Abstract
Objective
To investigate potential factors influencing initial length of hospital stay (LOS) for infants with neonatal abstinence syndrome (NAS) in Florida.
Methods
The study population included 2984 term, singleton live births in 33 Florida hospitals. We used hierarchical linear modeling to evaluate the association of community, hospital, and individual factors with LOS.
Results
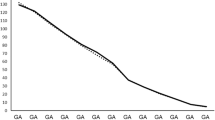
The average LOS of infants diagnosed with NAS varied significantly across hospitals. Individual-level factors associated with increased LOS for NAS included event year (P < 0.001), gestational age at birth (P < 0.001), maternal age (P = 0.002), maternal race and ethnicity (P < 0.001), maternal education (P = 0.032), and prenatal care adequacy (P < 0.001). Average annual hospital NAS volume (P = 0.022) was a significant hospital factor.
Conclusion
NAS varies widely across hospitals in Florida. In addition to focusing on treatment regimens, to reduce LOS, public health and quality improvement initiatives should identify and adopt strategies that can minimize the prevalence and impact of these contributing factors.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Hudak ML, Tan RC. Neonatal drug withdrawal. Pediatrics. 2012;129:e540–60.
Harper RG, Solish GI, Purow HM, Sang E, Panepinto WC. The effect of a methadone treatment program upon pregnant heroin addicts and their newborn infants. Pediatrics. 1974;54:300–5.
Fricker HS. Narcotic addiction, pregnancy, and the newborn. Am J Dis Child. 1978;132:360.
Madden JD, Chappel JN, Zuspan F, Gumpel J, Mejia A, Davis R. Observation and treatment of neonatal narcotic withdrawal. Am J Obstet Gynecol. 1977;127:199–201.
Ostrea EM, Chavez CJ, Strauss ME. A study of factors that influence the severity of neonatal narcotic withdrawal. J Pediatr. 1976;88:642–5.
Winkelman TNA, Villapiano N, Kozhimannil KB, Davis MM, Patrick SW. Incidence and costs of neonatal abstinence syndrome among infants with Medicaid: 2004–2014. Pediatrics. 2018;141.
Ko JY, Patrick SW, Tong VT, Patel R, Lind JN, Barfield WD. Incidence of neonatal abstinence syndrome—28 States, 1999–2013. Morb Mortal Wkly Rep. 2016;65:799–802.
Patrick SW, Davis MM, Lehmann CU, Cooper WO, Cooper WO. Increasing incidence and geographic distribution of neonatal abstinence syndrome: United States 2009 to 2012. J Perinatol. 2015;35:650–5.
McQueen K, Murphy-Oikonen J. Neonatal Abstinence Syndrome. Longo DL, editor. N Engl J Med. 2016;375:2468–79.
Tolia VN, Patrick SW, Bennett MM, Murthy K, Sousa J, Smith PB, et al. Increasing Incidence of the Neonatal Abstinence Syndrome in U.S. Neonatal ICUs. N Engl J Med. 2015;372:2118–26.
Cleary BJ, Donnelly JM, Strawbridge JD, Gallagher PJ, Fahey T, White MJ, et al. Methadone and perinatal outcomes: a retrospective cohort study. Am J Obstet Gynecol. 2011;204:139.e1–9.
Lee J, Hulman S, Musci M, Stang E. Neonatal abstinence syndrome: influence of a combined inpatient/outpatient methadone treatment regimen on the average length of stay of a Medicaid NICU population. Popul Health Manag. 2015;18:392–7.
Tolia VN, Murthy K, Bennett MM, Greenberg RG, Benjamin DK, Smith PB, et al. Morphine vs methadone treatment for infants with neonatal abstinence syndrome. J Pediatr. 2018;203:185–9.
Brown MS, Hayes MJ, Thornton LM. Methadone versus morphine for treatment of neonatal abstinence syndrome: a prospective randomized clinical trial. J Perinatol. 2015;35:278–83.
Patrick SW, Kaplan HC, Passarella M, Davis MM, Lorch SA. Variation in treatment of neonatal abstinence syndrome in US children’s hospitals, 2004–2011. J Perinatol. 2014;34:867–72.
Hall ES, Wexelblatt SL, Crowley M, Grow JL, Jasin LR, Klebanoff MA, et al. A multicenter cohort study of treatments and hospital outcomes in neonatal abstinence syndrome. Pediatrics. 2014;134:e527–34.
Patrick SW, Schumacher RE, Benneyworth BD, Krans EE, McAllister JM, Davis MM. Neonatal abstinence syndrome and associated health care expenditures: United States, 2000–2009. JAMA. 2012;307:1934–40.
Corr TE, Hollenbeak CS. The economic burden of neonatal abstinence syndrome in the United States. Addiction. 2017;112:1590–9.
Hekman KA, Grigorescu VI, Cameron LL, Miller CE, Smith RA. Neonatal withdrawal syndrome, Michigan, 2000–2009. Am J Prev Med. 2013;45:113–7.
Grisham LM, Stephen MM, Coykendall MR, Kane MF, Maurer JA, Bader MY. Eat, sleep, console approach: a family-centered model for the treatment of neonatal abstinence syndrome. Adv Neonatal Care. 2019;19:138–44.
Grossman MR, Lipshaw MJ, Osborn RR, Berkwitt AK. A novel approach to assessing infants with neonatal abstinence syndrome. Hosp Pediatr. 2018;8:1–6.
Kotelchuck M. An evaluation of the Kessner adequacy of prenatal care index and a proposed adequacy of prenatal care utilization index. Am J Public Health. 1994;84:1414–20.
Florida Department of Health. FLHealthCHARTS—birth query system. 2019. http://www.flhealthcharts.com/FLQUERY/Birth/BirthRpt.aspx.
Ko JY, Wolicki S, Barfield WD, Patrick SW, Broussard CS, Yonkers KA, et al. CDC grand rounds: public health strategies to prevent neonatal abstinence syndrome. Morb Mortal Wkly Rep. 2017;66:242–5.
Florida Department of Health. E-FORCSE Home Page. 2019. http://www.floridahealth.gov/statistics-and-data/e-forcse/.
ACOG Committee on Health Care for Underserved Women; American Society of Addiction Medicine. ACOG Committee Opinion No. 524: opioid abuse, dependence, and addiction in pregnancy. Obstet Gynecol. 2012;119:1070–6.
Substance Abuse and Mental Health Services Administration. Federal guidelines for opioid treatment programs. HHS Publication No. (SMA) PEP15-FEDGUIDEOTP. 2015. http://store.samhsa.gov.
Wachman EM, Grossman M, Schiff DM, Philipp BL, Minear S, Hutton E, et al. Quality improvement initiative to improve inpatient outcomes for Neonatal Abstinence Syndrome. J Perinatol. 2018;38:1114–22.
Krans EE, Cochran G, Bogen DL. Caring for opioid-dependent pregnant women: prenatal and postpartum care considerations. Clin Obstet Gynecol. 2015;58:370–9.
Jutte DP, Roos LL, Brownell MD. Administrative record linkage as a tool for public health research. Annu Rev Public Health. 2011;32:91–108.
Funding
This study was partially supported by a contract from the Florida Department of Health.
Author information
Authors and Affiliations
Contributions
All authors conceptualized and designed the study. CNR, and TRF conducted data analysis. CNR drafted the initial manuscript and received critical input from TRF, AKM, MLH, MB, RSK, REW, and WMS in the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Reid, C.N., Foti, T.R., Mbah, A.K. et al. Multilevel factors associated with length of stay for neonatal abstinence syndrome in Florida’s NICUs: 2010–2015. J Perinatol 41, 1389–1396 (2021). https://doi.org/10.1038/s41372-020-00815-8
Received:
Revised:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41372-020-00815-8
This article is cited by
-
Maternal substance use disorder and neonatal health: epidemiologic and socioeconomic determinants in a case-control study, Shiraz, Iran
BMC Pregnancy and Childbirth (2025)
-
Increasing usage of mother’s own milk in neonates at risk of neonatal abstinence syndrome: MOM-NAS quality improvement initiative
Journal of Perinatology (2021)