functionality of vital organs, and represents a significant recognized risk factor for the majority of chronic diseases4. Osteoporosis is a widespread age-related disease characterized as a skeletal condition distinguished by compromised bone integrity, increasing susceptibility to fractures5. The prevalence of osteoporosis is lower in males compared to females due to greater bone mass, shorter longevity, and the absence of a male equivalent to menopause6. As a result, the rate of bone loss is heightened in women, resulting in the earlier manifestation of osteoporosis relative to men. This process is often linked to the onset of menopause and the accompanying decrease in estrogen levels. In women experiencing estrogen deficiency, the initial rate of bone loss is significantly greater than that caused by other age-related mechanisms6. The incidence of osteoporosis in women increases with age progression attributable to diminishing bone mineral density. At age 60, the prevalence is about 10%, rising to 20% at age 70, 40% at age 80, and reaching two-thirds by age 907. In 1994, the World Health Organization (WHO) established a definition for osteoporosis based on a bone mineral density (BMD) threshold of − 2.5 standard deviations (SDs) or lower than the mean value for young adult females, commonly referred to as a T-score of − 2.5 SD or below. Approximately 200 million women globally meet the osteoporosis criterion of a T-score of − 2.5 SD or lower8,9.
An essential factor in the prevention of osteoporosis is the adoption of suitable health-promoting frameworks, lifestyle modifications, and daily habits that enhance individual quality of life and efficiency10,11. Thus, promoting preventive behaviors such as engaging in physical activity and maintaining a balanced diet serves as a simple yet effective means of disease prevention and health promotion. One of the primary global health priorities is to increase the number of women who receive education on osteoporosis12.
The modification of behavioral patterns that affect osteoporosis requires changes in individual behavior; consequently, self-care practices can play a pivotal role in the prevention of this condition among older women. Self-care encompasses a range of activities undertaken by patients to ensure the stability of their condition, including self-care maintenance, monitoring of disease-related signs and symptoms, and appropriate responses to these signs and symptoms, termed self-care management13. The asymptomatic progression of osteoporosis complicates self-care monitoring and management efforts. However, the principles of self-care maintenance can be effectively utilized by patients with osteoporosis. Previous studies, including research by Malekmirzaie et al., have shown that self-care behaviors play a crucial role in preventing and managing osteoporosis in elderly women. Their findings indicate that women who engage in higher levels of self-care and possess greater health literacy are less likely to develop osteoporosis. This suggests that promoting self-care practices and enhancing health literacy could be effective strategies in reducing the risk of osteoporosis among older women14. These individuals typically need to engage in various activities that promote disease stability and reduce fracture risk, such as adhering to medication schedules, consuming a diet rich in calcium, and wearing non-slip shoes15. Among these factors, nutrition and diet are recognized as a significant component of effective self-care16. Nutrition, as a modifiable risk factor for osteoporosis, significantly influences both the development and preservation of bone mass. Optimal nutritional health, characterized by sufficient intake of dietary protein, calcium, vitamin D, as well as fruits and vegetables, contributes positively to bone integrity. Conversely, diets high in calories and excessive alcohol intake have been linked to diminished bone mass and an increased incidence of fractures17. Additionally, various factors such as body mass index (BMI), smoking habits, and recent fractures have been found to adversely affect self-care behaviors in postmenopausal women diagnosed with osteoporosis18. These elements can complicate the management of the condition, making it more challenging for women to engage in and sustain effective self-care practices. By addressing these factors through targeted interventions, it may be possible to improve self-care and overall health outcomes for this group. Thus, this study aimed to assess the protective role of self-care behaviors and a healthy diet in older women with osteoporosis. It also sought to examine the relationship between self-care behaviors and dietary intake in older women with osteoporosis compared to their healthy counterparts.
Methods
Study design
The present study is a cross-sectional descriptive-comparative analysis involving 250 elderly postmenopausal women diagnosed with osteoporosis aged 60 and above, who were referred to the bone density measurement center of Sina Hospital in Tabriz, Iran, between October 2021 and January 2022. The research was approved by the Ethics Committee of Tabriz University of Medical Sciences (IR.TBZMED.REC.1400.343), with verification that all experimental procedures were performed in accordance with ethical guidelines and regulations. A portion of this research project has been previously published in our earlier article14. The written informed consent was obtained from the participants.
Sample size
The sample size was determined based on the study by Abdolalipour et al.19 regarding the nutrition scale score in postmenopausal women with osteoporosis and healthy women. Using the formula for the difference in mean in two independent groups with a one-tailed test, Mean1: m1 = 27.4, m2 = 26.0), standard deviations sd1 = 4.5 and sd2 = 4, effect size d = 0.328, 80% power, and 95% confidence level, the sample size was estimated to be 116 individuals per group. Considering the probability of a 5–10% dropout, the sample size was adjusted to 125 individuals per group, resulting in a total of 250 participants.
Inclusion and exclusion criteria
The study included postmenopausal women aged 60 years and above who had experienced amenorrhea for at least 12 consecutive months, women with a lumbar spine or femoral neck T-score of ≥ − 1 (healthy women), women with a lumbar spine or femoral neck T-score of ≤ − 2.5 (osteoporotic women), ability to communicate verbally to answer questions, and willingness to participate in the study. The exclusion criteria included: bone diseases other than osteoporosis, metastatic bone diseases, malignancies, renal failure and kidney diseases, use of bone metabolism-affecting drugs, including intravenous bisphosphonates in the past 5 years, or oral bisphosphonates in the past 6 months, and cumulative use of oral bisphosphonates for more than three years or more than one month between 6 and 12 months before the study, use of parathyroid hormone analogs in the past 12 months, use of hormonal drugs or corticosteroids, hereditary diseases (hemophilia, thalassemia, hemochromatosis), endocrine disorders (such as Cushing’s syndrome, hyperthyroidism, primary hyperparathyroidism, and type 1 diabetes), chronic liver diseases, biliary tract abnormalities, and gastrointestinal disorders (such as primary biliary cirrhosis, celiac disease, Crohn’s disease, gastric surgery, or complete gastrectomy), body mass index less than 18.5, and excessive use of cigarettes, alcohol, and drugs.
These exclusion criteria were established to ensure that the study focused on the specific impact of self-care behaviors and dietary habits on osteoporosis, without the confounding effects of other significant health conditions or treatments.
Bone mineral density
The BMD of the femoral neck and lumbar spine (L1–L4) was assessed using a Hologic QDR 4500 W (S/N 50266) dual-energy X-ray absorptiometry (DXA) densitometer, operated by an experienced radiologist. The diagnosis of osteoporosis followed the World Health Organization (WHO) criteria. According to the WHO, a T-score of − 2.5 SD or lower, compared to the average BMD of young adults, indicates osteoporosis, while a T-score of − 1.0 or higher signifies normal bone density20.
Data collection tools
Three questionnaires were used for data collection: The first was a demographic questionnaire that gathered information on age, menopause age, education level, occupation, household income, marital status, BMI, physical activity type and amount, parity, smoking history, abortion history, osteoporosis-related fractures, and calcium and vitamin D supplement intake.
The second questionnaire was the Menopausal Self-Care Questionnaire (MSCQ), designed to evaluate self-care practices in menopausal women. Developed by Kafaei Atrian et al.21 based on Waltz’s instrument development method and Orem’s self-care theory, it consists of 33 items across four dimensions: physical, mental, social, and information acquisition. Items are rated on a five-point Likert scale: 1: “Never”; 2: “Rarely”; 3: “Sometimes”; 4: “Often”; and 5: “Always” The possible total scores for the subscales are as follows: general health (45), screening (30), nutrition (25), memory (15), hot flashes and night sweats (15), sexuality (15), and social communication (20). The total possible score for the questionnaire ranges from 33 to 165, with higher scores indicating greater self-care ability22. The questionnaire was psychometrically validated in Iran by Kafaei Atrian et al., reporting a content validity ratio of 0.7, a content validity index of 0.7, an ICC rate of 0.76, and a Cronbach’s alpha of 0.8821.
Dietary behavior was measured using the Calcium and Vitamin D Food Frequency Questionnaire (FFQ). This questionnaire includes 74 food items containing calcium and vitamin D across 9 food groups, developed based on scientific texts23,24. After completing the questionnaire, the amounts of nutrients consumed per day were calculated and analyzed using Nutritionist IV software (San Bruno, Canada) adapted for Iranian dietary patterns, which converts the recorded food items into grams to assess calcium and vitamin D intake.
To determine the validity of this questionnaire, face validity was used. For face validity, the opinions of ten faculty members from Tabriz University of Medical Sciences were utilized, and their comments were incorporated into the questionnaire. Additionally, for the reliability of this questionnaire, the internal consistency method was employed. Cronbach’s alpha was reported as 0.792. The intraclass correlation coefficient was 0.946 (95% CI 0.864–0.979, p < 0.001).
After explaining the objectives and methods of the study, and obtaining written consent, data were collected using questionnaires and through interviews by the researcher in a private room, respecting the privacy of the individuals. Data collection through structured interviewer-administered questionnaires significantly reduced the occurrence of missing values. For remaining incomplete records, a multiple imputation approach using chained equations (MICE) was applied, with sensitivity analyses confirming robustness of imputed datasets. For participants unable to read, verbal consent was obtained following detailed explanations.
Statistical analysis
Statistical Package for the Social Sciences (SPSS) version 23 (IBM SPSS Statistics, IBM Corporation, Chicago, IL) was used for data analysis. The normality of data distribution was evaluated, utilizing Kolmogorov–Smirnov test. Descriptive data were depicted as frequency, percentage, mean (SD). Bivariate statistical tests such as independent t test, Chi-square test, and Fisher’s exact test were used to analyze the relation between self-care behavior, daily calcium, and vitamin D intake with socio-demographic characteristics. Then, the independent variables with P < 0.2 in the bivariate tests were entered into the multivariate linear regression model with backward strategy. Before conducting multivariate analysis, the assumptions of the regression including normality of the residuals, homogeneity of the residual variance, multicollinearity of independent variables, and independence of the residuals were studied.
Results
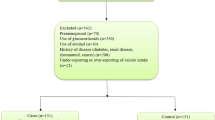
In this study, 548 women aged 60–70 years were assessed for eligibility criteria. Of these, 245 women were excluded due to ineligibility and 53 subjects were excluded due to unwillingness to participate. Finally, 125 healthy eligible women and 125 women with osteoporosis were included in this study and necessary information was collected.
The mean (standard deviation: SD) of the total self-care score in healthy women (118.97 (14.98)) was significantly higher than that in the osteoporotic women (84.7 (19.92)), from the range of 33–165 (p < 0.001). Regarding the relationship between demographic characteristics and the total score of self-care behaviors in elderly women, stratified by osteoporosis status, in the osteoporosis group, the mean and SD of self-care varied across categories of household income (p < 0.001). In the healthy group, there was a significant difference in the mean (SD) of self-care across age, education, household income level, supplement type, and exercise (p < 0.05). Specifically, in the 60–65 age group compared to the 66–70 age group, those with diploma/university education, those with income exceeding expenses, those taking combined calcium/vitamin D supplements, and those exercising regulary, the self-care score was significantly higher compared to the other groups (Table 1).
The mean (SD) daily dietary calcium intake in healthy women was 850.52 (147.92) mg, which was significantly higher than that in the osteoporotic women, 546.71 (60.28) mg (p < 0.001). In the osteoporotic group, the mean (SD) dietary calcium intake significantly varied across age, income level, type of supplement, and BMI (p < 0.05). Notably, in the older age group (66–70), those with income exceeding expenses, soy, calcium, and vitamin D supplement users, individuals with normal BMI, calcium intake was higher compared to other groups. In the healthy women, the mean (SD) dietary calcium intake varied across age, education, income, and exercise (p < 0.05). Specifically, in the younger age group (60–65), those with higher education, those with income exceeding expenses, and those exercising regulary, dietary calcium intake was higher compared to other groups (Table 2).
The mean (SD) daily dietary intake of vitamin D in healthy women was 3.38 (0.65) mg, which was significantly higher than that in the osteoporotic women 2.0 (0.34) mg (p < 0.001). In the osteoporotic group, the mean (SD) dietary intake of vitamin D statistically varied across age, education, and income (p < 0.05). Notably, in the older age group (66–70), those with no formal education, income below expenses, dietary vitamin D intake was higher compared to other groups. In the healthy group, the mean (SD) dietary vitamin D intake significantly varied across categoreies of age, household income, type of supplement, and exercise (p < 0.05). Specifically, in the younger age group (60–65), in the group with income below expenses, those taking combined calcium/vitamin D supplements, and individuals exercising regularly, dietary vitamin D intake was higher compared to other groups (Table 3).
According to the multivariate linear regression model, household income in women with osteoporosis and variables of age, education, hosehold income, exercise, supplement use, and BMI in healthy individuals were identified as predictors of self-care behavior. Also, according to this model, and household income level in women with osteoporosis, and exercise in healthy individuals were determined as the predictors of dietary calcium intake. Moreover, the education, and household income in women with osteoporosis, and the exercise variables in healthy individuals were identified as the predictors of dietary vitamin D intake (Table 4).
Discussion
This research provides important insights into the self-care behaviors and their determinants, especially dietary intake related to vitamin D and calcium intake among elderly women, comparing healthy individuals and those with osteoporosis. In this study, the mean self-care score was notably higher in healthy women compared to those with osteoporosis. The self-care scores in both groups were notably influenced by household income. Moreover, healthy women reported increased daily intakes of dietary calcium and vitamin D from foods and supplements relative to women diagnosed with osteoporosis. A multivariate analysis revealed that household income, age, education, exercise, and BMI were predictors of self-care and dietary intakes.
The results showed that the average total self-care score was significantly higher in healthy women compared to women with osteoporosis. This significant difference indicates that healthy women are considerably more motivated to participate in activities that promote their well-being and health maintenance. In the osteoporosis group, household income was a key predictor of self-care behaviors, wherein, higher income levels reflecting greater health management. The evaluation of healthy women indicated younger women, those with higher education, and those with higher household income reported better self-care practices.
Self-care is defined as a set of deliberate, learned, and purpose-driven practices and activities that individuals engage in to preserve and improve their health25. Self-care practices are predominantly recommended for individuals in a state of health, with their objective centered on disease prevention. Nevertheless, these practices are equally essential for the well-being of individuals afflicted with chronic illnesses26,27. The global burden of chronic non-communicable diseases (NCDs) is predominantly driven by modifiable lifestyle determinants, notably poor dietary patterns, physical inactivity, tobacco use, and harmful levels of alcohol consumption. These behavioral risk factors are strongly correlated with the rising incidence of NCDs across populations28.
The connection between education level and self-care behaviors is notable. Studies suggest that people with higher education levels generally possess better knowledge and are more adept at understanding and implementing self-care behavioral guidelines than those with lower education levels. The findings of the study by Khademi et al.29 align with our results, which suggest that higher education levels are linked to improved self-care behaviors in menopausal women. Their research indicated that menopausal women with at least a diploma had higher average self-care attitude scores compared to those with less than a diploma. Similarly, a research conducted in Iran indicated patients with an education level of guidance school or higher had the highest self-care scores, compared to those who were illiterate or had only an elementary school education30. Additionally, a study conducted in Tanahun, Nepal31revealed that illiterate patients were three times more likely to exhibit poor self-care behaviors than their literate counterparts. In the same way, a study conducted in England, the Netherlands, and Norway/Sweden demonstrated that a lower educational level is linked to more negative attitudes towards discussing alcohol in healthcare, further highlighting the influence of education on self-care behaviors32.
The association between income level and self-care behaviors is multifaceted. Our results are consistent with earlier research showing that income level significantly impacts self-care behaviors and health outcomes. For example, Rechenberg et al.33 discovered that individuals from low- and moderate-income families faced a higher risk of poorer health outcomes compared to those from high-income families. Other studies have also demonstrated the influence of income level, underscoring the necessity of addressing income disparities to enhance self-care and overall health across different income groups. In contrast to our findings, Babazadeh et al. observed that as household income levels increased, self-care behaviors significantly decreased30.
In the present study, the analysis of the osteoporosis group revealed that household income was an important predictor of self-care behaviors. Higher income levels are likely to afford better access to healthcare resources.
-In this study, younger women, those with higher education, and higher income in the healthy group had a higher intake of calcium (Food and supplement). This highlights the importance of education and socioeconomic status in dietary habits. In the osteoporosis group, older women, those with higher income, and individuals with a normal BMI had a higher intake of calcium.
Calcium is crucial for maintaining bone health at every stage of life, which is why it is important to ensure adequate calcium intake. Insufficient calcium consumption can have detrimental effects on bone metabolism34. The primary mechanism by which low dietary calcium intake negatively impacts BMD involves the increase in parathyroid hormone (PTH) levels. This elevation in PTH accelerates bone resorption to maintain the optimal serum calcium concentration35. Adequate levels of vitamin D may help prevent or mitigate the effect of low calcium intake on the rise in PTH levels36.
Self-care activities, especially those concerning the intake of dietary calcium, are essential for the prevention and management of osteoporosis. According to a study conducted in India37women aged 51 and older had lower dietary calcium intakes than those aged 19 to 50, but total calcium intake was similar between the groups. This suggests older women compensate with calcium supplements. A higher proportion of older women used these supplements, contributing 21% of their total calcium intake, compared to 13% for younger women.
In line with our findings, previous research has established a significant connection between socioeconomic factors and calcium intake. Most of these studies have shown that individuals with lower income levels are more likely to have insufficient calcium intake38,39,40,41. Additionally, individuals with lower education levels also exhibit inadequate calcium consumption42. Therefore, populations with lower income and education levels often have insufficient calcium intake, which can lead to higher BMI and an increased risk of obesity. Jacqmain et al.43 conducted a study on 470 adults and found that calcium had a potential impact on body weight and fat mass, particularly in women. Their results align with the findings of Zemel et al.44which showed that women with low calcium intake had significantly higher BMI. One possible physiological mechanism for the effect of calcium intake on fat mass involves the calcitropic hormones, PTH and 1,25(OH)2D. Both PTH and 1,25(OH)2D have been suggested to reduce fat breakdown and increase fat synthesis, potentially through increases in the amount of intracellular calcium in adipocytes44.
In our study, osteoprotic women with low income, and lower education levels had a greater tendency to use vitamin D (dietary and supplements). This may indicate a greater reliance on supplements among individuals with lower education and higher income levels. It might seem that individuals with higher incomes are more likely to receive higher daily doses of vitamin D, possibly due to better access to vitamin D-rich foods, fortified products, and dietary supplements, as previously reported in studies such as those by Moore et al.,45. According to Moore et al.‘s investigation, which aimed to determine whether dietary, supplemental, and total vitamin D intakes in the USA are influenced by income, race/ethnicity, or gender, participants with high incomes were more likely to use vitamin D supplements (33.0%) compared to those with medium (22.5%) or low (17.6%) incomes45.
A major strength of the current study is its focus on a large population of older women, a high-risk group particularly vulnerable to osteoporosis. This emphasis is crucial as it targets a population more severely affected by the condition, providing valuable insights for effective interventions and preventive strategies. However, one limitation is that while the study effectively identifies causal relationships, its precision is limited, potentially impacting the reliability and generalizability of the findings. It is important to note that the current study was exploratory in nature, without any preliminary data, and the sample size was determined based on nutrition scores among healthy and osteoporotic elderly women. Conducting longitudinal studies to follow changes in bone status and the effects of calcium and vitamin D intake over time can help better understand causal relationships and long-term effects. The findings of this study are not applicable to elderly women with secondary osteoporosis and those with osteopenia. Since patients with osteopenia constitute a population with a high incidence of osteoporotic fractures, it is suggested that future studies include elderly osteopenic women in addition to other groups. Additionally, we excluded women with bisphosphonate use from the study, so the results are not generalizabile for these women.
Conclusion
This study highlights significant disparities in self-care behaviors and dietary patterns between postmenopausal women with osteoporosis and their healthy counterparts. The findings demonstrate that healthy elderly women exhibit markedly higher self-care scores and significantly greater daily dietary intake of calcium and vitamin D compared to osteoporotic women, underscoring the critical role of nutrition and self-management in bone health. Multivariate analysis identified socioeconomic factors (household income, education), lifestyle factors (exercise), and biological factors (age, BMI) as key predictors of self-care practices and nutrient intake. These results emphasize the need for targeted, multifaceted interventions that address modifiable determinants, such as improving dietary education, promoting physical activity, and enhancing socioeconomic support, particularly among osteoporotic populations.
Data availability
The data will be provided upon request to the corresponding author of this article.
References
Bao, J. et al. Current state of care for the elderly in China in the context of an aging population. Biosci. Trends. 16, 107–118 (2022).
Bhasin, S., Kerr, C., Oktay, K. & Racowsky, C. The implications of reproductive aging for the health, vitality, and economic welfare of human societies. J. Clin. Endocrinol. Metab. 104, 3821–3825. https://doi.org/10.1210/jc.2018-02677 (2019).
Eggersdorfer, M. et al. Hidden hunger: solutions for America’s aging populations. Nutrients. 10, 1210. https://doi.org/10.3390/nu10091210 (2018).
MacNee, W., Rabinovich, R. A. & Choudhury, G. Ageing and the border between health and disease. Eur. Respir. J. 44, 1332–1352. https://doi.org/10.1183/09031936.00134014 (2014).
Orimo, H. et al. Japanese 2011 guidelines for prevention and treatment of osteoporosis—executive summary. Arch. Osteoporos. 7, 3–20. https://doi.org/10.1007/s11657-012-0083-2 (2012).
Bonnick, S. L. Osteoporosis in men and women. Clin. Cornerstone. 8, 28–39. https://doi.org/10.1016/S1098-3597(06)80064-3 (2006).
Kanis, J. Assessment of osteoporosis at the primary health care level. WHO Collaborating Centre for Metabolic Bone Diseases (WHO Collaborating Centre for Metabolic Bone Diseases, 2007).
Kanis, J. A., Melton, I. I. I., Christiansen, L. J., Johnston, C., Khaltaev, N. & C. C. & The diagnosis of osteoporosis. J. Bone Min. Res. 9, 1137–1141. https://doi.org/10.1002/jbmr.5650090802 (1994).
Cooper, C., Campion, G. & Melton, L. r. Hip fractures in the elderly: a world-wide projection. Osteoporos. Int. 2, 285–289. https://doi.org/10.1007/BF01623184 (1992).
Kelley, G. A., Kelley, K. S. & Tran, Z. V. Resistance training and bone mineral density in women: a meta-analysis of controlled trials. Am. J. Phys. Med. Rehabil. 80, 65–77. https://doi.org/10.1097/00002060-200101000-00017 (2001).
Baheiraei, A., Ritchie, J. E., Eisman, J. A. & Nguyen, T. V. Psychometric properties of the Persian version of the osteoporosis knowledge and health belief questionnaires. Maturitas. 50, 134–139. https://doi.org/10.1016/j.maturitas.2004.04.007 (2005).
Sedlak, C. A., Doheny, M. O., Estok, P. J. & Zeller, R. A. Tailored interventions to enhance osteoporosis prevention in women. Orthop. Nurs. 24, 270–276. https://doi.org/10.1097/00006416-200507000-00009 (2005).
Riegel, B., Jaarsma, T. & Strömberg, A. A middle-range theory of self-care of chronic illness. Adv. Nurs. Sci. 35, 194–204. https://doi.org/10.1097/ANS.0b013e318261b1ba (2012).
Malekmirzaei, E., Farshbaf-Khalili, A. & Pakpour, V. The self-care behaviors and health literacy can play important preventive roles in older female osteoporosis. BMC Women’s Health. 23, 429. https://doi.org/10.1186/s12905-023-02587-7 (2023).
Cittadini, N. et al. Development and testing of a new instrument to measure self-care in patients with osteoporosis: the self-care of osteoporosis scale. Int. J Bone Fragil. 1, 28–33 (2021).
Barlow, J., Wright, C., Sheasby, J., Turner, A. & Hainsworth, J. Self-management approaches for people with chronic conditions: a review. Patient Educ. Couns. 48, 177–187. https://doi.org/10.1016/S0738-3991(02)00032-0 (2002).
Levis, S. & Lagari, V. S. The role of diet in osteoporosis prevention and management. Curr. Osteoporos. Rep. 10, 296–302. https://doi.org/10.1007/s11914-012-0114-3 (2012).
Cittadini, N. et al. Factors influencing self-care in postmenopausal women with osteoporosis: the guardian Angel® multicentric longitudinal study. Maturitas 161, 7–11. https://doi.org/10.1016/j.maturitas.2022.06.005 (2022).
Abdolalipour, S., Mirghafourvand, M., Ghassab-Abdollahi, N. & Farshbaf-Khalili, A. Health-promoting lifestyle and quality of life in affected and unaffected menopausal women by primary osteoporosis. J. Educ. Health Promot. 10, 45. https://doi.org/10.4103/jehp.jehp_1230_20 (2021).
Cosman, F. et al. Clinician’s guide to prevention and treatment of osteoporosis. Osteoporos. Int. 25, 2359–2381. https://doi.org/10.1007/s00198-014-2794-2 (2014).
Kafaei-Atrian, M., Solhi, M., Azar, F. E. F. & Atoof, F. Development and psychometric evaluation of the menopausal self-care questionnaire in a sample of Iranian postmenopausal women. Nurs. Midwifery Stud. 8, 210–216. https://doi.org/10.4103/nms.nms_34_18 (2019).
Beni, H. M., Maasoumi, Z., Pashaeypoor, R., Haghani, S. & S. & The effects of self-care education based on the health literacy index on self-care and quality of life among menopausal women: a randomized clinical trial. BMC Women’s Health. 22, 452. https://doi.org/10.1186/s12905-022-02036-x (2022).
Malekzadeh, J. & Fararooei, M. Preventing of osteoporosis: applying the health belief model. Adv. Nurs Midwifery. 24, 15–22 (2015).
Raymond, J. L. & Morrow, K. Krause and Mahan’s Food and the Nutrition Care Process e-book (Elsevier Health Sciences, 2020).
Godfrey, C. M. et al. The experience of self-care: a systematic review. JBI Libr. Syst. Rev. 8, 1351–1460. https://doi.org/10.11124/01938924-201008340-00001 (2010).
Levin, L. S. & Idler, E. L. Self-care in health. Annu. Rev. Public. Health. 4, 181–201. https://doi.org/10.1146/annurev.pu.04.050183.001145 (1983).
Iovino, P., Uchmanowicz, I. & Vellone, E. Self-care: an effective strategy to manage chronic diseases. Adv. Clin. Exp. Med. 33, 767–771. https://doi.org/10.17219/acem/191102 (2024).
Dolatkhah, N. et al. Nutrition knowledge and attitude in medical students of Tabriz university of medical sciences in 2017–2018. BMC Res. Notes. 12, 1–6. https://doi.org/10.1186/s13104-019-4788-9 (2019).
Khademi, K., Kaveh, M. H., Asadollahi, A. & Nazari, M. Development and validation of the women’s Self-care knowledge and attitude questionnaire (WSKAQ). BMC Public. Health. 24, 2338. https://doi.org/10.1186/s12889-024-17782-8 (2024).
Babazadeh, T., Lotfi, Y. & Ranjbaran, S. Predictors of self-care behaviors and glycemic control among patients with type 2 diabetes mellitus. Front. Public. Health. 10, 1031655. https://doi.org/10.3389/fpubh.2022.1031655 (2023).
Baral, I. A. & Baral, S. Self-care management among patients with type 2 diabetes mellitus in tanahun, Nepal. Arch. Community Med. Public. Health. 7, 037–042 (2021).
Karlsson, N. et al. Relationship between educational level and attitudes towards alcohol conversations in healthcare: A cross-sectional survey conducted in four European countries. Int. J. Public. Health. 68, 1605634. https://doi.org/10.3389/ijph.2023.1605634 (2023).
Rechenberg, K., Whittemore, R., Grey, M., Jaser, S. & Group, T. R. Contribution of income to self-management and health outcomes in pediatric type 1 diabetes. Pediatr. Diabetes. 17, 120–126. https://doi.org/10.1111/pedi.12334 (2016).
Zhu, K. & Prince, R. L. Calcium and bone. Clin. Biochem. 45, 936–942. https://doi.org/10.1016/j.clinbiochem.2012.05.006 (2012).
Choi, H. S. et al. Low serum vitamin D is associated with high risk of diabetes in Korean adults. J. Nutr. 141, 1524–1528. https://doi.org/10.3945/jn.111.139121 (2011).
Steingrimsdottir, L., Gunnarsson, O., Indridason, O. S., Franzson, L. & Sigurdsson, G. Relationship between serum parathyroid hormone levels, vitamin D sufficiency, and calcium intake. JAMA. 294, 2336–2341. https://doi.org/10.1001/jama.294.18.2336 (2005).
Riggin, A. D. Calcium Intake in Low-Income Women in Indiana (College of Health and Human Sciences, 2009).
Cormick, G. & Belizán, J. M. Calcium intake and health. Nutrients. 11, 1606. https://doi.org/10.3390/nu11071606 (2019).
Wallace, T. C., Reider, C. & Fulgoni, V. L. Calcium and vitamin D disparities are related to gender, age, race, household income level, and weight classification but not vegetarian status in the united states: analysis of the NHANES 2001–2008 data set. J. Am. Coll. Nutr. 32, 321–330. https://doi.org/10.1080/07315724.2013.817642 (2013).
Shlisky, J. et al. Calcium deficiency worldwide: prevalence of inadequate intakes and associated health outcomes. Ann. N. Y. Acad. Sci. 1512, 10–28. https://doi.org/10.1111/nyas.14758 (2022).
Marshall, K., Teo, L., Shanahan, C., Legette, L. & Mitmesser, S. H. Inadequate calcium and vitamin D intake and osteoporosis risk in older Americans living in poverty with food insecurities. PLoS One. 15, e0235042. https://doi.org/10.1371/journal.pone.0235042 (2020).
Cembranel, F., Wagner, K. J. P., González-Chica, D. A. & d’Orsi, E. Education and income levels are associated with energy and micronutrient intake. Int. J. Vitam. Nutr. 90, 228–238. https://doi.org/10.1024/0300-9831/a000295 (2019).
Jacqmain, M., Doucet, E., Després, J. P., Bouchard, C. & Tremblay, A. Calcium intake, body composition, and lipoprotein-lipid concentrations in adults. Am. J. Clin. Nutr. 77, 1448–1452. https://doi.org/10.1093/ajcn/77.6.1448 (2003).
Zemel, M. B., Shi, H., Greer, B., Dirienzo, D. & Zemel, P. C. Regulation of adiposity by dietary calcium. FASEB J. 14, 1132–1138. https://doi.org/10.1096/fasebj.14.9.1132 (2000).
Moore, C. E., Radcliffe, J. D. & Liu, Y. Vitamin D intakes of adults differ by income, gender and race/ethnicity in the USA, 2007 to 2010. Public Health. Nutr. 17, 756–763. https://doi.org/10.1017/S1368980013002920 (2014).
Acknowledgements
This study received ethical approval and financial support from the Vice-Chancellor of Research and Technology at Tabriz University of Medical Sciences (Grant No. 67688). The authors extend their sincere appreciation to the nurses and administrative staff at Sina Hospital in Tabriz, Iran, for their invaluable assistance during data collection and participant coordination.
Funding
This work was supported by Tabriz University of Medical Sciences (Grant No. 67688 to Vahid Pakpour).
Author information
Authors and Affiliations
Contributions
All authors have taken responsibility for the content of the manuscript, agreed to its submission, reviewed the findings, and approved the final version. V.P. and A.FKh. conceptualized the study design, which was executed by E.M. and S.B. A.FKh. prepared the manuscript with contributions from all co-authors.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Farshbaf-Khalili, A., Malekmirzaei, E., Babaie, S. et al. The determinants of self-care behaviors and calcium–vitamin D intake in elderly women: a comparative study of osteoporosis and healthy counterparts. Sci Rep 15, 27290 (2025). https://doi.org/10.1038/s41598-025-12755-4
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41598-025-12755-4