Abstract
Objective
Characterize the types and doses of commonly administered perioperative drugs in inguinal hernia (IH) repair for premature infants.
Study design
Single-center, retrospective cohort study.
Results
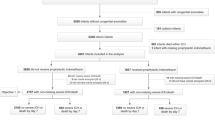
In total, 112 premature infants underwent IH repair between 2010 and 2015. Twenty-one drugs were used during IH repair, with each infant receiving a median seven drugs. Acetaminophen (88%), bupivacaine (84%), cisatracurium (74%), sevoflurane (72%), and propofol (71%) were the most commonly used agents. Thirty-two infants underwent additional procedures with IH repair. Additional procedures were not associated with a higher number of perioperative drugs, however infants with additional procedures were exposed to higher cumulative doses of cisatracurium (p < 0.001) and fentanyl (p = 0.002).
Conclusion
There is wide variability in the drugs and doses used for a common surgical procedure in this population, even within a single center. Future research should focus on the safety and efficacy of the most commonly used perioperative drugs described in this study.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Filan PM, Hunt RW, Anderson PJ, Doyle LW, Inder TE. Neurologic outcomes in very preterm infants undergoing surgery. J Pediatr. 2012;160:409–14.
Stolwijk LJ, Keunen K, de Vries LS, Groenendaal F, van der Zee DC, van Herwaarden MYA, et al. Neonatal surgery for noncardiac congenital anomalies: neonates at risk of brain injury. J Pediatr. 2017;182:335–41 e331.
Hunt RW, Hickey LM, Burnett AC, Anderson PJ, Cheong JLY, Doyle LW, et al. Early surgery and neurodevelopmental outcomes of children born extremely preterm. Arch Dis Child Fetal Neonatal Ed. 2018;103:F227–F232.
Anand KJ, Sippell WG, Aynsley-Green A. Randomised trial of fentanyl anaesthesia in preterm babies undergoing surgery: effects on the stress response. Lancet. 1987;1:243–8.
Hatfield LA, Meyers MA, Messing TM. A systematic review of the effects of repeated painful procedures in infants: is there a potential to mitigate future pain responsivity? J Nurs Educ Pract. 2013;3:99–112.
Hillier SC, Krishna G, Brasoveanu E. Neonatal anesthesia. Semin Pediatr Surg. 2004;13:142–51.
Harris PA, Taylor R, Thielke R, Payne J, Gonzalez N, Conde JG. Research electronic data capture (REDCap)-a metadata-driven methodology and workflow process for providing translational research informatics support. J Biomed Inform. 2009;42:377–81.
Harris PA, Taylor R, Minor BL, Elliott V, Fernandez M, O’Neal L, et al. The REDCap consortium: building an international community of software platform partners. J Biomed Inform. 2019;95:103208.
U.S. Food and Drug Administration. Drug safety and availability—FDA drug safety communication: FDA review results in new warnings about using general anesthetics and sedation drugs in young children and pregnant women. 2016. https://www.fda.gov/Drugs/DrugSafety/ucm532356.htm. Accessed 25 Feb 2020.
Briner A, Nikonenko I, De Roo M, Dayer A, Muller D, Vutskits L. Developmental stage-dependent persistent impact of propofol anesthesia on dendritic spines in the rat medial prefrontal cortex. Anesthesiology. 2011;115:282–93.
Brambrink AM, Back SA, Riddle A, Gong X, Moravec MD, Dissen GA, et al. Isoflurane-induced apoptosis of oligodendrocytes in the neonatal primate brain. Ann Neurol. 2012;72:525–35.
Creeley CE, Dikranian KT, Dissen GA, Back SA, Olney JW, Brambrink AM. Isoflurane-induced apoptosis of neurons and oligodendrocytes in the fetal rhesus macaque brain. Anesthesiology. 2014;120:626–38.
Woodward TJ, Timic Stamenic T, Todorovic SM. Neonatal general anesthesia causes lasting alterations in excitatory and inhibitory synaptic transmission in the ventrobasal thalamus of adolescent female rats. Neurobiol Dis. 2019;127:472–81.
Sun LS, Li G, Miller TL, Salorio C, Byrne MW, Bellinger DC, et al. Association between a single general anesthesia exposure before age 36 months and neurocognitive outcomes in later childhood. JAMA. 2016;315:2312–20.
Warner DO, Zaccariello MJ, Katusic SK, Schroeder DR, Hanson AC, Schulte PJ, et al. Neuropsychological and behavioral outcomes after exposure of young children to procedures requiring general anesthesia: The Mayo Anesthesia Safety in Kids (MASK) study. Anesthesiology. 2018;129:89–105.
McCann ME, de Graaff JC, Dorris L, Disma N, Withington D, Bell G, et al. Neurodevelopmental outcome at 5 years of age after general anaesthesia or awake-regional anaesthesia in infancy (GAS): an international, multicentre, randomised, controlled equivalence trial. Lancet. 2019;393:664–77.
Chidambaran V, Costandi A, D’Mello A. Propofol: a review of its role in pediatric anesthesia and sedation. CNS Drugs. 2015;29:543–63.
Filho EM, Riechelmann MB. Propofol use in newborns and children: is it safe? A systematic review. J Pediatr. 2020;96:289–309.
Ramgolam A, Hall GL, Zhang G, Hegarty M, von Ungern-Sternberg BS. Inhalational versus intravenous induction of anesthesia in children with a high risk of perioperative respiratory adverse events: a randomized controlled trial. Anesthesiology. 2018;128:1065–74.
Hong H, Hahn S, Choi Y, Jang MJ, Kim S, Lee JH, et al. Evaluation of propofol in comparison with other general anesthetics for surgery in children younger than 3 years: a systematic review and meta-analysis. J Korean Med Sci. 2019;34:e124.
Shah PS, Shah VS. Propofol for procedural sedation/anaesthesia in neonates. Cochrane Datab Syst Rev. 2011;3:Cd007248.
Loepke AW, Soriano SG. An assessment of the effects of general anesthetics on developing brain structure and neurocognitive function. Anesth Analg. 2008;106:1681–707.
Kumar VH, Clive J, Rosenkrantz TS, Bourque MD, Hussain N. Inguinal hernia in preterm infants (< or = 32-week gestation). Pediatr Surg Int. 2002;18:147–52.
Funding
NHLBI K24 HL143283.
Author information
Authors and Affiliations
Contributions
CD, SEH, RGG, KMC, MML, and WMJ: Conceived and designed the analysis. CD and WMJ: Performed the analysis and wrote the first draft of the manuscript. SEH, PPM, KOZ, DKB, RGG, KMC, MML: Reviewed and made significant edits to the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Dorismond, C., Hunter, S.E., McNaull, P.P. et al. Wide range of perioperative drugs and doses used in inguinal hernia repairs for premature infants. J Perinatol 41, 577–581 (2021). https://doi.org/10.1038/s41372-020-00864-z
Received:
Revised:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41372-020-00864-z