Abstract
Background
Movement behaviours, including moderate-to-vigorous-intensity physical activity (MVPA), light-intensity physical activity (LPA), sedentary behaviour (SB), and sleep, influence childhood adiposity. However, their collective impact on adiposity from a sex-specific perspective remains underexplored. Our research examined the sex-specific longitudinal associations of 24-h movement behaviours with body mass index (BMI) and abdominal adiposity among children.
Methods
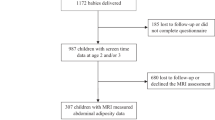
In the Growing Up in Singapore Towards healthy Outcomes (GUSTO) cohort study, we repeatedly measured 24-h movement behaviours using wrist-worn accelerometers (ActiGraph GT3x) and assessed adiposity (BMI, abdominal circumference, and MRI-based abdominal fat volumes) at three time points (ages 5.5–6, 7.5–8, and 10–10.5 years) within the same children in a longitudinal design. Compositional multivariable linear mixed-effect modelling and isotemporal substitution were used to estimate the associations.
Results
531 children (49.5% girls) were included in the analysis. Significant interactions between movement behaviours and sex were observed across all outcomes. In girls, higher MVPA relative to other behaviours was linked to lower BMI [−0.8 (−1.5, −0.1) kg/m²] and total abdominal adiposity [−225.5 (−451.6, −2.5) mL], while in boys, longer sleep duration was associated with lower BMI [−1.6 (−3.2, −0.1) kg/m²] and total abdominal adiposity [−624.2 (−1225.6, −31.3) mL]. The isotemporal substitution model showed that replacing 30 min of LPA/SB with MVPA reduced BMI and abdominal circumference by 1–2% and MRI-measured abdominal adiposity by 6–9% in both sexes. However, replacing LPA/SB with sleep reduced BMI and abdominal circumference by 1% and MRI-measured adiposity by 3–6% only in boys, with no changes in girls. These associations were pronounced on visceral adiposity.
Conclusion
This study highlights sex-specific associations of movement behaviours with adiposity in school-aged children, with stronger associations observed in MRI-derived measures compared to conventional adiposity indices. Replacing LPA/SB with MVPA reduced BMI and abdominal adiposity in both sexes, with particularly pronounced effects on visceral adiposity. However, sleep replacement benefits were observed only in boys, suggesting the need for gender-sensitive approaches in lifestyle interventions.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
Data availability
The dataset supporting the conclusions of this article can be made available upon request and after approval by the GUSTO Executive Committee.
References
Kumari S, Shukla S, Acharya S. Childhood obesity: prevalence and prevention in modern society. Cureus. 2022;14:e31640.
Vogelezang S, Gishti O, Felix JF, van der Beek EM, Abrahamse-Berkeveld M, Hofman A, et al. Tracking of abdominal subcutaneous and preperitoneal fat mass during childhood. The Generation R Study. Int J Obes. 2016;40:595–600.
Kindblom JM, Lorentzon M, Hellqvist A, Lönn L, Brandberg J, Nilsson S, et al. BMI changes during childhood and adolescence as predictors of amount of adult subcutaneous and visceral adipose tissue in men: the GOOD Study. Diabetes. 2009;58:867–74.
Pischon T, Boeing H, Hoffmann K, Bergmann M, Schulze MB, Overvad K, et al. General and abdominal adiposity and risk of death in Europe. N Engl J Med. 2008;359:2105–20.
Shah RV, Murthy VL, Abbasi SA, Blankstein R, Kwong RY, Goldfine AB, et al. Visceral adiposity and the risk of metabolic syndrome across body mass index. MESA Study JACC Cardiovasc Imaging. 2014;7:1221–35.
Sanchez-Lastra MA, Ding D, Del Pozo Cruz B, Dalene KE, Ayán C, Ekelund U, et al. Joint associations of device-measured physical activity and abdominal obesity with incident cardiovascular disease: a prospective cohort study. Br J Sports Med. 2024;58:196.
López-Gil JF, Tapia-Serrano MA, Sevil-Serrano J, Sánchez-Miguel PA, García-Hermoso A. Are 24-hour movement recommendations associated with obesity-related indicators in the young population? A meta-analysis. Obesity. 2023;31:2727–39.
Alanazi YA, Sousa-S E, Chong KH, Parrish AM, Okely AD. Systematic review of the relationships between 24-hour movement behaviours and health indicators in school-aged children from arab-speaking countries. Int J Environ Res Public Health. 2021;18:8640
Feng J, Zheng C, Sit CH, Reilly JJ, Huang WY. Associations between meeting 24-hour movement guidelines and health in the early years: a systematic review and meta-analysis. J Sports Sci. 2021;39:2545–57.
Morrissey B, Taveras E, Allender S, Strugnell C. Sleep and obesity among children: a systematic review of multiple sleep dimensions. Pediatr Obes. 2020;15:e12619.
Wiersma R, Haverkamp BF, van Beek JH, Riemersma AMJ, Boezen HM, Smidt N, et al. Unravelling the association between accelerometer-derived physical activity and adiposity among preschool children: a systematic review and meta-analyses. Obes Rev. 2020;21:e12936.
Biddle SJH, García Bengoechea E, Wiesner G. Sedentary behaviour and adiposity in youth: a systematic review of reviews and analysis of causality. Int J Behav Nutr Phys Act. 2017;14:43.
Bosy-Westphal A, Booke C-A, Blöcker T, Kossel E, Goele K, Later W, et al. Measurement site for waist circumference affects its accuracy as an index of visceral and abdominal subcutaneous fat in a Caucasian population. J Nutr. 2010;140:954–61.
Mohammad A, De Lucia Rolfe E, Sleigh A, Kivisild T, Behbehani K, et al. Validity of visceral adiposity estimates from DXA against MRI in Kuwaiti men and women. Nutr Diab. 2017;7:e238–e.
Horan M, Gibney E, Molloy E, McAuliffe F. Methodologies to assess paediatric adiposity. Ir J Med Sci. 2015;184:53–68.
Sadananthan SA, Prakash B, Leow MKS, Khoo CM, Chou H, Venkataraman K, et al. Automated segmentation of visceral and subcutaneous (deep and superficial) adipose tissues in normal and overweight men. J Magn Reson Imaging. 2015;41:924–34.
Saelens BE, Grow HM, Stark LJ, Seeley RJ, Roehrig H. Efficacy of increasing physical activity to reduce children’s visceral fat: a pilot randomized controlled trial. Int J Pediatr Obes. 2011;6:102–12.
Saelens BE, Seeley RJ, van Schaick K, Donnelly LF, O’Brien KJ. Visceral abdominal fat is correlated with whole-body fat and physical activity among 8-y-old children at risk of obesity2. Am J Clin Nutr. 2007;85:46–53.
Owens S, Gutin B, Allison J, Riggs S, Ferguson M, Litaker M, et al. Effect of physical training on total and visceral fat in obese children. Med Sci sports Exerc. 1999;31:143–8.
Rubín L, Gába A, Pelclová J, Štefelová N, Jakubec L, Dygrýn J, et al. Changes in sedentary behavior patterns during the transition from childhood to adolescence and their association with adiposity: a prospective study based on compositional data analysis. Arch Public Health. 2022;80:1.
Morales-Ghinaglia N, Larsen M, He F, Calhoun SL, Vgontzas AN, Liao J, et al. Circadian misalignment impacts the association of visceral adiposity with elevated blood pressure in adolescents. Hypertension. 2023;80:861–71.
Pedisic Z, Dumuid D, Olds TS. Integrating sleep, sedentary behaviour, and physical activity research in the emerging field of time-use epidemiology: definitions, concepts, statistical methods, theoretical framework, and future directions. Kinesiology. 2017;49:252.
Dumuid D, Pedišić Ž, Stanford TE, Martín-Fernández JA, Hron K, Maher CA, et al. The compositional isotemporal substitution model: a method for estimating changes in a health outcome for reallocation of time between sleep, physical activity and sedentary behaviour. Stat Methods Med Res. 2019;28:846–57.
Volpato LA, Costa JC, Lopes WA, Sasaki JE, Romanzini CLP, Ronque ERV, et al. Time reallocations from sedentary behavior to physical activity and cardiovascular risk factors in children and adolescents: a systematic review. J Phys Act Health. 2023;20:1084–91.
Bourke M, Harrison Z, Fortnum K, Thomas G, O’Flaherty M, Mulcahy SK, et al. Association between 24-hour movement behaviors and adiposity in children and adolescents: a compositional data meta-analysis. Obes Rev. 2025;26:e13884.
Sadananthan SA, Tint MT, Michael N, Aris IM, Loy SL, Lee KJ, et al. Association between early life weight gain and abdominal fat partitioning at 4.5 years is sex, ethnicity, and age dependent. Obesity. 2019;27:470–8.
Padmapriya N, Chen B, Goh CMJL, Shek LPC, Chong YS, Tan KH, et al. 24-hour movement behaviour profiles and their transition in children aged 5.5 and 8 years – findings from a prospective cohort study. Int J Behav Nutr Phys Act. 2021;18:145.
Gába A, Dygrýn J, Štefelová N, Rubín L, Hron K, Jakubec L. Replacing school and out-of-school sedentary behaviors with physical activity and its associations with adiposity in children and adolescents: a compositional isotemporal substitution analysis. Environ Health Prevent Med. 2021;26:16.
Nogueira JA, Macedo da Costa TH. Gender differences in physical activity, sedentary behavior, and their relation to body composition in active Brazilian adolescents. J Phys Act Health. 2009;6:93–8.
Basterfield L, Pearce MS, Adamson AJ, Frary JK, Parkinson KN, Wright CM, et al. Physical activity, sedentary behavior, and adiposity in English children. Am J Prev Med. 2012;42:445–51.
Tanaka C, Reilly JJ, Huang WY. Longitudinal changes in objectively measured sedentary behaviour and their relationship with adiposity in children and adolescents: systematic review and evidence appraisal. Obes Rev. 2014;15:791–803.
Soh SE, Chong YS, Kwek K, Saw SM, Meaney MJ, Gluckman PD, et al. Insights from the Growing Up in Singapore Towards Healthy Outcomes (GUSTO) cohort study. Ann Nutr Metab. 2014;64:218–25.
Soh SE, Tint MT, Gluckman PD, Godfrey KM, Rifkin-Graboi A, Chan YH, et al. Cohort profile: Growing Up in Singapore Towards healthy Outcomes (GUSTO) birth cohort study. Int J Epidemiol. 2014;43:1401–9.
van Hees VT, Gorzelniak L, Dean León EC, Eder M, Pias M, Taherian S, et al. Separating movement and gravity components in an acceleration signal and implications for the assessment of human daily physical activity. PloS One. 2013;8:e61691–e.
Jairo HM, Alex VR, Florian H, Séverine S, Vincent. TvH. GGIR: a research community–driven open source R package for generating physical activity and sleep outcomes from multi-day raw accelerometer data. J Meas Phys Behav. 2019;2:188–96.
van Hees VT, Sabia S, Anderson KN, Denton SJ, Oliver J, Catt M, et al. A novel, open access method to assess sleep duration using a wrist-worn accelerometer. PLOS One. 2015;10:e0142533.
van Hees VT, Sabia S, Jones SE, Wood AR, Anderson KN, Kivimäki M, et al. Estimating sleep parameters using an accelerometer without sleep diary. Sci Rep. 2018;8:12975.
Hildebrand M, Van Hees VT, Hansen BH, Ekelund ULF. Age group comparability of raw accelerometer output from wrist- and hip-worn monitors. Med Sci sports Exerc. 2014;46:1816–24.
Hildebrand M, Hansen BH, van Hees VT, Ekelund U. Evaluation of raw acceleration sedentary thresholds in children and adults. Scand J Med Sci sports. 2017;27:1814–23.
Kway YM, Thirumurugan K, Michael N, Tan KH, Godfrey KM, Gluckman P, et al. A fully convolutional neural network for comprehensive compartmentalization of abdominal adipose tissue compartments in MRI. Comput Biol Med. 2023;167:107608.
Kway YM, Thirumurugan K, Tint MT, Michael N, Shek LP, Yap FKP, et al. Automated segmentation of visceral, deep subcutaneous, and superficial subcutaneous adipose tissue volumes in mri of neonates and young children. Radio Artif Intell. 2021;3:e200304.
Conway JM, Ingwersen LA, Vinyard BT, Moshfegh AJ. Effectiveness of the US Department of Agriculture 5-step multiple-pass method in assessing food intake in obese and nonobese women. Am J Clin Nutr. 2003;77:1171–8.
Package ‘missForest’. 2022. https://www.r-project.org, https://github.com/stekhoven/missForest.
Fairclough SJ, Dumuid D, Taylor S, Curry W, McGrane B, Stratton G, et al. Fitness, fatness and the reallocation of time between children’s daily movement behaviours: an analysis of compositional data. Int J Behav Nutr Phys Act. 2017;14:64.
Chastin SF, Palarea-Albaladejo J, Dontje ML, Skelton DA. Combined effects of time spent in physical activity, sedentary behaviors and sleep on obesity and cardio-metabolic health markers: a novel compositional data analysis approach. PLoS One. 2015;10:e0139984.
van den Boogaart KG, Tolosana-Delgado R, Bren M. “compositions”: R package to analyze compositional data. 2022. https://cran.r-project.org/web/packages/compositions/index.html.
Lu Z, Guo J, Liu C, Wu J, Zhao C, Wang F, et al. Reallocation of time to moderate-to-vigorous physical activity and estimated changes in physical fitness among preschoolers: a compositional data analysis. BMC Public Health. 2024;24:2823.
Alves JM, Belcher BR, McAlister KL, Chow T, Xiang AH, Page KA. The reallocation of sedentary time is associated with longitudinal improvements in cardiometabolic outcomes during childhood. J Pediatr. 2025;285:114680.
Chen H, Wang LJ, Xin F, Liang G, Zhou YL. Associations between 24-h movement behaviours and BMI in Chinese primary- and middle- school students. J Exerc Sci Fit. 2023;21:186–92.
Gába A, Pedišić Ž, Štefelová N, Dygrýn J, Hron K, Dumuid D, et al. Sedentary behavior patterns and adiposity in children: a study based on compositional data analysis. BMC Pediatr. 2020;20:147.
Taylor RW, Grant AM, Williams SM, Goulding A. Sex differences in regional body fat distribution from pre- to postpuberty. Obesity. 2010;18:1410–6.
Fairclough SJ, Dumuid D, Taylor S, Curry W, McGrane B, Stratton G. et al. Fitness, fatness and the reallocation of time between children's daily movement behaviours: an analysis of compositional data. Int J Behav Nutr Phys Activity. 2017;14:64
Carson V, Tremblay MS, Chastin SFM. Cross-sectional associations between sleep duration, sedentary time, physical activity, and adiposity indicators among Canadian preschool-aged children using compositional analyses. BMC public health. 2017;17:848.
Telford RM, Telford RD, Olive LS, Cochrane T, Davey R. Why are girls less physically active than boys? Findings from the LOOK Longitudinal Study. PLoS One. 2016;11:e0150041.
Söğüt M, Clemente FM, Clark CCT, Nikolaidis PT, Rosemann T, Knechtle B. Variations in central adiposity, cardiovascular fitness, and objectively measured physical activity according to weight status in children (9-11 years). Front Physiol. 2019;10:936
Kellam S, Olvera N, Leung P, Liu J, Smith D. Effect of exercise dosages on adiposity indices in overweight girls. Salud Publ Mex. 2013;55 Suppl 3:415–21.
Cano A, Ventura L, Martinez G, Cugusi L, Caria M, Deriu F, et al. Analysis of sex-based differences in energy substrate utilization during moderate-intensity aerobic exercise. Eur J Appl Physiol. 2022;122:29–70.
Kostyak JC, Kris-Etherton P, Bagshaw D, DeLany JP, Farrell PA. Relative fat oxidation is higher in children than adults. Nutr J. 2007;6:19.
Power ML, Schulkin J. Sex differences in fat storage, fat metabolism, and the health risks from obesity: possible evolutionary origins. Br J Nutr. 2008;99:931–40.
Taheri S, Lin L, Austin D, Young T, Mignot E. Short sleep duration is associated with reduced leptin, elevated ghrelin, and increased body mass index. PLoS Med. 2004;1:e62.
Wu BN, O’Sullivan AJ. Sex differences in energy metabolism need to be considered with lifestyle modifications in humans. J Nutr Metab. 2011;2011:391809.
Chaput JP. Sleep patterns, diet quality and energy balance. Physiol Behav. 2014;134:86–91.
Staiano AE, Katzmarzyk PT. Ethnic and sex differences in body fat and visceral and subcutaneous adiposity in children and adolescents. Int J Obes. 2012;36:1261–9.
Cooke LJ, Wardle J. Age and gender differences in children’s food preferences. Br J Nutr. 2005;93:741–6.
Deslippe AL, Bergeron C, Cohen TR. Boys and girls differ in their rationale behind eating: a systematic review of intrinsic and extrinsic motivations in dietary habits across countries. Front Nutr. 2023;10:1256189.
Chatham RE, Mixer SJ. Cultural influences on childhood obesity in ethnic minorities: a qualitative systematic review. J Transcult Nurs. 2020;31:87–99.
Kracht CL, Katzmarzyk PT, Champagne CM, Broyles ST, Hsia DS, Newton RL, et al. Association between sleep, sedentary time, physical activity, and adiposity in adolescents: a prospective observational study. Med Sci sports Exerc. 2023;55:110–8.
García-Hermoso A, Saavedra JM, Ramírez-Vélez R, Ekelund U, Del Pozo-Cruz B. Reallocating sedentary time to moderate-to-vigorous physical activity but not to light-intensity physical activity is effective to reduce adiposity among youths: a systematic review and meta-analysis. Obes Rev. 2017;18:1088–95.
Samadi M, Sadrzade-Yeganeh H, Azadbakht L, Jafarian K, Rahimi A, Sotoudeh G. Sensitivity and specificity of body mass index in determining obesity in children. J Res Med Sci. 2013;18:537–42.
Hurter L, Fairclough SJ, Knowles ZR, Porcellato LA, Cooper-Ryan AM, Boddy LM. Establishing raw acceleration thresholds to classify sedentary and stationary behaviour in children. Children. 2018;5:172.
Trost SG. Population-level physical activity surveillance in young people: are accelerometer-based measures ready for prime time? Int J Behav Nutr Phys Act. 2020;17:28.
Freedson PS, John D. Comment on Estimating Activity and Sedentary Behavior from an Accelerometer on the Hip and Wrist. Med Sci Sports Exercise. 2013;45:962–3.
Acknowledgements
We thank the GUSTO study group, operational managers, research fellows, study coordinators, and data management team, as well as the participants for their valuable contributions and cooperation. The GUSTO study group includes: Airu Chia, Andrea Cremaschi, Anna Magdalena Fogel, Anne Eng Neo Goh, Anne Rifkin-Graboi, Anqi Qiu, Arijit Biswas, Bee Wah Lee, Birit Froukje Philipp Broekman, Candida Vaz, Chai Kiat Chng, Chan Shi Yu, Choon Looi Bong, Daniel Yam Thiam Goh, Dawn Xin Ping Koh, Dennis Wang, Desiree Y. Phua, E Shyong Tai, Elaine Kwang Hsia Tham, Elaine Phaik Ling Quah, Elizabeth Huiwen Tham, Evelyn Chung Ning Law, Evelyn Keet Wai Lau, Evelyn Xiu Ling Loo, Fabian Kok Peng Yap, Falk Müller-Riemenschneider, Franzolini Beatrice, George Seow Heong Yeo, Gerard Chung Siew Keong, Hannah Ee Juen Yong, Helen Yu Chen, Hong Pan, Huang Jian, Huang Pei, Hugo P S van Bever, Hui Min Tan, Iliana Magiati, Inez Bik Yun Wong, Ives Lim Yubin, Ivy Yee-Man Lau, Jacqueline Chin Siew Roong, Jadegoud Yaligar, Jerry Kok Yen Chan, Jia Xu, Johan Gunnar Eriksson, Jonathan Tze Liang Choo, Jonathan Y. Bernard, Jonathan Yinhao Huang, Joshua J. Gooley, Jun Shi Lai, Karen Mei Ling Tan, Keith M. Godfrey, Keri McCrickerd, Kok Hian Tan, Kothandaraman Narasimhan, Krishnamoorthy Naiduvaje, Kuan Jin Lee, Li Chen, Lieng Hsi Ling, Lin Lin Su, Ling-Wei Chen, Lourdes Mary Daniel, Lynette Pei-Chi Shek, Maria De Iorio, Marielle V. Fortier, Mary Foong-Fong Chong, Mary Wlodek, Mei Chien Chua, Melvin Khee-Shing Leow, Michael J. Meaney, Michelle Zhi Ling Kee, Min Gong, Mya Thway Tint, Navin Michael, Neerja Karnani, Ngee Lek, Noor Hidayatul Aini Bte Suaini, Oon Hoe Teoh, Peter David Gluckman, Priti Mishra, Queenie Ling Jun Li, Sambasivam Sendhil Velan, Seang Mei Saw, See Ling Loy, Seng Bin Ang, Shang Chee Chong, Shiao-Yng Chan, Shirong Cai, Shu-E Soh, Stephen Chin-Ying Hsu, Suresh Anand Sadananthan, Swee Chye Quek, Tan Ai Peng, Varsha Gupta, Victor Samuel Rajadurai, Wee Meng Han, Wei Wei Pang, Yap Seng Chong, Yin Bun Cheung, Yiong Huak Chan, Yung Seng Lee, Zhang Han.
Funding
This research is supported by the Singapore National Research Foundation under its Translational and Clinical Research (TCR) Flagship Programme and administered by the Singapore Ministry of Health’s National Medical Research Council (NMRC), Singapore- NMRC/TCR/004-NUS/2008; NMRC/TCR/012-NUHS/2014. Additional funding is provided by the Singapore Institute for Clinical Sciences, Agency for Science Technology and Research (A*STAR), Singapore. KMG is supported by the UK Medical Research Council (MC_UU_12011/4), the National Institute for Health and Care Research (NIHR Senior Investigator (NF-SI-0515-10042) and NIHR Southampton Biomedical Research Centre (NIHR203319)) and Alzheimer’s Research UK (ARUK-PG2022A-008). For the purpose of Open Access, the author has applied a Creative Commons Attribution (CC BY) licence to any Author Accepted Manuscript version arising from this submission. JYB was supported by a grant from the Agence Nationale de la Recherche (ANR) (iSCAN project, ANR-20-CE36-0001).
Author information
Authors and Affiliations
Contributions
KHT, YSC, YSL, FY, MFFG, KMG and JGE conceived and designed the cohort study; NP, SAS, JYB and FMR designed the present work; NP, SAS, NM, JYT and JYB contributed to data collection, data process and data analysis; NP drafted the manuscript with the guidance of FMR, and SAS, NM, MTT, SYXT, AC, SC, KMG, JGE and SSV added important intellectual content; all authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Competing interests
KMG receiving reimbursement for speaking at conferences sponsored by companies selling nutritional products. KMG, YSC and SYC report being part of an academic consortium that has received research funding from Abbott Nutrition, Nestle and Danone. No other disclosures were reported.
Ethics approval and consent to participate
All participating women signed written informed consent for themselves and on behalf of their offspring at enrolment. The study received ethical approval from the National Healthcare Group Domain Specific Review Board (D/2009/021, B/2014/00406 and D/2010/210) and the SingHealth Centralised Institutional Review Board (CIRB 2018/2767 and CIRB 2018/3138). All methods were performed in accordance with the relevant guidelines and regulations.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Padmapriya, N., Sadananthan, S.A., Michael, N. et al. Sex-specific longitudinal associations between repeatedly measured movement behaviours and adiposity measures in school-aged children: a compositional data analysis approach. Int J Obes 50, 546–557 (2026). https://doi.org/10.1038/s41366-025-01969-1
Received:
Revised:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41366-025-01969-1