Abstract
Background:
Appearance of glandular breast tissue may be difficult to distinguish from fat tissue by palpation, especially in obese girls. To our knowledge, validation of the clinical assessment of pubertal breast stages by magnetic resonance imaging (MRI) has never been performed. Our objective was to report normative data of glandular breast tissue volume and validate the clinical evaluation of pubertal breast staging by MRI of breast tissue and to evaluate circulating reproductive hormone levels and estrogen-dependent transabdominal ultrasound (TAUS) parameters as markers of glandular breast tissue.
Methods:
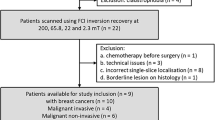
Glandular breast tissue volume quantified by MRI and breast stage evaluation was performed in 100 healthy peripubertal girls. Circulating levels of follicle-stimulating hormone (FSH), luteinizing hormone (LH), inhibin B, and estradiol were measured by immunoassays. Ovarian volume, uterine volume, and endometrial thickness were assessed by TAUS.
Results:
Glandular breast tissue volume was positively associated with Tanner stages (r = 0.858, P < 0.001). The sensitivity and specificity of breast palpation to detect presence of glandular breast tissue using MRI as gold standard were 96 and 95%, respectively. The best parameters to distinguish prepubertal girls from girls with breast development were: LH (area under the curve (AUC) by receiver operating characteristic analysis = 0.871), inhibin B (AUC = 0.847) and estradiol (AUC = 0.830).
Conclusion:
Clinical palpation reliably detects the presence of glandular breast tissue.
Similar content being viewed by others
Log in or create a free account to read this content
Gain free access to this article, as well as selected content from this journal and more on nature.com
or
References
Marshall WA, Tanner JM. Variations in pattern of pubertal changes in girls. Arch Dis Child 1969;44:291–303.
Rasmussen AR, Wohlfahrt-Veje C, Tefre de Renzy-Martin K, et al. Validity of self-assessment of pubertal maturation. Pediatrics 2015;135:86–93.
Schlossberger NM, Turner RA, Irwin CE Jr . Validity of self-report of pubertal maturation in early adolescents. J Adolesc Health 1992;13:109–13.
Aksglaede L, Sørensen K, Petersen JH, Skakkebaek NE, Juul A. Recent decline in age at breast development: the Copenhagen Puberty Study. Pediatrics 2009;123:e932–9.
Biro FM, Galvez MP, Greenspan LC, et al. Pubertal assessment method and baseline characteristics in a mixed longitudinal study of girls. Pediatrics 2010;126:e583–90.
Herman-Giddens ME. Recent data on pubertal milestones in United States children: the secular trend toward earlier development. Int J Androl 2006;29:241–6; discussion 286–90.
Sun SS, Schubert CM, Liang R, et al. Is sexual maturity occurring earlier among U.S. children? J Adolesc Health 2005;37:345–55.
Jaruratanasirikul S, Chanpong A, Tassanakijpanich N, Sriplung H. Declining age of puberty of school girls in southern Thailand. World J Pediatr 2014;10:256–61.
Herman-Giddens ME, Slora EJ, Wasserman RC, et al. Secondary sexual characteristics and menses in young girls seen in office practice: a study from the Pediatric Research in Office Settings network. Pediatrics 1997;99:505–12.
Sun SS, Schubert CM, Chumlea WC, et al. National estimates of the timing of sexual maturation and racial differences among US children. Pediatrics 2002;110:911–9.
Euling SY, Herman-Giddens ME, Lee PA et al. Examination of US puberty-timing data from 1940 to 1994 for secular trends: panel findings. Pediatrics 2008;121:172–91.
Neely EK, Wilson DM, Lee PA, Stene M, Hintz RL. Spontaneous serum gonadotropin concentrations in the evaluation of precocious puberty. J Pediatr 1995;127:47–52.
Boisen KA, Kaleva M, Main KM, et al. Difference in prevalence of congenital cryptorchidism in infants between two Nordic countries. Lancet 2004;363:1264–9.
Chellakooty M, Schmidt IM, Haavisto AM, et al. Inhibin A, inhibin B, follicle-stimulating hormone, luteinizing hormone, estradiol, and sex hormone-binding globulin levels in 473 healthy infant girls. J Clin Endocrinol Metab 2003;88:3515–20.
Mouritsen A, Johansen ML, Wohlfahrt-Veje C, et al. Determination of adrenal volume by MRI in healthy children: associations with age, body size, pubertal stage and serum levels of adrenal androgens. Clin Endocrinol (Oxf) 2014;81:183–9.
Hagen CP, Mouritsen A, Mieritz MG, et al. Uterine volume and endometrial thickness in healthy girls evaluated by ultrasound (3-dimensional) and magnetic resonance imaging. Fertil Steril 2015;104:452–9.e2.
Wohlfahrt-Veje C, Tinggaard J, Winther K, et al. Body fat throughout childhood in 2647 healthy Danish children: agreement of BMI, waist circumference, skinfolds with dual X-ray absorptiometry. Eur J Clin Nutr 2014;68:664–70.
Slaughter MH, Lohman TG, Boileau RA, et al. Skinfold equations for estimation of body fatness in children and youth. Hum Biol 1988;60:709–23.
Hagen CP, Mouritsen A, Mieritz MG, et al. Circulating AMH reflects ovarian morphology by magnetic resonance imaging and 3D ultrasound in 121 healthy girls. J Clin Endocrinol Metab 2015;100:880–90.
Author information
Authors and Affiliations
Corresponding author
Supplementary information
Supplementary Figure (download JPEG )
(JPEG 1198 kb)
Rights and permissions
About this article
Cite this article
Fugl, L., Hagen, C., Mieritz, M. et al. Glandular breast tissue volume by magnetic resonance imaging in 100 healthy peripubertal girls: evaluation of clinical Tanner staging. Pediatr Res 80, 526–530 (2016). https://doi.org/10.1038/pr.2016.125
Received:
Accepted:
Published:
Issue date:
DOI: https://doi.org/10.1038/pr.2016.125
This article is cited by
-
Early breast development in overweight girls: does estrogen made by adipose tissue play a role?
International Journal of Obesity (2019)
-
Anthropometry, DXA, and leptin reflect subcutaneous but not visceral abdominal adipose tissue on MRI in 197 healthy adolescents
Pediatric Research (2017)