Abstract
Background/objectives
Reference data for bioelectrical impedance analysis (BIA) parameters remain limited in youth, making sarcopenia assessment challenging. This study aimed to establish BIA reference values and determine sarcopenia cutoff points and prevalence in youth.
Subjects/methods
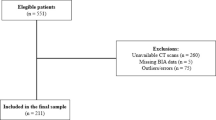
This cross-sectional study analyzed 1451 youth aged 10–25 years who underwent BIA using data from a nationwide survey. Reference values for body composition were established using the least mean squares method, which estimates age-specific percentiles. Sarcopenia was defined using skeletal muscle mass index (SMI), fat-free mass-to-fat ratio (FFM-MFR), and appendicular skeletal muscle mass-to-fat ratio (ASM-MFR) with age- and sex-specific cutoff values.
Results
Muscle-related parameters, including fat-free mass, fat-free mass index, ASM, and SMI, increased during puberty in both sexes, with a more pronounced increase in males, followed by a plateau or gradual increase after adolescence. Fat-related parameters, including fat mass, fat mass index, and percentage body fat, decreased until age 14 years in males before increasing, whereas in females, they increased until adolescence and declined after early adulthood. The prevalence of sarcopenia was 2.05% in males and 1.04% in females based on SMI, 5.21% in males and 6.38% in females based on FFM-MFR, and 5.06% in males and 5.79% in females based on ASM-MFR.
Conclusions
This study established BIA-based body composition reference values for youth using nationally representative data, identified age- and sex-specific sarcopenia cutoff points and prevalence estimates, and highlighted age- and sex-specific differences. These findings provide a valuable resource for the early identification and management of sarcopenia in youth.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
Data availability
Data can be made available upon request to the corresponding author.
Code availability
The SAS and R scripts used for the analysis are available from the corresponding author upon reasonable request.
References
Joppa P, Tkacova R, Franssen FM, Hanson C, Rennard SI, Silverman EK, et al. Sarcopenic obesity, functional outcomes, and systemic inflammation in patients with chronic obstructive pulmonary disease. J Am Med Dir Assoc. 2016;17:712–8.
Coelho-Júnior HJ, Marques FL, Sousa CV, Marzetti E, Aguiar SDS. Age- and sex-specific normative values for muscle mass parameters in 18,625 Brazilian adults. Front Public Health. 2023;11:1287994.
Park SH, Kim MJ, Kim B, Lee GY, Seo YM, Park JY, et al. Association between Disability and Edema Index Values in Rural Older Adult Osteosarcopenia Patients. Yonsei Med J. 2022;63:873–80.
McCarthy HD, Samani-Radia D, Jebb SA, Prentice AM. Skeletal muscle mass reference curves for children and adolescents. Pediatr Obes. 2014;9:249–59.
Brantlov S, Ward LC, Jødal L, Rittig S, Lange A. Critical factors and their impact on bioelectrical impedance analysis in children: a review. J Med Eng Technol. 2017;41:22–35.
Nakao T, Komiya S. Reference norms for a fat-free mass index and fat mass index in the Japanese child population. J Physiol Anthropol Appl Human Sci. 2003;22:293–8.
Zembura M, Matusik P. Sarcopenic obesity in children and adolescents: a systematic review. Front Endocrinol. 2022;13:914740.
Cruz-Jentoft AJ, Bahat G, Bauer J, Boirie Y, Bruyère O, Cederholm T, et al. Sarcopenia: revised European consensus on definition and diagnosis. Age Ageing. 2019;48:16–31.
Chen LK, Woo J, Assantachai P, Auyeung TW, Chou MY, Iijima K, et al. Asian Working Group for Sarcopenia: 2019 Consensus Update on Sarcopenia Diagnosis and Treatment. J Am Med Dir Assoc. 2020;21:300–7.e2.
Campa F, Gobbo LA, Stagi S, Cyrino LT, Toselli S, Marini E, et al. Bioelectrical impedance analysis versus reference methods in the assessment of body composition in athletes. Eur J Appl Physiol. 2022;122:561–89.
Xiao J, Purcell SA, Prado CM, Gonzalez MC. Fat mass to fat-free mass ratio reference values from NHANES III using bioelectrical impedance analysis. Clin Nutr. 2018;37:2284–7.
Kim JH, Yun S, Hwang SS, Shim JO, Chae HW, Lee YJ, et al. The 2017 Korean National Growth Charts for children and adolescents: development, improvement, and prospects. Korean J Pediatr. 2018;61:135–49.
Janssen I, Heymsfield SB, Ross R. Low relative skeletal muscle mass (sarcopenia) in older persons is associated with functional impairment and physical disability. J Am Geriatr Soc. 2002;50:889–96.
Gould H, Brennan SL, Kotowicz MA, Nicholson GC, Pasco JA. Total and appendicular lean mass reference ranges for Australian men and women: the Geelong osteoporosis study. Calcif Tissue Int. 2014;94:363–72.
Zhao Y, Gong JX, Ji YT, Zhao XY, He L, Cai SZ, et al. Cross-sectional study of characteristics of body composition of 24,845 children and adolescents aged 3-17 years in Suzhou. BMC Pediatr. 2023;23:358.
Worldwide trends in body-mass index, underweight, overweight, and obesity from 1975 to 2016: a pooled analysis of 2416 population-based measurement studies in 128·9 million children, adolescents, and adults. Lancet. 2017;390:2627–42.
Mensah GA, Roth GA, Fuster V. The Global Burden of Cardiovascular Diseases and Risk Factors: 2020 and Beyond. J Am Coll Cardiol. 2019;74:2529–32.
Gätjens I, Schmidt SCE, Plachta-Danielzik S, Bosy-Westphal A, Müller MJ. Body composition characteristics of a load-capacity model: age-dependent and sex-specific percentiles in 5- to 17-year-old children. Obes Facts. 2021;14:593–603.
Hanssen B, Peeters N, Vandekerckhove I, De Beukelaer N, Bar-On L, Molenaers G, et al. The contribution of decreased muscle size to muscle weakness in children with spastic cerebral palsy. Front Neurol. 2021;12:692582.
Maloney SJ. The relationship between asymmetry and athletic performance: a critical review. J Strength Cond Res. 2019;33:2579–93.
Ozel S, Switzer L, Macintosh A, Fehlings D. Informing evidence-based clinical practice guidelines for children with cerebral palsy at risk of osteoporosis: an update. Dev Med Child Neurol. 2016;58:918–23.
Kweon S, Kim Y, Jang MJ, Kim Y, Kim K, Choi S, et al. Data resource profile: the Korea National Health and Nutrition Examination Survey (KNHANES). Int J Epidemiol. 2014;43:69–77.
Haam JH, Kim BT, Kim EM, Kwon H, Kang JH, Park JH, et al. Diagnosis of Obesity: 2022 Update of Clinical Practice Guidelines for Obesity by the Korean Society for the Study of Obesity. J Obes Metab Syndr. 2023;32:121–9.
Korea Disease C, Prevention A. Korea National Health and Nutrition Examination Survey (KNHANES): Performing Institutions. Knhanes.
Heymsfield SB, Brown J, Ramirez S, Prado CM, Tinsley GM, Gonzalez MC. Are Lean Body Mass and Fat-Free Mass the Same or Different Body Components? A Critical Perspective. Adv Nutr. 2024;15:100335.
Heymsfield SB, Wang Z, Baumgartner RN, Ross R. Human body composition: advances in models and methods. Annu Rev Nutr. 1997;17:527–58.
AlMasud AA, Alothman SA, Benajiba N, Alqahtani S, Alatr AA, Alshatowy AA, et al. Relationship of fat mass index and fat free mass index with body mass index and association with sleeping patterns and physical activity in Saudi young adults women. J Health Popul Nutr. 2025;44:64.
Steffl M, Chrudimsky J, Tufano JJ. Using relative handgrip strength to identify children at risk of sarcopenic obesity. PLoS ONE. 2017;12:e0177006.
Cole TJ, Green PJ. Smoothing reference centile curves: the LMS method and penalized likelihood. Stat Med. 1992;11:1305–19.
Chumlea WC, Guo SS, Kuczmarski RJ, Flegal KM, Johnson CL, Heymsfield SB, et al. Body composition estimates from NHANES III bioelectrical impedance data. Int J Obes Relat Metab Disord. 2002;26:1596–609.
Schmidt SC, Bosy-Westphal A, Niessner C, Woll A. Representative body composition percentiles from bioelectrical impedance analyses among children and adolescents. The MoMo study. Clin Nutr. 2019;38:2712–20.
Lim JS, Shin CH, Yang SW. Changes and Their Correlations of Body Compositions and Serum Leptin Concentrations according to the Progression of Tanner Stage in Healthy Children and Adolescents. J Korean Soc Pediatr Endocrinol. 2003;8:162–73.
Miller BS, Sarafoglou K, Addo OY. Development of tanner stage-age adjusted CDC height curves for research and clinical applications. J Endocr Soc. 2020;4:bvaa098.
Guthold R, Stevens GA, Riley LM, Bull FC. Global trends in insufficient physical activity among adolescents: a pooled analysis of 298 population-based surveys with 1·6 million participants. Lancet Child Adolesc Health. 2020;4:23–35.
Song K, Kwon A, Chae HW, Suh J, Choi HS, Choi Y, et al. Vitamin D status is associated with bone mineral density in adolescents: Findings from the Korea National Health and Nutrition Examination Survey. Nutr Res. 2021;87:13–21.
Song K, Park G, Choi Y, Oh JS, Choi HS, Suh J, et al. Association of vitamin D status and physical activity with lipid profile in Korean children and adolescents: a population-based study. Children. 2020;7:241.
Deurenberg P, Yap M, van Staveren WA. Body mass index and percent body fat: a meta analysis among different ethnic groups. Int J Obes Relat Metab Disord. 1998;22:1164–71.
Lee DH, Kang SC, Hwang SS, Lee YJ, Kim HY, Lee SY, et al. Establishing reference values for percentage of appendicular skeletal muscle mass and their association with metabolic syndrome in Korean adolescents. Ann Pediatr Endocrinol Metab. 2023;28:237–44.
Lee TK, Kim YM, Lim HH. Comparison of anthropometric, metabolic, and body compositional abnormalities in Korean children and adolescents born small, appropriate, and large for gestational age: a population-based study from KNHANES V (2010-2011). Ann Pediatr Endocrinol Metab. 2024;29:29–37.
Author information
Authors and Affiliations
Contributions
Kyungchul Song: Conceptualization, Methodology, Formal analysis, Investigation, and Writing–original draft; Eunju Lee, Hye Sun Lee, and Hana Lee: Resources, Data curation and Formal analysis; Joon Young Kim and Youngha Choi: Methodology; and Hyun Wook Chae: Conceptualization, Methodology, Writing–review & editing, and Supervision.
Corresponding author
Ethics declarations
Competing interests
All authors declare no conflicts of interest.
Ethics approval and consent to participate
All methods were performed in accordance with the relevant guidelines and regulations, including the principles of the Declaration of Helsinki. This study was approved by the Institutional Review Board of Yonsei University Gangnam Severance Hospital (IRB No. 3-2024-0467). Written informed consent was obtained from all participants.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Song, K., Lee, E., Lee, H.S. et al. Body composition references, sarcopenia cutoffs, and prevalence in youth using bioelectrical impedance analysis. Int J Obes 50, 319–328 (2026). https://doi.org/10.1038/s41366-025-01892-5
Received:
Revised:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41366-025-01892-5