Abstract
Objective
To evaluate whether in a historical cohort of preterm infants, body composition at term equivalent age (TEA) correlated with Bayley scores at 2 years of corrected age.
Study design
Ninety-five preterm babies were admitted to our neonatal intensive unit and underwent air-displacement plethysmography assessment at TEA. Of these, 74 completed Bayley tests at 2 years. We used multiple linear regression analysis to assess the association of body composition with Bayley scores.
Results
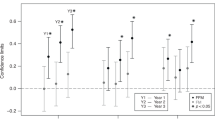
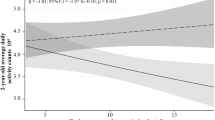
Mean gestational age and birthweight of our population were respectively 29.8 (±2.2) weeks and 1150 (±330) grams. Higher fat-free mass (FFM) z-score was associated with higher language (adjusted r = 0.28, p = 0.03) and motor composite scores (adjusted r = 0.33, p = 0.03) in both univariate and multiple regression analysis including birth weight, sex, maternal university degree, mechanical ventilation, and bilingualism.
Conclusions
In our study FFM at term equivalent age was associated with higher Bayley composite motor and language scores at 2 years.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Johnson MJ, Wootton SA, Leaf AA, Jackson AA. Preterm birth and body composition at term equivalent age: a systematic review and meta-analysis. Pediatrics. 2012;130:e640–9.
Ehrenkranz RA, Dusick AM, Vohr BR, Wright LL, Wrage LA, Poole WK. Growth in the neonatal intensive care unit influences neurodevelopmental and growth outcomes of extremely low birth weight infants. Pediatrics. 2006;117:1253–61.
Ramel SE, Gray HL, Christiansen E, Boys C, Georgieff MK, Demerath EW. Greater early gains in fat-free mass, but not fat mass, are associated with improved neurodevelopment at 1 year corrected age for prematurity in very low birth weight preterm infants. J Pediatr. 2016;173:108–15.
Pfister KM, Zhang L, Miller NC, Ingolfsland EC, Demerath EW, Ramel SE. Early body composition changes are associated with neurodevelopmental and metabolic outcomes at 4 years of age in very preterm infants. Pediatr Res. 2018;84:713–8.
Scheurer JM, Zhang L, Plummer EA, Hultgren SA, Demerath EW, Ramel SE. Body composition changes from infancy to 4 Years and associations with early childhood cognition in preterm and full-term children. Neonatology. 2018;114:169–76.
Frondas-Chauty A, Simon L, Flamant C, Hanf M, Darmaun D, Rozé JC. Deficit of Fat Free Mass inVery Preterm Infants at Discharge is Associated with neurological Impairment at Age 2 Years. J Pediatr. 2018;196:301–4.
Ramel SE, Haapala J, Super J, Boys C, Demerath EW. Nutrition, illness and body composition in very low birth weight preterm infants: implications for nutritional management and neurocognitive outcomes. Nutrients. 2020;12:145.
Paviotti G, De Cunto A, Zennaro F, Boz G, Travan L, Cont G, et al. Higher growth, fat and fat-free masses correlate with larger cerebellar volumes in preterm infants at term. Acta Paediatr. 2017;106:918–25.
Urlando A, Dempster P, Aitkens S. A new air displacement plethysmograph for the measurement of body composition in infants. Pediatr Res. 2003;53:486–92.
Bertino E, Spada E, Occhi L, Coscia A, Giuliani F, Gagliardi L, et al. Neonatal anthropometric charts: the Italian neonatal study compared with other European studies. J Pediatr Gastroenterol Nutr. 2010;51:353–61.
Norris T, Ramel S, Catalano P, Caoimh C, Roggero P, Murray D, et al. New charts for the assessment of body composition, according to air-displacement plethysmography, at birth and across the first 6 mo of life. Am J Clin Nutr. 2019;109:1353–60.
Shim SY, Ahn HM, Cho SJ, Park EU. Early aggressive nutrition enhances language development in very low-birthweight infants. Pediatrics Int. 2014;56:845–50.
Simon L, Théveniaut C, Flamant C, Frondas-Chauty A, Darmaun D, Rozé JC. In preterm infants, length growth below expected growth during hospital stay predicts poor neurodevelopment at 2 years. Neonatology. 2018;114:135–41.
Belfort MB, Gillman MW, Buka SL, Casey PH, McCormick MC. Preterm infant linear growth and adiposity gain: trade-offs for later weight status and intelligence quotient. J Pediatr. 2013;163:1564–9.
Ramel SE, Demerath EW, Gray HL, Younge N, Boys C, Georgieff MK. The relationship of poor linear growth velocity with neonatal illness and two-year neurodevelopment in preterm infants. Neonatology. 2012;102:19–24.
Meyers JM, Tan S, Bell EF, Duncan AF, Guillet R, Stoll BJ, et al. Neurodevelopmental outcomes among extremely premature infants with linear growth restriction. J Perinatol. 2019;39:193–202.
Vliegenthart RJS, van Kaam AH, Aarnoudse-Moens CSH, van Wassenaer AG, Wes, Onland W. Duration of mechanical ventilation and neurodevelopment in preterm infants. Arch Dis Child Fetal Neonatal Ed. 2019;0:F1–5.
Patra K, Greene MM, Patel AL, Meier P. Maternal education level predicts cognitive, language, and motor outcome in preterm infants in the second year of life. Am J Perinatol. 2016;33:738–44.
Lowe JR, Nolen TL, Vohr B, Adams-Chapman I, Duncan AF, Watterberg K. Effect of primary language on developmental testing in children born extremely preterm. Acta Paediatr. 2013;102:896–900.
Van Veen S, Remmmers S, Aarnoudse-Moens CSH, Oosterlaan J, van Kaam AH, van Wassenaer-Leemhuis AG. Multilingualism was associated with lower cognitive outcomes in children who were born very and extremely preterm. Acta Paediatr. 2019;108:479–85.
Patra K, Hamilton M, Johnson TJ, Greene M, Dabrowski E, Meier PP, et al. NICU human milk dose and 20-month neurodevelopmental outcome in very low birth weight infants. Neonatology. 2017;112:330–6.
Lechner BE, Vohr BR. Neurodevelopmental outcomes of preterm infants fed human milk: a systematic review. Clin Perinatol. 2017;44:69–83.
Bills SE, Johnston JD, Shi D, Bradshaw J. Social-environmental moderators of neurodevelopmental outcomes in youth born preterm: a systematic review. Child Neuropsychol. 2020;21:1–20.
Acknowledgements
We thank Dr Pierpaolo Brovedani for the collaboration in the follow-up visits of the preterm infants of Our Unit. We also acknowledge our mentor Dr. Sergio Demarini.
Author information
Authors and Affiliations
Contributions
JB had primary responsibility for protocol development, supervision of data collection and curation, and writing of the manuscript. FMR participated in the development of the analytical framework for the study and reviewed the manuscript. MB was responsible for Bayley testing at 2 years of age. FV was responsible for initial data collection and participated in the preliminary data analysis. LT participated in data collection, in the development of the analytical framework for the study and review of the manuscript. GP supervised the design of the study, performed the final data analyses and contributed to the writing of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Bua, J., Risso, F.M., Bin, M. et al. Association between body composition at term equivalent age and Bayley scores at 2 years in preterm infants. J Perinatol 41, 1852–1858 (2021). https://doi.org/10.1038/s41372-021-01074-x
Received:
Revised:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41372-021-01074-x
This article is cited by
-
Neonatal malnutrition, body composition, and childhood obesity in critically ill infants
Maternal Health, Neonatology and Perinatology (2025)
-
Fat-free mass is associated with neurodevelopment outcomes in extremely preterm infants up to 3 years of age
Pediatric Research (2025)
-
Differential associations between body composition indices and neurodevelopment during early life in term-born infants: findings from the Pakistan cohort: Multi-Center Body Composition Reference Study
European Journal of Clinical Nutrition (2024)
-
Body composition measurement for the preterm neonate: using a clinical utility framework to translate research tools into clinical care
Journal of Perinatology (2022)