Abstract
Aim:
A novel hemostatic sealant based on the in situ gel formation of gelatin catalyzed by thrombin and crosslinked by transglutaminase was designed. The aim of this study was to investigate the efficacy of the hemostatic sealant in control of bleeding caused by liver trauma in dogs.
Methods:
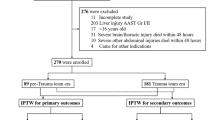
Hepatic trauma that mimicked the grade III–IV rupture of liver was made in 20 dogs. The traumatic lesion was topically administered the hemostatic sealant (treatment group, n=10), or a thrombin solution (control group, n=10). The time to achieve hemostasis and the blood loss were measured. Contrast-enhanced ultrasound (CEUS) examination was performed in each animal on d 3, d 7, and d 10 d postoperatively to study the healing of the lesions.
Results:
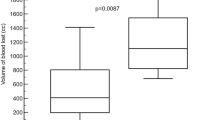
The mean time to achieve hemostasis in the treatment group was significantly shorter than that in the control group (1.20±0.33 vs 6.70±0.64 min, P<0.05). The mean blood loss in the treatment group was significantly less than that in the control group (47.22±8.61 vs 79.29±11.97 mL, P<0.05). In CEUS examination, the traumatic lesions in the treatment group became significantly smaller on d 3, and disappeared on d 7, whereas the lesions in the control group still existed on d 10. Ascites were never found during 10 d follow-up in the treatment group but were observed on d 3 and d 7 in the control group.
Conclusion:
Compared with thrombin, the novel hemostatic sealant shows much better efficacy in hemostasis and may promote wound healing in dog liver trauma.
Similar content being viewed by others
Log in or create a free account to read this content
Gain free access to this article, as well as selected content from this journal and more on nature.com
or
References
Hoyt DB, Bulger EM, Knudson MM, Morris J, Lerardi R, Sugerman HJ, et al. Death in the operating room: an analysis of a multi-center experience. J Trauma 1994; 37: 426–32.
Chapman WC, Singla N, Genyk Y, McNeil JW, Renkens KL, Revnolds TC, et al. A phase 3, randomized, double-blind comparative study of the efficacy and safety of topical recombinant human thrombin and bovine thrombin in surgical hemostasis. J Am Coll Surg 2007; 205: 256–65.
Spotnitz WD, Burks S . Hemostats, sealants, and adhesives: components of the surgical toolbox. Transfusion 2008; 48:1502–16.
Nasso G, Piancone F, Bonifazi R, Romano V, Visicchio G, De Filippo CM, et al. Prospective, randomized clinical trial of the FloSeal matrix sealant in cardiac surgery. Ann Thorac Surg 2009; 88: 1520–6.
Cravello L, Mimari R, Agostini A, Pelleqrin V, Limet L, Bartoli JM . Uterine artery embolisation to treat severe haemorrhage following legal abortion. J Gynecol Obstet Biol Reprod (Paris) 2007; 36: 500–2.
Renkens KL Jr, Payner TD, Leipzig TJ, Feuer H, Morone MA, Koers JM, et al. A multicenter, prospective, randomized trial evaluating a new hemostatic agent for spinal surgery. Spine (Phila Pa 1976) 2001; 26: 1645–50.
Leixnering M, Reichetseder J, Schultz A, Fiql M, Wassermann E, Thurnher M, et al. Gelatin thrombin granules for hemostasis in a severe traumatic liver and spleen rupture model in swine. J Trauma 2008; 64: 456–61.
Parviainen V, Joenväärä S, Tukiainen E, Llmakunnas M, Isoniemi H, Renkonen R . Relative quantification of several plasma proteins during liver transplantation surgery. J Biomed Biotechnol 2011; 2011: 248613.
Tagaya N, Abe A, Kubota K . Needlescopic surgery for liver, gallbladder and spleen diseases. J Hepatobiliary Pancreat Sci 2011; 18: 516–24.
Hick EJ, Morey AF, Harris RA, Morris MS . Gelatin matrix treatment of complex renal injuries in a porcine model. J Urol 2005; 173: 1801–4.
Gill IS, Ramani AP, Spaliviero M, Xu M, Finelli A, Kaouk JH, et al. Improved hemostasis during laparoscopic partial nephrectomy using gelatin matrix thrombin sealant. Urology 2005; 65: 463–6.
Desai PJ, Maynes LJ, Zuppan C, Berqe, KA, Torrey R, et al. Hand-assisted laparoscopic partial nephrectomy in the porcine model using gelatin matrix hemostatic sealant without hilar occlusion. J Endourol 2005; 19: 566–9.
Baumann A, Caversaccio M . Hemostasis in endoscopic sinus surgery using a specific gelatin-thrombin based agent (FloSeal). Rhinology 2003; 41: 244–9.
Angioli R, Muzii L, Montera R, Damiani P, Bellati F, Plotti F, et al. Feasibility of the use of novel matrix hemostatic sealant (FloSeal) to achieve hemostasis during laparoscopic excision of endometrioma. J Minim Invasive Gynecol 2009; 16: 153–6.
Madhuri TK, Tailor A, Butler-Manuel S . Use of surgical sealant in debulking surgery for advanced ovarian carcinoma-case report. Eur J Gynaecol Oncol 2010; 31: 582–3.
Chen T, Embree HD, Brown EM, Taylor MM, Payne GF . Enzyme-catalyzed gel formation of gelatin and chitosan: potential for in situ applications. Biomaterials 2003; 24: 2831–41.
Ballantyne B, Jordan SL . Toxicological, medical, and industrial hygiene aspects of glutaraldehyde with particular reference to its biocidal use in cold sterilization procedures. J Appl Toxicol 2001; 21: 131–51.
Babin H, Dickinson E . Influence of transglutaminase treatment on the thermoreversible gelation of gelatin. Food Hydrocoll 2001; 15: 271–6.
Motoki M, Seguro, K . Transglutaminase and its use for food processing trends. Food Sci Technol 1998; 9: 204–10.
Yokoyama K, Nio N, Kikuchi Y . Properties and applications of microbial transglutaminase. Appl Microbiol Biotechnol 2004; 64: 447–54.
Jurgensen K, Aeschlimann D, Cavin V, Genge M, Hunziker EB . A new biological glue for cartilage-cartilage interfaces: tissue transglutaminase. J Bone Joint Surg Am 1997; 79: 185–93.
Tan Y, Chen X, Huang JH, Huang DP, Wang JH . Eficacy of microbial transglutaminase on wound healing in rats. Chin Biotech 2007; 27: 85–90.
Karpuj MV, Becher NW, Springer JE, Chabas D, Youssef S, Pedotti R, et al. Prolonged survival and decreased abnormal movements in transgenic model of Huntington disease, with administration of the transglutaminase inhibitor cystamine. Nat Med 2002; 8: 143–9.
Fuchsbauer HL, Gerber U, Engelmann J, Seeger T, Sinks C, Hecht T . Influence of gelatin matrices cross-linked with transglutaminase on the properties of an enclosed bioactive material using beta-galactosidase as model system. Biomaterials 1996; 17: 1481–8.
Lim LT, Mine Y, Tung MA . Barrier and tensile properties of transglutaminase cross-linked gelatin films as affected by relative humidity, temperature, and glycerol content. J Food Sci 1999; 64: 616–22.
Bohidar HB, Maity S . Polarized light scattering study from gelatin solutions and gels. Eur Polym J 1998; 34: 1361–70.
Liu Y, Kopelman D, Wu LQ, Hijji K, Attar I, Preiss-Bloom O, et al. Biomimetic sealant based on gelatin and microbial transglutaminase: an initial in vivo investigation. J Biomed Mater Res B Appl Biomater 2009; 91: 5–16.
Moore EE, Cogbill TH, Jurkovich GJ, Shackford SR, Malangoni MA, Champion HR . Organ injury scaling: spleen and liver (1994 revision). J Trauma 1995; 38: 323–4.
Morel DR, Schwieger I, Hohn L, Terrettaz J, Llull JB, Cornioley YA, et al. Human pharmacokinetics and safety evaluation of SonoVue, a new contrast agent for ultrasound imaging. Invest Radiol 2000; 35: 80–5.
Hutchinson RW, Broughton D, Barbolt TA, Prandl T, Muench T, Rockar R, et al. Hemostatic effectiveness of Fibrin pad after partial nephrectomy in swine. J Surg Res 2011; 167: 291–8.
Acheson EM, Kheirabadi BS, Deguzman R, Dick EJ Jr, Holcomb JB . Comparison of hemorrhage control agents applied to lethal extremity arterial hemorrhages in swine. J Trauma 2005; 59: 865–74.
Achneck HE, Sileshi B, Jamiolkowski RM, Albala DM, Shapiro MJ, Larson JH . A comprehensive review of topical hemostatic agents: efficacy and recommendations for use. Ann Surg 2010; 251: 217–28.
Sarfati MR, DiLorenzo DJ, Kraiss LW, Galt SW . Severe coagulopathy following intraoperative use of topical thrombin. Ann Vasc Surg 2004; 18: 349–51.
Tomizawa Y . Clinical benefits and risk analysis of topical hemostats: a review. J Artif Organs 2005; 8: 137–42.
Bennett SL, Melanson DA, Torchiana DF, Wiseman DM, Sawhney AS . Next-generation hydrogel films as tissue sealants and adhesion barriers. J Card Surg 2003; 18: 494–9.
Kakinoki S, Taguchi T . Antitumor effect of an injectable in-situ forming drug delivery system composed of a novel tissue adhesive containing doxorubicin hydrochloride. Eur J Pharm Biopharm 2007; 67: 676–81.
Martinez-de-la-Casa JM, Rayward O, Saenz-Frances F, Mendez C, Bueso ES, Garcia-Feijoo J . Use of a fibrin adhesive for conjunctival closure in trabeculectomy. Acta Ophthalmol 2012. DOI: 10.1111/j.1755-3768.2012.02436.x.
Pursifull NF, Morey AF . Tissue glues and nonsuturing techniques. Curr Opin Urol 2007; 17: 396–401.
Pusateri AE, Holcomb JB, Kheirabadi BS, Alam HB, Wade CE, Ryan KL . Making sense of the preclinical literature on advanced hemostatic products. J Trauma 2006; 60: 674–82.
Davis NE, Ding S, Forster RE, Pinkas DM, Barron AE . Modular enzymatically crosslinked protein polymer hydrogels for in situ gelation. Biomaterials 2010; 31: 7288–97.
Chen TH, Embree HD, Brown EM, Taylor MM, Payne GF . Enzyme-catalyzed gel formation of gelatin and chitosan: Potential for in situ applications. Biomaterials 2003; 24: 2831–41.
McDermott MK, Chen TH, Williams CM, Markley KM, Payne GF . Mechanical properties of biomimetic tissue adhesive based on the microbial transglutaminase-catalyzed crosslinking of gelatin. Biomacromolecules 2004; 5: 1270–9.
Chen T, Janjua R, McDermott MK, Bernstein SL, Steidl SM, Payne GF . Gelatin-based biomimetic tissue adhesive. Potential for retinal reattachment. J Biomed Mater Res B Appl Biomater 2006; 77: 416–22.
Catalano O, Lobianco R, Rase MM, Siani A . Blunt hepatic trauma: evaluation with contrast-enhanced sonography: sonographic findings and clinical application. J Ultrasound Med 2005; 24: 299–310.
Yekun L, Shasha W, Xiangsheng Z, Qi C, Guoxin L, Feng H . Contrast-enhanced ultrasound for blunt hepatic trauma: an animal experiment. Am J Emerg Med 2010; 28: 828–33.
Valentino M, Serrra C, Pavilica P, Barozzi L . Contrast-enhanced ultrasound for blunt abdominal trauma. Semin Ultrasound CT MR 2007; 28: 130–40.
Acknowledgements
The financial support of the National Natural Science Foundation of China (No 81071279) is greatly acknowledged.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Xie, X., Tian, Jk., Lv, Fq. et al. A novel hemostatic sealant composed of gelatin, transglutaminase and thrombin effectively controls liver trauma-induced bleeding in dogs. Acta Pharmacol Sin 34, 983–988 (2013). https://doi.org/10.1038/aps.2013.17
Received:
Accepted:
Published:
Issue date:
DOI: https://doi.org/10.1038/aps.2013.17
Keywords
This article is cited by
-
Plasma-based fast-gelling biohybrid gels for biomedical applications
Scientific Reports (2019)