Abstract
Background/objectives
Time-restricted eating (TRE) induces a metabolic shift in substrate utilization increasing lipolysis and ketogenesis. These metabolic changes raise the possibility of a differential effect on energy balance regulation following TRE-induced weight loss. The aim of this study is to evaluate the impact of TRE on energy balance homeostasis in individuals with overweight/obesity and type 2 diabetes (T2DM) who participated in a recently reported trial achieving substantial weight reduction (−3.86% body weight).
Subjects/methods
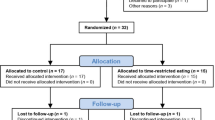
In this randomized cross-over trial, 39 participants with overweight/obesity and T2DM were randomized to either 6 weeks of TRE (20 h fasting/4 h eating) or standard lifestyle, followed by 4-week washout and then the other dietary intervention for 6 weeks. At each study visit at baseline, 6-, 10-, and 16-week participants completed a 75 g oral glucose tolerance test (OGTT). We measured fasting and post-challenge responses of glucose, glucagon, GLP-1, ghrelin, leptin, and peptide YY.
Results
TRE-induced calorie deficit as participants self-reported ingested −384 ± 488 Kcal/day less during TRE as compared to the standard lifestyle period (P < 0.001) with no differences in macronutrient distribution. There were no differences in responses to OGTT induced by TRE as compared to standard lifestyle for glucagon (AUC0–120 min 0.04 ± 23.5, P = 0.99), GLP-1 (AUC0–120 min 1.6 ± 67.6, P = 0.98), ghrelin (AUC0–120 min 31.0 ± 32.4, P = 0.35), and peptide YY (AUC0–120 min −33.9 ± 65.6, P = 0.61). Importantly, TRE-induced weight loss promoted a significant decrease in both fasting leptin (−2445 ± 885 ng/mL, P = 0.009) and leptin response to OGTT (AUC0–120 min −12776 ± 3088, P < 0.001) as compared to standard lifestyle. In addition, a significant increase in fasting ghrelin (28 ± 11.3 pg/mL, P = 0.02) was observed post-TRE as compared to pre-intervention.
Conclusions
These findings demonstrate that TRE does not prevent the physiologic compensatory changes associated with weight reduction in individuals with overweight/obesity and T2DM.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
Data availability
De-identified data can be made available under restricted access from the corresponding author, for academic purposes, subject to a material transfer agreement and approval of the Mount Sinai Hospital Research Ethics Board.
References
Bray GA, Frühbeck G, Ryan DH, Wilding JP. Management of obesity. Lancet. 2016;387:1947–56.
American Diabetes Association Professional Practice Committee. Summary of revisions: Standards of Care in Diabetes–2024. Diabetes Care. 2024;47:S5–10.
Varkevisser RDM, van Stralen MM, Kroeze W, Ket JCF, Steenhuis IHM. Determinants of weight loss maintenance: a systematic review. Obes Rev. 2019;20:171–211.
Wing RR, Phelan S. Long-term weight loss maintenance. Am J Clin Nutr. 2005;82:222S–5S.
Dombrowski SU, Knittle K, Avenell A, Araújo-Soares V, Sniehotta FF. Long term maintenance of weight loss with nonsurgical interventions in obese adults: systematic review and metaanalyses of randomised controlled trials. The BMJ. 2014;348:g2646.
Sumithran P, Prendergast LA, Delbridge E, Purcell K, Shulkes A, Kriketos A, et al. Long-term persistence of hormonal adaptations to weight loss. N Engl J Med. 2011;365:1597–604.
Nymo S, Coutinho SR, Eknes PH, et al. Investigation of the long-term sustainability of changes in appetite after weight loss. Int J Obes. 2018;42:1489–99.
Iepsen EW, Lundgren J, Holst JJ, Madsbad S, Torekov SS. Successful weight loss maintenance includes long-term increased meal responses of GLP-1 and PYY3-36. Eur J Endocrinol. 2016;174:775–84.
de Cabo R, Mattson MP. Effects of intermittent fasting on health, aging, and disease. N Engl J Med. 2019;381:2541–51.
Manoogian ENC, Chow LS, Taub PR, Laferrère B, Panda S. Time-restricted eating for the prevention and management of metabolic diseases. Endocr Rev. 2022;43:405–36.
Borgundvaag E, Mak J, Kramer CK. Metabolic impact of intermittent fasting in patients with type 2 diabetes mellitus: a systematic review and meta-analysis of interventional studies. J Clin Endocrinol Metab. 2021;106:902–11.
Sutton EF, Beyl R, Early KS, Cefalu WT, Ravussin E, Peterson CM. Early time-restricted feeding improves insulin sensitivity, blood pressure, and oxidative stress even without weight loss in men with prediabetes. Cell Metab. 2018;27:1212–21.e3.
Anton SD, Moehl K, Donahoo WT, Marosi K, Lee SA, Mainous AG, et al. Flipping the metabolic switch: understanding and applying the health benefits of fasting. Obesity. 2018;26:254–68.
Ezpeleta M, Cienfuegos S, Lin S, Pavlou V, Gabel K, Tussing-Humphreys L, et al. Time-restricted eating: watching the clock to treat obesity. Cell Metab. 2023;19:S1550-413100454-0.
Kramer CK, Zinman B, Feig DS, Retnakaran R. The impact of time-restricted eating on beta-cell function in adults with type 2 diabetes. J Clin Endocrinol Metab. 2025;110:e2045–53.
Arab L, Tseng CH, Ang A, Jardack P. Validity of a multipass, web-based, 24-hour self-administered recall for assessment of total energy intake in blacks and whites. Am J Epidemiol. 2011;174:1256–65.
Parker BA, Sturm K, MacIntosh CG, Feinle C, Horowitz M, Chapman IM. Relation between food intake and visual analogue scale ratings of appetite and other sensations in healthy older and young subjects. Eur J Clin Nutr. 2004;58:212–8.
Cienfuegos S, Gabel K, Kalam F, Ezpeleta M, Wiseman E, Pavlou V, et al. Effects of 4- and 6-h time-restricted feeding on weight and cardiometabolic health: a randomized controlled trial in adults with obesity. Cell Metab. 2020;32:366–78.e3.
Lin S, Cienfuegos S, Ezpeleta M, Gabel K, Pavlou V, Mulas A, et al. Time-restricted eating without calorie counting for weight loss in a racially diverse population: a randomized controlled trial. Ann Intern Med. 2023;176:885–95.
Pavlou V, Cienfuegos S, Lin S, Ezpeleta M, Ready K, Corapi S, et al. Effect of time-restricted eating on weight loss in adults with type 2 diabetes: a randomized clinical trial. JAMA Netw Open. 2023;6:e2339337.
Dhurandhar NV, Schoeller D, Brown AW, Heymsfield SB, Thomas D, Sørensen TI, et al. Energy Balance Measurement Working Group. Energy balance measurement: when something is not better than nothing. Int J Obes. 2015;39:1109–13.
Hansen TK, Dall R, Hosoda H, et al. Weight loss increases circulating levels of ghrelin in human obesity. Clin Endocrinol. 2002;6:203–6.
Rosenbaum M, Nicolson M, Hirsch J, Murphy E, Chu F, Leibel RL. Effects of weight change on plasma leptin concentrations and energy expenditure. J Clin Endocrinol Metab. 1997;82:3647–54.
Nymo S, Coutinho SR, Jorgensen J, Rehfeld JF, Truby H, Kulseng B, et al. Timeline of changes in appetite during weight loss with a ketogenic diet. Int J Obes. 2017;41:1224–31.
Coutinho SR, With E, Rehfeld JF, Kulseng B, Truby H, Martins C. The impact of rate of weight loss on body composition and compensatory mechanisms during weight reduction: a randomized control trial. Clin Nutr. 2018;37:1154–62.
Liu D, Huang Y, Huang C, Yang S, Wei X, Zhang P, et al. Calorie restriction with or without time-restricted eating in weight loss. N Engl J Med. 2022;386:1495–504.
Lowe DA, Wu N, Rohdin-Bibby L, Moore AH, Kelly N, Liu YE, et al. Effects of time-restricted eating on weight loss and other metabolic parameters in women and men with overweight and obesity: the TREAT randomized clinical trial. JAMA Intern Med. 2020;180:1491–9.
Acknowledgements
The corresponding author (CKK) had full access to all the data in the study and had final responsibility for the decision to submit for publication. This study was supported by the Canadian Institutes of Health Research (CIHR) (PJT 166091) (CKK). RR holds the Boehringer Ingelheim Chair in Beta-cell Preservation, Function, and Regeneration at Mount Sinai Hospital. The funders had no role in study design, data collection and analysis, or writing of the manuscript.
Funding
This study was supported by the Canadian Institutes of Health Research (CIHR) (PJT 166091) (CKK). RR holds the Boehringer Ingelheim Chair in Beta-cell Preservation, Function, and Regeneration at Mount Sinai Hospital. The funders had no role in study design, data collection and analysis, or writing of the manuscript.
Author information
Authors and Affiliations
Contributions
CKK, RR and BZ designed the study. CKK and RR acquired the data. CKK led study implementation, performed the statistical analyses, and wrote the manuscript. CKK, BZ, DF and RR contributed to the interpretation of the data and critical revision of the manuscript. CKK, BZ, DF and RR approved the manuscript.
Corresponding author
Ethics declarations
Competing interests
All authors declare no competing interests related to the submitted work. CKK reports research grants from Boehringer Ingelheim, outside of the submitted work. DSF reports an investigator-initiated grant from Dexcom, in-kind donations from Dexcom and Tandem and honoraria from Novo-Nordisk, Sanofi and Ypsomed, outside the submitted work. RR reports grants from Boehringer Ingelheim, grants and personal fees from Novo Nordisk, personal fees from Sanofi, personal fees from Eli Lilly, outside the submitted work. All other authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Kramer, C.K., Zinman, B., Feig, D.S. et al. The effects of time-restricted eating on energy balance regulation in adults with overweight/obesity and type 2 diabetes. Int J Obes (2026). https://doi.org/10.1038/s41366-026-02042-1
Received:
Revised:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41366-026-02042-1