Abstract
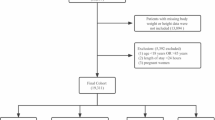
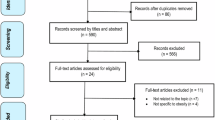
Recent studies have suggested that obesity might be protective in specific conditions such as critical illness; however, there are controversial data in critically ill children with obesity. The aim of this study was to investigate the association of obesity with mortality and other outcomes in these patients. We conducted a systematic review of observational studies investigating obesity in critically ill children, published by August 2017 in PubMed and Scopus. After screening documents, 15 articles with 142119 patients were included in the systematic review and meta-analysis. The results were reported with odds ratio (OR) or standard mean difference (SMD). The primary outcome was mortality and the secondary outcomes were length of ICU stay (ICU LOS), length of hospital stay (hospital LOS), and duration of mechanical ventilation (MV). The analysis showed that critically ill children without obesity had lower risk of mortality compared to patients with obesity (OR 0.79, 95% CI 0.64 to 0.97, P = 0.025, I2 = 35.2%). Hospital LOS was also significantly lower in children without obesity (pooled SMD −0.12, 95% CI −0.21 to −0.04, P = 0.004, I2 = 8.1%). There were no differences in ICU LOS (95% CI −0.19 to 0.01, P = 0.083) and duration of MV (95% CI −0.22 to 0.03, P = 0.136) between critically ill children with and without obesity. In conclusion, the current systematic review and meta-analysis revealed that critically ill children with obesity have higher risk of mortality and length of hospital stay compared to the group without obesity. Further prospective studies are essential to elucidate the role of obesity and underlying mechanisms in predicting outcomes of critically ill children.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
References
Hales CM, Fryar CD, Carroll MD, Freedman DS, Ogden CL. Trends in obesity and severe obesity prevalence in us youth and adults by sex and age, 2007–2008 to 2015–2016. JAMA. 2018;319:1723–5.
Reilly JJ, Kelly J. Long-term impact of overweight and obesity in childhood and adolescence on morbidity and premature mortality in adulthood: systematic review. Int J Obes. 2011;35:891–8.
Brown CV, Velmahos GC. The consequences of obesity on trauma, emergency surgery, and surgical critical care. World J Emerg Surg. 2006;1:27.
Patel JJ, Rosenthal MD, Miller KR, Codner P, Kiraly L, Martindale RG. The critical care obesity paradox and implications for nutrition support. Curr Gastroenterol Rep. 2016;18:45.
Shashaty MG, Stapleton RD. Physiological and management implications of obesity in critical illness. Ann Am Thorac Soc. 2014;11:1286–97.
Pickkers P, de Keizer N, Dusseljee J, Weerheijm D, van der Hoeven JG, Peek N. Body mass index is associated with hospital mortality in critically ill patients: an observational cohort study. Crit Care Med. 2013;41:1878–83.
Ward SL, Gildengorin V, Valentine SL, Sapru A, Curley MA, Thomas N, et al. Impact of weight extremes on clinical outcomes in pediatric acute respiratory distress syndrome. Crit Care Med. 2016;44:2052–9.
Bechard LJ, Rothpletz-Puglia P, Touger-Decker R, Duggan C, Mehta NM. Influence of obesity on clinical outcomes in hospitalized children: a systematic review. JAMA Pediatr. 2013;167:476–82.
Kuczmarski RJ, Ogden CL, Grummer-Strawn LM, Flegal KM, Guo SS, Wei R, et al. CDC growth charts: United States. Adv Data. 2000;314:1–27.
WHO Child Growth. Standards based on length/height, weight and age. Acta Paediatr Suppl. 2006;76–85.
de Onis M, Onyango AW, Borghi E, Siyam A, Nishida C, Siekmann J. Development of a WHO growth reference for school-aged children and adolescents. Bull World Health Organ. 2007;85:660–7.
Wells G, Shea B, O'Connell D, Peterson J, Welch V, Losos M, et al. The Newcastle-Ottawa Scale (NOS) for assessing the quality of nonrandomised studies in meta-analyses. 2011. http://www.ohri.ca/programs/clinical_epidemiology/oxford.asp.
Vaughan N, Tweed J, Greenwell C, Notrica DM, Langlais CS, Peter SD, et al. The impact of morbid obesity on solid organ injury in children using the ATOMAC protocol at a pediatric level I trauma center. J Pediatr Surg. 2017;52:345–8.
Chen MY, Yang YJ. Being underweight is an independent risk factor for poor outcomes among acutely critically ill children. Nutr Clin Pract. 2017;33:433–8.
Martinez EE, Ariagno KA, Stenquist N, Anderson D, Munoz E, Mehta NM. Energy and protein delivery in overweight and obese children in the pediatric intensive care unit. Nutr Clin Pract. 2017;32:414–9.
Anton-Martin P, Papacostas M, Lee E, Nakonezny PA, Green ML. Underweight status is an independent predictor of in-hospital mortality in pediatric patients on extracorporeal membrane oxygenation. JPEN J Parenter Enteral Nutr. 2016; pii: 0148607116673185.
Bechard LJ, Duggan C, Touger-Decker R, Parrott JS, Rothpletz-Puglia P, Byham-Gray L, et al. Nutritional status based on body mass index is associated with morbidity and mortality in mechanically ventilated critically ill children in the PICU. Crit Care Med. 2016;44:1530–7.
Ross PA, Newth CJ, Leung D, Wetzel RC, Khemani RG. Obesity and mortality risk in critically Ill children. Pediatrics . 2016;137:e20152035.
Ross E, Burris A, Murphy JT. Obesity and outcomes following burns in the pediatric population. J Pediatr Surg. 2014;49:469–73.
Goh VL, Wakeham MK, Brazauskas R, Mikhailov TA, Goday PS. Obesity is not associated with increased mortality and morbidity in critically ill children. JPEN J Parenter Enter Nutr. 2013;37:102–8.
Alselaim N, Malaekah H, Saade M, Hussein M, Altokhais T, Albedah K, et al. Does obesity impact the pattern and outcome of trauma in children? J Pediatr Surg. 2012;47:1404–9.
Backstrom IC, MacLennan PA, Sawyer JR, Creek AT, Rue LW III, Gilbert SR. Pediatric obesity and traumatic lower-extremity long-bone fracture outcomes. J Trauma acute care Surg. 2012;73:966–71.
Kraft R, Herndon DN, Williams FN, Al-Mousawi AM, Finnerty CC, Jeschke MG. The effect of obesity on adverse outcomes and metabolism in pediatric burn patients. Int J Obes. 2012;36:485–90.
Srinivasan V, Nadkarni VM, Helfaer MA, Carey SM, Berg RA, American Heart Association National Registry of Cardiopulmonary Resuscitation I. Childhood obesity and survival after in-hospital pediatric cardiopulmonary resuscitation. Pediatrics. 2010;125:e481–8.
Rana AR, Michalsky MP, Teich S, Groner JI, Caniano DA, Schuster DP. Childhood obesity: a risk factor for injuries observed at a level-1 trauma center. J Pediatr Surg. 2009;44:1601–5.
Brown CV, Neville AL, Salim A, Rhee P, Cologne K, Demetriades D. The impact of obesity on severely injured children and adolescents. J Pediatr Surg. 2006;41:88–91.
Sterne JA, Gavaghan D, Egger M. Publication and related bias in meta-analysis: power of statistical tests and prevalence in the literature. J Clin Epidemiol. 2000;53:1119–29.
Tait AR, Voepel-Lewis T, Burke C, Kostrzewa A, Lewis I. Incidence and risk factors for perioperative adverse respiratory events in children who are obese. Anesthesiology. 2008;108:375–80.
Oliveros H, Villamor E. Obesity and mortality in critically ill adults: a systematic review and meta-analysis. Obesity. 2008;16:515–21.
Hogue CW Jr., Stearns JD, Colantuoni E, Robinson KA, Stierer T, Mitter N, et al. The impact of obesity on outcomes after critical illness: a meta-analysis. Intensive Care Med. 2009;35:1152–70.
Akinnusi ME, Pineda LA, El Solh AA. Effect of obesity on intensive care morbidity and mortality: a meta-analysis. Crit Care Med. 2008;36:151–8.
Gruberg L, Weissman NJ, Waksman R, Fuchs S, Deible R, Pinnow EE, et al. The impact of obesity on the short-term and long-term outcomes after percutaneous coronary intervention: the obesity paradox? J Am Coll Cardiol. 2002;39:578–84.
Preiser JC, Ichai C, Orban JC, Groeneveld AB. Metabolic response to the stress of critical illness. Br J Anaesth. 2014;113:945–54.
Marques MB, Langouche L. Endocrine, metabolic, and morphologic alterations of adipose tissue during critical illness. Crit Care Med. 2013;41:317–25.
Grigoras I, Branisteanu D, Ungureanu D, Rusu D, Ristescu I. Early dynamics of leptin plasma level in surgical critically ill patients: a prospective comparative study. Chir (Bucur). 2014;109:66–72.
Bornstein S, Licinio J, Tauchnitz R, Engelmann L, Negrao A, Gold P, et al. Plasma leptin levels are increased in survivors of acute sepsis: associated loss of diurnal rhythm in cortisol and leptin secretion. J Clin Endocrinol & Metab. 1998;83:280–3.
Arnalich F, López J, Codoceo R, Jiménez M, Madero R, Montiel C. Relationship of plasma leptin to plasma cytokines and human survival in sepsis and septic shock. J Infect Dis. 1999;180:908–11.
Koch A, Sanson E, Voigt S, Helm A, Trautwein C, Tacke F. Serum adiponectin upon admission to the intensive care unit may predict mortality in critically ill patients. J Crit Care. 2011;26:166–74.
Kaplan JM, Denenberg A, Monaco M, Nowell M, Wong H, Zingarelli B. Changes in peroxisome proliferator-activated receptor-gamma activity in children with septic shock. Intensive Care Med. 2010;36:123–30.
Flegal KM, Ioannidis JPA. The obesity paradox: a misleading term that should be abandoned. Obesity. 2018;26:629–30.
Li S, Wang Z, Huang J, Fan J, Du H, Liu L, et al. Systematic review of prognostic roles of body mass index for patients undergoing lung cancer surgery: does the 'obesity paradox' really exist? Eur J Cardiothorac Surg. 2017;51:817–28.
Acknowledgements
This manuscript has been supported by Iran University of Medical Sciences.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Alipoor, E., Hosseinzadeh-Attar, M.J., Yaseri, M. et al. Association of obesity with morbidity and mortality in critically ill children: a systematic review and meta-analysis of observational studies. Int J Obes 43, 641–651 (2019). https://doi.org/10.1038/s41366-019-0319-y
Received:
Revised:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41366-019-0319-y
This article is cited by
-
Height status matters for risk of mortality in critically ill children
Journal of Intensive Care (2024)
-
Association of obesity with mortality and clinical outcomes in children and adolescents with transplantation: A systematic review and meta-analysis
Reviews in Endocrine and Metabolic Disorders (2021)