Abstract
Background and aims
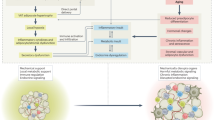
Visceral adipose tissue (VAT) plays a key role in metabolic dysfunction, and it is increasingly recognised as a contributor to metabolic dysfunction-associated steatotic liver disease (MASLD) and other chronic liver conditions. However, the systemic metabolic pathways linking VAT to liver disease remain unclear. This study aimed to identify metabolic signatures associated with VAT and examine their potential role as mediators in the relationship between VAT accumulation and the risks of MASLD, cirrhosis and hepatoma.
Methods
This prospective study included 269,018 UK Biobank participants without baseline liver disease. Predicted VAT mass was estimated using sex-specific models on the basis of anthropometric and bioimpedance measures. Incident liver outcomes were identified via ICD-coded hospital records. A VAT-related metabolic signature was derived from 251 circulating metabolites by using elastic net regression. Associations with liver disease risks were assessed using Cox models. Mediation analysis estimated the proportion of the VAT–MASLD association explained by the metabolic signature.
Results
Over a median follow-up of 14.3 years, 2658 MASLD, 671 cirrhosis and 444 hepatoma cases occurred. Each standard deviation increase in VAT was associated with increased risks of MASLD (HR: 1.70; 95% CI: 1.62–1.79), cirrhosis (HR: 1.27; 95% CI: 1.15–1.40) and hepatoma (HR: 1.15; 95% CI: 1.02–1.30). The VAT-related metabolic signature (156 metabolites, primarily lipoprotein subclasses and lipids) was independently associated with MASLD (HR: 1.89; 95% CI: 1.72–2.08) and mediated 40.0% of the VAT–MASLD association. No significant mediation was observed for cirrhosis or hepatoma.
Conclusions
VAT and its metabolic signature are strongly associated with MASLD risk, partly explaining its pathogenesis through systemic metabolic alterations.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
Data availability
The data for this study were obtained from the UK Biobank under Application Number 55794. Researchers wishing to access these data can apply directly through the UK Biobank website (www.ukbiobank.ac.uk).
References
Targher G, Byrne CD, Tilg H. MASLD: a systemic metabolic disorder with cardiovascular and malignant complications. Gut. 2024;73:691–702.
Alqudah O, Alshahwan HF, Alsamhouri JF, Yamin S, Kaffaf A, Alassaf M, et al. Metabolic dysfunction-associated steatotic liver disease MASLD: Jordan’s perspective based on knowledge and attitude determinants. Risk Manag Healthc Policy. 2024;17:2483–91.
Wang X, Zhang L, Dong B. Molecular mechanisms in MASLD/MASH-related HCC. Hepatology. 2024;82:1303–24.
Powell EE, Wong VW, Rinella M. Non-alcoholic fatty liver disease. Lancet. 2021;397:2212–24.
Younossi Z, Anstee QM, Marietti M, Hardy T, Henry L, Eslam M, et al. Global burden of NAFLD and NASH: trends, predictions, risk factors and prevention. Nat Rev Gastroenterol Hepatol. 2018;15:11–20.
Harrison SA, Allen AM, Dubourg J, Noureddin M, Alkhouri N. Challenges and opportunities in NASH drug development. Nature medicine. 2023;29:562–73.
Byrne CD, Targher G. NAFLD: a multisystem disease. J Hepatol. 2015;62:S47–64.
van der Poorten D, Milner KL, Hui J, Hodge A, Trenell MI, Kench JG, et al. Visceral fat: a key mediator of steatohepatitis in metabolic liver disease. Hepatology. 2008;48:449–57.
Meroni M, Chiappori F, Paolini E, Longo M, De Caro E, Mosca E, et al. A novel gene signature to diagnose MASLD in metabolically unhealthy obese individuals. Biochem Pharmacol. 2023;218:115925.
Tilg H, Ianiro G, Gasbarrini A, Adolph TE. Adipokines: masterminds of metabolic inflammation. Nat Rev Immunol. 2025;25:250–65.
Raja G, Gupta H, Gebru YA, Youn GS, Choi YR, Kim HS, et al. Recent advances of microbiome-associated metabolomics profiling in liver disease: principles, mechanisms, and applications. Int J Mol Sci. 2021;22:1160.
Park G, Jung S, Wellen KE, Jang C. The interaction between the gut microbiota and dietary carbohydrates in nonalcoholic fatty liver disease. Exp Mol Med. 2021;53:809–22.
Zhang S, Wang Z, Wang Y, Zhu Y, Zhou Q, Jian X, et al. A metabolomic profile of biological aging in 250,341 individuals from the UK Biobank. Nat Commun. 2024;15:8081.
Pecani M, Andreozzi P, Cangemi R, Corica B, Miglionico M, Romiti GF, et al. Metabolic syndrome and liver disease: re-appraisal of screening, diagnosis, and treatment through the paradigm shift from NAFLD to MASLD. J Clin Med. 2025;14:2750.
Lind L, Salihovic S, Risérus U, Kullberg J, Johansson L, Ahlström H, et al. The plasma metabolomic profile is differently associated with liver fat, visceral adipose tissue, and pancreatic fat. J Clin Endocrinol Metab. 2021;106:e118–e29.
Starekova J, Hernando D, Pickhardt PJ, Reeder SB. Quantification of liver fat content with CT and MRI: state of the art. Radiology. 2021;301:250–62.
Sudlow C, Gallacher J, Allen N, Beral V, Burton P, Danesh J, et al. UK Biobank: an open access resource for identifying the causes of a wide range of complex diseases of middle and old age. PLoS Med. 2015;12:e1001779.
Karlsson T, Rask-Andersen M, Pan G, Höglund J, Wadelius C, Ek WE, et al. Contribution of genetics to visceral adiposity and its relation to cardiovascular and metabolic disease. Nat Med. 2019;25:1390–5.
Vell MS, Loomba R, Krishnan A, Wangensteen KJ, Trebicka J, Creasy KT, et al. Association of statin use with risk of liver disease, hepatocellular carcinoma, and liver-related mortality. JAMA Netw Open. 2023;6:e2320222.
Chen HW, Liu K, Cao BF, Zhong Q, Zhou R, Li LH, et al. Combined associations of visceral adipose tissue and adherence to a Mediterranean lifestyle with T2D and diabetic microvascular complications among individuals with prediabetes. Cardiovasc Diabetol. 2024;23:201.
Rinella ME, Lazarus JV, Ratziu V, Francque SM, Sanyal AJ, Kanwal F, et al. A multisociety Delphi consensus statement on new fatty liver disease nomenclature. J Hepatol. 2023;79:1542–56.
Hagström H, Adams LA, Allen AM, Byrne CD, Chang Y, Grønbaek H, et al. Administrative coding in electronic health care record-based research of NAFLD: an expert panel consensus statement. Hepatology. 2021;74:474–82.
Zhong Q, Zhou R, Huang YN, Huang RD, Li FR, Chen HW, et al. Frailty and risk of metabolic dysfunction-associated steatotic liver disease and other chronic liver diseases. J Hepatol. 2024;82:427–37.
Caussy C, Alquiraish MH, Nguyen P, Hernandez C, Cepin S, Fortney LE, et al. Optimal threshold of controlled attenuation parameter with MRI-PDFF as the gold standard for the detection of hepatic steatosis. Hepatology. 2018;67:1348–59.
Marjot T, Ray DW, Williams FR, Tomlinson JW, Armstrong MJ. Sleep and liver disease: a bidirectional relationship. Lancet Gastroenterol Hepatol. 2021;6:850–63.
Lu S, Xie Q, Kuang M, Hu C, Li X, Yang H, et al. Lipid metabolism, BMI and the risk of nonalcoholic fatty liver disease in the general population: evidence from a mediation analysis. J Transl Med. 2023;21:192.
Ding Z, Wei Y, Peng J, Wang S, Chen G, Sun J. The potential role of C-reactive protein in metabolic-dysfunction-associated fatty liver disease and aging. Biomedicines. 2023;11:2711.
Julkunen H, Cichońska A, Slagboom PE, Würtz P. Metabolic biomarker profiling for identification of susceptibility to severe pneumonia and COVID-19 in the general population. Elife. 2021;10:e63033.
Meinshausen N, Bühlmann P. Stability Selection. J R Stat Soc Ser B Stat Methodol. 2010;72:417–73.
Alli BY. InteractionR: an R package for full reporting of effect modification and interaction. Softw Impacts. 2021;10:100147.
Zhou Y, Su X, Tan H, Xiao J. Association between metabolic score for visceral fat index and BMI-adjusted skeletal muscle mass index in American adults. Lipids Health Dis. 2025;24:29.
Yang SJ, Li HR, Zhang WH, Liu K, Zhang DY, Sun LF, et al. Visceral fat area (VFA) superior to BMI for predicting postoperative complications after radical gastrectomy: a prospective cohort study. J Gastrointest Surg. 2020;24:1298–306.
Tao M, Zhou G, Liu J, He M, Wang C, Luo X, et al. Visceral adipose tissue and risk of nonalcoholic fatty liver disease: a Mendelian randomization study. Clin Endocrinol (Oxf). 2023;99:370–7.
Montano-Loza AJ, Mazurak VC, Ebadi M, Meza-Junco J, Sawyer MB, Baracos VE, et al. Visceral adiposity increases risk for hepatocellular carcinoma in male patients with cirrhosis and recurrence after liver transplant. Hepatology. 2018;67:914–23.
Kubota S, Yabe D. Visceral adipose tissue quality and its impact on metabolic health. J Clin Endocrinol Metab. 2024;109:e1665–e6.
Chen H, Liu Y, Liu D, Liang Y, Zhu Z, Dong K, et al. Sex- and age-specific associations between abdominal fat and non-alcoholic fatty liver disease: a prospective cohort study. J Mol Cell Biol. 2024;15:mjad069.
Xu FQ, Xu QY, Zhu ZJ, Jin L, Ye TW, Du CF, et al. Visceral and ectopic fat are more predictively associated with primary liver cancer than overall obesity from genetic sights: a Mendelian randomization study. Int J Cancer. 2024;154:530–7.
Dong J, Dennis K, Venkatakrishnan R, Hodson L, Tomlinson JW. The impact of estrogen deficiency on liver metabolism: implications for hormone replacement therapy. Endocr Rev. 2025;46:790–809.
Milani I, Chinucci M, Leonetti F, Capoccia D. MASLD: prevalence, mechanisms, and sex-based therapies in postmenopausal women. Biomedicines. 2025;13:855.
Zamani M, Alizadeh-Tabari S, Ajmera V, Singh S, Murad MH, Loomba R. Global prevalence of advanced liver fibrosis and cirrhosis in the general population: a systematic review and meta-analysis. Clin Gastroenterol Hepatol. 2025;23:1123–34.
Unger RH, Scherer PE. Gluttony, sloth and the metabolic syndrome: a roadmap to lipotoxicity. Trends Endocrinol Metab. 2010;21:345–52.
Gavin KM, Bessesen DH. Sex differences in adipose tissue function. Endocrinol Metab Clin North Am. 2020;49:215–28.
Lee BP, Dodge JL, Terrault NA. National prevalence estimates for steatotic liver disease and subclassifications using consensus nomenclature. Hepatology. 2024;79:666–73.
Ipsen DH, Lykkesfeldt J, Tveden-Nyborg P. Molecular mechanisms of hepatic lipid accumulation in non-alcoholic fatty liver disease. Cell Mol Life Sci. 2018;75:3313–27.
Katsiki N, Mikhailidis DP, Mantzoros CS. Non-alcoholic fatty liver disease and dyslipidemia: an update. Metabolism. 2016;65:1109–23.
Gluchowski NL, Becuwe M, Walther TC, Farese RV Jr. Lipid droplets and liver disease: from basic biology to clinical implications. Nat Rev Gastroenterol Hepatol. 2017;14:343–55.
Musso G, Saba F, Cassader M, Gambino R. Lipidomics in pathogenesis, progression and treatment of nonalcoholic steatohepatitis (NASH): recent advances. Prog Lipid Res. 2023;91:101238.
Ghadir MR, Riahin AA, Havaspour A, Nooranipour M, Habibinejad AA. The relationship between lipid profile and severity of liver damage in cirrhotic patients. Hepat Mon. 2010;10:285–8.
Xia T, Du M, Li H, Wang Y, Zha J, Wu T, et al. Association between liver MRI proton density fat fraction and liver disease risk. Radiology. 2023;309:e231007.
Arvind A, Osganian SA, Cohen DE, Corey KE. Lipid and lipoprotein metabolism in liver disease. In: Feingold KR, Ahmed SF, Anawalt B, Blackman MR, Boyce A, Chrousos G, et al., editors. Endotext. South Dartmouth (MA): MDText.com, Inc. Copyright © 2000-2025, MDText.com,Inc.; 2000.
Hoekstra M, Van Eck M. High-density lipoproteins and non-alcoholic fatty liver disease. Atheroscler Plus. 2023;53:33–41.
Chait A, den Hartigh LJ. Adipose tissue distribution, inflammation and its metabolic consequences, including diabetes and cardiovascular disease. Front Cardiovasc Med. 2020;7:22.
Freedland ES. Role of a critical visceral adipose tissue threshold (CVATT) in metabolic syndrome: implications for controlling dietary carbohydrates: a review. Nutr Metab (Lond). 2004;1:12.
Pivovarova-Ramich O, Loske J, Hornemann S, Markova M, Seebeck N, Rosenthal A, et al. Hepatic Wnt1 inducible signaling pathway protein 1 (WISP-1/CCN4) associates with markers of liver fibrosis in severe obesity. Cells. 2021;10:1048.
Shim YR, Jeong WI. Recent advances of sterile inflammation and inter-organ cross-talk in alcoholic liver disease. Exp Mol Med. 2020;52:772–80.
Kulkarni A, Bowers LW. The role of immune dysfunction in obesity-associated cancer risk, progression, and metastasis. Cell Mol Life Sci. 2021;78:3423–42.
Chen HW, Wang SA, Xu ZY, Shao ZH, Zhong Q, Wei YF, et al. Association of predicted visceral fat percentage with dementia risk in older adults: the role of genetic risk and lifestyle. Neurology. 2025;104:e213630.
Acknowledgements
The authors wish to express their gratitude to all the participants of the UK Biobank and all individuals involved in establishing the UK Biobank study.
Funding
This study was supported by the National Natural Science Foundation of China (82173607) and the Guangdong Basic and Applied Basic Research Foundation (2024A1515011969).
Author information
Authors and Affiliations
Contributions
SAW provided substantial contributions to the conception and design. SAW, HWC, QZ and ZYX contributed to data analysis and interpretation. SAW and HWC drafted the article. QZ, ZYX, YFW, CYZ, QRL, ZHS, KL and BFC contributed to visualisation. All authors critically revised the article and approved the final version to be published.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Wang, SA., Chen, HW., Zhong, Q. et al. Association between metabolic signatures of predicted VAT mass and risk of MASLD and other chronic liver diseases. Int J Obes (2026). https://doi.org/10.1038/s41366-026-02067-6
Received:
Revised:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41366-026-02067-6