Abstract
Background
Hurricane Maria left many homes in Puerto Rico with prolonged flooding, structural damage, and indoor microbial growth, conditions that can drive respiratory illness and immune dysregulation.
Objective
To assess the pro-inflammatory potential of post-flooding indoor dust and track two-year shifts in household risk profiles by integrating pro-inflammatory biomarkers, fungal exposure, and self-reported structural damage, mental health, and respiratory outcomes.
Methods
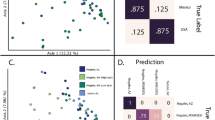
Dust samples were collected from 50 households in a San Juan community one year and again from 35 of those same households two years after the hurricane. Dust sample extracts (DSEs) were prepared and incubated with pooled peripheral blood from volunteers residing outside Puerto Rico. Pro-inflammatory cytokines interleukin-1β (IL-1β), IL-6, and IL-8 were quantified using ELISA; airborne fungal abundance was assessed on malt extract and G25N agars. Survey data captured self-reported respiratory and mental-health scores using the SF-12v2 Health Survey, structural water damage, and remediation efforts. Principal component analysis (PCA) and k-means clustering were applied to identify household clusters, while Sankey plots were used to visualize the transitions of household risk.
Results
IL-1β emerged as the most responsive cytokine, showing the greatest median reduction from Year 1 to Year 2 and across household water-damage categories. Three clusters emerged in Year 1, driven by structural damage, IL-1β, and fungal load. By Year 2, only two clusters remained, shaped more by self-reported respiratory and psychological distress than by structural damage. Sankey analysis revealed that some households transitioned into higher-risk profiles over time despite apparent household structural recovery.
Impact
-
Indoor environmental hazards persist long after floodwaters in the aftermaths of hurricanes recede, yet few studies integrate biological, environmental, structural, psychosocial, and respiratory health data to track household risk over time.
-
Using a human whole-blood pyrogen assay and multivariate clustering, this two-year study of Hurricane-María–affected homes in Puerto Rico shows that dust-induced IL-1β is a sensitive pro-inflammatory biomarker and that residual risk shifts from structural-microbial drivers to psychosocial-respiratory burdens during recovery.
-
The multidomain “risk-profile” framework provides a reproducible template for post-disaster exposure assessment and can help public-health officials prioritize targeted remediation, health surveillance, and mental-health support as climate-related disasters increase.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 6 print issues and online access
$259.00 per year
only $43.17 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
Data availability
The metadata for this study can be found at the following link: https://osf.io/fmkhj/?view_only=9fe2324f73c24c82b745f5bc5e3f143d.
References
Reuben A, Manczak EM, Cabrera LY, Alegria M, Bucher ML, Freeman EC, et al. The interplay of environmental exposures and mental health: setting an agenda. Environ Health Perspect. 2022;130:25001.
Schwartz RM, Gillezeau CN, Liu B, Lieberman-Cribbin W, Taioli E. Longitudinal impact of hurricane sandy exposure on mental health symptoms. Int J Environ Res Public Health. 2017;14:957.
Li A, Toll M, Martino E, Wiesel I, Botha F, Bentley R. Vulnerability and recovery: long-term mental and physical health trajectories following climate-related disasters. Soc Sci Med. 2023;320:115681.
Rando RJ, Lefante JJ, Freyder LM, Jones RN. Respiratory health effects associated with restoration work in post-Hurricane Katrina New Orleans. J Environ Public Health. 2012;2012:462478.
Schwab KJ, Gibson KE, Williams DAL, Kulbicki KM, Lo CP, Mihalic JN, et al. Microbial and chemical assessment of regions within New Orleans, LA impacted by Hurricane Katrina. Environ Sci Technol. 2007;41:2401–6.
Brandt M, Brown C, Burkhart J, Burton N, Cox-Ganser J, Damon S, et al. Mold prevention strategies and possible health effects in the aftermath of hurricanes and major floods. MMWR. Recommendations and reports : Morbidity and mortality weekly report. Recomm Rep / Cent Dis Control. 2006;55:1–27.
Rao CY, Kurukularatne C, Garcia-Diaz JB, Kemmerly SA, Reed D, Fridkin SK, et al. Implications of detecting the mold syncephalastrum in clinical specimens of New Orleans residents after Hurricanes Katrina and Rita. J Occup Environ Med. 2007;49:411.
Adams TN, Redlich CA, Glazer CS, Gulati M. Hypersensitivity pneumonitis associated with home mold exposure: a retrospective cohort analysis. PLoS ONE. 2025;20:e0323093.
Pakdehi M, Ahmadisharaf E, Azimi P, Yan Z, Keshavarz Z, Caballero C, et al. Modeling the latent impacts of extreme floods on indoor mold spores in residential buildings: application of machine learning algorithms. Environ Int. 2025;196:109319.
Bakshi A, Van Doren A, Berens AS, Jacob C, Omari A, Foreman A, et al. Sociodemographic and housing factors for flood and mold damage in the Greater New Orleans Area after Hurricane Ida. Disaster Med Public Health Prep. 2025;19:e164.
Al-Shaarani A, Pecoraro L. A review of pathogenic airborne fungi and bacteria: unveiling occurrence, sources, and profound human health implication. Front Microbiol. 2024;15:1428415.
Pasch RJ, Penny AB, Berg R. Tropical Cyclone Report: Hurricane Maria (AL152017), 16-30 September 2017. Miami, FL: National Hurricane Center, National Oceanic and Atmospheric Administration; 2018.
Rivera R, Rolke W. Estimating the death toll of Hurricane Maria. Significance. 2018;15:8–9.
Orengo-Aguayo R, Stewart RW, de Arellano MA, Suárez-Kindy JL, Young J. Disaster exposure and mental health among puerto rican youths after Hurricane Maria. JAMA Netw Open. 2019;2:e192619.
Gargano LM, Locke S, Jordan HT, Brackbill RM. Lower respiratory symptoms associated with environmental and reconstruction exposures after Hurricane Sandy. Disaster Med Public Health Prep. 2018;12:697–702.
Barbeau DN, Grimsley LF, White LE, El-Dahr JM, Lichtveld M. Mold exposure and health effects following Hurricanes Katrina and Rita. Annu Rev Public Health. 2010;31:165–78.
Rao CY, Riggs MA, Chew GL, Muilenberg ML, Thorne PS, Sickle DV, et al. Characterization of airborne molds, endotoxins, and glucans in homes in New Orleans after Hurricanes Katrina and Rita. Appl Environ Microbiol. 2007;73:1630–4.
Bloom E, Grimsley LF, Pehrson C, Lewis J, Larsson L. Molds and mycotoxins in dust from water-damaged homes in New Orleans after Hurricane Katrina. Indoor Air. 2009;19:153–8.
Rabito FA, Iqbal S, Kiernan MP, Holt E, Chew GL. Children’s respiratory health and mold levels in New Orleans after Katrina: a preliminary look. J Allergy Clin Immunol. 2008;121:622–5.
Chew GL, Wilson J, Rabito FA, Grimsley F, Iqbal S, Reponen T, et al. Mold and endotoxin levels in the aftermath of Hurricane Katrina: a pilot project of homes in New Orleans undergoing renovation. Environ Health Perspect. 2006;114:1883–9.
He Q, Gao H, L-m, Xu, Lu Y, Wang C, et al. Analysis of IL-6 and IL-1β release in cryopreserved pooled human whole blood stimulated with endotoxin. Innate Immun. 2018;24:316–22.
Farokhi A, Heederik D, Smit LAM. Respiratory health effects of exposure to low levels of airborne endotoxin – a systematic review. Environ Health. 2018;17:14.
Mendy A, Salo PM, Cohn RD, Wilkerson J, Zeldin DC, Thorne PS. House dust endotoxin association with chronic bronchitis and emphysema. Environ Health Perspect. 2018;126:037007.
Zhang Z, Myers JMB, Brandt EB, Ryan PH, Lindsey M, Mintz-Cole RA, et al. β-Glucan exacerbates allergic asthma independent of fungal sensitization and promotes steroid-resistant TH2/TH17 responses. J Allergy Clin Immunol. 2017;139:54–65.e8.
Noss I, Ozment TR, Graves BM, Kruppa MD, Rice PJ, Williams DL. Cellular and molecular mechanisms of fungal β-(1→6)-glucan in macrophages. Innate Immun. 2015;21:759–69.
Meldrum K, Evans SJ, Burgum MJ, Doak SH, Clift MJD. Determining the toxicological effects of indoor air pollution on both a healthy and an inflammatory-comprised model of the alveolar epithelial barrier in vitro. Part Fibre Toxicol. 2024;21:25.
Velez-Torres LN, Bolanos-Rosero B, Godoy-Vitorino F, Rivera-Mariani FE, Maestre JP, Kinney K, et al. Hurricane Maria drives increased indoor proliferation of filamentous fungi in San Juan, Puerto Rico: a two-year culture-based approach. PeerJ. 2022;10:e12730.
Negherbon JP, Romero K, Williams DAL, Guerrero-Preston RE, Hartung T, Scott AL, et al. Whole blood cytokine response to local traffic-related particulate matter in Peruvian children with and without asthma. Front Pharmacol. 2017;8:157.
Rivera-Mariani FE, Vysyaraju K, Negherbon J, Levetin E, Horner WE, Hartung T, et al. Comparison of the Interleukin-1β-inducing potency of allergenic spores from higher fungi (Basidiomycetes) in a cryopreserved human whole blood system. Int Arch Allergy Immunol. 2014;163:154–62.
Daneshian M, Aulock Sv, Hartung T. Assessment of pyrogenic contaminations with validated human whole-blood assay. Nat Protoc. 2009;4:1709–21.
Ulland TK, Ferguson PJ, Sutterwala FS. Evasion of inflammasome activation by microbial pathogens. J Clin Investig. 2015;125:469–77.
Wouters IM, Douwes J, Thorne PS, Heederik D, Doekes G. Inter- and intraindividual variation of endotoxin- and β(1 → 3)-glucan-induced cytokine responses in a whole blood assay. Toxicol Ind Health. 2002;18:15–27.
Terpstra T, Gutteling JM, Geldof GD, Kappe LJ. The perception of flood risk and water nuisance. Water Sci Technol. 2006;54:431–9.
Terpstra, T. Re: Informaation request/Risk perception instrument [Email]. (2019).
Bose S, Rivera-Mariani F, Chen R, Williams D, Belli A, Aloe C, et al. Domestic exposure to endotoxin and respiratory morbidity in former smokers with COPD. Indoor Air. 2016;26:734–42.
Rivera-Mariani FE. Cryopreserved human whole blood: a human-based in vitro immunotoxicological system. Alterna Lab Anim. 2013;41:483–90.
Vesentini S, Soncini M, Fiore GB, Redaelli A. Mechanisms of Polymyxin B endotoxin removal from extracorporeal blood flow: molecular interactions. Contrib Nephrol. 2010;167:45–54.
Mantovani A, Dinarello CA, Molgora M, Garlanda C. Interleukin-1 and related cytokines in the regulation of inflammation and immunity. Immunity. 2019;50:778–95.
Jung Y, Wen T, Mingler MK, Caldwell JM, Wang YH, Chaplin DD, et al. IL-1β in eosinophil-mediated small intestinal homeostasis and IgA production. Mucosal Immunol. 2015;8:930.
Dinarello CA. Interleukin-1 in the pathogenesis and treatment of inflammatory diseases. Blood. 2011;117:3720–32.
Franchi L, Kamada N, Nakamura Y, Burberry A, Kuffa P, Suzuki S, et al. NLRC4-driven production of IL-1β discriminates between pathogenic and commensal bacteria and promotes host intestinal defense. Nat Immunol. 2012;13:449.
Tröger B, Heidemann M, Osthues I, Knaack D, Göpel W, Herting E, et al. Modulation of S. epidermidis-induced innate immune responses in neonatal whole blood. J Microbiol Immunol Infect 2018;53:240–9.
Liebers V, Raulf-Heimsoth M, Linsel G, Goldscheid N, Düser M, Stubel H, et al. Evaluation of quantification methods of occupational endotoxin exposure. J Toxicol Environ Health Part A. 2007;70:1798–805.
Alwis KU, Milton DK. Recombinant factor C assay for measuring endotoxin in house dust: comparison with LAL, and (1 → 3)-β-D-glucans. Am J Ind Med. 2006;49:296–300.
Oneal GA, Postma J, Odom-Maryon T, Butterfield P. Retest of a principal components analysis of two household environmental risk instruments. Res Nurs Health. 2016;39:277–85.
Homenauth E, Kajeguka D, Kulkarni MA. Principal component analysis of socioeconomic factors and their association with malaria and arbovirus risk in Tanzania: a sensitivity analysis. J Epidemiol Community Health. 2017;71:1046–51.
Hailu A, Lindtjorn B, Deressa W, Gari T, Loha E, Robberstad B. Equity in long-lasting insecticidal nets and indoor residual spraying for malaria prevention in a rural South Central Ethiopia. Malar J. 2016;15:366.
Shezi B, Jafta N, Naidoo RN. Potential health risks of indoor particulate matter heavy metals in resource-constrained settings of South Africa. Atmosphere. 2024;15:911.
Mikolai J, Keenan K, Kulu H. Intersecting household-level health and socio-economic vulnerabilities and the COVID-19 crisis: an analysis from the UK. SSM Popul Health. 2020;12:100628.
Mwalwimba IK, Manda M, Ngongondo C. Measuring vulnerability to assess households resilience to flood risks in Karonga district, Malawi. Nat Hazards. 2024;120:6609–28.
John Vincent EL. Unveiling the recipe for disaster vulnerability: a multidimensional analysis in Dumaguete City, Philippines. Philipp Soc Sci J. 2024;6:85–95.
Acknowledgements
We are grateful to all the families that participated in this study, and the volunteers who participated in the blood draws. We also want to acknowledge Summer Pellechio and Ruslan Fomenko, who contributed to performing human whole blood and immunological assays. We are also grateful to the field team for their remarkable job administering the surveys and carrying out the indoor sampling of the homes.
Funding
This work was supported by the National Institute of Environmental Health Sciences of the National Institute of Health (R21ES029762). The funding body was not involved in study design; data collection, analysis, or interpretation; manuscript preparation; or the decision to submit for publication. The content is solely the responsibility of the authors and does not necessarily represent the official views of the funders.
Author information
Authors and Affiliations
Contributions
Conceptualization: Felix E. Rivera-Mariani, Hayat Srour, Filipa Godoy-Vitorino, Benjamín Bolaños-Rosero, Lorraine N. Vélez-Torres, Juan P. Maestre, Kerry Kinney, Humberto Cavallin. Funding Acquisition: Humberto Cavallin, Kerry Kinney, Juan P. Maestre, Felix E. Rivera-Mariani, Filipa Godoy-Vitorino, Benjamín Bolaños-Rosero. Field Sampling: Humberto Cavallin, Juan P. Maestre, Lorraine N. Vélez-Torres, Benjamín Bolaños-Rosero. Project Administration: Humberto Cavallin, Kerry Kinney. Immunological Analysis: Felix E. Rivera-Mariani, Hayat Srour. Data Analysis: Felix E. Rivera-Mariani, Hayat Srour. Writing: Felix E. Rivera-Mariani, Hayat Srour, Filipa Godoy-Vitorino, Benjamín Bolaños-Rosero, Lorraine N. Vélez-Torres, Juan P. Maestre, Kerry Kinney, Humberto Cavallin.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethics approval
All procedures involving human participants were performed in accordance with relevant guidelines and regulations, including the Declaration of Helsinki and institutional policies. The household recruitment, survey administration, and in-home environmental sampling (dust/air) were approved by the University of Puerto Rico–Río Piedras Institutional Review Board (IRB #1718-058). Whole-blood draws for the human whole-blood pyrogen assay (HWBPA) was approved by the Larkin University Institutional Review Board (IRB protocol LCH-1-022018). Only adults (≥21 years) were enrolled. Informed consent was obtained from all participants, including the primary household respondent for survey and sampling, and all blood donors for phlebotomy and use of de-identified samples. This manuscript contains no identifiable images or personal data of individual participants.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Rivera-Mariani, F.E., Srour, H., Godoy-Vitorino, F. et al. Indoor dust, immune activation, and household exposure risk after Hurricane Maria: a two-year pilot prospective cohort study in Puerto Rico. J Expo Sci Environ Epidemiol (2025). https://doi.org/10.1038/s41370-025-00835-6
Received:
Revised:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41370-025-00835-6