Abstract
Aim:
This study aimed to compare the efficacy and safety between standard and low-dose tirofiban in the treatment of elderly high-risk non-ST-segment elevation acute coronary syndrome (NSTE-ACS) patients who underwent percutaneous coronary intervention (PCI).
Methods:
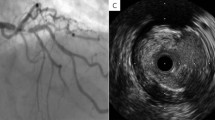
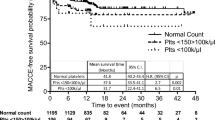
Ninety-four very elderly (≥80 years) high-risk patients with NSTE-ACS were randomly assigned to the standard or the low-dose group. Upstream tirofiban was administered intravenously with a bolus dose of 0.4 μg·kg−1·min−1 over a period of 30 min after the diagnosis had been confirmed, and was followed by a 36−48 h infusion of 0.10 μg·kg−1·min−1 or 0.075 μg·kg−1·min−1. PCI was performed within 24 h of admission. Platelet aggregation inhibition and thrombolysis in myocardial infarction (TIMI) grade flow were assessed. The major adverse cardiac events (MACEs), including death, myocardial infarction, recurrent angina and urgent target-vessel revascularization (TVR), were documented at 7 d, 30 d, and 6 months, and bleeding events were recorded at 7 d.
Results:
Although a significantly higher inhibition of platelet aggregation was observed in the standard-dose group (P<0.05), angiographic PCI success was similar between the two groups (P>0.05). The rate of MACEs was not significantly different at 7 days (2.1% vs 4.4%, P=0.61), 30 days (6.3% vs 8.7%, P=0.71) and 6 months (14.6% vs 17.4%, P=0.71). Major bleeding events were significantly higher in the standard-dose group (10.4% vs 0.0%, P=0.03).
Conclusion:
In very elderly high-risk patients with NSTE-ACS undergoing PCI, low-dose tirofiban offered about the same level of protection from major ischemic events that standard doses did, with less associated bleeding.
Similar content being viewed by others
Log in or create a free account to read this content
Gain free access to this article, as well as selected content from this journal and more on nature.com
or
References
Harrington RA, Becker RC, Cannon CP, Gutterman D, Lincoff AM, Popma JJ, et al. Antithrombotic therapy for non-ST-segment elevation acute coronary syndromes: American College of Chest Physicians Evidence-Based Clinical Practice Guidelines (8th Edition). Chest 2008; 133(6 Suppl): 670S–707S.
Inhibition of the platelet glycoprotein IIb/IIIa receptor with tirofiban in unstable angina and non-Q-wave myocardial infarction. Platelet Receptor Inhibition in Ischemic Syndrome Management in Patients Limited by Unstable Signs and Symptoms (PRISM-PLUS) Study Investigators. N Engl J Med 1998; 338: 1488–97.
Cannon CP, Weintraub WS, Demopoulos LA, Vicari R, Frey MJ, Lakkis N, et al. Comparison of early invasive and conservative strategies in patients with unstable coronary syndromes treated with the glycoprotein IIb/IIIa inhibitor tirofiban. N Engl J Med 2001; 344: 1879–87.
Bolognese L, Falsini G, Liistro F, Angioli P, Ducci K, Taddei T, et al. Randomized comparison of upstream tirofiban versus downstream high bolus dose tirofiban or abciximab on tissue-level perfusion and troponin release in high-risk acute coronary syndromes treated with percutaneous coronary interventions: the EVEREST trial. J Am Coll Cardiol 2006; 47: 522–8.
Task Force for Diagnosis and Treatment of Non-ST-Segment Elevation Acute Coronary Syndromes of European Society of Cardiology, Bassand JP, Hamm CW, Ardissino D, Boersma E, Budaj A, et al. Guidelines for the diagnosis and treatment of non-ST-segment elevation acute coronary syndromes. Eur Heart J 2007; 28: 1598–660.
Anderson JL, Adams CD, Antman EM, Bridges CR, Califf RM, Casey DE Jr, et al. ACC/AHA 2007 guidelines for the management of patients with unstable angina/non-ST-elevation myocardial infarction: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Writing Committee to Revise the 2002 Guidelines for the Management of Patients With Unstable Angina/Non-ST-Elevation Myocardial Infarction) developed in collaboration with the American College of Emergency Physicians, the Society for Cardiovascular Angiography and Interventions, and the Society of Thoracic Surgeons endorsed by the American Association of Cardiovascular and Pulmonary Rehabilitation and the Society for Academic Emergency Medicine. J Am Coll Cardiol 2007; 50: e1–e157.
Alexander KP, Newby LK, Cannon CP, Armstrong PW, Gibler WB, Rich MW, et al. Acute coronary care in the elderly, part I: Non-ST-segment-elevation acute coronary syndromes: a scientific statement for healthcare professionals from the American Heart Association Council on Clinical Cardiology: in collaboration with the Society of Geriatric Cardiology. Circulation 2007; 115: 2549–69.
Sadeghi HM, Grines CL, Chandra HR, Dixon SR, Boura JA, Dukkipati S, et al. Percutaneous coronary interventions in octogenarians. Glycoprotein IIb/IIIa receptor inhibitors' safety profile. J Am Coll Cardiol 2003; 42: 428–32.
Bach RG, Cannon CP, Weintraub WS, DiBattiste PM, Demopoulos LA, Anderson HV, et al. The effect of routine, early invasive management on outcome for elderly patients with non-ST-segment elevation acute coronary syndromes. Ann Intern Med 2004; 141: 186–95.
Kaehler J, Meinertz T, Hamm CW . Coronary interventions in the elderly. Heart 2006; 92: 1167–71.
Eikelboom JW, Mehta SR, Anand SS, Xie C, Fox KA, Yusuf S . Adverse impact of bleeding on prognosis in patients with acute coronary syndromes. Circulation 2006; 114: 774–82.
The Thrombolysis in Myocardial Infarction (TIMI) trial. Phase I findings. TIMI Study Group. N Engl J Med 1985; 312: 932–6.
Rao AK, Pratt C, Berke A, Jaffe A, Ockene I, Schreiber TL, et al. Thrombolysis in myocardial infarction (TIMI) trial-phase I: hemorrhagic manifestations and changes in plasma fibrinogen and the fibrinolytic system in patients treated with recombinant tissue plasminogen activator and streptokinase. J Am Coll Cardiol 1988; 11: 1–11.
Bavry AA, Kumbhani DJ, Rassi AN, Bhatt DL, Askari AT . Benefit of early invasive therapy in acute coronary syndromes: a meta-analysis of contemporary randomized clinical trials. J Am Coll Cardiol 2006; 48: 1319–25.
Stone GW, Bertrand ME, Moses JW, Ohman EM, Lincoff AM, Ware JH, et al. Routine upstream initiation vs deferred selective use of glycoprotein IIb/IIIa inhibitors in acute coronary syndromes: the ACUITY Timing Trial. JAMA 2007; 297: 591–602.
Kimmelstiel C, Badar J, Covic L, Waxman S, Weintraub A, Jacques S, et al. Pharmacodynamics and pharmacokinetics of the platelet GPIIb/IIIa inhibitor tirofiban in patients undergoing percutaneous coronary intervention: implications for adjustment of tirofiban and clopidogrel dosage. Thromb Res 2005; 116: 55–66.
Avezum A, Makdisse M, Spencer F, Gore JM, Fox KA, Montalescot G, et al. Impact of age on management and outcome of acute coronary syndrome: observations from the Global Registry of Acute Coronary Events (GRACE). Am Heart J 2005; 149: 67–73.
Alexander KP, Roe MT, Chen AY, Lytle BL, Pollack CV Jr, Foody JM, et al. Evolution in cardiovascular care for elderly patients with non-ST-segment elevation acute coronary syndromes: results from the CRUSADE National Quality Improvement Initiative. J Am Coll Cardiol 2005; 46: 1479–87.
Devlin G, Gore JM, Elliott J, Wijesinghe N, Eagle KA, Avezum A, et al. Management and 6-month outcomes in elderly and very elderly patients with high-risk non-ST-elevation acute coronary syndromes: the Global Registry of Acute Coronary Events. Eur Heart J 2008; 29: 1275–82.
Acknowledgements
We thank Mr Hong-zhi HUANG for language revision.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Lin, Yl., Chen, Ll., Luo, Yk. et al. Benefit of standard versus low-dose tirofiban for percutaneous coronary intervention in very elderly patients with high-risk acute coronary syndrome. Acta Pharmacol Sin 30, 553–558 (2009). https://doi.org/10.1038/aps.2009.38
Received:
Accepted:
Published:
Issue date:
DOI: https://doi.org/10.1038/aps.2009.38
Keywords
This article is cited by
-
Safety Profile and Complication Rates in Emergency Off-label Use of Tirofiban in Interventional Neuroradiology
Clinical Neuroradiology (2023)
-
Severe thrombocytopenia and alveolar hemorrhage represent two types of bleeding tendency during tirofiban treatment: case report and literature review
International Journal of Hematology (2012)